Fibromyalgia
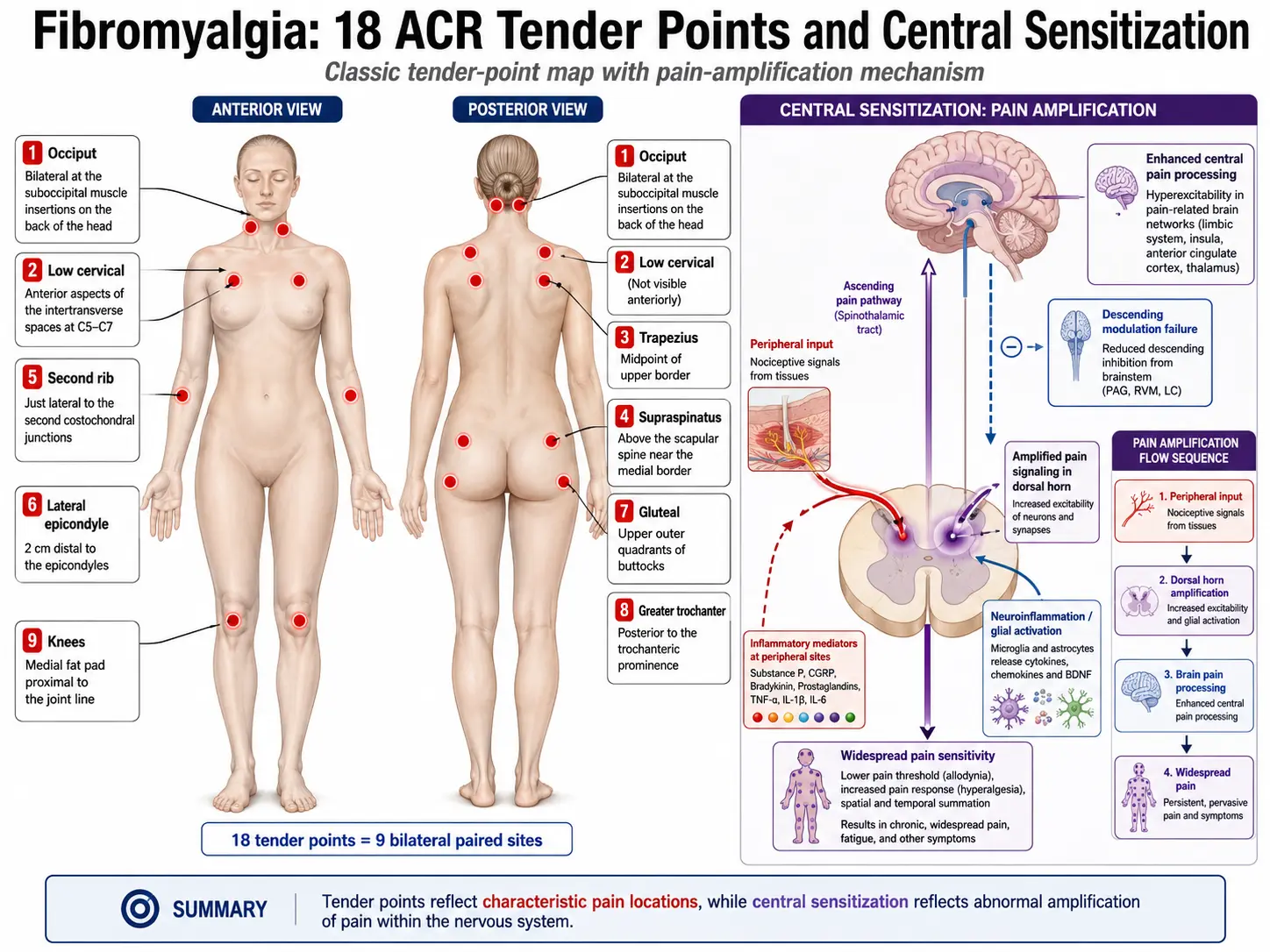
Table of Contents
- What is Fibromyalgia?
- Tender Points and Modern Diagnostic Criteria
- Central Sensitization Mechanism
- Symptoms Beyond Pain
- Common Comorbidities
- Conventional Treatment
- Lifestyle and Integrative Approaches
- Research Papers
- Connections
- Featured Videos
What is Fibromyalgia?
