Sleep Hygiene: A Naturopathic Guide to Restorative Sleep

From a naturopathic perspective, sleep is not merely the absence of wakefulness — it is the single most powerful healing modality available to the human body. Every night, the body enters a state of profound repair, detoxification, and regeneration that no supplement, diet, or therapy can replicate. When sleep is disrupted or insufficient, the consequences cascade through every organ system. This guide provides an evidence-based, naturopathic approach to optimizing sleep through environmental design, lifestyle practices, nutrition, and targeted supplementation.
Table of Contents
- 1. Sleep as the Foundation of Health
- 2. The Sleep-Disease Connection
- 3. Sleep Architecture: Stages and Cycles
- 4. Circadian Rhythm and the Master Clock
- 5. Blue Light and Melatonin Suppression
- 6. Optimal Sleep Environment
- 7. Evening Routine Protocol
- 8. Morning Routine for Better Sleep
- 9. Natural Sleep Supplements
- 10. Foods That Promote Sleep
- 11. Foods and Substances That Disrupt Sleep
- 12. Exercise Timing and Sleep
- 13. Stress, Cortisol Dysregulation, and Sleep
- 14. Sleep Disorders Overview
- 15. When to Seek Professional Help
- 16. Cautions and Contraindications
- Featured Videos
1. Sleep as the Foundation of Health
Sleep is the master regulator of human physiology. During sleep, the body performs functions that are impossible or severely impaired during waking hours. Understanding these processes reveals why compromised sleep leads so reliably to chronic disease.
Cellular Repair and Tissue Regeneration
During deep sleep, the body releases growth hormone (GH) from the anterior pituitary gland. GH stimulates tissue repair, muscle growth, and the regeneration of damaged cells throughout the body. Without adequate deep sleep, wound healing slows, muscle recovery declines, and the aging process accelerates.
Brain Detoxification via the Glymphatic System
The glymphatic system — the brain's dedicated waste-clearance pathway — becomes 10 to 20 times more active during sleep. Cerebrospinal fluid flushes through brain tissue, removing metabolic waste products including beta-amyloid and tau proteins, both implicated in Alzheimer's disease. This detoxification process is almost entirely dependent on sleep.
Memory Consolidation and Learning
During sleep, the hippocampus replays the day's experiences and transfers important information to the neocortex for long-term memory storage. Both declarative memory (facts) and procedural memory (skills) depend on adequate sleep. A single night of poor sleep can reduce the ability to form new memories by up to 40 percent.
Immune System Activation
Sleep is when the immune system performs critical maintenance. The body produces and releases cytokines, T-cells, and natural killer cells during sleep. Studies show that individuals sleeping fewer than six hours per night are more than four times as likely to catch a cold when exposed to the virus compared to those sleeping seven or more hours.
Hormone Production and Regulation
Sleep governs the production and timing of numerous hormones including melatonin, growth hormone, testosterone, leptin (satiety), ghrelin (hunger), insulin, cortisol, and thyroid-stimulating hormone. Disrupted sleep creates widespread hormonal imbalance that affects metabolism, appetite, mood, and reproductive health.
2. The Sleep-Disease Connection
Chronic sleep deprivation — defined as consistently sleeping fewer than seven hours per night — is now recognized as a significant risk factor for numerous serious diseases. The mechanisms are well-established and deeply concerning.
Obesity and Metabolic Syndrome
Sleep deprivation increases ghrelin (the hunger hormone) by up to 28 percent and decreases leptin (the satiety hormone) by 18 percent, leading to increased appetite and cravings for high-calorie, high-carbohydrate foods. Additionally, insulin sensitivity drops dramatically after even a few nights of restricted sleep, promoting fat storage and insulin resistance.
Type 2 Diabetes
Sleeping fewer than six hours per night is associated with a 40 to 50 percent increased risk of developing type 2 diabetes. Sleep deprivation impairs glucose tolerance and reduces insulin sensitivity to a degree comparable to the early stages of diabetes itself.
Cardiovascular Disease
Short sleep duration elevates blood pressure, increases systemic inflammation (measured by C-reactive protein), and promotes atherosclerosis. Individuals sleeping fewer than six hours per night have a 48 percent greater risk of developing or dying from coronary heart disease and a 15 percent greater risk of stroke.
Alzheimer's Disease and Neurodegeneration
The glymphatic system's inability to clear beta-amyloid plaques during insufficient sleep creates a vicious cycle: poor sleep leads to amyloid accumulation, which further disrupts sleep, accelerating cognitive decline. Research suggests that chronic sleep deprivation in midlife significantly increases Alzheimer's risk later in life.
