ADHD (Attention-Deficit/Hyperactivity Disorder)
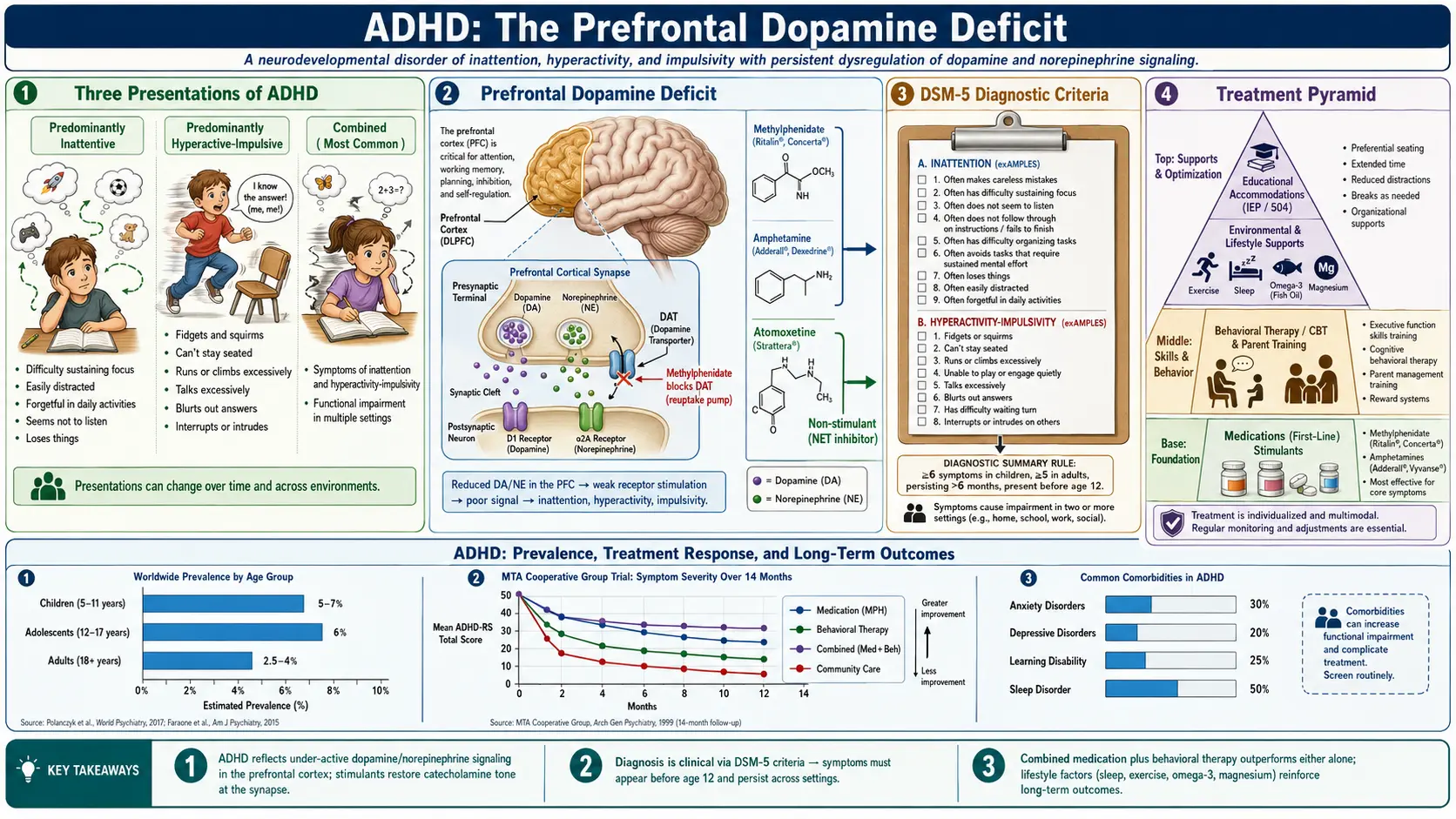
Table of Contents
- What is ADHD?
- Types of ADHD
- Symptoms of ADHD
- Causes and Risk Factors
- Diagnosis
- Treatment Options
- Prevention Strategies
- Complications of ADHD
- Research Papers
- Connections
- Featured Videos
What is ADHD?
ADHD is a neurodevelopmental disorder that affects children and often continues into adulthood. It is characterized by patterns of inattention, hyperactivity, and impulsivity that interfere with daily functioning and development.
Types of ADHD
1. Predominantly Inattentive Presentation
- Difficulty focusing on tasks and sustaining attention.
- Common symptoms include being easily distracted, forgetfulness, and difficulty organizing tasks.
2. Predominantly Hyperactive-Impulsive Presentation
- Hyperactivity: Fidgeting, excessive movement, and talking excessively.
- Impulsivity: Acting without thinking, interrupting others, or having difficulty waiting for their turn.
3. Combined Presentation
- Combination of inattention and hyperactivity-impulsivity: This is the most common type of ADHD.
Symptoms of ADHD
Symptoms can vary and may be more noticeable in some settings than others.
Inattention Symptoms
- Difficulty maintaining attention during tasks or play activities.
- Easily distracted by unrelated stimuli.
- Forgetfulness in daily activities.
- Difficulty organizing tasks and activities.
- Fails to follow through on instructions and does not complete tasks.
Hyperactivity and Impulsivity Symptoms
- Fidgeting or tapping hands and feet.
- Inability to stay seated when expected to do so.
- Excessive talking and difficulty engaging in quiet activities.
- Interrupts or intrudes on conversations or games.
- Impatience and difficulty waiting for a turn.
