Omega-3 Fatty Acids
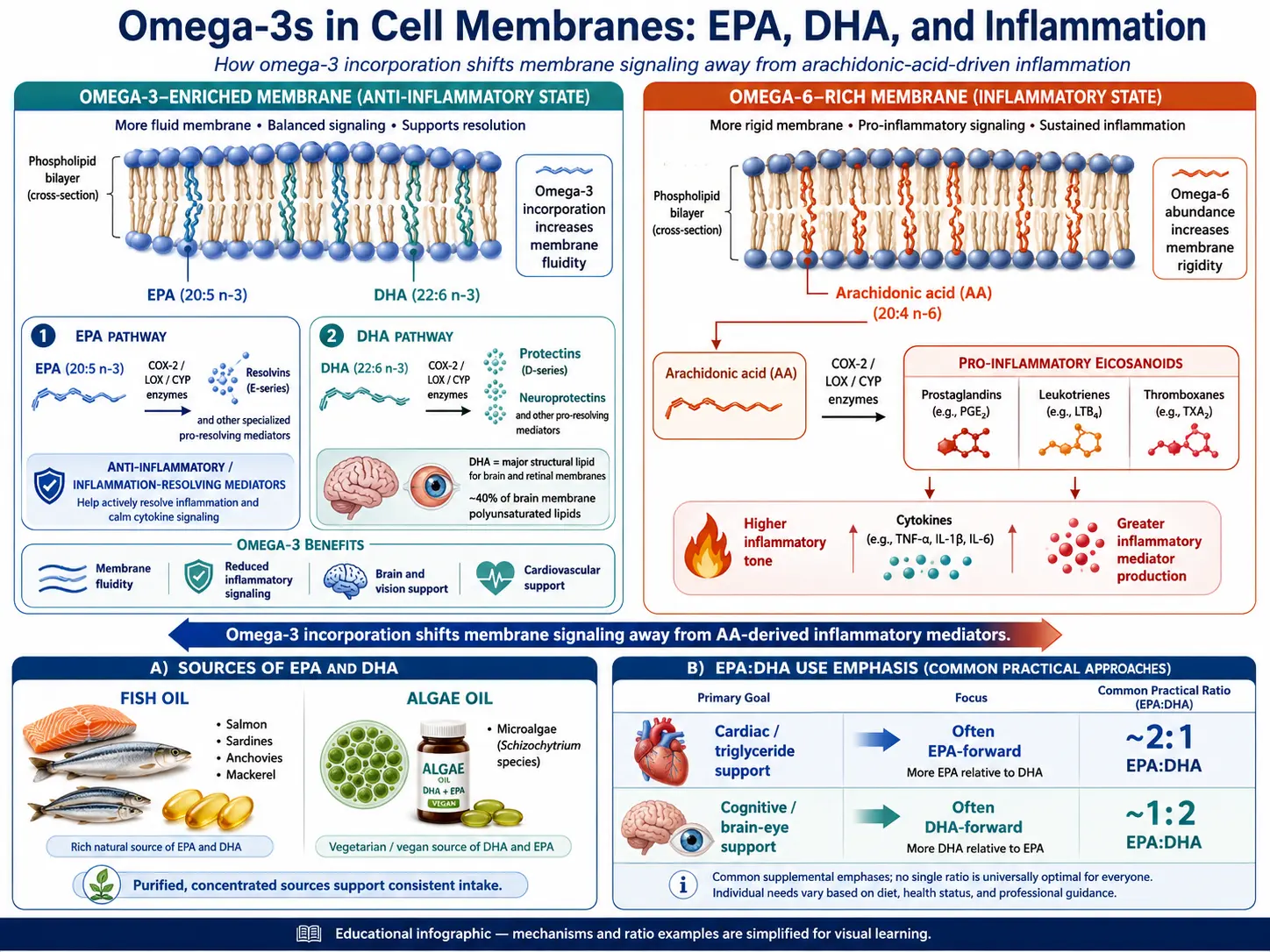
Table of Contents
- Introduction
- The Three Types: ALA, EPA, and DHA
- Brain Health and Cognitive Function
- Cardiovascular Health
- Anti-Inflammatory Mechanisms
- Joint Health and Arthritis
- Mental Health: Depression, Anxiety, and ADHD
- Eye Health and Vision
- Pregnancy and Fetal Brain Development
- Omega-3 to Omega-6 Ratio
- Food Sources
- Fish Oil vs Krill Oil vs Algae Oil Supplements
- Mercury and Heavy Metal Concerns
- Recommended Daily Intake
- Cautions and Contraindications
- Research Papers
- Connections
- Featured Videos
Introduction
Omega-3 fatty acids are among the most extensively researched and therapeutically significant nutrients in naturopathic medicine. These essential polyunsaturated fatty acids cannot be synthesized by the human body in adequate quantities and must therefore be obtained through diet or supplementation. As a naturopathic doctor, I consider omega-3 fatty acids to be foundational to nearly every treatment protocol I develop, given their profound influence on inflammation, neurological function, cardiovascular health, and cellular integrity.
The modern Western diet has created a widespread deficiency in omega-3 fatty acids while simultaneously flooding the body with pro-inflammatory omega-6 fatty acids. This imbalance is at the root of many chronic diseases that plague our society, including heart disease, autoimmune conditions, neurodegenerative disorders, and mood disturbances. Understanding omega-3 fatty acids, their distinct forms, and their therapeutic applications is essential for anyone seeking to optimize their health through evidence-based natural medicine.
Throughout human evolution, our ancestors consumed a diet rich in omega-3 fatty acids from wild game, fish, seeds, and leafy greens. The ratio of omega-6 to omega-3 in ancestral diets is estimated to have been approximately 1:1 to 4:1. Today, the average Western diet has shifted this ratio to an alarming 15:1 or even 20:1, driving chronic systemic inflammation and contributing to the epidemic of inflammatory diseases we observe in clinical practice.
The Three Types: ALA, EPA, and DHA
There are three principal forms of omega-3 fatty acids, each with distinct biochemical roles and dietary sources. Understanding the differences between these forms is critical for making informed choices about diet and supplementation.
Alpha-Linolenic Acid (ALA)
ALA is an 18-carbon omega-3 fatty acid found primarily in plant-based foods. It is considered the parent omega-3 because the body can theoretically convert it into the longer-chain forms, EPA and DHA. However, this conversion is extremely inefficient in humans, with studies suggesting that only about 5 to 10 percent of ALA is converted to EPA, and less than 1 to 5 percent is converted to DHA. ALA serves primarily as an energy source and has some independent anti-inflammatory properties. Rich sources include flaxseed, chia seeds, hemp seeds, and walnuts.
Eicosapentaenoic Acid (EPA)
EPA is a 20-carbon long-chain omega-3 fatty acid that plays a central role in the body's anti-inflammatory pathways. It serves as a precursor to series-3 prostaglandins and series-5 leukotrienes, which are potent anti-inflammatory mediators. EPA competes with arachidonic acid (an omega-6 fatty acid) for the same enzymatic pathways, effectively reducing the production of pro-inflammatory eicosanoids. EPA is particularly valued in naturopathic practice for its cardiovascular and mood-regulating benefits. It is found predominantly in fatty fish and marine sources.
Docosahexaenoic Acid (DHA)
DHA is a 22-carbon long-chain omega-3 fatty acid that is the most structurally significant omega-3 in the human body. It is a major structural component of the brain, cerebral cortex, retina, and cellular membranes throughout the body. DHA constitutes approximately 40 percent of the polyunsaturated fatty acids in the brain and approximately 60 percent of those in the retina. Its unique molecular structure provides the fluidity and flexibility that neuronal membranes require for rapid signal transmission. DHA is found primarily in fatty fish, fish oil, and algae-based supplements.
Brain Health and Cognitive Function
The relationship between DHA and brain health is one of the most compelling areas of omega-3 research. DHA constitutes approximately 40 percent of all polyunsaturated fatty acids in the brain, making it the single most abundant omega-3 in neural tissue. This concentration is not incidental; DHA is structurally essential for the formation and maintenance of neuronal membranes, synaptic connections, and myelin sheaths.