Cancer
The World Health Organization has classified nighttime shift work as a probable carcinogen. Sleep deprivation suppresses natural killer cell activity — the immune cells responsible for identifying and destroying cancer cells. Studies have linked insufficient sleep to increased risk of breast, colorectal, and prostate cancers.
Depression and Anxiety
Sleep and mental health share a bidirectional relationship. Sleep deprivation amplifies activity in the amygdala (the brain's emotional center) by up to 60 percent while reducing connectivity with the prefrontal cortex (responsible for rational thought and emotional regulation). Insomnia increases the risk of developing depression by tenfold.
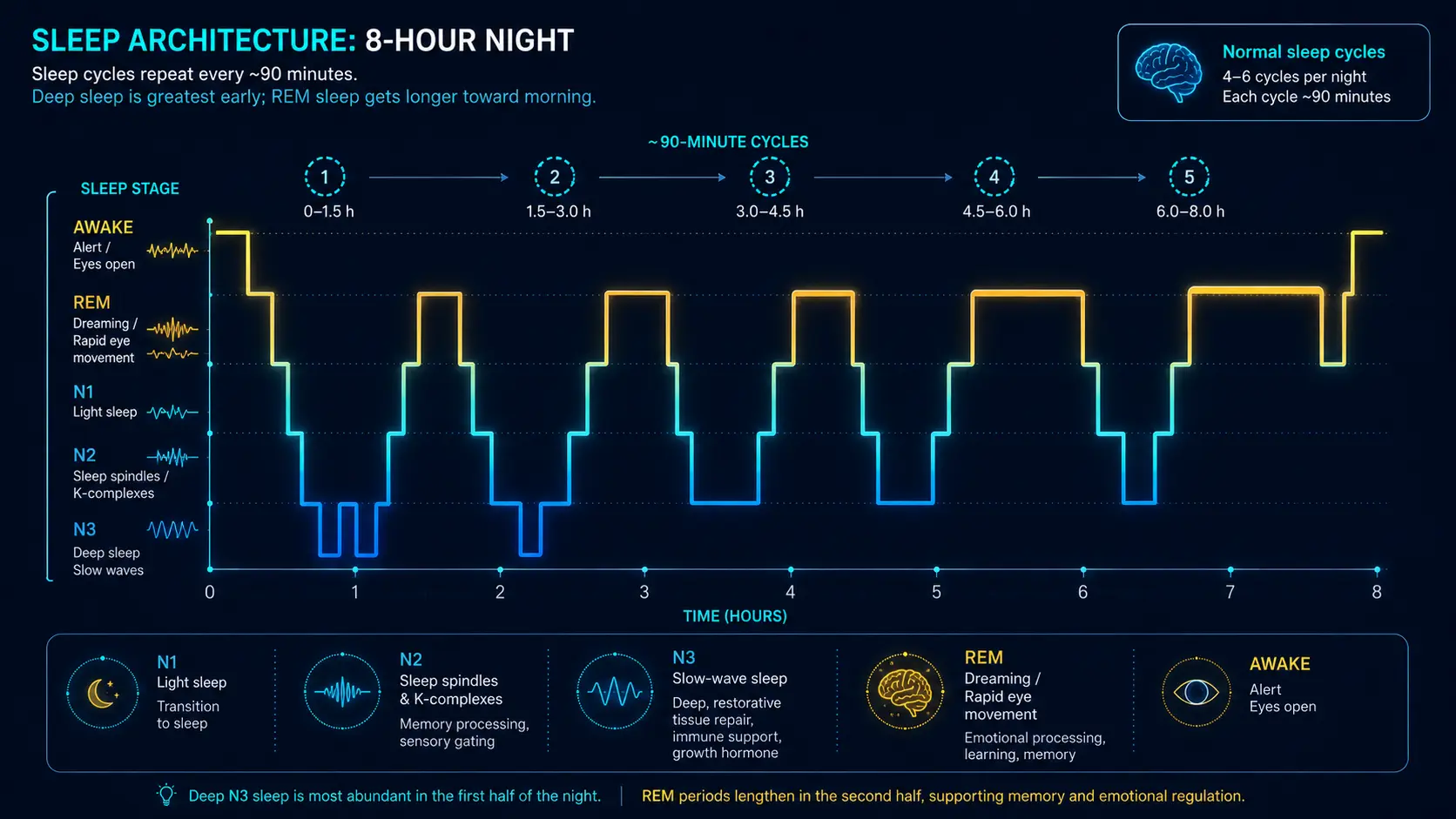
3. Sleep Architecture: Stages and Cycles
Understanding the structure of sleep helps explain why both quantity and quality matter. Sleep is not a uniform state but a carefully orchestrated progression through distinct stages, each serving vital functions.
