Human Parasites: Common Infections, Symptoms, Testing, and Treatment
Parasites are organisms that live on or in another organism (the host) and depend on the host for survival, often at the host's expense. Globally, parasitic infections remain a major source of disease — the World Health Organization estimates that more than 1.5 billion people carry intestinal worms, hundreds of millions are affected by malaria, and tens of millions live with chronic infections like Chagas, schistosomiasis, and toxoplasmosis. Even in high-income countries with safe water and food, sub-clinical parasitic infections are more common than most people realize, particularly among travelers, immigrants, immunocompromised patients, dog and cat owners, and those who consume undercooked meat or unwashed produce.
This page is an overview hub. It covers what parasites are, the most common categories you may encounter, signs and symptoms, how testing actually works (and why it often misses), conventional and naturopathic treatment options, and prevention. For drug-specific information, see the Fenbendazole page; for botanical antiparasitic options, the Herbs section.
Table of Contents
- Categories of Human Parasites
- Protozoa
- Helminths (Worms)
- Ectoparasites
- Symptoms and Red Flags
- Testing: What's Available and What Misses
- Conventional Treatment
- Naturopathic and Botanical Approaches
- Fenbendazole — A Note on Off-Label Use
- Prevention
- Research Papers and References
- Connections
- Featured Videos
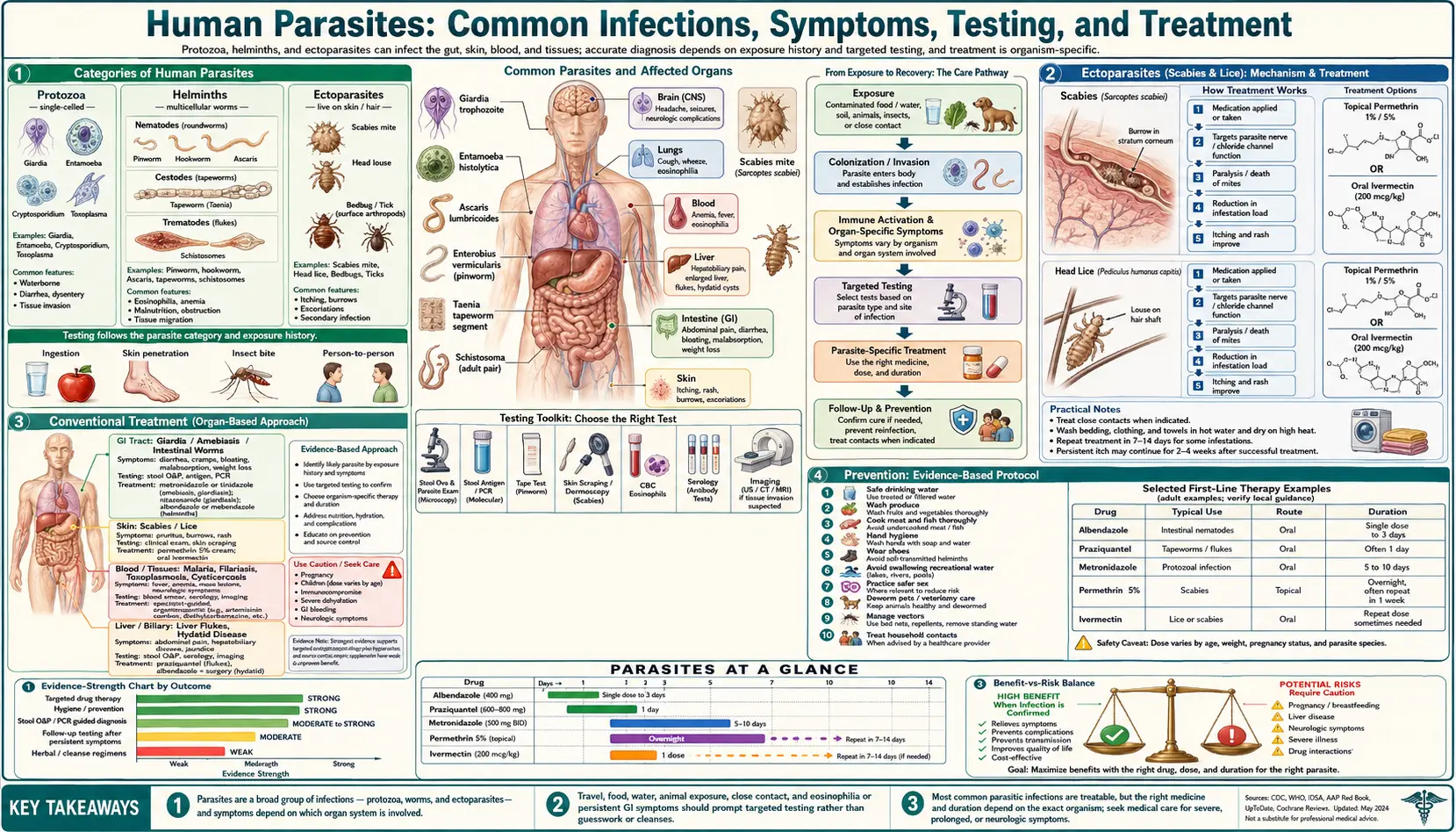
Categories of Human Parasites
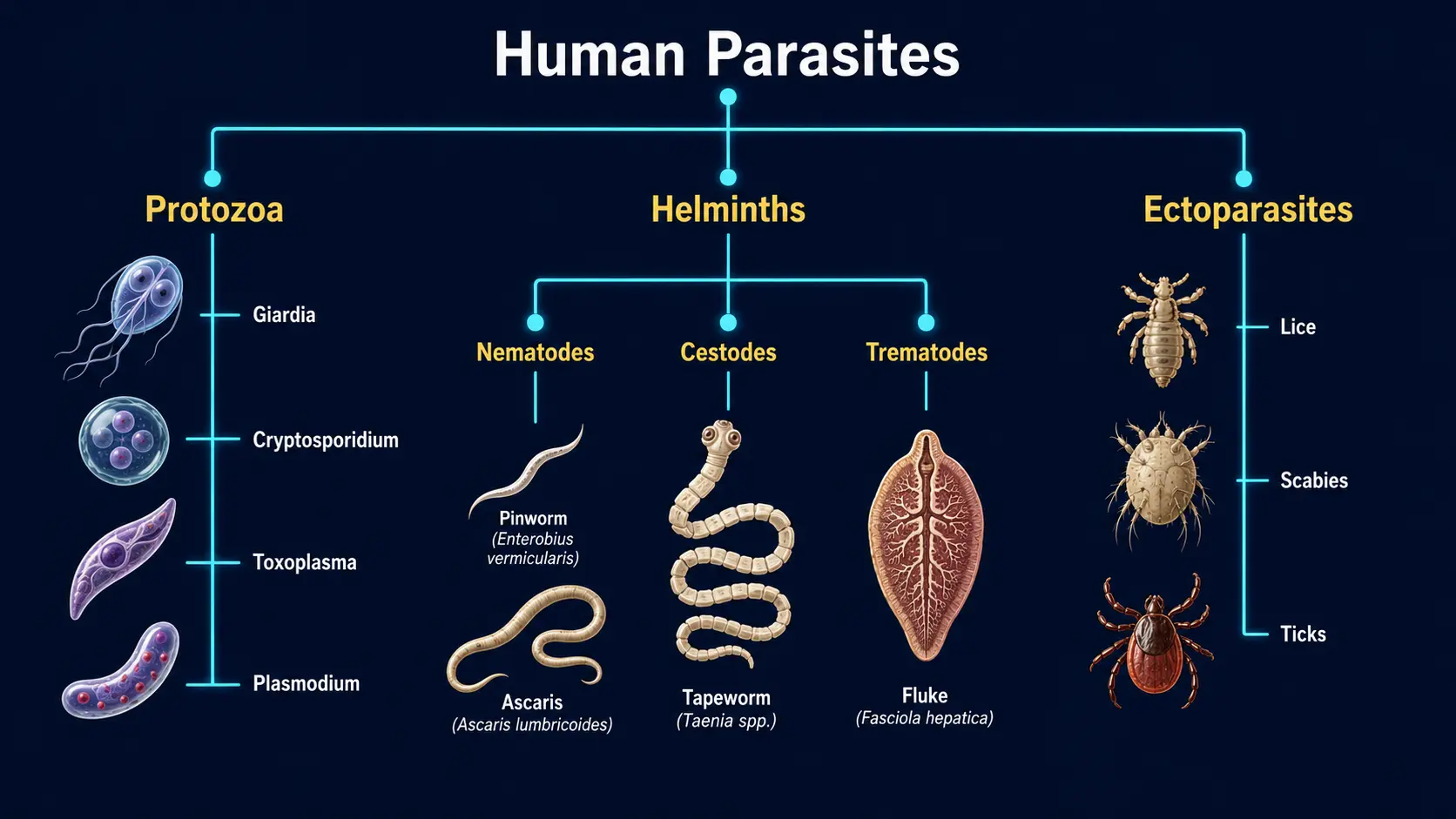
Human parasites fall into three broad biological categories, and several common species in each:
- Protozoa — single-celled organisms; reproduce inside the host. Examples: Giardia lamblia, Cryptosporidium, Entamoeba histolytica, Blastocystis, Toxoplasma gondii, Plasmodium (malaria).