The brain is approximately 60 percent fat by dry weight, and the quality of dietary fat directly influences the composition and function of brain cell membranes. When DHA is abundant, neuronal membranes become more fluid and flexible, facilitating faster neurotransmitter signaling, improved receptor sensitivity, and more efficient communication between brain cells. Conversely, when DHA is deficient, the body substitutes other fatty acids into neural membranes, resulting in less optimal structure and impaired signaling.
Research has demonstrated that adequate DHA intake supports multiple aspects of cognitive function, including memory formation and retrieval, learning capacity, attention and focus, processing speed, and executive function. In aging populations, higher omega-3 levels are associated with reduced rates of cognitive decline, lower risk of Alzheimer's disease, and better preservation of brain volume over time. Neuroimaging studies have shown that individuals with higher omega-3 blood levels tend to have larger hippocampal volumes, the brain region most critical for memory.
From a naturopathic perspective, I emphasize DHA supplementation for patients experiencing brain fog, difficulty concentrating, memory complaints, or those with a family history of neurodegenerative disease. DHA also supports neuroplasticity, the brain's ability to form new neural connections and adapt to new information, making it valuable at every stage of life from infancy through old age.
Cardiovascular Health
Omega-3 fatty acids, particularly EPA and DHA, exert profound protective effects on the cardiovascular system through multiple mechanisms. The cardiovascular benefits of omega-3s are among the most extensively studied and well-established in nutritional medicine.
Triglyceride Reduction
One of the most consistent and dose-dependent effects of omega-3 supplementation is the reduction of serum triglycerides. High-dose EPA and DHA (2 to 4 grams per day) can reduce triglyceride levels by 25 to 45 percent. This effect occurs through multiple pathways: omega-3s decrease hepatic synthesis of very-low-density lipoprotein (VLDL), increase fatty acid beta-oxidation, and reduce lipogenesis in the liver. For patients with hypertriglyceridemia, omega-3 supplementation is one of the most effective natural interventions available.
Blood Pressure Regulation
Omega-3 fatty acids promote vasodilation by enhancing the production of nitric oxide, a potent vasodilator, in the endothelial lining of blood vessels. Meta-analyses have demonstrated that omega-3 supplementation can reduce systolic blood pressure by approximately 2 to 5 mmHg and diastolic blood pressure by 1 to 3 mmHg. While these reductions may appear modest, even small decreases in blood pressure at the population level significantly reduce the risk of stroke and heart attack.
Anti-Inflammatory and Anti-Atherogenic Effects
Chronic inflammation is a driving force behind atherosclerosis, the formation of arterial plaques that underlies most cardiovascular events. Omega-3 fatty acids reduce the expression of inflammatory cytokines, adhesion molecules, and chemokines that promote plaque formation. They also stabilize existing plaques, making them less likely to rupture and cause acute events such as heart attacks or strokes. EPA and DHA reduce the production of platelet-activating factor and thromboxane A2, thereby decreasing platelet aggregation and reducing the risk of thrombotic events.
Heart Rhythm Stabilization
Omega-3 fatty acids have antiarrhythmic properties, meaning they help stabilize the electrical activity of the heart. They modulate ion channels in cardiac cell membranes, particularly sodium and calcium channels, reducing the susceptibility to dangerous cardiac arrhythmias. This mechanism is one reason why populations with high fish consumption, such as the Japanese and Greenland Inuit, have historically exhibited lower rates of sudden cardiac death.
Anti-Inflammatory Mechanisms
The anti-inflammatory properties of omega-3 fatty acids represent one of their most therapeutically valuable attributes. Understanding these mechanisms is essential for naturopathic practitioners who seek to address the root cause of chronic disease rather than merely suppressing symptoms.
EPA and DHA serve as precursors to a class of specialized pro-resolving mediators (SPMs) known as resolvins, protectins, and maresins. These lipid mediators are fundamentally different from conventional anti-inflammatory agents because they do not simply suppress the inflammatory response; instead, they actively promote its resolution. This distinction is critical because unresolved inflammation is the hallmark of chronic disease.
Resolvins