NREM Stage 1 (Light Sleep)
- Duration: 1 to 5 minutes per cycle
- Brain waves: Transition from alpha to theta waves
- Function: The bridge between wakefulness and sleep; muscles relax, heart rate and breathing slow
- Easily awakened during this stage; you may experience hypnic jerks (sudden muscle twitches)
NREM Stage 2 (True Sleep Onset)
- Duration: 10 to 25 minutes per cycle (constitutes about 50 percent of total sleep)
- Brain waves: Theta waves with sleep spindles and K-complexes
- Function: Memory consolidation begins; body temperature drops, heart rate slows further
- Sleep spindles are critical for learning and memory processing
NREM Stage 3 (Deep Sleep / Slow-Wave Sleep)
- Duration: 20 to 40 minutes per cycle (more in the first half of the night)
- Brain waves: Large, slow delta waves
- Function: Physical restoration, growth hormone release, immune system strengthening, glymphatic clearance
- This is the most restorative stage — difficult to awaken from; waking during this stage causes grogginess (sleep inertia)
- Deep sleep declines with age, which contributes to age-related health decline
REM Sleep (Rapid Eye Movement)
- Duration: 10 to 60 minutes per cycle (lengthens as the night progresses)
- Brain waves: Fast, desynchronized activity similar to wakefulness
- Function: Emotional processing, creative problem-solving, memory integration, dreaming
- The body enters temporary muscle paralysis (atonia) to prevent acting out dreams
- REM sleep is essential for emotional resilience and psychological health
The 90-Minute Sleep Cycle
A complete sleep cycle lasts approximately 90 minutes and progresses through all four stages. A healthy adult completes four to six cycles per night (6 to 9 hours). The composition of each cycle shifts throughout the night: deep sleep dominates the first half of the night, while REM sleep dominates the second half. This is why cutting sleep short by even one hour disproportionately reduces REM time.
4. Circadian Rhythm and the Master Clock
The circadian rhythm is the body's internal 24-hour clock that governs the timing of sleep, wakefulness, hormone release, body temperature, and countless other physiological processes. Disrupting this rhythm has consequences far beyond poor sleep.
The Suprachiasmatic Nucleus (SCN)
The master clock resides in the suprachiasmatic nucleus, a tiny cluster of approximately 20,000 neurons located in the hypothalamus, directly above the optic chiasm. The SCN receives light information from specialized intrinsically photosensitive retinal ganglion cells (ipRGCs) in the eyes and uses this input to synchronize the body's internal clock with the external light-dark cycle.
The Melatonin Rhythm
As darkness falls, the SCN signals the pineal gland to begin producing melatonin, the body's primary sleep-signaling hormone. Melatonin levels typically begin rising approximately two hours before habitual bedtime (a period called dim-light melatonin onset, or DLMO), peak in the middle of the night, and fall to nearly undetectable levels by morning. Melatonin does not force sleep — it signals to the body that it is time to sleep.
The Cortisol Rhythm
Cortisol, the body's primary stress and alertness hormone, follows an opposite pattern. Cortisol reaches its lowest point around midnight, then begins rising in the early morning hours. It peaks approximately 30 to 45 minutes after waking — a phenomenon called the cortisol awakening response (CAR). This cortisol surge provides the energy and alertness needed to start the day. When cortisol rhythm is disrupted by chronic stress, shift work, or irregular schedules, both sleep initiation and daytime energy suffer profoundly.
Zeitgebers (Time Givers)
The circadian rhythm is entrained (synchronized) by environmental cues called zeitgebers:
- Light exposure — The most powerful zeitgeber, particularly morning sunlight
- Meal timing — Regular eating schedules help synchronize peripheral clocks in the liver and gut
- Physical activity — Exercise provides timing cues, especially when performed consistently
- Social interaction — Regular social schedules contribute to rhythm stability
- Temperature cycles — The body's core temperature rhythm closely tracks the circadian clock
5. Blue Light and Melatonin Suppression
Of all the modern factors disrupting human sleep, artificial blue light exposure after sunset may be the most pervasive and damaging. Understanding the mechanism is key to protecting sleep quality.
The ipRGCs in the retina that communicate with the SCN are most sensitive to light in the blue wavelength range (460 to 490 nanometers). This is precisely the wavelength emitted in high concentrations by LED screens (phones, tablets, computers, televisions) and LED/fluorescent lighting.
