Choline: The Essential Nutrient for Brain, Liver, and Cellular Health
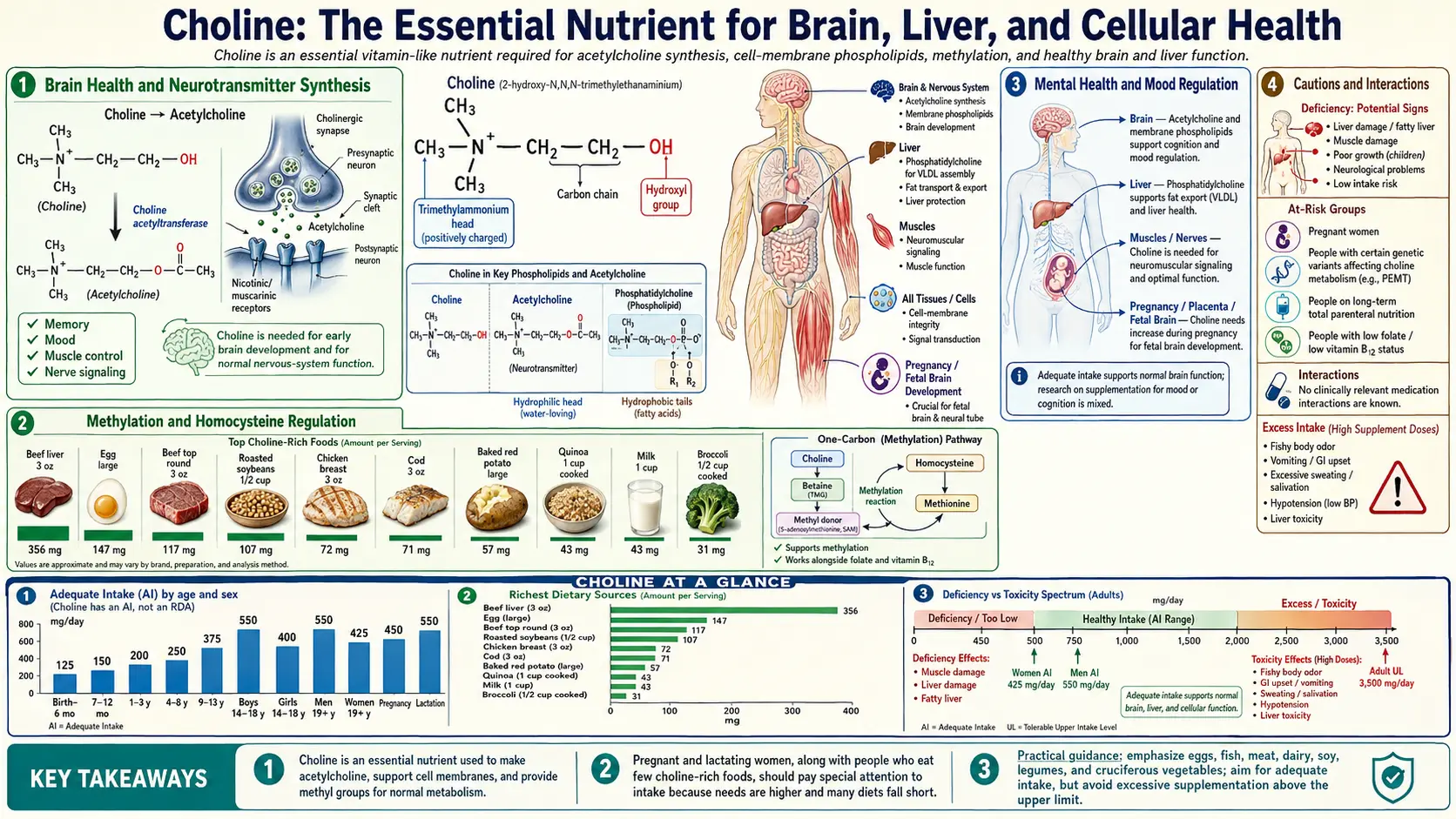
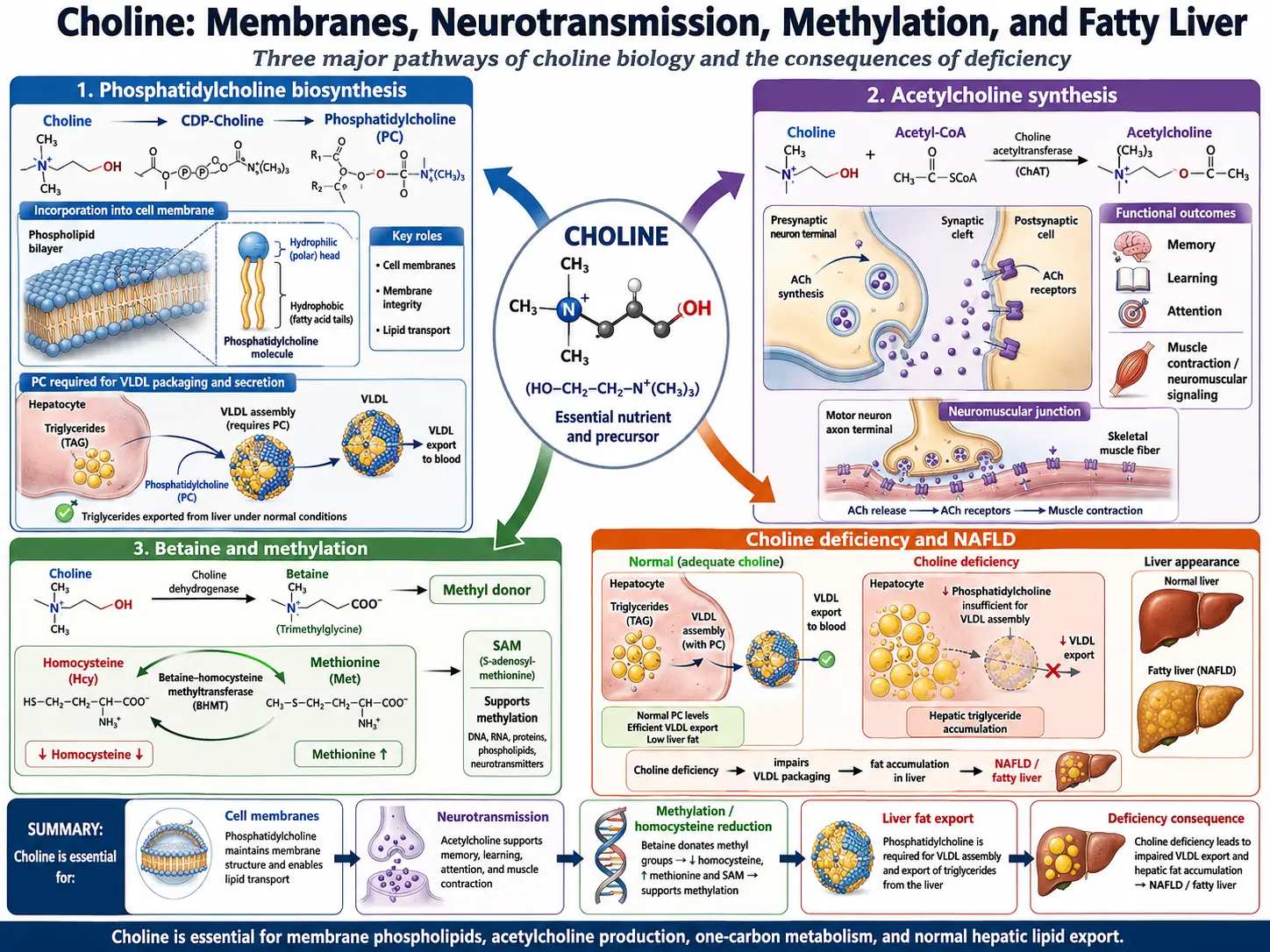
Choline is an essential nutrient that, despite its critical importance to virtually every organ system in the body, remains one of the most under-consumed nutrients in modern diets. Recognized as an essential nutrient by the Institute of Medicine in 1998, choline serves as a precursor to the neurotransmitter acetylcholine, the phospholipid phosphatidylcholine, and the methyl donor betaine. It is fundamental to brain development, liver function, cell membrane integrity, muscle movement, and nervous system signaling. An estimated 90% of Americans do not meet the adequate intake for choline, making it one of the most widespread nutritional shortfalls in the Western world.