Resolvins are derived from both EPA (E-series resolvins) and DHA (D-series resolvins). They actively signal immune cells to cease the inflammatory response, promote the clearance of cellular debris and apoptotic cells, and restore tissue homeostasis. Resolvin E1, derived from EPA, has been shown to be extraordinarily potent, with anti-inflammatory activity at nanomolar concentrations that exceeds many pharmaceutical anti-inflammatory agents.
Protectins
Protectin D1, also known as neuroprotectin D1 when produced in neural tissue, is derived from DHA and has demonstrated remarkable neuroprotective and anti-inflammatory properties. It protects neurons from oxidative stress-induced apoptosis, reduces the infiltration of inflammatory cells into damaged tissues, and promotes the survival of retinal pigment epithelial cells. In the brain, neuroprotectin D1 has been shown to reduce the neurotoxicity of amyloid-beta peptides, the pathological proteins associated with Alzheimer's disease.
Maresins
Maresins, derived from DHA by macrophages, promote the resolution of inflammation and tissue regeneration. Maresin 1 enhances the phagocytic activity of macrophages, helping them clear dead cells and debris from inflamed tissues, while simultaneously reducing the production of pro-inflammatory cytokines. This dual action makes maresins particularly important in wound healing and tissue repair.
Beyond SPM production, omega-3 fatty acids reduce inflammation through additional mechanisms. They decrease the activity of nuclear factor kappa-B (NF-kB), a master transcription factor that controls the expression of hundreds of inflammatory genes. They also reduce the production of pro-inflammatory cytokines including interleukin-1 (IL-1), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-alpha).
Joint Health and Arthritis
Omega-3 fatty acids have demonstrated significant therapeutic value in the management of inflammatory joint conditions, particularly rheumatoid arthritis and osteoarthritis. As a naturopathic doctor, I frequently incorporate omega-3 supplementation into treatment plans for patients with joint pain and stiffness.
In rheumatoid arthritis, the immune system mistakenly attacks the synovial membranes lining the joints, causing chronic inflammation, pain, swelling, and progressive joint destruction. Omega-3 fatty acids, particularly EPA, compete with arachidonic acid for incorporation into immune cell membranes. When immune cells contain more EPA and less arachidonic acid, they produce fewer pro-inflammatory eicosanoids such as prostaglandin E2 and leukotriene B4, which are key mediators of joint inflammation and pain.
Multiple randomized controlled trials have demonstrated that omega-3 supplementation in doses of 3 to 6 grams of combined EPA and DHA per day can significantly reduce morning stiffness, the number of tender and swollen joints, pain severity, and the need for nonsteroidal anti-inflammatory drugs (NSAIDs) in rheumatoid arthritis patients. Some studies have shown that patients are able to reduce or discontinue NSAID use after several months of consistent omega-3 supplementation.
In osteoarthritis, while the pathology is primarily degenerative rather than autoimmune, inflammation still plays a significant role in symptom progression. Omega-3 fatty acids have been shown to reduce the production of cartilage-degrading enzymes (matrix metalloproteinases) and inflammatory mediators within osteoarthritic joints. Animal studies have demonstrated that omega-3 supplementation can reduce the progression of cartilage degradation, and human trials suggest improvements in pain and function.
For optimal joint health outcomes, I recommend sustained supplementation over a minimum of 8 to 12 weeks, as the anti-inflammatory effects of omega-3s build gradually as they are incorporated into cell membranes throughout the body.
Mental Health: Depression, Anxiety, and ADHD
The connection between omega-3 fatty acids and mental health has become one of the most active and promising areas of nutritional psychiatry. Epidemiological studies consistently show that populations with higher fish consumption have lower rates of depression, and individuals with depression tend to have lower blood levels of omega-3 fatty acids compared to non-depressed controls.
Depression
EPA appears to be the more therapeutically relevant omega-3 for the treatment of depression. Meta-analyses of randomized controlled trials have shown that supplements containing a higher proportion of EPA to DHA (at least 60 percent EPA) are more effective for depressive symptoms than DHA-predominant formulations. The proposed mechanisms include EPA's ability to reduce neuroinflammation, modulate the hypothalamic-pituitary-adrenal (HPA) axis stress response, enhance serotonin transmission by improving receptor sensitivity, and support the integrity of neural membranes. Doses of 1 to 2 grams of EPA per day have shown the most consistent antidepressant effects in clinical trials.