The Impact of Evening Blue Light
- Melatonin suppression: Even moderate blue light exposure in the evening can suppress melatonin production by 50 percent or more and delay melatonin onset by up to 90 minutes
- Circadian phase delay: Blue light tricks the SCN into thinking it is still daytime, pushing the entire sleep-wake cycle later
- Reduced sleep quality: Even when total sleep time is adequate, blue light exposure before bed reduces the proportion of restorative deep sleep and REM sleep
- Increased alertness: Blue light stimulates cortisol production at a time when it should be declining
Protective Strategies
- Use blue-light-blocking glasses (amber or red-tinted) starting two hours before bed
- Enable night mode or f.lux-type software on all devices
- Switch to warm-toned lighting (2700K or lower, or use red/amber bulbs) in the evening
- Use candlelight or salt lamps in the hour before sleep
- Avoid screens entirely in the final hour before bed when possible
6. Optimal Sleep Environment
The bedroom environment has a profound impact on sleep quality. From a naturopathic perspective, the sleeping space should be treated as a sanctuary optimized for rest and recovery.
Temperature: 65 to 68 Degrees Fahrenheit (18 to 20 Degrees Celsius)
The body must drop its core temperature by approximately 2 to 3 degrees Fahrenheit to initiate and maintain sleep. A bedroom that is too warm impairs this natural thermoregulation. Research consistently identifies the 65 to 68 degree Fahrenheit range as optimal for most adults. Consider using breathable, natural-fiber bedding (cotton, linen, wool) and wearing minimal or no clothing to facilitate heat dissipation.
Darkness
Complete darkness is essential for optimal melatonin production. Even small amounts of light — from alarm clocks, standby LEDs, or streetlights through curtains — can suppress melatonin through the skin and closed eyelids. Use blackout curtains or a high-quality sleep mask. Cover or remove any light-emitting devices from the bedroom.
Noise
Environmental noise disrupts sleep architecture even when it does not fully awaken you. The brain continues processing sound during sleep, and noise triggers micro-arousals that fragment sleep cycles. Options for noise management include white noise machines, earplugs, or addressing the source of noise directly. Consistent, low-frequency background sound is generally less disruptive than intermittent or unpredictable noise.
Mattress and Pillow
An unsupportive or aging mattress can cause pain, pressure points, and overheating, all of which impair sleep. Replace mattresses every 7 to 10 years. Choose pillows that maintain proper cervical spine alignment for your sleeping position. Consider mattresses made from natural materials (organic cotton, natural latex, wool) to minimize chemical off-gassing.
Electromagnetic Fields (EMF)
While research is ongoing, a precautionary approach to EMF in the bedroom is consistent with naturopathic principles. Consider placing phones in airplane mode or in another room, removing Wi-Fi routers from the bedroom, and unplugging electronics near the bed. At minimum, keep devices at least three feet from the head during sleep.
7. Evening Routine Protocol
A consistent evening routine signals the body and brain that sleep is approaching, allowing the natural cascade of hormonal and physiological changes to unfold properly. Think of the evening routine as a gradual transition from sympathetic (fight-or-flight) to parasympathetic (rest-and-digest) nervous system dominance.
Two Hours Before Bed
- Dim all household lights — Switch to warm, low-wattage bulbs or use lamps instead of overhead lighting
- Put on blue-light-blocking glasses if screens are still in use
- Finish eating — The last meal or snack should be consumed at least two to three hours before bed to allow digestion
- No vigorous exercise — Gentle stretching or yoga is acceptable, but intense workouts should be completed earlier
One Hour Before Bed
- Screens off — Turn off phones, tablets, computers, and television
- Take a warm bath or shower — The subsequent drop in body temperature as you cool down mimics the natural thermoregulation that precedes sleep
- Engage in relaxation practices — Deep breathing exercises, progressive muscle relaxation, meditation, gentle stretching, journaling, or reading a physical book
- Prepare the bedroom — Ensure the room is cool, dark, and quiet
Thirty Minutes Before Bed
- Take sleep-supportive supplements if part of your protocol
- Practice gratitude or prayer — Shifting the mind toward positive or peaceful thoughts reduces cortisol
- Perform gentle breathwork — The 4-7-8 breathing technique (inhale for 4, hold for 7, exhale for 8) activates the parasympathetic nervous system
- Go to bed at the same time every night — Consistency is one of the most powerful sleep regulators
8. Morning Routine for Better Sleep
Paradoxically, what you do in the first 30 to 60 minutes after waking is one of the most powerful determinants of sleep quality that night. The morning routine anchors the circadian rhythm and sets the timing for melatonin release 14 to 16 hours later.