- Helminths — multicellular worms. Three subgroups: roundworms (nematodes), flatworms (cestodes / tapeworms), and flukes (trematodes).
- Ectoparasites — live on the skin surface. Examples: lice, scabies mites, bed bugs, ticks (when feeding).
Protozoa
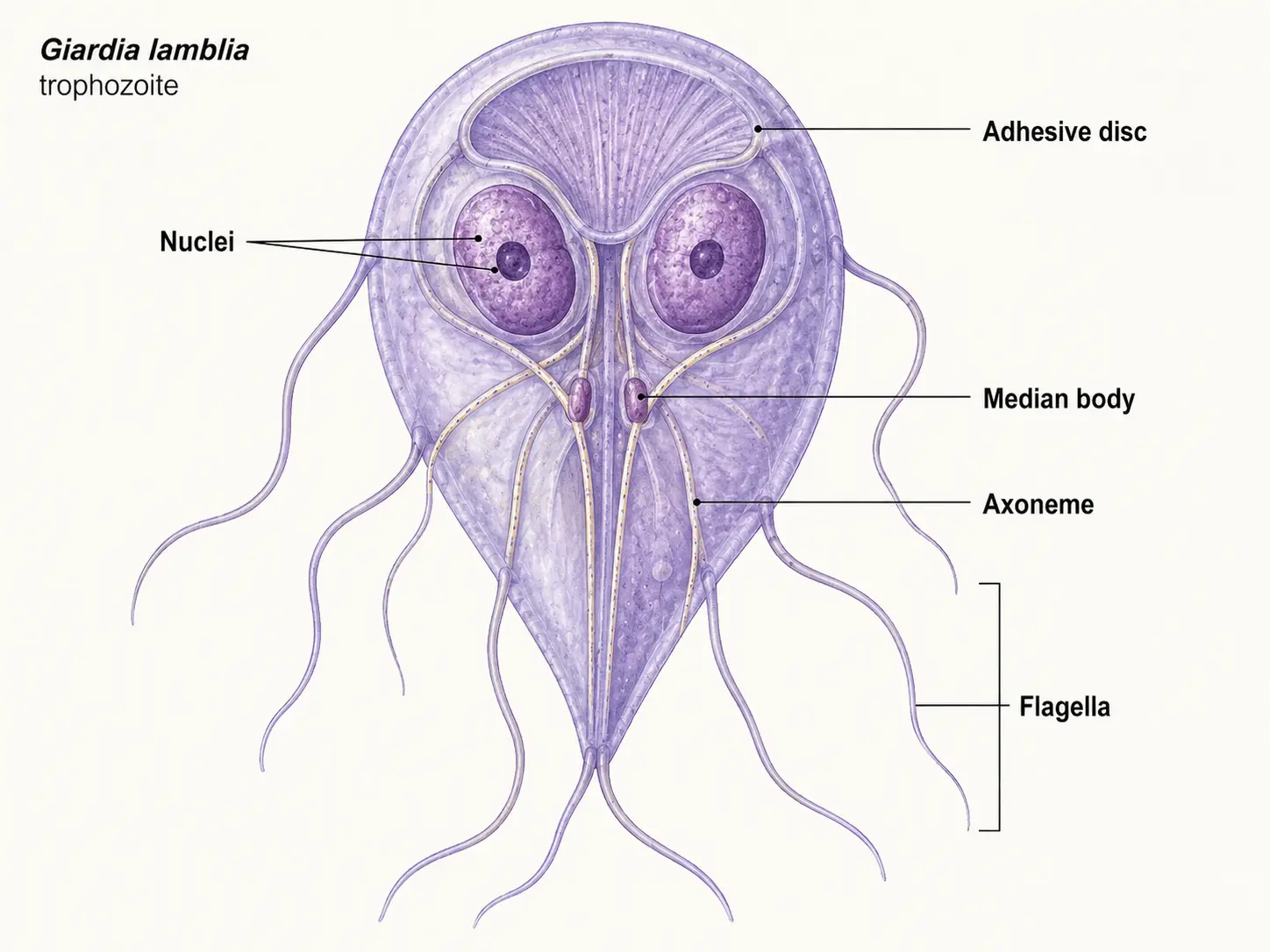
Giardia lamblia
The most common waterborne protozoan in the developed world. Acquired from contaminated water (lakes, streams, well water) or person-to-person fecal-oral spread (daycare settings). Causes "beaver fever": chronic diarrhea, foul-smelling stools, bloating, gas, fatigue, and malabsorption. Diagnosis is by stool antigen (more sensitive) or stool ova-and-parasite microscopy (less sensitive). First-line treatment: tinidazole or metronidazole; nitazoxanide for resistant cases.