Fibromyalgia is a chronic widespread pain syndrome characterized by amplified pain signaling throughout the central nervous system. It is now recognized as a central sensitization disorder — a malfunction in how the brain and spinal cord process pain — rather than a primary muscle, joint, or autoimmune disease. Patients experience pain in regions where there is no detectable tissue damage, because the nervous system itself has become hypersensitive.
Fibromyalgia affects approximately 2 to 4 percent of the general population, making it one of the most common chronic pain conditions in clinical medicine. It shows a strong female predominance, with women diagnosed roughly three times more often than men. Onset is most common between ages 30 and 55, though children, adolescents, and older adults can also develop the condition. Fibromyalgia frequently coexists with other chronic illnesses, and patients often report a triggering event — physical trauma, surgery, viral infection, severe psychological stress, or pregnancy — that preceded the onset of widespread pain.
Despite causing significant disability, fibromyalgia produces no visible inflammation, no tissue destruction, and no abnormal lab markers on standard testing. This combination historically led to the condition being dismissed as psychosomatic, but modern neuroimaging, quantitative sensory testing, and functional MRI studies have produced clear, reproducible evidence of altered central nervous system pain processing.
Tender Points and Modern Diagnostic Criteria
The diagnosis of fibromyalgia has evolved substantially over the past three decades, moving away from a strict tender-point examination toward a symptom-based clinical assessment.
1990 ACR Tender Point Criteria (Historical)
The original 1990 American College of Rheumatology (ACR) criteria required:
- Widespread pain for at least 3 months, present in all four quadrants of the body and along the axial skeleton.
- Pain on palpation at at least 11 of 18 designated tender points when 4 kg of pressure was applied (about the force needed to blanch a fingernail bed).
The 18 tender points are bilateral and located at the occiput (suboccipital muscle insertions), low cervical (anterior intertransverse spaces of C5-C7), trapezius (midpoint of the upper border), supraspinatus (above the medial scapular spine), second rib (costochondral junction), lateral epicondyle (2 cm distal), gluteal (upper outer quadrant), greater trochanter (posterior to the trochanteric prominence), and medial knee (medial fat pad). The diagram on this page identifies all 18 sites.
While the tender-point exam is no longer the diagnostic gold standard, it remains a useful clinical sign and a teaching tool that helps patients visualize where their nervous system has become hypersensitive.
2016 ACR Revised Criteria (Current Standard)
Modern criteria abandon the tender-point count in favor of two patient-reported instruments. A diagnosis of fibromyalgia requires all three of the following:
- Widespread Pain Index (WPI) and Symptom Severity Score (SSS) meeting one of these thresholds:
- WPI ≥ 7 AND SSS ≥ 5, OR
- WPI of 4 to 6 AND SSS ≥ 9
- Generalized pain present in at least 4 of 5 body regions (upper left, upper right, lower left, lower right, axial).
- Symptoms present at a similar level for at least 3 months.
The Widespread Pain Index is a 0-to-19 count of body areas where the patient has experienced pain in the past week. The Symptom Severity Score rates fatigue, waking unrefreshed, and cognitive symptoms (each 0 to 3) plus a count of additional somatic symptoms (0 to 3), giving a 0-to-12 total. Importantly, the 2016 criteria explicitly state that fibromyalgia can be diagnosed independently of other coexisting conditions, and fibromyalgia does not exclude another rheumatologic or systemic diagnosis.
Central Sensitization Mechanism
Central sensitization is the core pathophysiology of fibromyalgia. In a healthy nervous system, peripheral pain signals are filtered, modulated, and dampened on their way to conscious awareness. In fibromyalgia, that filtering system breaks down, and ordinary sensory input is amplified into pain.
Amplified Pain Signaling in the Dorsal Horn
Pain fibers from the body synapse first in the dorsal horn of the spinal cord. In fibromyalgia, repeated nociceptive input causes "wind-up" — second-order neurons in the dorsal horn become progressively more excitable, firing more strongly to the same input. NMDA receptors are recruited, glutamate release increases, and the threshold for pain transmission drops. Once this state is established, it tends to self-sustain even after the original trigger is gone.
Failure of Descending Modulation
The brain normally sends inhibitory signals down the spinal cord through the periaqueductal gray and rostral ventromedial medulla, using serotonin and norepinephrine as primary neurotransmitters to dampen incoming pain. Fibromyalgia patients show decreased levels of serotonin and norepinephrine in cerebrospinal fluid and reduced descending inhibition on quantitative sensory testing. This is the mechanistic basis for why SNRI medications (duloxetine, milnacipran) and tricyclic antidepressants (amitriptyline) work in fibromyalgia — they restore descending inhibition.