Sunlight Exposure Within 30 Minutes of Waking
Exposure to bright, natural sunlight within the first 30 minutes of waking is the single most effective way to calibrate the circadian clock. Aim for at least 10 to 15 minutes of direct outdoor sunlight (30 minutes or more on overcast days). Do not wear sunglasses during this exposure — the light must reach the ipRGCs in the retina. This morning light pulse triggers a cortisol awakening response, suppresses residual melatonin, and starts the timer for melatonin production to begin that evening.
Consistent Wake Time
Waking at the same time every day — including weekends — is more important for circadian rhythm stability than consistent bedtime. Varying your wake time by even one to two hours on weekends (so-called "social jet lag") can disrupt the circadian rhythm for several days afterward. Choose a wake time you can maintain seven days a week and hold to it rigidly.
Morning Movement
Light physical activity in the morning — a walk, gentle stretching, or yoga — reinforces the cortisol awakening response and provides additional circadian cues through body temperature elevation and neurotransmitter release.
Delay Caffeine
Wait at least 60 to 90 minutes after waking before consuming caffeine. Caffeine consumed immediately upon waking interferes with the cortisol awakening response and can lead to an afternoon energy crash that drives further caffeine consumption, ultimately impairing sleep.
9. Natural Sleep Supplements
When sleep hygiene practices alone are insufficient, certain natural compounds can provide meaningful support. From a naturopathic perspective, supplements should complement — never replace — foundational sleep practices.
Magnesium Glycinate
- Dose: 200 to 400 mg elemental magnesium, taken 30 to 60 minutes before bed
- Mechanism: Activates the parasympathetic nervous system, regulates GABA receptors, relaxes muscles, and reduces cortisol
- The glycinate form is preferred for sleep because glycine itself has calming properties and this form is gentle on the digestive system
- An estimated 50 percent of adults are deficient in magnesium, making this one of the highest-yield sleep interventions
L-Theanine
- Dose: 100 to 400 mg, taken 30 to 60 minutes before bed
- Mechanism: An amino acid found in green tea that increases alpha brain wave activity, promoting relaxed alertness transitioning to calm; increases GABA, serotonin, and dopamine
- Does not cause drowsiness — it reduces anxiety and mental chatter that prevent sleep onset
- Particularly effective for individuals whose sleep difficulty is driven by an overactive mind
GABA (Gamma-Aminobutyric Acid)
- Dose: 100 to 300 mg before bed
- Mechanism: The primary inhibitory neurotransmitter in the brain; supplemental GABA may promote relaxation and reduce sleep latency
- Oral GABA's ability to cross the blood-brain barrier is debated, but many individuals report subjective benefit; it may also act through the enteric nervous system (gut-brain axis)
Glycine
- Dose: 3 grams before bed
- Mechanism: Lowers core body temperature by promoting peripheral vasodilation; acts as an inhibitory neurotransmitter
- Research shows glycine supplementation improves subjective sleep quality, reduces daytime sleepiness, and improves cognitive performance the following day
Tart Cherry Extract (Natural Melatonin Source)
- Dose: 500 mg tart cherry extract or 8 ounces tart cherry juice concentrate
- Mechanism: Contains natural melatonin and anti-inflammatory compounds (anthocyanins) that support sleep
- Preferred over synthetic melatonin in naturopathic practice because it provides melatonin in a whole-food context with synergistic compounds
- If using supplemental melatonin directly, start with the lowest effective dose (0.3 to 0.5 mg), as most commercial doses (3 to 10 mg) are far higher than physiological levels
Valerian Root
- Dose: 300 to 600 mg standardized extract, taken 30 minutes to 2 hours before bed
- Mechanism: Increases GABA levels in the brain by inhibiting GABA reuptake and breakdown
- Effects may take two to four weeks of consistent use to reach full benefit
- Often combined with hops extract for enhanced effect
Passionflower
- Dose: 250 to 500 mg extract or one cup of passionflower tea before bed
- Mechanism: Increases GABA levels; shown in clinical trials to improve sleep quality comparably to some pharmaceutical sleep aids
- Particularly useful for sleep disruption related to anxiety
Ashwagandha
- Dose: 300 to 600 mg of KSM-66 or Sensoril extract
- Mechanism: An adaptogenic herb that lowers cortisol, reduces stress, and promotes a sense of calm; contains triethylene glycol, which has been shown to promote NREM sleep
- Best suited for individuals whose sleep difficulties are rooted in chronic stress and elevated cortisol
10. Foods That Promote Sleep
Certain foods contain compounds that directly support the biochemistry of sleep. Incorporating these into the evening diet can make a meaningful difference in sleep onset and quality.