Anxiety
While the evidence for omega-3s in anxiety disorders is less extensive than for depression, several studies have demonstrated beneficial effects. A notable study in medical students found that omega-3 supplementation (2.5 grams per day) reduced anxiety symptoms by 20 percent compared to placebo, along with measurable reductions in pro-inflammatory cytokines. Omega-3s may reduce anxiety through their anti-inflammatory effects on the brain, their modulation of the stress response, and their ability to improve the fluidity of neuronal membranes involved in emotional regulation.
Attention Deficit Hyperactivity Disorder (ADHD)
Children and adults with ADHD frequently exhibit lower blood levels of omega-3 fatty acids compared to those without the condition. Multiple meta-analyses have shown that omega-3 supplementation, particularly combinations of EPA and DHA, can produce modest but statistically significant improvements in ADHD symptoms including inattention, hyperactivity, and impulsivity. While omega-3s are not a replacement for comprehensive ADHD management, they represent a safe and beneficial adjunctive therapy. In my practice, I recommend omega-3 supplementation as a foundational intervention for all patients with ADHD, alongside dietary modifications and other naturopathic strategies.
Eye Health and Vision
DHA is the predominant structural fatty acid in the retina, constituting approximately 60 percent of all polyunsaturated fatty acids in this critical tissue. The photoreceptor cells of the retina have the highest concentration of DHA of any cell type in the body, reflecting the essential role this fatty acid plays in visual function.
DHA contributes to the fluidity and flexibility of photoreceptor cell membranes, which must undergo rapid conformational changes during the process of phototransduction, the conversion of light signals into electrical impulses that the brain interprets as vision. Adequate DHA levels support optimal visual acuity, contrast sensitivity, and the speed of visual processing.
Age-related macular degeneration (AMD) is the leading cause of vision loss in older adults, and omega-3 fatty acids have been extensively studied for their potential to prevent or slow its progression. Epidemiological studies consistently show that higher dietary intake of omega-3 fatty acids, particularly from fatty fish, is associated with a reduced risk of developing AMD. The anti-inflammatory and antioxidant properties of DHA and its derivative neuroprotectin D1 help protect retinal cells from the oxidative damage and chronic inflammation that drive AMD progression.
Dry eye syndrome is another common condition that responds favorably to omega-3 supplementation. Omega-3 fatty acids improve the lipid composition of the meibomian gland secretions that form the outer oily layer of the tear film, reducing tear evaporation. They also decrease inflammation of the lacrimal glands and ocular surface. Studies have shown that omega-3 supplementation can significantly improve symptoms of dry eye, including irritation, burning, and blurred vision, with benefits typically appearing after 6 to 12 weeks of consistent supplementation.
Pregnancy and Fetal Brain Development
Omega-3 fatty acids, particularly DHA, are critically important during pregnancy and lactation for optimal fetal and infant neurodevelopment. The developing brain undergoes its most rapid period of growth during the third trimester and the first two years of life, and DHA is required in substantial quantities during this period to support neuronal membrane formation, synaptogenesis, and myelination.
During the third trimester, the fetus accumulates approximately 50 to 70 milligrams of DHA per day, drawing primarily from maternal stores. This transfer can significantly deplete maternal DHA levels, particularly in women who do not consume adequate omega-3s through diet or supplementation. Maternal DHA depletion has been associated with increased risk of postpartum depression and suboptimal cognitive development in offspring.
Research has demonstrated that adequate maternal DHA intake during pregnancy is associated with improved infant cognitive development and higher scores on tests of visual acuity and processing, longer gestational duration and reduced risk of preterm birth, higher birth weight, reduced risk of postpartum depression in mothers, and improved problem-solving abilities and attention in early childhood.