Elevated Excitatory Neurotransmitters
CSF studies consistently show that fibromyalgia patients have 2 to 3 times higher levels of substance P and elevated glutamate compared with healthy controls. Substance P is a pain-amplifying neuropeptide; glutamate is the primary excitatory neurotransmitter. The combination drives the dorsal horn into a chronic, hyper-excitable state.
Low-Grade Neuroinflammation and Glial Activation
More recent research has identified microglial activation — the brain's resident immune cells switching into an inflammatory mode — as a driver of central sensitization. Activated microglia release pro-inflammatory cytokines (IL-1β, IL-6, TNF-α), prostaglandins, and reactive oxygen species, all of which sensitize neighboring neurons. This neuroinflammation model explains why anti-inflammatory strategies, low-dose naltrexone (which dampens microglial activation), and lifestyle interventions that reduce systemic inflammation often help fibromyalgia patients.
Altered Brain Connectivity
Functional MRI shows that fibromyalgia patients have increased connectivity between the default mode network and the insula (a key pain-processing region). Innocuous pressure that produces no pain in healthy controls activates pain centers in fibromyalgia brains. The condition is, mechanistically, a brain disorder of pain interpretation.
Symptoms Beyond Pain
Although widespread pain is the defining feature, fibromyalgia is a multi-system illness. Most patients experience a constellation of symptoms that often impair daily life as much as the pain itself.
- Chronic fatigue: persistent, profound exhaustion not relieved by rest. For many patients, fatigue is more disabling than pain. It often resembles the fatigue of ME/CFS.
- Fibro fog (cognitive dysfunction): difficulty concentrating, word-finding problems, short-term memory lapses, slowed processing speed, and trouble multitasking. Patients describe it as "brain in molasses." Fibro fog is now recognized as a core feature, not a side effect of pain.
- Non-restorative sleep: patients fall asleep but wake unrefreshed. Sleep studies show reduced deep (stage N3) sleep and intrusion of alpha-wave activity into delta-wave (deep) sleep — the so-called alpha-delta sleep anomaly.
- Morning stiffness: prolonged stiffness on waking, sometimes lasting hours, which improves with gentle movement.
- Headaches and migraines: tension-type headaches and migraines are several times more common than in the general population.
- Irritable bowel syndrome (IBS): alternating constipation and diarrhea, bloating, and abdominal pain are reported by 30 to 70 percent of fibromyalgia patients.
- Paresthesias: numbness, tingling, "pins and needles," or burning sensations, often in the hands and feet, without an identifiable peripheral nerve cause.
- Sensory hypersensitivity: heightened sensitivity to bright light, loud sounds, strong smells, and temperature extremes. Patients often describe being overwhelmed in stores, restaurants, or crowded spaces.
- Mood disturbance: depression and anxiety are roughly three to four times more common than in the general population. These are not the cause of fibromyalgia but reflect shared neurochemistry (serotonin, norepinephrine) and the burden of living with chronic pain.
- Autonomic symptoms: dizziness on standing, palpitations, temperature dysregulation, and dry eyes/mouth, often overlapping with POTS or Sjogren's syndrome.
Common Comorbidities
Up to 70 percent of fibromyalgia patients have at least one comorbid condition, and many have several overlapping syndromes. The pattern of comorbidities suggests shared underlying mechanisms involving central sensitization, autonomic dysfunction, mast cell activation, and connective tissue laxity.
- Irritable bowel syndrome (IBS): shares the same gut-brain hypersensitivity pattern. Up to 70 percent of fibromyalgia patients meet IBS criteria.
- Myalgic encephalomyelitis / chronic fatigue syndrome (ME/CFS): the overlap is so substantial that some researchers consider fibromyalgia and ME/CFS two presentations of a single underlying neuroimmune disorder.
- Postural orthostatic tachycardia syndrome (POTS): orthostatic intolerance is common; the dysautonomia that drives POTS may be part of the same neurological dysregulation.
- Mast cell activation syndrome (MCAS): many fibromyalgia patients have unexplained flushing, hives, food sensitivities, and chemical sensitivities consistent with mast cell involvement.