Tryptophan-Rich Foods
Tryptophan is the amino acid precursor to serotonin, which is subsequently converted to melatonin. Foods high in tryptophan include:
- Turkey and chicken
- Eggs
- Pumpkin seeds and sesame seeds
- Nuts (especially almonds and walnuts)
- Wild-caught salmon and other oily fish (also high in omega-3 fatty acids and vitamin D, both linked to better sleep)
- Dairy products (for those who tolerate them)
Complex Carbohydrates
A moderate serving of complex carbohydrates at dinner (sweet potatoes, quinoa, oats, brown rice) enhances tryptophan uptake into the brain by stimulating insulin, which clears competing amino acids from the bloodstream. Pairing a tryptophan-rich protein with a complex carbohydrate at dinner is a time-tested strategy for sleep support.
Kiwifruit
Multiple studies have found that consuming two kiwifruits one hour before bed significantly improves sleep onset, duration, and efficiency. Kiwis are rich in serotonin, antioxidants, and folate, all of which may contribute to their sleep-promoting effects.
Tart Cherries
As noted in the supplement section, tart cherries are one of the few natural food sources of melatonin. Consuming tart cherry juice or whole tart cherries in the evening has been shown to increase sleep duration by up to 84 minutes in clinical trials.
Other Sleep-Supportive Foods
- Chamomile tea — Contains apigenin, which binds to GABA receptors and promotes sedation
- Warm milk — Contains tryptophan and calcium; the warmth and ritual also contribute to relaxation
- Bananas — Contain magnesium, potassium, and tryptophan
- Honey (raw) — A small amount may help by providing glucose that allows tryptophan to enter the brain more easily and supports liver glycogen stores overnight
11. Foods and Substances That Disrupt Sleep
Just as certain foods promote sleep, others can profoundly disrupt it. Avoiding these substances — particularly in the second half of the day — is essential for sleep optimization.
Caffeine
Caffeine is an adenosine receptor antagonist — it blocks the sleep-pressure signal that accumulates throughout the day. What most people fail to appreciate is caffeine's half-life of 5 to 7 hours. This means that a cup of coffee at 2:00 PM still has half its caffeine circulating at 7:00 to 9:00 PM. Even if you can "fall asleep" after caffeine, studies show it reduces deep sleep by 15 to 20 percent. For optimal sleep, establish a caffeine cutoff by noon, or earlier for slow metabolizers (those with certain CYP1A2 gene variants).
Alcohol
Alcohol is one of the most misunderstood substances in relation to sleep. While it is a sedative that can speed sleep onset, alcohol profoundly disrupts sleep architecture:
- Suppresses REM sleep, particularly in the first half of the night
- Causes sleep fragmentation in the second half of the night as alcohol is metabolized
- Relaxes upper airway muscles, worsening snoring and sleep apnea
- Disrupts body temperature regulation
- Acts as a diuretic, increasing nighttime awakenings
Even moderate alcohol consumption (one to two drinks) significantly impairs sleep quality. If consumed, allow at least three to four hours between the last drink and bedtime.
Heavy Meals Close to Bedtime
Large, high-fat, or spicy meals consumed within two to three hours of bed can cause gastroesophageal reflux, digestive discomfort, and elevated core body temperature — all of which impair sleep onset and maintenance. If you are hungry before bed, opt for a small, light snack combining a tryptophan source with a small amount of complex carbohydrate.
Refined Sugar and High-Glycemic Foods
High-sugar foods consumed in the evening cause blood glucose spikes followed by crashes. These blood sugar fluctuations trigger cortisol and adrenaline release during the night, leading to nighttime awakenings, often between 2:00 and 4:00 AM. Stabilizing blood sugar through the evening and overnight is critical for uninterrupted sleep.
12. Exercise Timing and Sleep
Regular physical activity is one of the most evidence-based interventions for improving sleep quality. However, the timing of exercise significantly influences its impact on sleep.
Benefits of Exercise for Sleep
- Increases time spent in deep sleep (slow-wave sleep)
- Reduces sleep onset latency (time to fall asleep)
- Decreases symptoms of insomnia and anxiety
- Helps regulate the circadian rhythm through body temperature effects
- Reduces cortisol and promotes the healthy evening decline needed for sleep
Optimal Timing
- Morning exercise (6:00 to 10:00 AM): Generally the most beneficial for sleep. Morning exercise combined with sunlight exposure provides powerful circadian entrainment. Elevates body temperature early in the day, allowing a greater drop by evening.
