Alpha-Gal Syndrome: The Tick-Driven Allergy to Red Meat

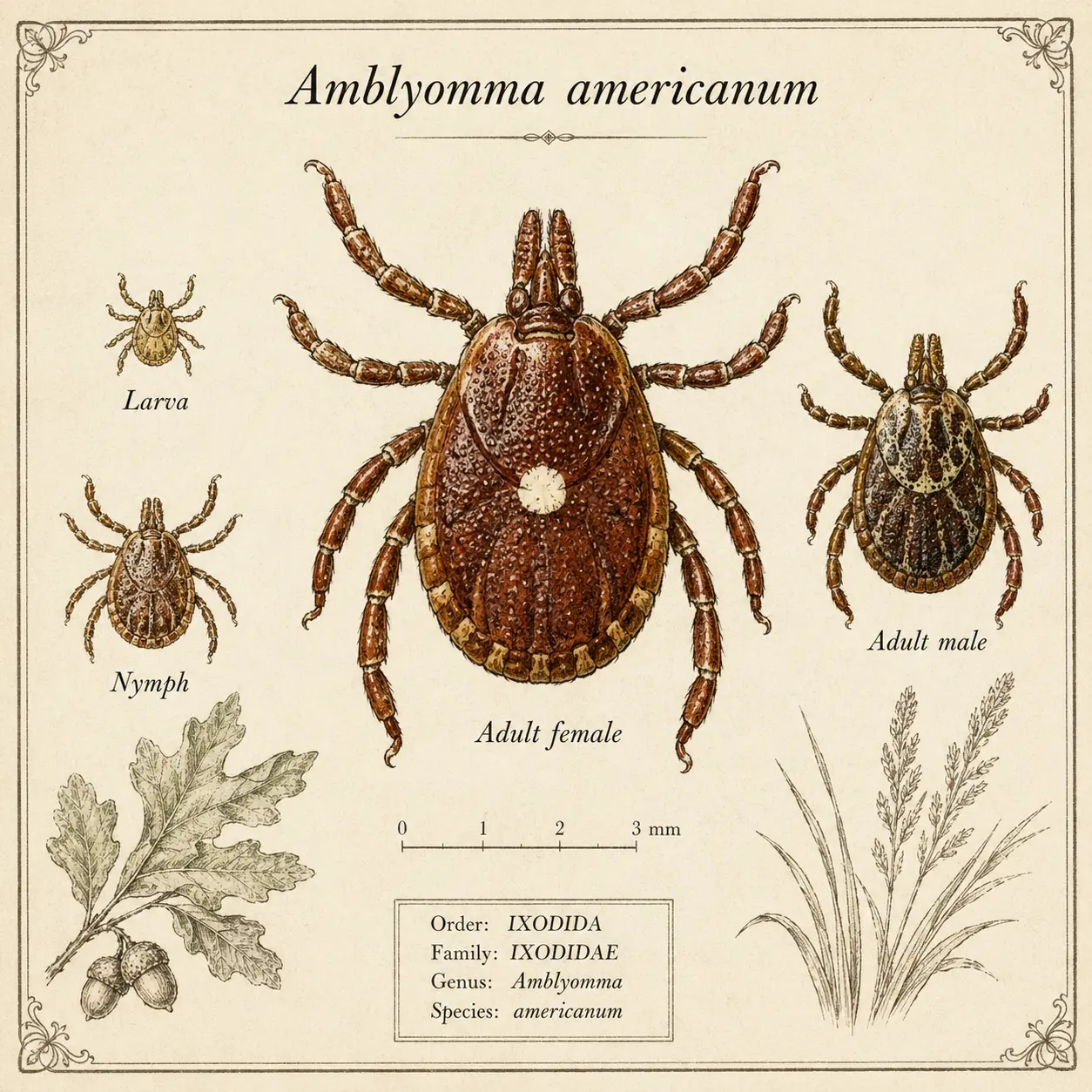
Alpha-gal syndrome (AGS) is an acquired allergy to a carbohydrate called galactose-α-1,3-galactose (alpha-gal) that is present in the flesh of non-primate mammals — beef, pork, lamb, venison, rabbit, goat — and in some mammal-derived products including gelatin, dairy, and certain medications. Unlike most food allergies, which develop in childhood or involve proteins, alpha-gal allergy is triggered in adults by the bite of specific ticks (primarily the lone star tick in the United States, Amblyomma americanum). Reactions are characteristically delayed — occurring 2 to 6 hours after eating red meat rather than immediately — which is one reason the condition went unrecognized for decades.
Deep-Dive Articles
Alpha-gal syndrome is a moving-target diagnosis — the food list is longer than you think, the medication cross-reactivity catches people off guard, and tick prevention is how you keep it from worsening over time. The eight articles below each tackle one piece: the science behind the tick, the complete mammalian-food avoidance list, the hidden medication sources, the emergency plan if you react, and what you can actually eat at restaurants. Start with whichever piece matches where you are right now.
Tick-Origin Science
How a lone star tick bite teaches your immune system to attack a sugar found in every mammal except primates. The molecular mimicry, which tick species cause it worldwide (Lone Star, castor bean, paralysis tick), and why a second tick bite can reset the clock years after you thought you’d recovered.
Complete Mammalian Foods List
Beyond obvious beef/pork/lamb: gelatin (jello, gummies, marshmallows, capsules), dairy (butter, cream, cheese — tolerance varies), lard, tallow, carrageenan questions, bone broth, organ meats. The complete avoid/allowed grocery-store reference.
Cross-Reactive Medications
Cetuximab (the drug that originally identified alpha-gal), heparin, porcine-derived pancreatic enzymes, bovine insulin, gelatin-containing vaccines (MMR, varicella, zoster, flu) and vaccine-capsule gelatin, magnesium stearate debate, and the pre-surgery medication list you need in your wallet.
Anaphylaxis Emergency Plan
Why delayed-onset anaphylaxis (3–6 hours after eating) is so easy to miss, how to use an EpiPen, when to call 911, the emergency kit for your bag and nightstand, and how to brief family members. The written action plan you hand to the ER.
Testing & Diagnosis
Alpha-gal IgE (Viracor, Mayo), total IgE + component testing, tryptase for co-existing MCAS, why skin-prick testing misses the diagnosis, titer interpretation (where is your number heading over time), and how to talk your doctor into ordering the right panel.
Restaurant & Travel Survival
Cuisines that are easy (most Asian, most Mediterranean fish dishes) vs. traps (hidden lard in refried beans, butter on steak, beef-stock sauces). Chef card templates, airplane meal ordering, cruise ship strategies, and country-by-country notes for travel.
Tick Bite Prevention
Permethrin-treated clothing (DIY + commercial), DEET vs. picaridin vs. oil-of-lemon-eucalyptus, tick checks that actually work, how to remove a tick correctly, yard management (leaf litter, deer, mice), and why every new bite can set your recovery back.
Natural History & Tolerance