Table of Contents
- Brain Health and Neurotransmitter Synthesis
- Liver Function and Fat Metabolism
- Cell Membrane Structure and Integrity
- Pregnancy and Fetal Development
- Methylation and Homocysteine Regulation
- Muscle Function and Athletic Performance
- Cardiovascular Health
- Mental Health and Mood Regulation
- Dietary Sources of Choline
- Deficiency Signs and Risk Factors
- Supplementation Forms and Dosing
- Cautions and Interactions
- Connections
- Featured Videos
1. Brain Health and Neurotransmitter Synthesis
Choline is the direct precursor to acetylcholine, one of the most important neurotransmitters in the human nervous system. Acetylcholine governs a staggering range of brain functions including memory formation, attention, learning, and the regulation of the sleep-wake cycle. It is also the primary neurotransmitter at the neuromuscular junction, where it triggers muscle contraction. Without adequate choline intake, the brain simply cannot produce sufficient acetylcholine to support optimal cognitive function.
Research has consistently demonstrated that higher choline intake is associated with better cognitive performance across the lifespan. A landmark study from Boston University, following over 1,400 adults for nearly a decade, found that individuals with higher dietary choline intake performed significantly better on tests of verbal memory and visual memory. Neuroimaging studies have shown that choline supplementation can increase the density of acetylcholine receptors in the brain, enhancing the efficiency of cholinergic neurotransmission.
The relationship between choline and age-related cognitive decline has attracted particular attention. As the brain ages, acetylcholine production naturally declines, contributing to the memory loss, reduced attention span, and slower information processing that characterize normal aging. In Alzheimer's disease, the degeneration of cholinergic neurons in the basal forebrain is one of the earliest and most prominent pathological features. In fact, the most commonly prescribed class of Alzheimer's medications, cholinesterase inhibitors (donepezil, rivastigmine, galantamine), works by preventing the breakdown of acetylcholine in the synaptic cleft. Ensuring adequate dietary choline throughout life may help maintain the cholinergic system and support cognitive resilience.
Animal studies have revealed that choline supplementation during critical developmental windows can produce lasting improvements in brain structure and function. Rodents given supplemental choline during gestation and early postnatal life show enhanced hippocampal development, improved spatial memory, and greater resistance to age-related cognitive decline. These findings suggest that choline's neuroprotective effects may be partly epigenetic, altering gene expression patterns that influence brain health for decades.
2. Liver Function and Fat Metabolism
The liver is one of the organs most dependent on adequate choline supply. Choline is required for the synthesis of phosphatidylcholine, the predominant phospholipid in very-low-density lipoprotein (VLDL) particles. VLDL is the primary vehicle by which the liver exports triglycerides to peripheral tissues. When choline is deficient, the liver cannot assemble and secrete VLDL properly, causing triglycerides to accumulate within hepatocytes. This leads to non-alcoholic fatty liver disease (NAFLD), a condition that can progress to steatohepatitis, fibrosis, and ultimately cirrhosis.
The connection between choline deficiency and fatty liver was dramatically demonstrated in controlled feeding studies where healthy volunteers placed on choline-deficient diets developed liver steatosis within weeks. Remarkably, the liver damage was fully reversible upon choline repletion, highlighting both the sensitivity of the liver to choline status and the therapeutic potential of choline supplementation in liver disease.
Choline also supports the liver's detoxification functions by contributing to the synthesis of glutathione, the body's master antioxidant, through the methionine-homocysteine cycle. Adequate choline helps maintain methylation capacity in the liver, which is essential for the Phase II conjugation reactions that neutralize and prepare toxins for excretion. Individuals with high alcohol consumption, those taking certain medications, and those with genetic polymorphisms in the PEMT gene (which affects endogenous choline synthesis) are at particularly high risk of choline-related liver dysfunction. Supporting liver health with choline-rich foods complements other liver cleansing protocols.
3. Cell Membrane Structure and Integrity
Every cell in the human body depends on choline for the structural integrity of its membranes. Phosphatidylcholine constitutes approximately 40-50% of the phospholipids in mammalian cell membranes, making it the single most abundant structural lipid in human cells. This phospholipid forms the fundamental bilayer architecture that separates the cell's interior from the extracellular environment, controls the passage of molecules in and out of the cell, and provides a platform for membrane-bound proteins involved in cell signaling.
Phosphatidylcholine's contribution to membrane fluidity is critical for normal cellular function. Cell membranes must maintain a precise balance between rigidity and fluidity to allow proper receptor function, ion channel activity, and vesicular transport. When choline intake is insufficient and phosphatidylcholine levels decline, membranes become more rigid and less functional, impairing cellular communication and nutrient transport. This is particularly consequential for rapidly dividing cells, including immune cells, red blood cells, and the epithelial cells lining the gut.