Cryptosporidium parvum
Another waterborne protozoan; resistant to chlorination, which is why municipal outbreaks still occur. Causes profuse watery diarrhea. Self-limited in immunocompetent adults but can be life-threatening in HIV/AIDS. Diagnosis: stool antigen, modified acid-fast staining. Nitazoxanide is the only FDA-approved treatment.
Entamoeba histolytica
Causes amebic dysentery (bloody diarrhea), liver abscess. Acquired from contaminated water or food, particularly in tropical and subtropical regions. Diagnosis: stool antigen / PCR (microscopy alone confuses pathogenic E. histolytica with non-pathogenic E. dispar). Treatment: metronidazole followed by a luminal agent (paromomycin or iodoquinol) to clear cyst-stage organisms.
Blastocystis spp
Common gut commensal that can become symptomatic in some hosts — chronic diarrhea, abdominal pain, urticaria. Causality is debated; many people carry Blastocystis without symptoms. Treatment is controversial; metronidazole or nitazoxanide can be tried in symptomatic cases. Often co-occurs with SIBO and IBS.
Toxoplasma gondii
Acquired from undercooked meat or cat feces (litter box, garden soil). About 30% of the world's adults are seropositive. Usually asymptomatic in immunocompetent hosts but can cause flu-like illness, lymphadenopathy, eye disease, and serious problems in pregnancy (congenital toxoplasmosis) and immunocompromise. Diagnosis: serology. Treatment: pyrimethamine + sulfadiazine + leucovorin in symptomatic or pregnant cases.
Plasmodium spp (malaria)
Mosquito-borne; the leading cause of parasite-related death worldwide. Symptoms include cyclic fever, chills, headache, and severe complications including cerebral malaria. Diagnosis: blood smear, rapid antigen tests, PCR. Treatment depends on species and resistance patterns: artemisinin combination therapies are first-line in most settings.