Major health organizations recommend that pregnant and lactating women consume at least 200 to 300 milligrams of DHA per day, though many naturopathic practitioners, including myself, recommend higher intakes of 500 to 1,000 milligrams of combined EPA and DHA. Women who do not regularly consume fatty fish should strongly consider a high-quality fish oil or algae-based DHA supplement during pregnancy and breastfeeding.
It is worth noting that the developing fetal brain preferentially incorporates DHA over other fatty acids, and no other fatty acid can substitute for DHA in this role. This makes adequate maternal omega-3 intake during pregnancy not merely beneficial but genuinely essential for optimal fetal neurodevelopment.
Omega-3 to Omega-6 Ratio
One of the most significant nutritional imbalances in the modern diet is the dramatic skewing of the omega-6 to omega-3 ratio. Both omega-6 and omega-3 fatty acids are essential, meaning the body cannot produce them and must obtain them from food. However, these two families of fatty acids have opposing effects on inflammation, and the ratio between them profoundly influences the body's inflammatory status.
Omega-6 fatty acids, particularly arachidonic acid, serve as precursors to pro-inflammatory eicosanoids including prostaglandin E2, thromboxane A2, and leukotriene B4. While these inflammatory mediators are necessary for acute immune responses, their chronic overproduction drives the pathology of numerous diseases. Omega-3 fatty acids, by contrast, produce anti-inflammatory and pro-resolving mediators that counterbalance this inflammatory signaling.
Anthropological and evolutionary evidence suggests that humans evolved on a diet with an omega-6 to omega-3 ratio of approximately 1:1 to 4:1. However, the modern Western diet, dominated by processed seed oils (soybean, corn, safflower, sunflower), grain-fed animal products, and processed foods, has shifted this ratio to approximately 15:1 to 20:1, and in some individuals even higher. This dramatic imbalance creates a pro-inflammatory biochemical environment that promotes chronic disease.
Restoring a healthier omega-6 to omega-3 ratio requires a dual approach: increasing omega-3 intake through fatty fish, high-quality supplements, and omega-3 rich plant foods, while simultaneously reducing omega-6 intake by minimizing the consumption of processed seed oils, fried foods, and conventionally raised animal products. In my clinical practice, I aim to help patients achieve a ratio of no greater than 4:1, with an ideal target closer to 2:1.
Specific dietary changes that improve this ratio include replacing soybean and corn oils with olive oil, avocado oil, or coconut oil for cooking; choosing grass-fed and pasture-raised animal products over grain-fed; consuming fatty fish two to three times per week; incorporating flaxseed, chia seeds, and walnuts into the daily diet; and dramatically reducing intake of processed and fast foods.
Food Sources
Obtaining omega-3 fatty acids from whole food sources is always the preferred approach in naturopathic medicine, as foods provide these essential fats in their natural matrix along with synergistic cofactors. The following are the most significant dietary sources of omega-3 fatty acids.
Wild-Caught Fatty Fish (EPA and DHA)
Fatty cold-water fish are the most concentrated dietary sources of the long-chain omega-3s EPA and DHA. The following species are particularly rich sources:
- Wild-caught salmon - Contains approximately 1,500 to 2,000 mg of combined EPA and DHA per 3.5-ounce serving. Sockeye and king salmon are the richest varieties. Always choose wild-caught over farmed salmon, as wild fish have a more favorable omega-3 to omega-6 ratio and lower contaminant levels.
- Sardines - An excellent and often overlooked source, providing approximately 1,400 mg of EPA and DHA per 3.5-ounce serving. Sardines are small, short-lived fish that accumulate very low levels of mercury and other heavy metals, making them one of the safest fish to consume regularly.
- Atlantic mackerel - Provides approximately 1,300 mg of EPA and DHA per serving. Choose Atlantic mackerel over king mackerel, which is a larger species that accumulates more mercury.
- Herring - Another small fatty fish rich in omega-3s, providing approximately 1,700 mg per serving with low mercury levels.
- Anchovies - Contain approximately 1,400 mg per serving and are among the lowest mercury fish available.
Cod Liver Oil
Cod liver oil has been used as a traditional health tonic for centuries and remains one of the most nutrient-dense omega-3 sources available. In addition to EPA and DHA, it naturally contains vitamins A and D in their bioavailable forms. A single tablespoon provides approximately 2,600 mg of combined omega-3s. I recommend cod liver oil from reputable brands that test for heavy metals and use molecular distillation to ensure purity.
Plant-Based Sources (ALA)