Beyond its structural role, phosphatidylcholine serves as a reservoir for signaling molecules. The enzyme phospholipase D cleaves phosphatidylcholine to release phosphatidic acid, a lipid second messenger involved in cell growth, survival, and proliferation. Phosphatidylcholine is also the primary source of arachidonic acid for the synthesis of eicosanoids, the lipid mediators that regulate inflammation, blood clotting, and immune responses. Through these pathways, choline influences cellular processes far beyond membrane architecture.
4. Pregnancy and Fetal Development
Choline requirements increase substantially during pregnancy, and the nutrient plays a role in fetal development that rivals that of folate. Choline is essential for neural tube closure, brain development, and the formation of the placenta. The developing fetal brain has an extraordinarily high demand for choline, which is actively transported across the placenta at concentrations three to four times higher than maternal blood levels.
A landmark randomized controlled trial conducted at Cornell University found that women who consumed 930 mg of choline per day during their third trimester (nearly double the adequate intake of 450 mg) gave birth to children who demonstrated significantly faster information processing speed at 4, 7, 10, and 13 months of age compared to children of mothers who consumed the standard amount. Follow-up studies showed that these cognitive advantages persisted into childhood, suggesting that maternal choline intake during pregnancy has lasting effects on offspring brain function.
Choline's role in fetal development extends beyond the brain. It is required for the proper formation of the placental vasculature, and choline deficiency during pregnancy has been associated with increased risk of preeclampsia, preterm birth, and low birth weight. Choline also interacts synergistically with folate and vitamin B12 in methyl group metabolism, and all three nutrients should be optimized during pregnancy for best outcomes. Despite these critical roles, choline is not included in most prenatal vitamin formulations, making dietary sources and targeted supplementation especially important for pregnant women.
5. Methylation and Homocysteine Regulation
Choline participates in one-carbon metabolism through its oxidation to betaine (trimethylglycine) in the liver and kidneys. Betaine serves as an alternative methyl donor in the conversion of homocysteine to methionine, a reaction catalyzed by the enzyme betaine-homocysteine methyltransferase (BHMT). This pathway operates in parallel with the folate-dependent remethylation pathway, providing a crucial backup system for homocysteine detoxification.
Elevated homocysteine is an independent risk factor for cardiovascular disease, stroke, cognitive decline, and neural tube defects. When folate or vitamin B12 intake is inadequate, the choline-betaine pathway becomes the primary means of homocysteine disposal. Studies have shown that individuals with low choline intake and low folate intake simultaneously have dramatically elevated homocysteine levels and increased risk of cardiovascular events. Conversely, supplementation with choline or betaine can significantly reduce plasma homocysteine concentrations.
The methylation reactions supported by choline extend far beyond homocysteine regulation. Methyl groups derived from choline-betaine are used for DNA methylation (a primary mechanism of epigenetic gene regulation), the synthesis of creatine (which accounts for the largest single use of methyl groups in the body), the production of phosphatidylcholine via the PEMT pathway, and the methylation of neurotransmitters and hormones. Inadequate choline intake can therefore produce widespread disturbances in epigenetic regulation, energy metabolism, and endocrine function.
6. Muscle Function and Athletic Performance
Choline's role as the precursor to acetylcholine gives it direct relevance to muscle function and exercise performance. Acetylcholine is the neurotransmitter released at neuromuscular junctions to trigger muscle fiber contraction. During prolonged or intense exercise, plasma choline levels can decline by 40% or more as choline is consumed to sustain acetylcholine production at heavily recruited neuromuscular junctions.
Studies of marathon runners, triathletes, and endurance athletes have documented significant drops in plasma choline during prolonged exercise, falling from normal levels of approximately 10 micromoles per liter to levels below 6 micromoles per liter. These depleted choline levels have been correlated with impaired exercise performance, increased fatigue, and delayed recovery. Supplementation with choline before or during prolonged exercise has been shown to maintain plasma choline levels and, in some studies, improve endurance performance and reduce perceived exertion.
Beyond the neuromuscular junction, choline supports muscle function through its role in cell membrane integrity and cellular energy metabolism. Phosphatidylcholine in muscle cell membranes undergoes significant turnover during exercise-induced mechanical stress, and adequate choline availability is necessary for membrane repair and maintenance. Choline also contributes to mitochondrial function in muscle cells through its role in producing trimethylglycine, which supports mitochondrial membrane integrity and oxidative phosphorylation.
