Chronic Pain
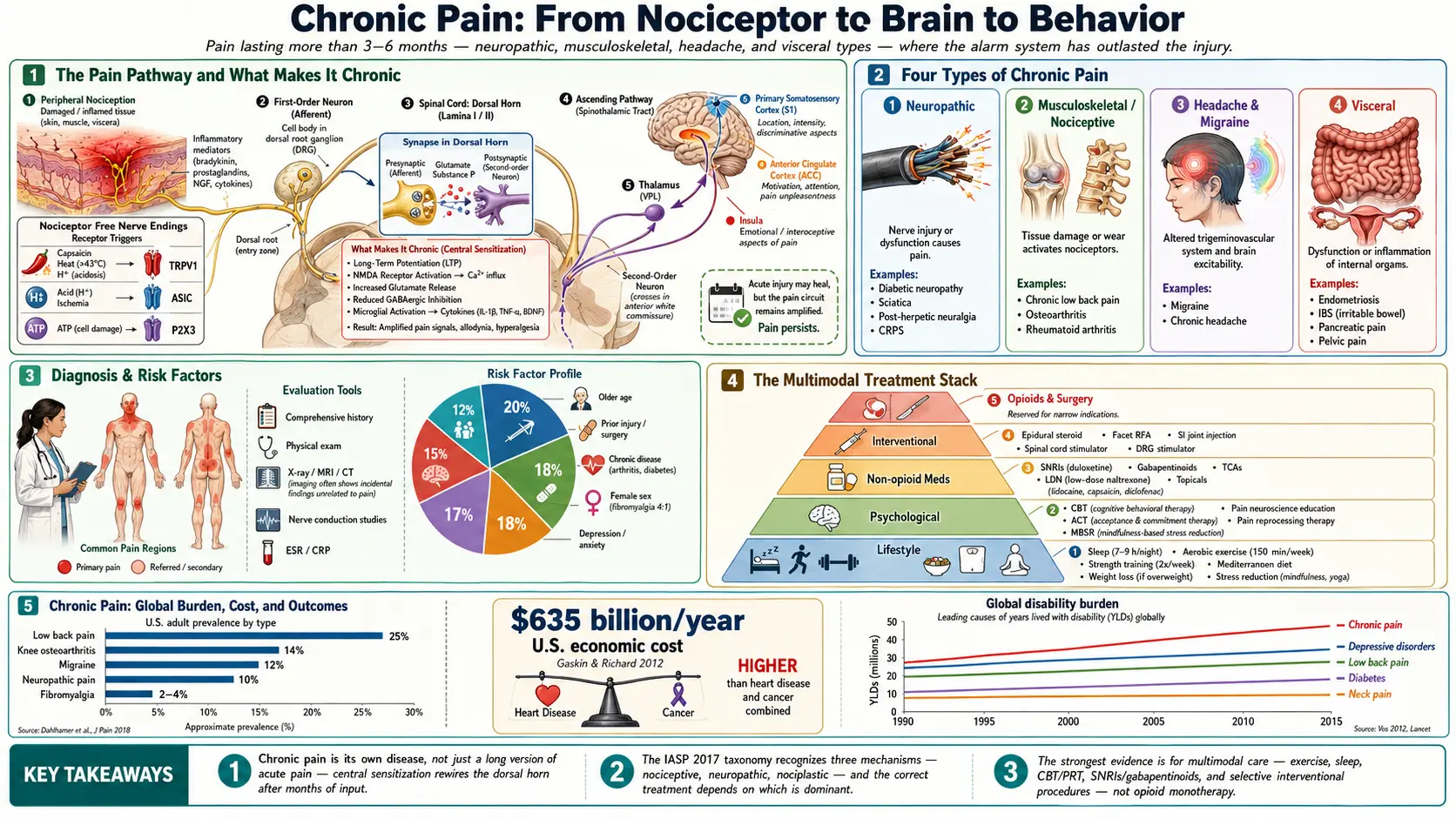
Table of Contents
- Deep-Dive Articles
- What is Chronic Pain?