- Hypermobile Ehlers-Danlos syndrome (hEDS) and joint hypermobility spectrum disorder: connective tissue laxity is overrepresented in fibromyalgia, especially in the POTS/MCAS triad.
- Migraine and tension-type headache: roughly half of fibromyalgia patients have chronic headache.
- Restless legs syndrome (RLS): occurs at 3 to 4 times the population rate.
- Depression and anxiety disorders: lifetime prevalence approaches 60 to 70 percent.
- Autoimmune conditions: rheumatoid arthritis, lupus, Sjogren's syndrome, and Hashimoto's thyroiditis frequently coexist with fibromyalgia. Up to 30 percent of patients with these autoimmune diseases also meet fibromyalgia criteria.
- Interstitial cystitis / bladder pain syndrome and temporomandibular disorder (TMD): both share the central sensitization mechanism.
Recognizing these comorbidities matters because treating fibromyalgia in isolation, while ignoring an active POTS, MCAS, or autoimmune component, often fails. Effective care requires mapping the whole pattern.
Conventional Treatment
No single drug works for everyone with fibromyalgia, and most medications produce only modest improvement (typically 30 to 50 percent reduction in pain in responders). Combination therapy and individualized regimens are the rule.
FDA-Approved Medications
- Pregabalin (Lyrica): an alpha-2-delta calcium channel ligand that reduces glutamate release. Typical dose 150 to 450 mg/day in divided doses. Common side effects: sedation, dizziness, weight gain, peripheral edema.
- Duloxetine (Cymbalta): a serotonin-norepinephrine reuptake inhibitor (SNRI) that restores descending inhibition. Typical dose 30 to 60 mg/day. Common side effects: nausea, dry mouth, insomnia, sexual dysfunction. Must be tapered to discontinue.
- Milnacipran (Savella): a more norepinephrine-weighted SNRI. Typical dose 100 to 200 mg/day in divided doses. Often better tolerated than duloxetine for some patients.
Common Off-Label Medications
- Gabapentin (Neurontin): similar mechanism to pregabalin, often used because it is less expensive. Typical dose 900 to 2400 mg/day in divided doses.
- Amitriptyline: low-dose tricyclic (10 to 50 mg at bedtime) improves sleep architecture, reduces pain, and is one of the longest-studied fibromyalgia treatments.
- Cyclobenzaprine: a tricyclic-related muscle relaxant; low doses (5 to 10 mg at bedtime) help with sleep and morning stiffness.
- Low-dose naltrexone (LDN): 1.5 to 4.5 mg at bedtime. At these very low doses, naltrexone briefly blocks opioid receptors, triggering compensatory endorphin upregulation, and — mechanistically more important — binds toll-like receptor 4 to dampen microglial activation. Multiple controlled trials show meaningful pain and quality-of-life improvement with minimal side effects. LDN is increasingly considered a first-line option in integrative practice.
Medications to Avoid
- Opioids: strong evidence shows opioids do not work for fibromyalgia and may worsen central sensitization through opioid-induced hyperalgesia. Tramadol has weak SNRI activity and is sometimes used short-term, but stronger opioids should be avoided.
- NSAIDs as primary therapy: fibromyalgia is not an inflammatory condition in the joints or muscles, so NSAIDs typically provide little benefit while carrying GI, renal, and cardiovascular risks.
- Long-term benzodiazepines: tolerance develops quickly, sleep architecture worsens over time, and dependence becomes a problem.
Lifestyle and Integrative Approaches
The strongest evidence in fibromyalgia is for non-pharmacologic interventions. Multimodal programs that combine graded exercise, mind-body therapy, sleep optimization, and targeted supplementation typically outperform medication alone.
Graded Exercise (Start Very Low and Slow)
Exercise is the single most evidence-based treatment for fibromyalgia — but only when done correctly. Aggressive starts trigger flares and drive patients away. The rule is "start where you are and build in tiny increments." A patient who can walk 5 minutes without flaring should walk 5 minutes daily for two weeks before adding a single minute. Once a steady baseline is established, slow upward progress is sustainable.
- Aerobic exercise: walking, stationary cycling, and water aerobics are best tolerated. Target 30 minutes most days, built up over weeks to months.
- Tai chi: multiple randomized trials show tai chi outperforms aerobic exercise for fibromyalgia pain, fatigue, and quality of life.
- Yoga (especially restorative or gentle): improves pain, mood, and sleep.
- Strength training: light resistance work, started gently, improves function over months.
