Osteoporosis
Deep-Dive Articles
The articles below expand this overview into DEXA, FRAX, specific medications, fracture prevention, and special populations. Written for patients, with real research citations.
DEXA Scan: T-score & Z-score
How DEXA measures bone density, what T-scores and Z-scores mean, trabecular bone score, and when to repeat.
FRAX & Treatment Thresholds
10-year fracture risk scoring, NOF/Endocrine Society thresholds for therapy, and how race/ethnicity modifiers fit.
Bisphosphonates
Oral vs IV bisphosphonates, dosing, drug holiday timing, jaw osteonecrosis and atypical femur fracture risks.
Denosumab, Romosozumab & Teriparatide
Anabolic vs antiresorptive therapy, ARCH/FRAME trials, rebound fractures after stopping denosumab, sequencing.
Calcium, Vitamin D & Protein
Daily targets, food-first vs supplements, vitamin D level goals, and the protein requirement for bone health.
Exercise for Bone Density
LIFTMOR trial, impact loading, balance training to prevent falls, and the exercises that actually build bone.
Postmenopausal Osteoporosis
Estrogen deficiency, hormone therapy's bone benefits, WHI reanalysis, and timing of therapy for bone health.
Secondary Osteoporosis
Hyperparathyroidism, hypogonadism, celiac disease, IBD, glucocorticoids, hyperthyroidism — what to screen for.
Fracture Prevention & Fall Risk
Home modifications, balance, medication reduction, hip protectors, and the post-fracture care gap.
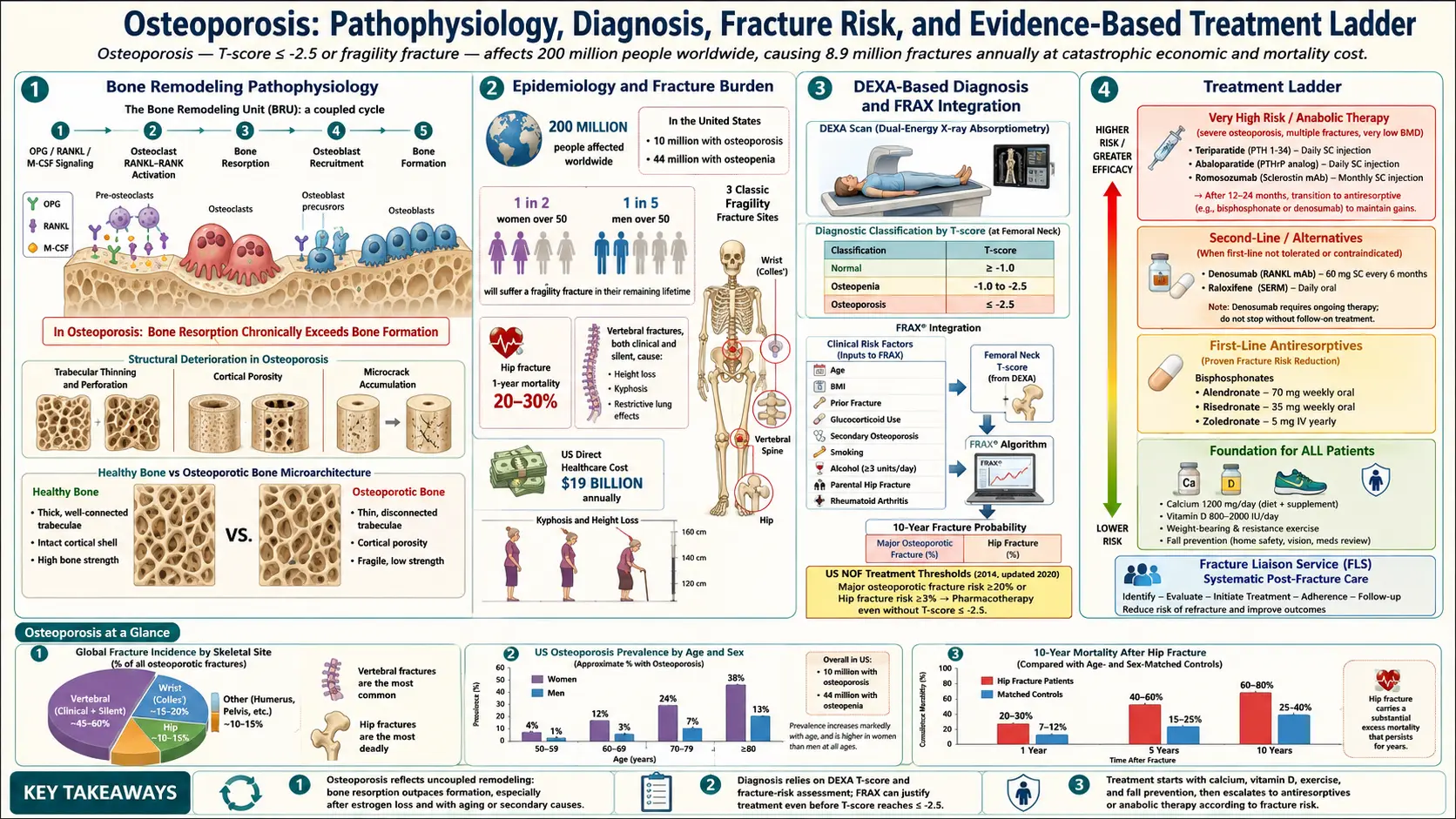
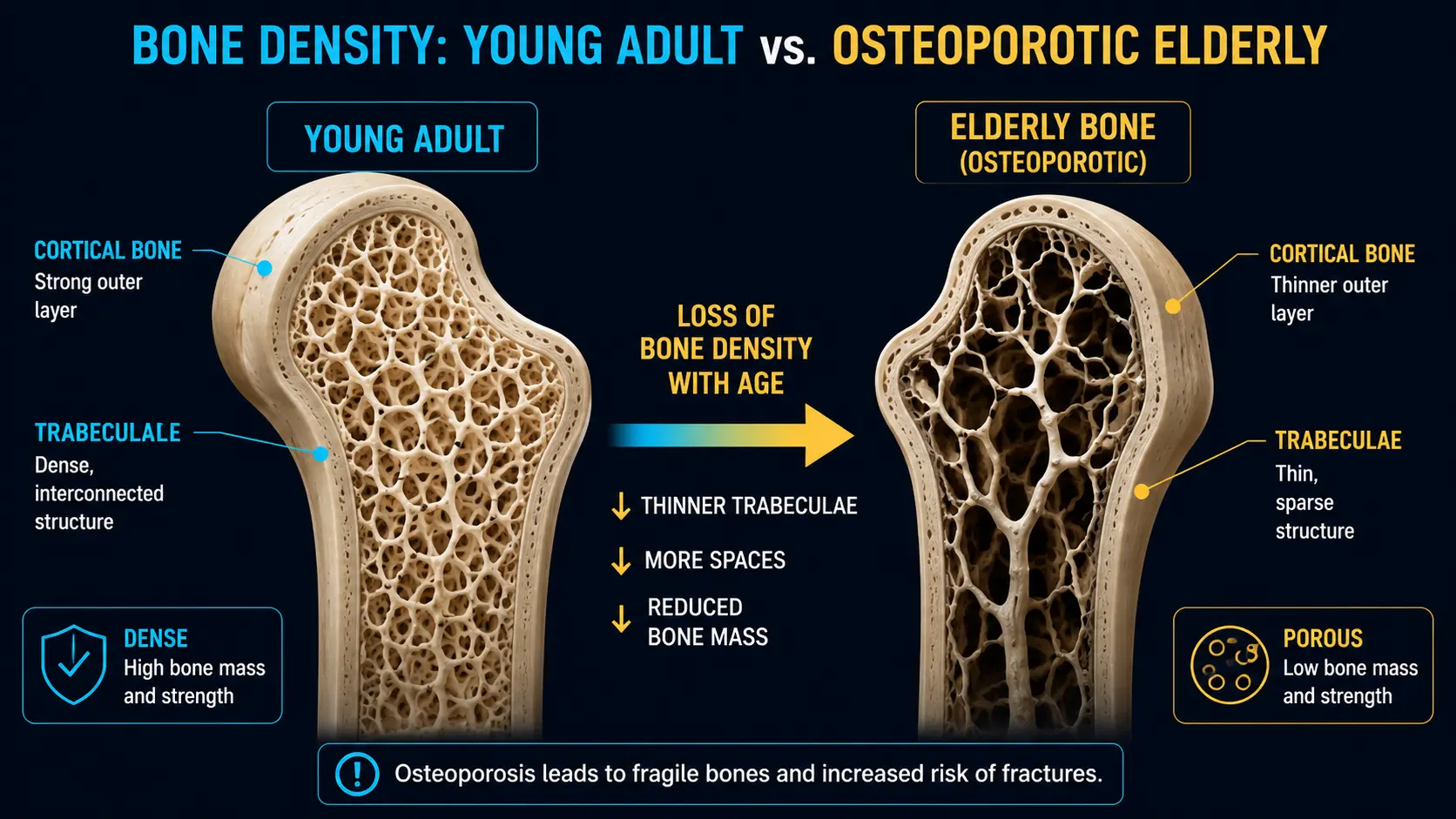
What is Osteoporosis?