- Flaxseed and flaxseed oil - The richest plant source of ALA, with one tablespoon of ground flaxseed providing approximately 1,600 mg of ALA. Flaxseed should be ground before consumption, as whole seeds pass through the digestive tract undigested.
- Chia seeds - Contain approximately 5,000 mg of ALA per ounce (about 2 tablespoons) and also provide fiber, protein, and minerals.
- Walnuts - One ounce (approximately 14 halves) provides about 2,500 mg of ALA, along with beneficial polyphenols and antioxidants.
- Hemp seeds - Provide approximately 1,000 mg of ALA per tablespoon, with a favorable omega-6 to omega-3 ratio of approximately 3:1.
Algae Oil (DHA and EPA)
Algae oil is the original source of omega-3 DHA in the marine food chain, as fish obtain their DHA by consuming algae or organisms that feed on algae. Algae-based supplements provide a direct source of preformed DHA and some EPA, making them the optimal omega-3 source for vegetarians, vegans, and individuals who prefer to avoid fish products entirely. High-quality algae oil supplements typically provide 400 to 500 mg of DHA per serving.
Fish Oil vs Krill Oil vs Algae Oil Supplements
Choosing the right omega-3 supplement can be confusing given the variety of options available. Each type has distinct characteristics, advantages, and considerations.
Fish Oil
Fish oil is the most widely used and extensively studied omega-3 supplement. It is available in two primary forms: natural triglyceride form and ethyl ester form. The triglyceride form has superior bioavailability, with studies showing approximately 50 percent better absorption compared to ethyl esters. High-quality fish oil supplements should be molecularly distilled to remove mercury, PCBs, and other contaminants, and should be tested by independent third-party laboratories for purity. Fish oil typically provides both EPA and DHA in varying ratios. Concentrated fish oils can provide 600 to 1,000 mg of combined EPA and DHA per softgel, making it easier to achieve therapeutic doses.
Krill Oil
Krill oil is derived from Antarctic krill, small crustaceans that are near the bottom of the marine food chain. Its primary advantage is that the omega-3s in krill oil are bound to phospholipids rather than triglycerides, which may enhance their absorption and incorporation into cell membranes. Krill oil also naturally contains astaxanthin, a powerful antioxidant that gives it its red color and helps protect the oil from oxidation. However, krill oil supplements typically contain lower total amounts of EPA and DHA per capsule (approximately 150 to 300 mg combined) compared to concentrated fish oil, meaning more capsules may be needed to achieve therapeutic doses. Krill oil is also generally more expensive per milligram of omega-3.
Algae Oil
Algae oil supplements are derived from microalgae cultivated in controlled environments, free from ocean-borne contaminants. They are the only plant-based source of preformed DHA and EPA, making them essential for vegans and vegetarians. Modern algae oil supplements can provide 400 to 500 mg of DHA per serving, with some newer formulations also offering meaningful amounts of EPA. Algae oil is inherently free from mercury and other heavy metals because it is produced in controlled aquaculture facilities. From a sustainability perspective, algae oil bypasses the marine food chain entirely, reducing pressure on ocean fish populations.
In my practice, I recommend high-quality, third-party tested fish oil in triglyceride form for most patients, algae oil for vegans and vegetarians, and krill oil for patients who prefer a phospholipid-bound form or who benefit from the additional astaxanthin content.
Mercury and Heavy Metal Concerns
One of the most common concerns patients raise about increasing their fish intake is the potential for mercury and heavy metal exposure. This is a legitimate concern that warrants careful consideration and a balanced approach.
Mercury, particularly methylmercury, is a potent neurotoxin that accumulates in the aquatic food chain through a process called bioaccumulation. Large, long-lived predatory fish at the top of the food chain, such as shark, swordfish, king mackerel, tilefish, and bigeye tuna, accumulate the highest levels of mercury and should be consumed rarely or avoided entirely, particularly by pregnant women, nursing mothers, and young children.
However, it is essential to recognize that the fish species richest in omega-3 fatty acids tend to be small, short-lived species that accumulate very low levels of mercury. Sardines, anchovies, herring, and wild-caught salmon are all excellent omega-3 sources with minimal mercury contamination. The health benefits of consuming these low-mercury, omega-3 rich fish far outweigh the risks of trace contaminant exposure.