- Causes of Chronic Pain
- Types of Chronic Pain
- Symptoms of Chronic Pain
- Risk Factors
- Diagnosis
- Treatment Options
- Prevention Strategies
- Complications of Chronic Pain
- Research Papers
- Connections
- References & Research
- Featured Videos
Deep-Dive Articles
The articles below go deeper into pain mechanisms, specific conditions, medication classes, interventional options, and the mind-body side of chronic pain. Written for patients, with real research citations.
Pain Mechanisms Explained
Nociceptive, neuropathic, and nociplastic pain — why mechanism matters for treatment, IASP 2017 taxonomy.
Central Sensitization
Wind-up, allodynia, hyperalgesia, and how the nervous system amplifies pain in fibromyalgia and ME/CFS.
CRPS (RSD)
Budapest criteria, early mobilization, sympathetic blocks, spinal cord stim, and why CRPS isn't "all in your head."
Chronic Low Back Pain
Imaging red flags, why MRIs mislead, ACP guidelines on exercise and CBT, role of injections and surgery.
Opioids for Chronic Pain
CDC 2022 revision, MME thresholds, buprenorphine for chronic pain, risk mitigation, tapering protocols.
Non-Opioid Medications
Gabapentin, pregabalin, duloxetine, amitriptyline, low-dose naltrexone — matching drug to pain mechanism.
Interventional Pain
Epidural steroids, medial branch blocks + radiofrequency ablation, spinal cord stimulators, dorsal root ganglion stim.
Pain Reprocessing & PNE
Boulder Back Pain Study, pain neuroscience education, fear-avoidance, and the mind-body pathway.
Sleep, Exercise & Lifestyle
Why poor sleep amplifies pain, graded movement, anti-inflammatory diet, and the 80/20 rule for pacing.
What is Chronic Pain?
Chronic pain is pain that lasts for more than 3 to 6 months or beyond the normal healing time of an injury. It can persist even after the initial cause is resolved and may affect various parts of the body, impacting a person’s physical and mental health.
Causes of Chronic Pain
- Injuries: Previous injuries or trauma can lead to long-lasting pain, even after the injury has healed.
- Medical conditions: Such as arthritis, fibromyalgia, endometriosis, and migraines.
- Nerve damage: Neuropathic pain can result from nerve injury or damage.
- Surgeries: Post-surgical pain can become chronic in some cases.
- Inflammatory conditions: Diseases like rheumatoid arthritis can lead to chronic pain.
Types of Chronic Pain
1. Neuropathic Pain
- Caused by nerve damage or dysfunction.
- Common examples: Diabetic neuropathy, sciatica, and shingles.
2. Musculoskeletal Pain
- Related to the muscles, bones, and joints.
- Common examples: Lower back pain, arthritis pain.
3. Headaches and Migraines
- Chronic headaches can be frequent and debilitating.
- Migraines involve severe, throbbing pain often accompanied by nausea and light sensitivity.
4. Visceral Pain
- Originates from internal organs.
- Common causes: Endometriosis, irritable bowel syndrome (IBS).
Symptoms of Chronic Pain
- Persistent pain: Can range from mild to severe and may be continuous or intermittent.
- Stiffness and reduced mobility: May limit movement and daily activities.
- Fatigue: Ongoing pain can lead to physical and mental exhaustion.
- Sleep disturbances: Difficulty falling or staying asleep due to pain.
- Mood changes: Depression, anxiety, and irritability are common.
- Decreased quality of life: Pain can limit participation in work, social activities, and hobbies.
Risk Factors
- Age: Chronic pain is more common in older adults.
- Previous injuries: History of trauma or surgery.
- Medical conditions: Arthritis, diabetes, and other chronic diseases.
- Gender: Women are more likely to experience chronic pain conditions like fibromyalgia.
- Stress and mental health: Conditions such as anxiety and depression can exacerbate pain.
Diagnosis
- Medical history and physical examination: Comprehensive assessment by a healthcare provider.
- Imaging tests: Such as X-rays, MRI, or CT scans to identify underlying issues.
- Blood tests: To rule out conditions like arthritis or infections.
- Nerve conduction studies: To evaluate nerve function if neuropathic pain is suspected.
Treatment Options
- Medications:
- Pain relievers: Over-the-counter options like acetaminophen and NSAIDs.
- Prescription drugs: Including opioids, anticonvulsants, and antidepressants for specific pain types.
- Topical treatments: Creams or patches that target pain locally.