Osteoporosis is a bone disease characterized by decreased bone density and strength, which makes bones more fragile and prone to fractures. It often progresses without symptoms until a fracture occurs.
Causes of Osteoporosis
- Bone remodeling imbalance: With age, the rate of bone breakdown exceeds the rate of new bone formation.
- Hormonal changes: Reduced estrogen levels in women (especially post-menopause) and testosterone levels in men contribute to bone loss.
- Calcium and vitamin D deficiency: Essential nutrients for bone health; low levels can accelerate bone loss.
- Genetics: Family history of osteoporosis increases risk.
- Medical conditions: Such as hyperthyroidism, celiac disease, and rheumatoid arthritis.
- Medications: Long-term use of corticosteroids and certain other drugs can weaken bones.
Risk Factors
- Age: Risk increases as you get older, especially after 50.
- Gender: Women are more likely to develop osteoporosis than men.
- Family history: Higher risk if a parent or sibling has osteoporosis.
- Body frame size: Smaller body frames have less bone mass to draw from as they age.
- Diet: Low intake of calcium and vitamin D contributes to bone loss.
- Lifestyle choices: Sedentary lifestyle, smoking, and excessive alcohol use increase risk.
Symptoms of Osteoporosis
Osteoporosis is often called a “silent disease” because bone loss occurs without symptoms. When symptoms do appear, they may include:
- Back pain: Caused by a fractured or collapsed vertebra.
- Loss of height over time
- Stooped posture
- Bone fractures: Occur more easily, especially in the hip, spine, or wrist.
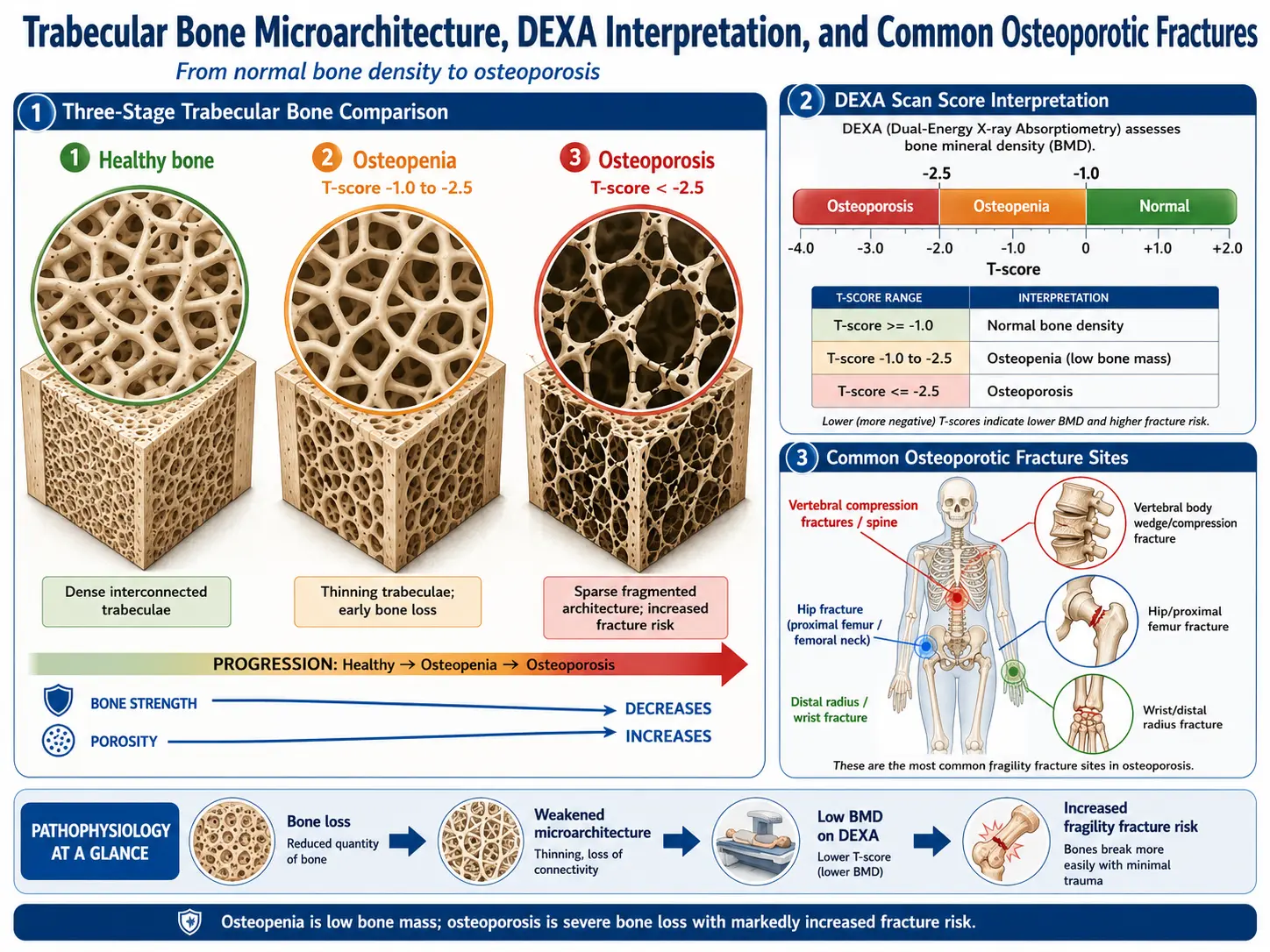
Diagnosis
- Bone density test (DEXA scan): The most common test to measure bone mineral density (BMD).