For those who prefer supplementation, reputable fish oil manufacturers use molecular distillation and other purification processes that effectively remove mercury, PCBs, dioxins, and other contaminants. High-quality fish oil supplements typically contain mercury levels far below detectable limits. Look for brands that provide Certificates of Analysis from independent third-party testing organizations such as the International Fish Oil Standards (IFOS) program or NSF International.
Additional strategies for minimizing heavy metal exposure while maximizing omega-3 intake include choosing wild-caught over farmed fish when possible, rotating fish species rather than consuming the same type repeatedly, supporting the body's natural detoxification pathways with adequate intake of selenium, zinc, and sulfur-containing amino acids, and considering algae-based omega-3 supplements as a completely contaminant-free alternative.
Recommended Daily Intake
Recommended daily intake of omega-3 fatty acids varies depending on the individual's health status, therapeutic goals, and the specific form of omega-3 being considered.
General Health Maintenance
For the general adult population seeking to maintain overall health, most expert bodies recommend a minimum intake of 250 to 500 mg of combined EPA and DHA per day. This can be achieved by consuming two to three servings of fatty fish per week or by taking a daily omega-3 supplement. The American Heart Association recommends at least two servings of fatty fish per week for cardiovascular health maintenance.
Therapeutic Doses for Specific Conditions
- Cardiovascular health and triglyceride reduction: 2,000 to 4,000 mg of combined EPA and DHA per day, under medical supervision.
- Depression and mood disorders: 1,000 to 2,000 mg of EPA per day, with EPA-predominant formulations (at least 60 percent EPA).
- Rheumatoid arthritis and inflammatory joint conditions: 3,000 to 6,000 mg of combined EPA and DHA per day.
- ADHD: 1,000 to 2,000 mg of combined EPA and DHA per day.
- Pregnancy and lactation: At least 300 mg of DHA per day, with many practitioners recommending 500 to 1,000 mg of combined EPA and DHA.
- Dry eye syndrome: 1,000 to 2,000 mg of combined EPA and DHA per day.
- Cognitive support in aging: 1,000 to 2,000 mg of combined EPA and DHA per day, with emphasis on DHA.
ALA Intake
The adequate intake for ALA is 1.1 grams per day for women and 1.6 grams per day for men. However, because conversion of ALA to EPA and DHA is so limited, plant-based ALA should be considered supplementary to, rather than a replacement for, preformed EPA and DHA from marine sources or algae-based supplements.
When initiating omega-3 supplementation, I advise patients to start at a moderate dose and increase gradually over 1 to 2 weeks to minimize any gastrointestinal side effects. Taking omega-3 supplements with meals that contain some fat significantly improves absorption. Dividing the daily dose into two servings (morning and evening) can also enhance absorption and tolerability.
Cautions and Contraindications
While omega-3 fatty acids are generally very safe and well-tolerated, there are important cautions that must be considered, particularly at higher therapeutic doses.
Blood Thinning Effects
Omega-3 fatty acids have mild antiplatelet and anticoagulant properties, meaning they can slightly reduce the blood's tendency to clot. At standard supplemental doses (up to 2 grams per day of combined EPA and DHA), this effect is generally considered beneficial for cardiovascular health. However, at higher doses, omega-3s may potentiate the effects of anticoagulant medications such as warfarin (Coumadin), heparin, and direct oral anticoagulants (DOACs), as well as antiplatelet drugs such as aspirin and clopidogrel (Plavix). Patients taking these medications should consult their healthcare provider before beginning high-dose omega-3 supplementation, and INR (International Normalized Ratio) should be monitored more closely when omega-3s are added to a warfarin regimen.
Surgical Considerations
Due to their mild anticoagulant effects, some surgeons recommend discontinuing high-dose omega-3 supplements 7 to 14 days before scheduled surgical procedures to minimize the theoretical risk of excessive bleeding. However, recent evidence suggests that standard omega-3 doses do not significantly increase surgical bleeding risk, and some progressive surgeons no longer require discontinuation. Patients should always discuss their supplement regimen with their surgical team prior to any procedure and follow their surgeon's specific recommendations.
Gastrointestinal Effects
