Anemia
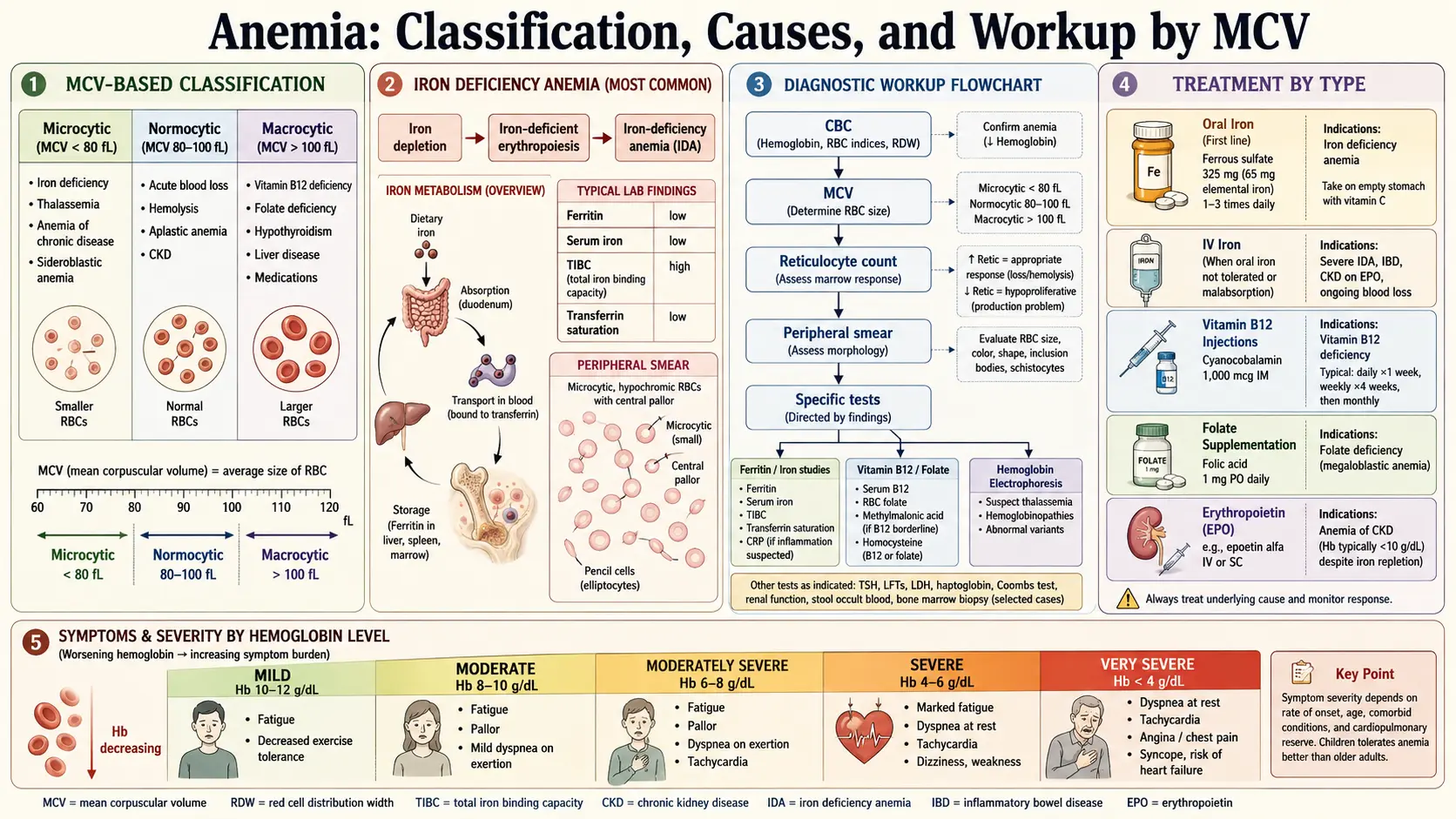
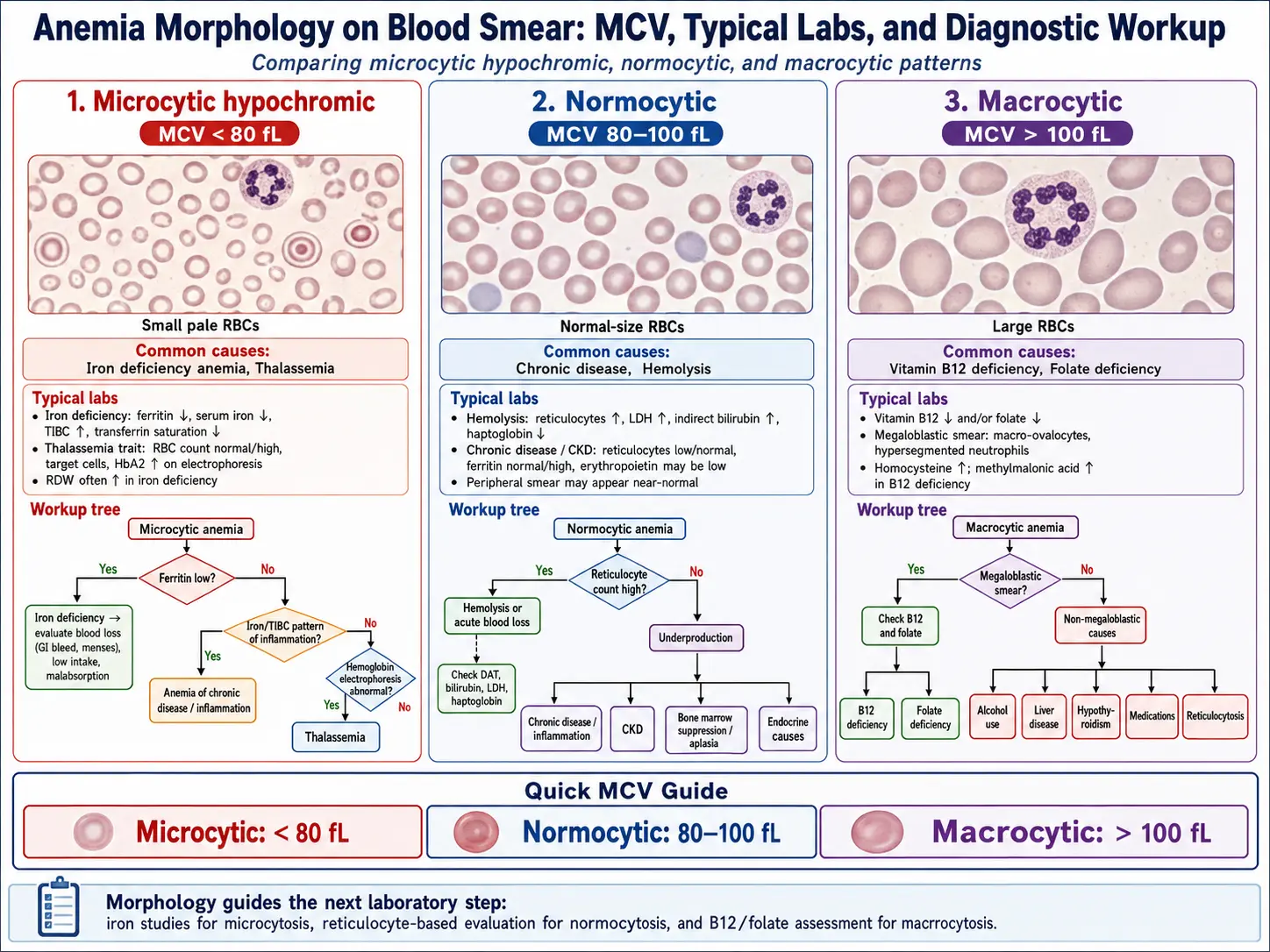
Table of Contents
- What is Anemia?
- Types of Anemia
- Common Symptoms of Anemia
- Causes and Risk Factors
- Diagnosis
- Treatment Options
- Prevention and Management Strategies
- Complications of Anemia
- Research Papers
- Connections
- Featured Videos
What is Anemia?
Anemia is a condition in which the body lacks enough healthy red blood cells to carry adequate oxygen to the body’s tissues. This can result in fatigue and weakness. There are various types of anemia, each with its own causes and treatments.
Types of Anemia
1. Iron-Deficiency Anemia
- Most common type of anemia.
- Caused by a lack of iron, which the body needs to produce hemoglobin.
- Common causes: Blood loss, poor diet, or an inability to absorb iron.
2. Vitamin Deficiency Anemia
- Includes megaloblastic anemia, such as vitamin B12 and folate deficiency anemia.
- Pernicious anemia: A type of B12 deficiency caused by the body's inability to absorb the vitamin.