Helminths (Worms)
Roundworms (nematodes)
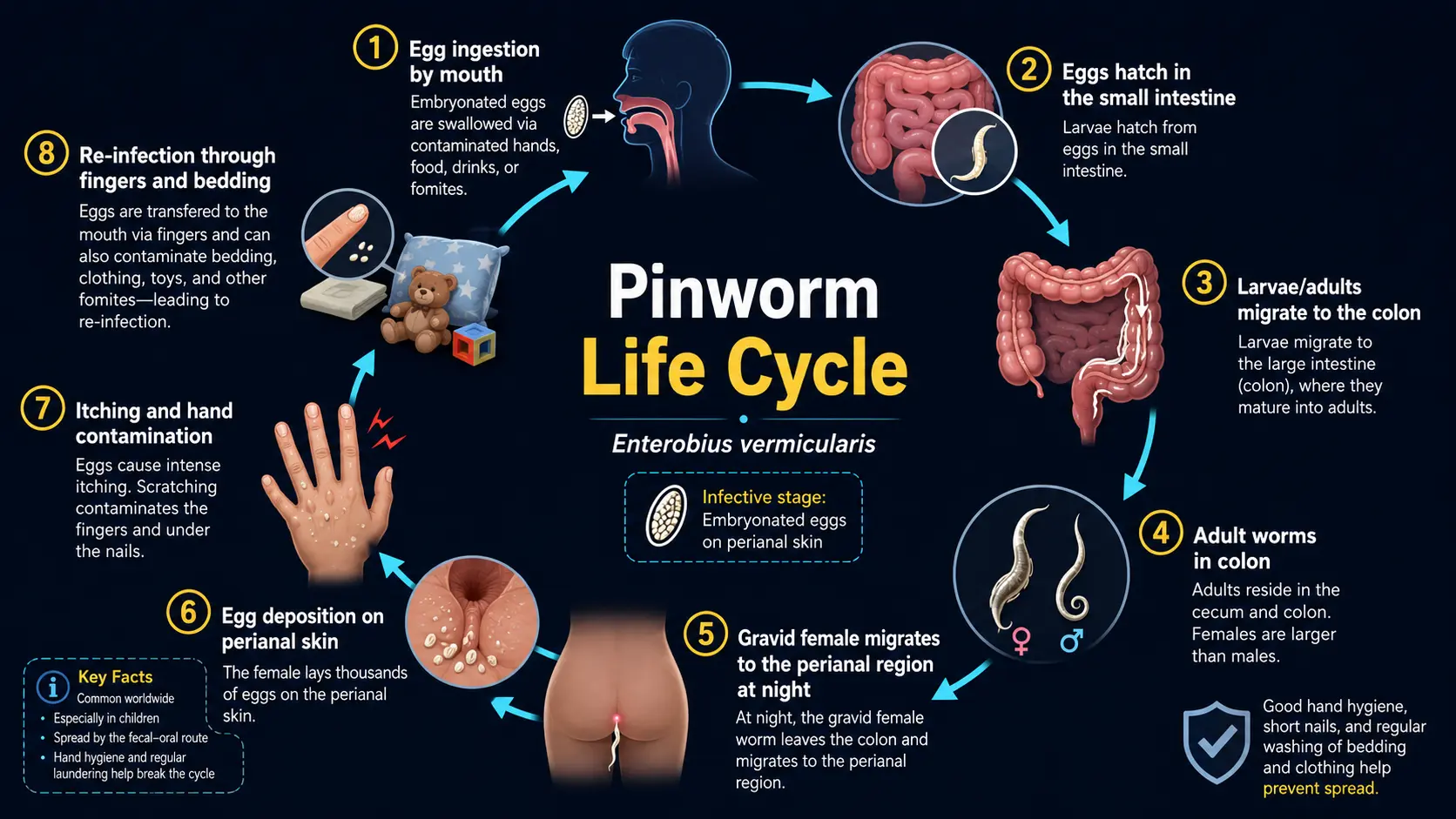
- Pinworm (Enterobius vermicularis) — the most common parasitic worm in the US. Children are the primary host; nighttime perianal itching is the classic symptom. Diagnosis: tape test. Treatment: mebendazole or albendazole; treat the whole household.
- Roundworm (Ascaris lumbricoides) — the largest intestinal worm; can grow to 35 cm. Acquired from contaminated soil; common in tropical regions. Most carriers are asymptomatic; heavy loads cause GI symptoms and rare obstruction. Treatment: albendazole or mebendazole.
- Hookworm (Necator americanus, Ancylostoma duodenale) — penetrates skin from contaminated soil. Causes iron-deficiency anemia from chronic blood loss in the gut. Treatment: albendazole or mebendazole + iron repletion.
- Whipworm (Trichuris trichiura) — tropical regions; usually asymptomatic, heavy infections cause dysentery and rectal prolapse in children. Treatment: albendazole + ivermectin combination is more effective than albendazole alone.
- Strongyloides stercoralis — auto-infective; can persist for decades. Highly dangerous in immunocompromise (hyperinfection syndrome). Diagnosis: serology + stool. Treatment: ivermectin.
- Trichinella spiralis — from undercooked pork or wild game. Causes muscle pain, fever, periorbital edema, eosinophilia. Diagnosis: serology, muscle biopsy. Treatment: albendazole + steroids in heavy infection.
Flatworms / tapeworms (cestodes)
- Beef tapeworm (Taenia saginata) and pork tapeworm (Taenia solium) — from undercooked meat. Pork tapeworm larvae can lodge in brain and muscle (cysticercosis). Treatment: praziquantel.
- Fish tapeworm (Diphyllobothrium latum) — from raw or undercooked freshwater fish; competes for vitamin B12. Treatment: praziquantel.