- Physical therapy: Exercises and stretching to improve mobility and reduce pain.
- Cognitive-behavioral therapy (CBT): Helps patients manage the mental impact of chronic pain.
- Alternative therapies:
- Acupuncture
- Massage therapy
- Chiropractic care
- Interventional procedures:
- Injections: Corticosteroid injections or nerve blocks.
- Implantable devices: Such as spinal cord stimulators.
Prevention Strategies
- Maintain a healthy lifestyle: Regular exercise, balanced diet, and weight management.
- Stay active: Physical activity can help keep muscles and joints strong.
- Manage stress: Techniques like mindfulness and meditation can reduce tension.
- Avoid repetitive strain: Take breaks during activities that strain muscles and joints.
Complications of Chronic Pain
- Depression and anxiety: Persistent pain can lead to mental health issues.
- Reduced mobility and disability: Can limit independence and ability to work.
- Sleep disorders: Insomnia and disrupted sleep patterns.
- Dependence on pain medication: Risk of addiction to opioids and other pain-relief drugs.
- Decreased quality of life: Impacts overall well-being and social interactions.
References & Research
Historical Background
The modern understanding of chronic pain as a distinct disease entity was shaped by John Bonica, who founded the first multidisciplinary pain clinic in 1947 and published "The Management of Pain" in 1953. Ronald Melzack and Patrick Wall proposed the gate control theory of pain in 1965, revolutionizing pain science. The International Association for the Study of Pain (IASP) was founded in 1973, and its classification of chronic pain was adopted by the WHO ICD-11 in 2019.
Key Research Papers
- Melzack R, Wall PD. Pain mechanisms: a new theory. Science. 1965;150(3699):971-979.
- Treede RD, et al. A classification of chronic pain for ICD-11. Pain. 2015;156(6):1003-1007.
- Gaskin DJ, Richard P. The economic costs of pain in the United States. Journal of Pain. 2012;13(8):715-724.
- Dowell D, Haegerich TM, Chou R. CDC guideline for prescribing opioids for chronic pain. JAMA. 2016;315(15):1624-1645.
- Vos T, et al. Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries: Global Burden of Disease Study 2010. The Lancet. 2012;380(9859):2163-2196.
- Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain. 2011;152(3 Suppl):S2-S15.
- Turk DC, Wilson HD, Cahana A. Treatment of chronic non-cancer pain. The Lancet. 2011;377(9784):2226-2235.
- Williams AC, Eccleston C, Morley S. Psychological therapies for the management of chronic pain (excluding headache) in adults. Cochrane Database of Systematic Reviews. 2012;(11):CD007407.
- Apkarian AV, et al. Human brain mechanisms of pain perception and regulation in health and disease. European Journal of Pain. 2005;9(4):463-484.
- Chou R, Huffman LH. Nonpharmacologic therapies for acute and chronic low back pain: a review of the evidence. Annals of Internal Medicine. 2007;147(7):492-504.
- Bushnell MC, Ceko M, Low LA. Cognitive and emotional control of pain and its disruption in chronic pain. Nature Reviews Neuroscience. 2013;14(7):502-511.
Research Papers
Explore current literature on chronic pain via PubMed topic searches. These links open live PubMed searches for the listed keywords — results update as new studies are indexed.
- Clinical trials on chronic pain — PubMed search
- Clinical trials on neuropathic pain — PubMed search
- Clinical trials on fibromyalgia — PubMed search
- Clinical trials on opioid chronic pain management — PubMed search
- Clinical trials on cognitive behavioral therapy chronic pain — PubMed search
- Clinical trials on central sensitization — PubMed search
- Clinical trials on chronic pain multidisciplinary — PubMed search
Connections
- Chronic Low Back Pain
- Interventional Pain
- Central Sensitization and Nociplastic Pain
- Non-Opioid Medications
- Pain Reprocessing Therapy
- Pain Mechanisms
- Sleep and Lifestyle for Chronic Pain
- Opioids for Chronic Pain
- Complex Regional Pain Syndrome
- Fibromyalgia
- Arthritis
- Depression
- Endometriosis
- Insomnia
- Migraine
- Chronic Fatigue Syndrome
- Peripheral Neuropathy
- Irritable Bowel Syndrome