3. Anemia of Chronic Disease
- Associated with chronic conditions such as cancer, kidney disease, and autoimmune disorders.
- Cause: The body’s response to chronic illness affects red blood cell production.
4. Aplastic Anemia
- Rare and serious condition where the bone marrow fails to produce enough blood cells.
- Causes: Autoimmune disease, exposure to toxic chemicals, certain drugs, or viral infections.
5. Hemolytic Anemia
- Caused by the destruction of red blood cells faster than the body can replace them.
- Can be inherited or acquired due to conditions like autoimmune diseases or certain medications.
6. Sickle Cell Anemia
- Inherited form of anemia characterized by abnormally shaped red blood cells.
- Causes chronic pain and complications due to blocked blood flow.
Common Symptoms of Anemia
- Fatigue
- Weakness
- Pale or yellowish skin
- Shortness of breath
- Dizziness or lightheadedness
- Chest pain
- Cold hands and feet
- Headaches
Causes and Risk Factors
- Blood loss: Due to heavy menstrual periods, ulcers, or trauma.
- Poor diet: Insufficient intake of iron, vitamin B12, or folate.
- Chronic diseases: Such as cancer, kidney disease, or inflammatory diseases.
- Family history: Certain types of anemia, such as sickle cell anemia or thalassemia, are inherited.
- Pregnancy: Increased blood volume during pregnancy can dilute red blood cells, leading to anemia.
Diagnosis
- Physical examination: To check for signs such as pale skin or rapid heartbeat.
- Blood tests:
- Complete blood count (CBC): Measures levels of red blood cells and hemoglobin.
- Iron tests: To check iron levels and storage.
- Vitamin B12 and folate tests: To identify deficiencies.
- Bone marrow biopsy: May be needed for cases of unexplained anemia or suspected bone marrow disorders.
Treatment Options
- Iron-deficiency anemia:
- Iron supplements: To replenish iron stores.
- Diet changes: Include iron-rich foods such as red meat, dark leafy greens, and fortified cereals.
- Vitamin deficiency anemia:
- Supplements: B12 or folic acid pills or injections.
- Diet adjustments: Consuming foods rich in B12 (meat, dairy) and folate (citrus fruits, beans).
- Anemia of chronic disease:
- Treat underlying condition: Managing the chronic disease can help improve anemia.
- Aplastic anemia:
- Blood transfusions or bone marrow transplant.
- Medications: Immunosuppressants or growth factors to stimulate blood cell production.
- Hemolytic anemia:
- Treat infections or discontinue drugs causing red blood cell destruction.
- Immunosuppressive medications if related to autoimmune causes.
Prevention and Management Strategies
- Eat a balanced diet: Include iron, vitamin B12, and folate-rich foods.
- Regular check-ups: Monitor health and manage conditions that may cause anemia.
- Take supplements as prescribed by a doctor, especially during pregnancy or if at risk for deficiencies.
- Manage chronic conditions: Proper management of chronic diseases can help prevent anemia.
Complications of Anemia
- Severe fatigue: Can interfere with daily life and productivity.
- Heart problems: Increased risk of arrhythmias or heart failure due to overworked heart compensating for low oxygen levels.
- Pregnancy complications: Risk of preterm birth and low birth weight.
- Delayed growth: In children, anemia can lead to growth and developmental delays.
Research Papers
The following PubMed topic searches return current peer-reviewed literature relevant to this condition. Each link opens a live PubMed query.
- Iron-deficiency anemia
- Anemia of chronic disease
- Vitamin B12 deficiency anemia
- Folate deficiency anemia
- Pernicious anemia
- Aplastic anemia
- Hemolytic anemia
- Anemia pregnancy
- Anemia elderly
- Anemia management guidelines
- Anemia global burden
- Hepcidin iron metabolism
Connections
- Iron
- Relationship Between Hemoglobin and Ceruloplasmin — why ceruloplasmin (the copper ferroxidase) is required to load iron into hemoglobin, and why "iron-deficiency anemia" is often functional copper deficiency.
- Thalassemia
- Vitamin B12
- Fatigue
- Complete Blood Count
- Lightheadedness
- Cold Hands and Feet
- Sickle Cell Disease
- Hemochromatosis
- Polycythemia Vera
- Thrombocytopenia
- Heart Palpitations
- Folate
- Hair Loss
- Iron Deficiency Anemia
- Vitamin B12 Test
- Kidney Disease
- Shortness of Breath