What the research shows about whether alpha-gal IgE drops over time (it usually does, 1–5 years with strict avoidance + no new tick bites), who has worse outcomes, and the experimental tolerance-building research that’s currently in clinical trials.
Alpha-Gal & Cardiovascular Risk
Emerging research linking alpha-gal sensitization to coronary plaque and CV risk.
Table of Contents
- Deep-Dive Articles
- What Alpha-Gal Is
- How Tick Bites Cause Food Allergy
- Geography and Epidemiology
- Symptoms and the Delayed Pattern
- Diagnosis
- What to Avoid
- Hidden Sources and Medication Considerations
- Management
- Prognosis
- Connections
- Featured Videos
What Alpha-Gal Is
Alpha-gal is a sugar molecule present in the tissues of all non-primate mammals. Humans, apes, and Old World monkeys lack the enzyme (alpha-1,3-galactosyltransferase) to make it, and most people make only very low levels of antibodies against it. In alpha-gal syndrome, the immune system is sensitized to this sugar and produces IgE antibodies against it, leading to allergic reactions when mammalian meat is ingested.
How Tick Bites Cause Food Allergy
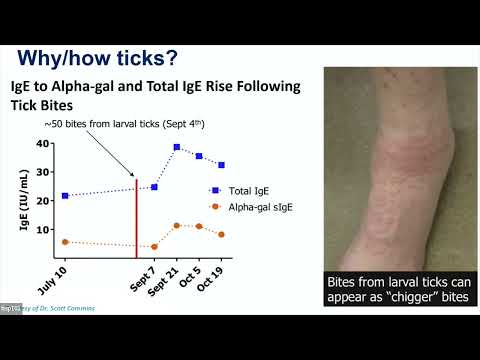
The lone star tick (and other tick species) has alpha-gal in its saliva. When the tick bites a human, it injects saliva with this sugar, and the immune system responds as though to a pathogen, producing IgE that specifically targets alpha-gal. On subsequent ingestion of mammalian meat, the IgE recognizes the dietary alpha-gal and triggers an allergic response — but because the sugar takes time to be processed and absorbed from dietary fat, the reaction is delayed by several hours rather than occurring immediately.
Geography and Epidemiology
Cases are most concentrated in the southeastern and south-central United States where the lone star tick is endemic, but its geographic range has expanded northward in recent decades, driving a commensurate expansion of AGS. The CDC estimates more than 450,000 Americans may have been affected since 2010; many cases are unrecognized. Cases are also reported in Europe (castor bean tick), Australia (paralysis tick), Africa, Asia, and Central and South America, each linked to local tick species.
Symptoms and the Delayed Pattern
- Hives, flushing, itching, angioedema
- Nausea, vomiting, diarrhea, abdominal cramping
- Wheezing, difficulty breathing
- Hypotension, palpitations, pre-syncope
- Full anaphylaxis in severe cases
- Waking in the middle of the night with symptoms several hours after an evening meat meal
The time delay — typically 3–6 hours post-ingestion — often leads patients and clinicians to miss the connection between meal and reaction. Cofactors such as alcohol, exercise, and NSAIDs can shorten the delay and intensify reactions.
Diagnosis
- Clinical history is often suggestive — delayed reactions after mammalian meat, often in someone with a history of tick exposure.
- Specific IgE testing to alpha-gal (galactose-alpha-1,3-galactose IgE) — the key serology.
- Skin-prick testing to beef, pork, or lamb extract is less reliable but can be supportive.
- Referral to an allergist familiar with AGS is valuable; the condition is still relatively new in many practices.
What to Avoid
- Beef, pork, lamb, venison, goat, rabbit, bison, elk, kangaroo, and all other mammalian meat
- Bone broth and soups made from mammalian bones
- Gelatin and gelatin-containing candies (gummy bears, marshmallows)
- Lard, tallow, and animal fats from mammals
- Organ meats