- Echinococcus granulosus (hydatid disease) — from dogs and livestock; forms cysts in liver and lung. Treatment: surgical or PAIR procedure + albendazole.
Flukes (trematodes)
- Schistosoma spp — freshwater snail intermediate host; dermatologic, GI, urinary tract, and chronic liver/bladder disease. Treatment: praziquantel.
- Liver flukes (Fasciola, Clonorchis, Opisthorchis) — from undercooked freshwater fish or contaminated watercress. Treatment: triclabendazole or praziquantel.
Ectoparasites
- Head/body/pubic lice — permethrin, malathion, ivermectin lotion
- Scabies (Sarcoptes scabiei) — intensely itchy skin burrows; permethrin cream or oral ivermectin
- Bed bugs (Cimex lectularius) — not a true infection; itchy bites; environmental control is the treatment
- Ticks — vectors for Lyme disease, Rocky Mountain spotted fever, anaplasmosis, babesiosis, alpha-gal syndrome (a meat allergy from Lone Star tick saliva — see Alpha-Gal Syndrome)
Symptoms and Red Flags
Parasitic infections can be asymptomatic, mild, or severe. Common chronic symptoms in patients who turn out to have a parasite:
- Chronic, intermittent diarrhea or alternating diarrhea and constipation
- Persistent abdominal pain, bloating, gas
- Foul-smelling, greasy, or floating stools (suggests fat malabsorption from giardia or other small-bowel infection)
- Unexplained weight loss
- Fatigue out of proportion to lifestyle
- Chronic urticaria (hives), itching, or unexplained rashes
- Iron-deficiency anemia in someone with adequate dietary intake (think hookworm or whipworm)
- Eosinophilia on CBC (helminth infections particularly)
- Nighttime perianal itching (pinworm)
- Teeth grinding in children (sometimes attributed to pinworm)
- Travel history with onset of new GI or systemic symptoms
Red flags warranting prompt medical evaluation: bloody diarrhea, fever, severe abdominal pain, jaundice, neurologic symptoms (seizures, focal deficits — possible neurocysticercosis), eye involvement (toxoplasmosis), respiratory symptoms with eosinophilia (Strongyloides hyperinfection), or any acute symptoms in an immunocompromised patient.
Testing: What's Available and What Misses
Parasite diagnosis is harder than most patients expect. The traditional "ova and parasites" stool exam (O&P) requires three specimens collected on different days and examined microscopically. Even at competent labs the sensitivity for many organisms is only 50–75% per single specimen. Modern alternatives are more sensitive:
- Stool antigen tests — widely available for Giardia, Cryptosporidium, and Entamoeba histolytica; sensitivities of 85–95% on a single specimen
- Multiplex PCR stool panels (BioFire FilmArray GI, BD MAX) — cover 22+ pathogens including parasites, bacteria, viruses; sensitivities > 95%; not yet standard at every hospital
- Serology — for tissue-invasive parasites that may not appear in stool: Strongyloides, Toxoplasma, Trichinella, Schistosoma, Cysticercus, Toxocara, Echinococcus
- Tape test — pinworm (perianal cellulose tape pressed against the skin in the morning before bathing)
- Blood smear — malaria, babesiosis, microfilariae
- Imaging — CT or MRI for neurocysticercosis, hydatid cysts, liver abscess
- Eosinophilia + IgE elevation on routine bloodwork — supporting evidence for helminth infection but non-specific
If you've had three negative O&P exams but the clinical suspicion remains high, ask about antigen testing, PCR multiplex, and serology — the older test misses many organisms.
Conventional Treatment
The major antiparasitic drug families:
- Benzimidazoles — albendazole, mebendazole, fenbendazole (veterinary, but used off-label). Disrupt parasite microtubules. Broad nematode coverage; some helminths.
- Avermectins — ivermectin. Disrupts glutamate-gated chloride channels in parasites. Effective against Strongyloides, scabies, lice, river blindness, lymphatic filariasis.
- 5-nitroimidazoles — metronidazole, tinidazole, secnidazole. Anaerobic protozoa: Giardia, amebiasis, trichomoniasis.
- Praziquantel — the universal cestode/trematode drug.
- Nitazoxanide — broad-spectrum: Cryptosporidium, Giardia, helminths; well-tolerated.
- Pyrantel pamoate — OTC in the US (Pin-X, Reese's Pinworm Medicine); pinworm and roundworm.