The most common side effects of omega-3 supplementation are mild gastrointestinal complaints, including fishy aftertaste, burping, nausea, and loose stools. These can be minimized by taking supplements with meals, starting at a lower dose and increasing gradually, using enteric-coated capsules, refrigerating or freezing fish oil capsules before taking them, and choosing high-quality products that are fresh and not oxidized.
Oxidation and Rancidity
Omega-3 fatty acids are highly susceptible to oxidation due to their multiple double bonds. Consuming oxidized (rancid) fish oil may be counterproductive, as lipid peroxidation products can promote rather than reduce inflammation. Always check the expiration date on supplements, store them in a cool, dark place or in the refrigerator, and discard any product that has a strong, unpleasant fishy or paint-like odor, which indicates oxidation.
Vitamin A Toxicity with Cod Liver Oil
Cod liver oil contains preformed vitamin A (retinol), and excessive consumption can lead to vitamin A toxicity, particularly in pregnant women where excess vitamin A is teratogenic. Pregnant women should use regular fish oil or algae-based DHA supplements rather than cod liver oil, unless the dose of vitamin A has been carefully calculated to remain within safe limits.
Allergies
Individuals with fish or shellfish allergies should exercise caution with fish oil and krill oil supplements, respectively. While highly purified fish oils may contain negligible amounts of fish protein (the allergenic component), there is still a theoretical risk of allergic reaction. Algae-based omega-3 supplements are a safe alternative for individuals with fish or shellfish allergies.
Despite these cautions, omega-3 fatty acids remain among the safest and most broadly beneficial supplements available. The vast majority of individuals can supplement with omega-3s safely, and the benefits of addressing omega-3 deficiency far outweigh the risks for most people.
Research Papers
Selected peer-reviewed literature. Links resolve to PubMed or DOI.
- Bhatt DL, Steg PG, Miller M, et al. Cardiovascular risk reduction with icosapent ethyl for hypertriglyceridemia (REDUCE-IT). N Engl J Med. 2019;380(1):11-22.
- Manson JE, Cook NR, Lee IM, et al. Marine n-3 fatty acids and prevention of cardiovascular disease and cancer (VITAL). N Engl J Med. 2019;380(1):23-32.
- ASCEND Study Collaborative Group. Effects of n-3 fatty acid supplements in diabetes mellitus. N Engl J Med. 2018;379(16):1540-1550.
- Mozaffarian D, Wu JH. Omega-3 fatty acids and cardiovascular disease: effects on risk factors, molecular pathways, and clinical events. J Am Coll Cardiol. 2011;58(20):2047-2067.
- Harris WS, Pottala JV, Varvel SA, et al. Erythrocyte omega-3 fatty acids increase and linoleic acid decreases with age. Prostaglandins Leukot Essent Fatty Acids. 2013;88(4):257-263.
- Calder PC. n-3 polyunsaturated fatty acids, inflammation, and inflammatory diseases. Am J Clin Nutr. 2006;83(6 Suppl):1505S-1519S.
- Yurko-Mauro K, McCarthy D, Rom D, et al. Beneficial effects of docosahexaenoic acid on cognition in age-related cognitive decline. Alzheimers Dement. 2010;6(6):456-464.
- Freeman MP, Hibbeln JR, Wisner KL, et al. Omega-3 fatty acids: evidence basis for treatment and future research in psychiatry. J Clin Psychiatry. 2006;67(12):1954-1967.
- Lorente-Cebrian S, Costa AG, Navas-Carretero S, et al. Role of omega-3 fatty acids in obesity, metabolic syndrome, and cardiovascular diseases: a review of the evidence. J Physiol Biochem. 2013;69(3):633-651.
- PubMed — omega-3 EPA DHA cardiovascular meta-analysis search.
- PubMed — DHA brain cognition supplementation search.
Connections
- Depression
- Salmon
- Arthritis
- Cardiovascular Disease
- Alzheimer's Disease
- Herring
- Sardines
- Vitamin D3
- Organ Meats
- Anxiety
- ADHD
- Mercury
- Walnuts
- Chia Seeds
- Vitamin A
- Atherosclerosis
- Stroke
- Hypertension
Featured Videos

What IF You Took Omega 3 Fatty Acids for 30 Days? [Benefits & Foods]

The Benefits Of Fish Oil & Why You Need Omega-3 | Nutritionist Explains | Myprotein

Omega-3 Fatty Acids (7 Great Sources...) - 2026
A Guide To Omega 3 Fatty Acids

5 Science-Based Benefits of Omega-3 Fatty Acids

Omega 3 Fatty Acid for Depression

Omega 3 Fatty Acids - The True Nutrients

7 Best Sources of DHA/EPA: Essential Omega-3 Fatty Acids

Omega 3 Fatty acids | Mechanism of action and health benefits | Food source | Omega 3 Supplements

OMEGA 3 Secret (Save $$$ on Supplements) 2026

Omega-3 Fatty Acids (DHA, EPA): Pharmacology Made Easy

Top Omega 3 Foods for Your Low Carb Diet

Omega 3 Vegan Foods Tier List (BEST & WORST SOURCES)

Hypothyroid Supplements - The POWER of Omega 3 Fatty Acids!

Vegetarian Sources of Omega 3 Fatty Acids | Foods That Are High In Omega 3s | Plant based Omega 3s

The Fishy Dilemmas with Omega-3 Fatty Acids