7. Cardiovascular Health
Choline's cardiovascular effects are multifaceted and include both protective mechanisms and considerations that warrant attention. On the protective side, choline's role in reducing homocysteine through the betaine pathway provides direct cardiovascular benefit, as elevated homocysteine is associated with endothelial dysfunction, accelerated atherosclerosis, and increased thrombotic risk. Epidemiological studies have found that individuals with higher choline intake have lower risk of coronary heart disease events.
Choline also supports cardiovascular health through its essential role in lipid transport. As a component of VLDL, phosphatidylcholine is necessary for the proper export of triglycerides from the liver to peripheral tissues. Choline deficiency leads to hepatic triglyceride accumulation and can contribute to dyslipidemia, both of which increase cardiovascular risk. Adequate choline intake helps maintain healthy lipid profiles and prevents the downstream metabolic consequences of impaired hepatic fat export.
However, an important nuance has emerged regarding choline metabolism and cardiovascular risk. Certain gut bacteria can convert choline into trimethylamine (TMA), which is subsequently oxidized in the liver to trimethylamine N-oxide (TMAO). Elevated TMAO levels have been associated with increased risk of atherosclerosis and cardiovascular events in some observational studies. Importantly, this conversion is heavily influenced by gut microbiome composition, and individuals with healthy, diverse gut flora may produce less TMAO from dietary choline. Consuming probiotics and fermented foods to support a healthy microbiome may help optimize choline metabolism and minimize TMAO production.
8. Mental Health and Mood Regulation
The cholinergic system plays a significant but often underappreciated role in mood regulation, emotional processing, and psychiatric health. Acetylcholine modulates the activity of other neurotransmitter systems including serotonin, dopamine, and norepinephrine, all of which are central to mood and emotional well-being. Disruptions in cholinergic signaling have been implicated in depression, anxiety, and bipolar disorder.
Clinical research has explored the use of choline and its derivatives in mood disorders with promising results. CDP-choline (citicoline), a form of choline that also provides cytidine, has been studied for its antidepressant-augmenting effects. A randomized controlled trial found that adding CDP-choline to standard antidepressant therapy improved treatment response in patients with major depressive disorder who had not responded adequately to medication alone. The proposed mechanism involves CDP-choline's ability to enhance dopamine receptor density and improve dopaminergic neurotransmission in the frontal cortex.
Choline's role in methylation also connects it to mental health through epigenetic mechanisms. Methyl groups derived from choline are used for the methylation of DNA and histones, processes that regulate the expression of genes involved in stress response, neurotransmitter synthesis, and neuroplasticity. Inadequate choline intake during critical developmental periods may alter the epigenetic programming of stress-response systems, potentially increasing vulnerability to anxiety and mood disorders later in life.
9. Dietary Sources of Choline
The richest dietary sources of choline are animal-derived foods, with eggs standing out as the single best source. A single large egg yolk contains approximately 147 mg of choline, primarily in the form of phosphatidylcholine. This makes eggs one of the most efficient and affordable ways to meet daily choline needs. Other excellent animal sources include beef liver (356 mg per 3 oz serving), salmon (187 mg per serving), chicken breast (72 mg per serving), and dairy products.
Plant-based sources of choline tend to provide lower amounts per serving but can still make meaningful contributions to total intake. Soybeans and soy-based products are among the richest plant sources, with one cup of cooked soybeans providing approximately 107 mg of choline. Cruciferous vegetables such as broccoli (63 mg per cup cooked) and Brussels sprouts are moderate sources. Quinoa, almonds, lentils, and peanuts also contribute to dietary choline intake.
The adequate intake (AI) for choline is 550 mg per day for adult men and 425 mg per day for adult women, rising to 450 mg during pregnancy and 550 mg during lactation. Meeting these targets through diet alone requires deliberate food choices, particularly for individuals who avoid eggs or organ meats. Vegetarians and vegans are at especially high risk of choline deficiency and may benefit from targeted supplementation or strategic food planning to ensure adequate intake.
10. Deficiency Signs and Risk Factors
Choline deficiency can manifest through a range of symptoms affecting the liver, brain, muscles, and metabolism. The earliest clinical sign is typically fatty liver (hepatic steatosis), which may be asymptomatic initially but can be detected through liver imaging or elevated liver enzymes on blood tests. As deficiency progresses, symptoms may include muscle damage (elevated creatine kinase), cognitive impairment (poor memory, difficulty concentrating), fatigue, and mood disturbances.