- Dairy and dairy-derived ingredients in more severely reactive patients
Poultry and seafood are safe — birds and fish do not contain alpha-gal.
Hidden Sources and Medication Considerations
- Gelatin capsules for medications and supplements.
- Medications in gelatin-based delivery systems.
- Cetuximab (Erbitux) — contains alpha-gal; major historical source of severe reactions.
- Some vaccines containing gelatin or bovine products.
- Heparin derived from porcine intestine.
- Bioprosthetic valves derived from bovine or porcine tissue.
- Magnesium stearate in some tablets.
- Carrageenan, glycerin, lanolin in some foods and cosmetics.
- Milk-based products for severely reactive patients.
Management
- Strict avoidance of mammalian meat and identified co-sensitizing products.
- Emergency epinephrine auto-injector.
- Antihistamines for mild reactions.
- Allergist follow-up; consider mast-cell stabilization if reactions are frequent.
- Prevent new tick bites — additional bites can re-boost IgE and worsen the condition.
- Check personal-care and pharmaceutical products for mammalian-derived ingredients.
- Educate family and food providers about hidden sources.
Prognosis
With avoidance of new tick bites, IgE levels can decline over months to years, and some patients regain tolerance of mammalian meat — though relapse after a new tick bite is typical. The condition is not necessarily lifelong but often is. Symptom severity varies widely between patients and over time.
Connections
- Natural History and Tolerance
- Tick Bite Prevention
- Mammalian Foods List
- Anaphylaxis Emergency Plan
- Tick-Origin Science
- Restaurant and Travel Survival
- Cross-Reactive Medications
- Testing and Diagnosis
- Alpha-Gal and Cardiovascular Risk
- Allergies
- Mast Cell Activation Syndrome
- Food Intolerance
- Lyme Disease
- Lyme Disease Prevention and Tick Removal
- Tick-Borne Co-Infections
- SIBO
- Elimination Diet
- Salmon
Research Papers
Explore current literature on alpha-gal syndrome via PubMed topic searches. These links open live PubMed searches for the listed keywords — results update as new studies are indexed.
- Clinical trials on alpha-gal syndrome — PubMed search
- Clinical trials on tick bite red meat allergy — PubMed search
- Clinical trials on galactose-alpha-1,3-galactose IgE — PubMed search
- Clinical trials on Lone Star tick Amblyomma americanum — PubMed search
- Clinical trials on alpha-gal allergy diagnosis — PubMed search
- Clinical trials on delayed anaphylaxis mammalian meat — PubMed search
Featured Videos

Alpha Gal Syndrome

What is alpha-gal syndrome?

Understanding Alpha-gal Syndrome with Dr. Rex Archer

What is alpha gal syndrome?

WHAT IS ALPHA-GAL SYNDROME? WHAT ARE ALPHA-GAL SYNDROME SYMPTOMS? A Doctor Explains

Alpha-gal syndrome creates nasty reaction to red meat

ILSI AM2020: Emerging Allergens: Case Study on Alpha-Gal Syndrome (Jamie Waldron)

A Tick Bite Can Make You Allergic to Red Meat? | Alpha-Gal Syndrome Explained by Allergists
Tick Bite and Anaphylaxis: The Many Faces of Alpha Gal Allergy

Living with Alpha gal Syndrome

Alpha-Gal Syndrome | ADH Public Health Grand Rounds

Beware the Bite: Ticks, Red Meat Allergies, and Alpha-Gal Syndrome

New Guidance on AlphaGal Syndromes GI Implications What to Know

Alpha Gal (Meat Allergy) - What is it?

Alpha gal Syndrome: It’s Not a Meat Allergy, It’s an Immune System Warning

Ask the Insider—Inside living with alpha-Gal syndrome 🍔🥓🥩 | Allergy Insider