- Afternoon exercise (1:00 to 5:00 PM): Also beneficial. Body temperature and muscle function peak in the late afternoon, making this optimal for performance. The subsequent body temperature decline several hours later coincides well with bedtime.
- Evening exercise (after 7:00 PM): Vigorous exercise within two to three hours of bedtime can impair sleep by elevating core body temperature, heart rate, cortisol, and adrenaline at a time when all should be declining. However, gentle activities such as yoga, tai chi, or a leisurely walk are generally sleep-supportive in the evening.
Consistency Matters
The sleep benefits of exercise are most pronounced with regular, consistent practice. A single bout of exercise may not noticeably improve sleep that night, but regular exercise over weeks produces significant and measurable improvements in sleep quality, duration, and efficiency.
13. Stress, Cortisol Dysregulation, and Sleep
Chronic stress may be the most common root cause of sleep difficulties in modern life. Understanding the cortisol-sleep relationship is essential for addressing sleep problems at their source.
The Normal Cortisol Curve
In a healthy individual, cortisol follows a predictable daily pattern: it peaks in the morning (providing energy and alertness), gradually declines throughout the day, reaches its lowest point around midnight, then begins rising again in the early morning hours. This pattern is called the diurnal cortisol rhythm.
How Chronic Stress Disrupts This Pattern
Under chronic stress, the hypothalamic-pituitary-adrenal (HPA) axis becomes dysregulated. Common patterns include:
- Elevated evening cortisol: Instead of declining, cortisol remains high at night, causing a "wired but tired" state — exhausted yet unable to fall asleep
- Flattened cortisol curve: Morning cortisol fails to rise adequately (causing difficulty waking and morning fatigue) while evening cortisol fails to drop sufficiently
- Cortisol spikes during the night: Stress-induced nighttime cortisol release causes awakenings, often between 2:00 and 4:00 AM, frequently accompanied by racing thoughts or anxiety
Naturopathic Approaches to Cortisol Regulation
- Adaptogenic herbs: Ashwagandha, rhodiola, holy basil (tulsi), and reishi mushroom help modulate the HPA axis and normalize cortisol patterns
- Phosphatidylserine: 100 to 300 mg in the evening has been shown to reduce elevated cortisol
- Mindfulness meditation: Regular practice reduces baseline cortisol levels and improves cortisol reactivity
- Breathwork: Slow, diaphragmatic breathing (especially extended exhales) directly activates the vagus nerve and shifts the nervous system toward parasympathetic dominance
- Journaling: Writing down worries and to-do lists before bed reduces cognitive arousal and rumination
- Nature exposure: Time spent in natural environments measurably reduces cortisol levels
14. Sleep Disorders Overview
While many sleep difficulties respond to lifestyle and naturopathic interventions, certain conditions require specific recognition and may need collaborative care with sleep medicine specialists.
Insomnia
Insomnia is characterized by difficulty falling asleep, staying asleep, or waking too early despite adequate opportunity for sleep, resulting in daytime impairment. It is classified as:
- Acute insomnia: Short-term (days to weeks), often triggered by stress, travel, or life changes
- Chronic insomnia: Occurring at least three nights per week for three months or more
The gold standard treatment for chronic insomnia is Cognitive Behavioral Therapy for Insomnia (CBT-I), which addresses the behavioral and thought patterns that perpetuate sleep difficulty. CBT-I is more effective than sleep medications in the long term and has no side effects. Naturopathic approaches complement CBT-I with sleep hygiene optimization, supplementation, and stress management.
Obstructive Sleep Apnea (OSA)
Obstructive sleep apnea is a condition in which the upper airway repeatedly collapses during sleep, causing breathing interruptions (apneas) that last 10 seconds or longer. These events trigger micro-arousals, fragment sleep, and reduce oxygen levels. Warning signs include:
- Loud, chronic snoring
- Witnessed pauses in breathing during sleep
- Gasping or choking upon awakening
- Excessive daytime sleepiness despite seemingly adequate sleep duration
- Morning headaches and dry mouth
- Difficulty concentrating and memory problems
OSA is a serious condition linked to hypertension, heart disease, stroke, diabetes, and sudden cardiac death. Diagnosis requires a sleep study (polysomnography). Treatment typically involves CPAP therapy (continuous positive airway pressure), though weight loss, positional therapy, oral appliances, and myofunctional therapy may also play a role depending on severity.