- Warm-water therapy: aquatic exercise in a heated pool (84 to 92°F) reduces gravitational load on tender tissue and produces significant pain reduction.
Cognitive Behavioral Therapy (CBT) and Mind-Body Approaches
CBT for chronic pain — not CBT for depression — targets pain catastrophizing, fear-avoidance behavior, and unhelpful coping patterns. Meta-analyses show clinically meaningful improvement in pain, function, and mood. Acceptance and commitment therapy (ACT), mindfulness-based stress reduction (MBSR), and pain reprocessing therapy show similar or superior results in some trials.
Sleep Hygiene
Restoring sleep architecture is essential because non-restorative sleep both reflects and worsens central sensitization. Strategies:
- Strict consistent sleep and wake times, even on weekends.
- Cool, dark, quiet bedroom; no screens in the hour before bed.
- Limit caffeine after noon and alcohol within 4 hours of bedtime.
- Treat coexisting sleep apnea (often missed in fibromyalgia patients).
- Low-dose amitriptyline, cyclobenzaprine, or trazodone if behavioral approaches alone are insufficient.
Targeted Supplementation
- Magnesium glycinate: 200 to 400 mg at bedtime. Magnesium is a natural NMDA receptor antagonist and muscle relaxant; deficiency is common. The glycinate form is well absorbed and gentle on the gut.
- Vitamin D: optimize serum 25(OH)D to 40 to 60 ng/mL. Multiple studies link low vitamin D to worse fibromyalgia pain, and supplementation in deficient patients improves symptoms.
- S-Adenosylmethionine (SAMe): 800 to 1600 mg/day in divided doses. Has antidepressant and anti-inflammatory effects; small trials show fibromyalgia benefit.
- Acetyl-L-carnitine: 1 to 2 g/day. Supports mitochondrial energy production; some randomized data show fatigue and pain improvement.
- Coenzyme Q10 (CoQ10): 200 to 400 mg/day of ubiquinol. Several trials show reduced pain and fatigue, likely via mitochondrial support and reduced oxidative stress.
- B-complex and methylated folate: support neurotransmitter synthesis; useful when methylation defects (MTHFR variants) are present.
Pacing and Energy Management
"Spoon theory" and energy pacing teach patients to budget activity in advance rather than push through and crash. The principle: do less than you think you can on good days, so you don't pay for it for three days afterward. Heart rate monitoring (staying below an individualized anaerobic threshold) and activity logging help patients identify their personal envelope.
Local Therapies
- Trigger-point injection or dry needling: temporary relief of focal pain.
- Myofascial release and gentle massage: many patients benefit from skilled bodywork delivered with the lightest possible pressure.
- Heat (warm baths, heating pads): helpful for stiffness and muscle pain.
- Transcutaneous electrical nerve stimulation (TENS): small but consistent benefit in trials.
Diet and Inflammation
While there is no single "fibromyalgia diet," reducing systemic inflammation through a Mediterranean-style or anti-inflammatory pattern — rich in vegetables, fruits, fish, olive oil, nuts, and limited in ultra-processed food and refined sugar — consistently improves pain and mood scores in trials. A subset of patients also benefit from gluten-free, low-FODMAP, or low-histamine eating, especially when MCAS or IBS overlap is present.
Research Papers
The following PubMed topic searches return current peer-reviewed literature relevant to this condition. Each link opens a live PubMed query.
- Fibromyalgia central sensitization
- Fibromyalgia ACR 2016 criteria
- Fibromyalgia pregabalin duloxetine milnacipran
- Low-dose naltrexone fibromyalgia
- Fibromyalgia exercise tai chi
- Fibromyalgia cognitive behavioral therapy
- Fibromyalgia magnesium
- Fibromyalgia vitamin D
- Fibromyalgia ME/CFS overlap
- Fibromyalgia neuroinflammation
- Fibromyalgia small fiber neuropathy
- Fibromyalgia sleep architecture
Connections
- Fibromyalgia (Orthopedics)
- Low-Dose Naltrexone for Fibromyalgia
- Central Sensitization Explained
- Exercise Pacing and Graded Movement
- Arthritis
- Lupus
- Gout
- Osteoporosis
- Ehlers-Danlos Syndrome
- POTS
- MCAS
- Chronic Pain
- Insomnia
- Anxiety
- Depression
- Low Dose Naltrexone
- Anti-Inflammatory Diet
- Sleep Hygiene