Causes and Risk Factors
- Genetics: ADHD often runs in families, suggesting a strong genetic link.
- Brain structure and function: Differences in brain regions responsible for attention and impulse control.
- Premature birth and low birth weight.
- Exposure to environmental toxins: Lead exposure or prenatal exposure to tobacco or alcohol.
Diagnosis
- Comprehensive evaluation: Conducted by a mental health professional or pediatrician based on behavior patterns and reported symptoms.
- Symptom criteria: Must meet the diagnostic criteria outlined in the DSM-5.
- Observation and reports: Feedback from parents, teachers, or other caregivers.
- Behavioral assessments: Standardized questionnaires and rating scales.
Treatment Options
- Medications:
- Stimulants: Such as methylphenidate (e.g., Ritalin) and amphetamines (e.g., Adderall). These are the most common and effective treatment for ADHD.
- Non-stimulants: Such as atomoxetine or guanfacine, used when stimulants are ineffective or cause side effects.
- Behavioral therapy:
- Parent training: Equips parents with strategies to manage their child’s behavior.
- Cognitive-behavioral therapy (CBT): Helps individuals develop better coping mechanisms and problem-solving skills.
- Educational support:
- Individualized Education Programs (IEP) or 504 plans can be set up in schools to provide accommodations.
- Lifestyle changes:
- Structured routines: Helps improve focus and organization.
- Regular physical activity: Exercise can help reduce symptoms by boosting brain function and overall mood.
- Balanced diet: Proper nutrition supports cognitive health.
Prevention Strategies
- Maintain a healthy pregnancy: Avoid exposure to tobacco, alcohol, and drugs during pregnancy.
- Early intervention: Identifying and addressing behavioral issues early can help manage symptoms.
Complications of ADHD
- Academic challenges: Difficulty focusing and following instructions can impact learning.
- Social difficulties: Impulsive behavior and difficulty in maintaining attention can lead to problems with relationships.
- Higher risk of accidents and injuries: Due to impulsivity and hyperactivity.
- Co-occurring conditions: Such as anxiety disorders, depression, and learning disabilities.
- Low self-esteem: Struggles in school and social settings can lead to feelings of inadequacy.
Research Papers
Historical Background
ADHD was first described in 1902 by British pediatrician Sir George Frederic Still, who identified a group of children with abnormal deficits in sustained attention and self-control. The condition was later termed "hyperkinetic reaction of childhood" in the DSM-II (1968) before evolving into the modern ADHD diagnosis in the DSM-III (1980) and subsequent revisions.
Key Research Papers
- Faraone SV, et al. The worldwide prevalence of ADHD: is it an American condition? World Psychiatry. 2003;2(2):104-113.
- Faraone SV, Biederman J, Mick E. The age-dependent decline of attention deficit hyperactivity disorder: a meta-analysis of follow-up studies. Psychological Medicine. 2006;36(2):159-165.
- MTA Cooperative Group. A 14-month randomized clinical trial of treatment strategies for attention-deficit/hyperactivity disorder (MTA Study). Archives of General Psychiatry. 1999;56(12):1073-1086.
- Jensen PS, et al. 3-year follow-up of the NIMH MTA study. Journal of the American Academy of Child & Adolescent Psychiatry. 2007;46(8):989-1002.
- Neale BM, et al. Meta-analysis of genome-wide association studies of attention-deficit/hyperactivity disorder. Journal of the American Academy of Child & Adolescent Psychiatry. 2010;49(9):906-920.
- Demontis D, et al. Discovery of the first genome-wide significant risk loci for attention deficit/hyperactivity disorder. Nature Genetics. 2019;51(1):63-75.
- Cortese S, et al. Cognitive training for attention-deficit/hyperactivity disorder: meta-analysis of clinical and neuropsychological outcomes. Journal of the American Academy of Child & Adolescent Psychiatry. 2015;54(3):164-174.
- Cortese S, et al. Comparative efficacy and tolerability of medications for attention-deficit hyperactivity disorder in children, adolescents, and adults: a systematic review and network meta-analysis. The Lancet Psychiatry. 2018;5(9):727-738.
- American Academy of Pediatrics. ADHD: clinical practice guideline for the diagnosis, evaluation, and treatment of ADHD in children and adolescents. Pediatrics. 2011;128(5):1007-1022.
- Faraone SV, et al. Attention-deficit/hyperactivity disorder. Nature Reviews Disease Primers. 2015;1:15020.
- Shaw P, et al. Attention-deficit/hyperactivity disorder is characterized by a delay in cortical maturation. Proceedings of the National Academy of Sciences. 2007;104(49):19649-19654.
- Kooij JJS, et al. Updated European Consensus Statement on diagnosis and treatment of adult ADHD. European Psychiatry. 2019;56:14-34.
PubMed Topic Searches
- PubMed: ADHD prevalence worldwide
- PubMed: ADHD stimulant treatment
- PubMed: ADHD genetics GWAS
- PubMed: ADHD adult diagnosis
- PubMed: ADHD comorbidity
- PubMed: ADHD CBT
- PubMed: ADHD dopamine
- PubMed: ADHD omega-3
- PubMed: ADHD sleep
- PubMed: ADHD neuroimaging
- PubMed: ADHD executive function
- PubMed: ADHD long-term outcomes
Connections
- Anxiety
- Depression
- Autism
- Insomnia
- Vitamin B6
- Magnesium
- Zinc
- Iron
- Omega-3 Fatty Acids
- Sleep Hygiene
- Stress Management
- Lead Poisoning
- Yellow 5 Tartrazine
- Red 40 Allura Red
- Bipolar Disorder
- PTSD
- Methylene Blue
- Pesticides