Other Sleep Disorders
- Restless Legs Syndrome (RLS): An irresistible urge to move the legs, often accompanied by uncomfortable sensations; often associated with iron deficiency, magnesium deficiency, or dopamine dysregulation
- Circadian Rhythm Disorders: Including delayed sleep phase disorder (natural sleep time is very late) and advanced sleep phase disorder (natural sleep time is very early)
- Parasomnias: Sleepwalking, sleep talking, night terrors, and REM sleep behavior disorder
15. When to Seek Professional Help
While naturopathic and lifestyle approaches are effective for many sleep difficulties, certain situations warrant prompt professional evaluation:
- You have been told you stop breathing or gasp during sleep
- Loud chronic snoring that disrupts your or your partner's sleep
- Excessive daytime sleepiness that impairs driving, work performance, or daily functioning despite apparently adequate sleep
- Sleep difficulties that persist for more than four weeks despite implementing comprehensive sleep hygiene measures
- Symptoms of restless legs syndrome that interfere with sleep onset
- Sleepwalking or other parasomnias that pose safety risks
- Sleep difficulties accompanied by depression, anxiety, or suicidal thoughts
- Unexplained morning headaches, dry mouth, or jaw pain upon waking
- Any sleep issue significantly impacting quality of life, relationships, or job performance
A naturopathic doctor can work collaboratively with sleep medicine physicians, providing integrative care that combines the best of conventional diagnostics (sleep studies, CPAP titration) with naturopathic therapeutics (supplementation, dietary optimization, stress management, and lifestyle modification).
16. Cautions and Contraindications
While the interventions described in this guide are generally safe, important cautions apply:
- Supplement interactions: Magnesium, valerian, passionflower, and other calming supplements may potentiate the effects of prescription sedatives, benzodiazepines, and anti-anxiety medications. Always consult a healthcare provider before combining supplements with prescription sleep medications.
- Melatonin cautions: Supplemental melatonin should be used at the lowest effective dose. High-dose melatonin (above 1 mg) can cause morning grogginess, vivid dreams, and may suppress the body's own melatonin production over time. Melatonin may interact with blood thinners, immunosuppressants, diabetes medications, and birth control pills.
- Ashwagandha cautions: Avoid during pregnancy and breastfeeding. May interact with thyroid medications, immunosuppressants, and sedatives. Individuals with autoimmune conditions should use under practitioner guidance.
- Valerian cautions: May cause headaches or digestive upset in some individuals. Do not combine with alcohol or other sedatives. Discontinue at least two weeks before scheduled surgery due to potential anesthetic interactions.
- Do not self-treat suspected sleep apnea: Sleep apnea is a potentially life-threatening condition that requires proper diagnosis and medical management. Supplements and lifestyle changes alone are insufficient for moderate to severe sleep apnea.
- Children and adolescents: Many sleep supplements are not well-studied in pediatric populations. Consult a pediatric naturopathic doctor or pediatrician before administering sleep supplements to children.
- Underlying medical conditions: Persistent insomnia can be a symptom of underlying conditions including thyroid disorders, chronic pain, depression, anxiety, and hormonal imbalances. Address root causes rather than relying solely on symptomatic treatment.
This article is for educational purposes only and does not constitute medical advice. Consult a licensed naturopathic doctor or healthcare provider before starting any new supplement regimen or making significant changes to your health routine.
Research Papers
Selected PubMed topic searches relevant to sleep physiology, circadian rhythms, and evidence-based non-pharmacologic sleep interventions.
- PubMed: Sleep hygiene and insomnia
- PubMed: Melatonin and circadian rhythm
- PubMed: Blue light and melatonin suppression
- PubMed: CBT-I for insomnia
- PubMed: Magnesium and sleep
- PubMed: Glycine and sleep quality
- PubMed: Sleep deprivation and cardiovascular risk
- PubMed: Sleep restriction and glucose metabolism
- PubMed: Shift work and circadian disruption
- PubMed: Sleep and thermoregulation
- PubMed: L-theanine and sleep
- PubMed: REM/SWS and memory consolidation
Connections
- Tart Cherry
- Valerian
- Chamomile
- Lavender
- Passionflower
- Glycine
- Tryptophan
- Magnesium & Sleep
- Magnesium Glycinate
- Anxiety
- Insomnia
- Obstructive Sleep Apnea
- Stress Management
- Natural Anxiety Relief
- Mouth Taping
- Longevity Protocols
- Breathwork
- Magnesium