- Antimalarials — artemisinin combinations, atovaquone-proguanil, chloroquine (where still effective), primaquine.
For most outpatient parasitic infections in the US, a confirmed diagnosis followed by a single targeted course is curative. Empiric treatment without diagnosis is occasionally appropriate (pinworm in symptomatic households, traveler's diarrhea in some settings) but generally suboptimal — the wrong drug for the wrong organism doesn't work.
Naturopathic and Botanical Approaches
Several traditional botanicals show in-vitro and limited clinical antiparasitic activity. They are most appropriate as adjuncts to conventional treatment, for sub-clinical dysbiosis, or in cases where targeted antiparasitic drugs are contraindicated. They should not replace conventional therapy in confirmed parasitic disease.
- Black seed (Nigella sativa) — thymoquinone has demonstrated activity against Schistosoma, Giardia, and tapeworm in animal models
- Garlic (Allium sativum) — allicin shows activity against Giardia and Entamoeba in vitro
- Pau d'arco (Tabebuia impetiginosa) — lapachol has historical use for parasitic and fungal infections
- Wormwood (Artemisia absinthium) — the historical anti-helminthic; artemisinin (from Artemisia annua) is the basis of modern anti-malarials
- Black walnut hull (Juglans nigra) — juglone has anti-parasitic activity; traditional in herbal protocols
- Cloves (Syzygium aromaticum) — eugenol; included in classic three-herb anti-parasitic combinations
- Pumpkin seeds (Cucurbita pepo) — cucurbitin; folk remedy for tapeworms
- Goldenseal (Hydrastis canadensis) — berberine has activity against Giardia and Entamoeba
- Cumin (Cuminum cyminum) — gut antimicrobial activity
- Probiotics — specific strains (Saccharomyces boulardii in particular) reduce Giardia symptoms and shedding
- Berberine-containing herbs — goldenseal, barberry; activity against Giardia, Entamoeba
Fenbendazole — A Note on Off-Label Use
Fenbendazole is a benzimidazole antiparasitic approved for veterinary use. It has gained significant attention online for off-label human use, including for helminth infections and in unproven cancer protocols. The page Fenbendazole covers what is and isn't established about safety, dosing, and the limits of the evidence. Anyone considering it should first work with a clinician who can confirm the parasitic diagnosis (so the right drug is chosen), check for drug interactions, and monitor for hepatic effects.
Prevention
- Cook meat thoroughly — pork, beef, fish, wild game (USDA temperatures: pork and beef 145°F, ground meat 160°F, poultry 165°F, fish 145°F)
- Wash hands after handling raw meat, after using the bathroom, after gardening, after handling pets, before food prep
- Wash fruits and vegetables, especially leafy greens, herbs, and produce eaten raw
- Drink water from safe sources; filter or boil suspect water; iodine or chlorine for backcountry use
- Avoid swallowing water in lakes, rivers, swimming pools (especially while traveling)
- Litter box hygiene — daily scoop, gloves; pregnant women should avoid handling cat litter
- Insect protection in endemic regions: DEET / picaridin, permethrin-treated clothing, bed nets
- Annual deworming for pets following veterinary protocols
- Children with confirmed pinworm: wash bedding, vacuum thoroughly, treat the whole household, repeat treatment in 2 weeks
- Travelers returning from tropical regions with new symptoms: ask about parasitology specifically
Research Papers and References
- Intestinal parasites diagnosis and treatment — PubMed search
- Giardia treatment options — PubMed search
- Albendazole and mebendazole for helminths — PubMed search
- Ivermectin for Strongyloides and scabies — PubMed search
- Multiplex stool PCR sensitivity — PubMed search
- Blastocystis and pathogenicity debate — PubMed search
- Botanical antiparasitic activity — PubMed search
- Eosinophilia and helminth infection — PubMed search
External Authoritative Resources
- CDC — Parasites Information
- WHO — Soil-Transmitted Helminth Infections
- CDC DPDx — Laboratory Identification of Parasites
Connections
- Fenbendazole
- Garlic
- Goldenseal
- Black Seed
- Cumin
- Barberry
- Pau d'Arco
- Berberine (Herb)
- Probiotics
- SIBO
- Alpha-Gal Syndrome
- Anemia
- Complete Blood Count
- Gut Healing
- Detox Protocols
- Malaria
- Abdominal Pain
- Oregano