Several populations are at elevated risk of choline deficiency. Pregnant and lactating women have dramatically increased choline demands that are rarely met through standard dietary advice. Postmenopausal women lose the estrogen-mediated stimulation of the PEMT enzyme, which normally allows the liver to synthesize some choline endogenously, making dietary intake even more critical. Vegetarians and vegans face challenges due to the relatively low choline content of most plant foods. Athletes engaged in prolonged endurance exercise may deplete choline stores faster than they can be replenished from diet.
Genetic factors also play a significant role in choline requirements. Approximately 40-45% of the population carries common polymorphisms in the MTHFR, PEMT, or CHDH genes that increase dietary choline requirements by impairing endogenous synthesis or increasing metabolic demand. Individuals with these variants may develop deficiency symptoms even at intake levels that would be adequate for the general population. Genetic testing for these polymorphisms can help identify individuals who may benefit from higher choline intake or supplementation.
11. Supplementation Forms and Dosing
Several forms of choline supplements are available, each with distinct characteristics and applications:
- Choline bitartrate: The most affordable and widely available form. Provides approximately 41% choline by weight. Suitable for general choline supplementation to support liver health and meet baseline requirements. Typical dosing is 500-1000 mg daily.
- CDP-choline (citicoline): A form that provides both choline and cytidine (which converts to uridine in the body). Particularly valued for cognitive enhancement and neuroprotection. Clinical studies have used doses of 250-1000 mg daily. Citicoline has been shown to improve memory, attention, and processing speed in aging adults and may enhance the effects of other nootropic compounds.
- Alpha-GPC (alpha-glycerophosphocholine): A highly bioavailable form that crosses the blood-brain barrier efficiently. Preferred for cognitive support and as a growth hormone secretagogue. Typical dosing for cognitive enhancement is 300-600 mg daily. Alpha-GPC has shown particular promise in age-related cognitive decline and is used clinically in some European countries for dementia support.
- Phosphatidylcholine (lecithin): Provides choline in the same form found naturally in cell membranes and food. Often derived from soy or sunflower. Preferred for liver support and lipid metabolism. Dosing typically ranges from 1200-2400 mg of lecithin daily, providing approximately 150-300 mg of choline.
When choosing a choline supplement, the intended purpose should guide the selection. For general health and liver support, choline bitartrate or phosphatidylcholine are cost-effective choices. For cognitive enhancement, CDP-choline or Alpha-GPC offer superior brain bioavailability. All forms are generally well-tolerated, though high doses may cause gastrointestinal discomfort, fishy body odor, or excessive sweating in some individuals.
12. Cautions and Interactions
- Upper intake level: The tolerable upper intake level for choline is 3,500 mg per day for adults. Exceeding this level may cause fishy body odor, sweating, gastrointestinal distress, hypotension, and liver toxicity. These effects are rare at standard supplemental doses.
- TMAO concerns: As discussed in the cardiovascular section, gut bacteria can convert choline to trimethylamine, which is oxidized to TMAO in the liver. While the clinical significance of TMAO remains debated, individuals with known cardiovascular disease may wish to discuss choline supplementation with their healthcare provider and focus on supporting a healthy gut microbiome.
- Drug interactions: Choline supplements may interact with anticholinergic medications (commonly prescribed for overactive bladder, allergies, and Parkinson's disease) by opposing their pharmacological effects. Cholinesterase inhibitors used for Alzheimer's disease may have enhanced effects when combined with choline supplementation.
- Genetic considerations: Individuals with trimethylaminuria (TMAU), a genetic condition affecting TMA metabolism, should limit choline intake as it exacerbates the characteristic fishy body odor associated with the condition.
- Pregnancy: While higher choline intake during pregnancy is generally beneficial, pregnant women should discuss supplementation with their healthcare provider, particularly if taking prenatal vitamins that may already contain some choline.
Connections
- Anxiety
- Vitamin B12
- Alzheimer's Disease
- Eggs
- Salmon
- Non-Alcoholic Fatty Liver Disease
- Depression
- Bipolar Disorder
- Vitamin B9
- Homocysteine
- Probiotics
- Methionine
- Cardiovascular Disease
- Creatine
- Liver Cleansing
- Lentils
- Beef
- Organ Meats