- Physical examination: Review of medical history and risk factors.
- Laboratory tests: To rule out other medical conditions that could cause bone loss.
Prevention Strategies
- Calcium-rich diet: Include dairy products, leafy greens, and fortified foods to maintain bone strength.
- Vitamin D intake: Sun exposure and foods like salmon and fortified milk help the body absorb calcium.
- Regular exercise: Weight-bearing and strength-training exercises can improve bone density.
- Avoid smoking: Smoking accelerates bone loss.
- Limit alcohol consumption: Excessive drinking can interfere with bone formation.
Treatment Options
- Medications:
- Bisphosphonates: Reduce bone loss and fracture risk (e.g., alendronate, risedronate).
- Monoclonal antibodies: Such as denosumab, which helps slow bone breakdown.
- Hormone-related therapy: Estrogen therapy can maintain bone density in postmenopausal women.
- Anabolic agents: Medications like teriparatide and abaloparatide that stimulate new bone formation.
- Calcium and vitamin D supplements: Ensure sufficient intake to support bone health.
- Lifestyle changes: Incorporating more physical activity and balanced nutrition into daily routines.
Complications of Osteoporosis
- Fractures: Most common and serious complication, especially in the hip and spine.
- Loss of mobility: Hip fractures can lead to reduced mobility and independence.
- Chronic pain: Can result from spinal fractures or bone damage.
- Height loss and spinal deformities: Fractures in the spine can lead to a curved or stooped posture.
- Increased risk of mortality: Especially after hip fractures in older adults.
Table of Contents
- What is Osteoporosis?
- Causes of Osteoporosis
- Deep-Dive Articles
- Risk Factors
- Symptoms of Osteoporosis
- Diagnosis
- Prevention Strategies
- Treatment Options
- Complications of Osteoporosis
- Research Papers
- Connections
- Featured Videos
Research Papers
Curated PubMed topic searches on Osteoporosis. Each link opens a live PubMed query so the result set stays current as new studies are indexed.
- PubMed topic search: Osteoporosis review
- PubMed topic search: DEXA bone density diagnosis
- PubMed topic search: Bisphosphonate osteoporosis trial
- PubMed topic search: Alendronate fracture prevention
- PubMed topic search: Denosumab osteoporosis
- PubMed topic search: Teriparatide osteoporosis
- PubMed topic search: Romosozumab fracture trial
- PubMed topic search: Vitamin D calcium bone density
- PubMed topic search: FRAX fracture risk assessment
- PubMed topic search: Postmenopausal osteoporosis
- PubMed topic search: Glucocorticoid-induced osteoporosis
- PubMed topic search: Magnesium bone density
Connections
- Bisphosphonates
- DEXA Scan: T-Score and Z-Score
- Calcium, Vitamin D and Protein Intake
- FRAX Risk Assessment
- Fracture Prevention and Fall Risk
- Secondary Osteoporosis Causes
- Denosumab, Romosozumab and Teriparatide
- Weight-Bearing and Resistance Exercise
- Postmenopausal Osteoporosis and Hormone Therapy
- Prunes (Bone Health)
- Prunes for Bone Health
- Calcium
- Magnesium
- Vitamin D3
- Vitamin K
- Arthritis
- Menopause and HRT
- Celiac Disease
- Hyperparathyroidism
- Kidney Disease
- Osteoarthritis
- Rheumatoid Arthritis