Ulcerative Colitis
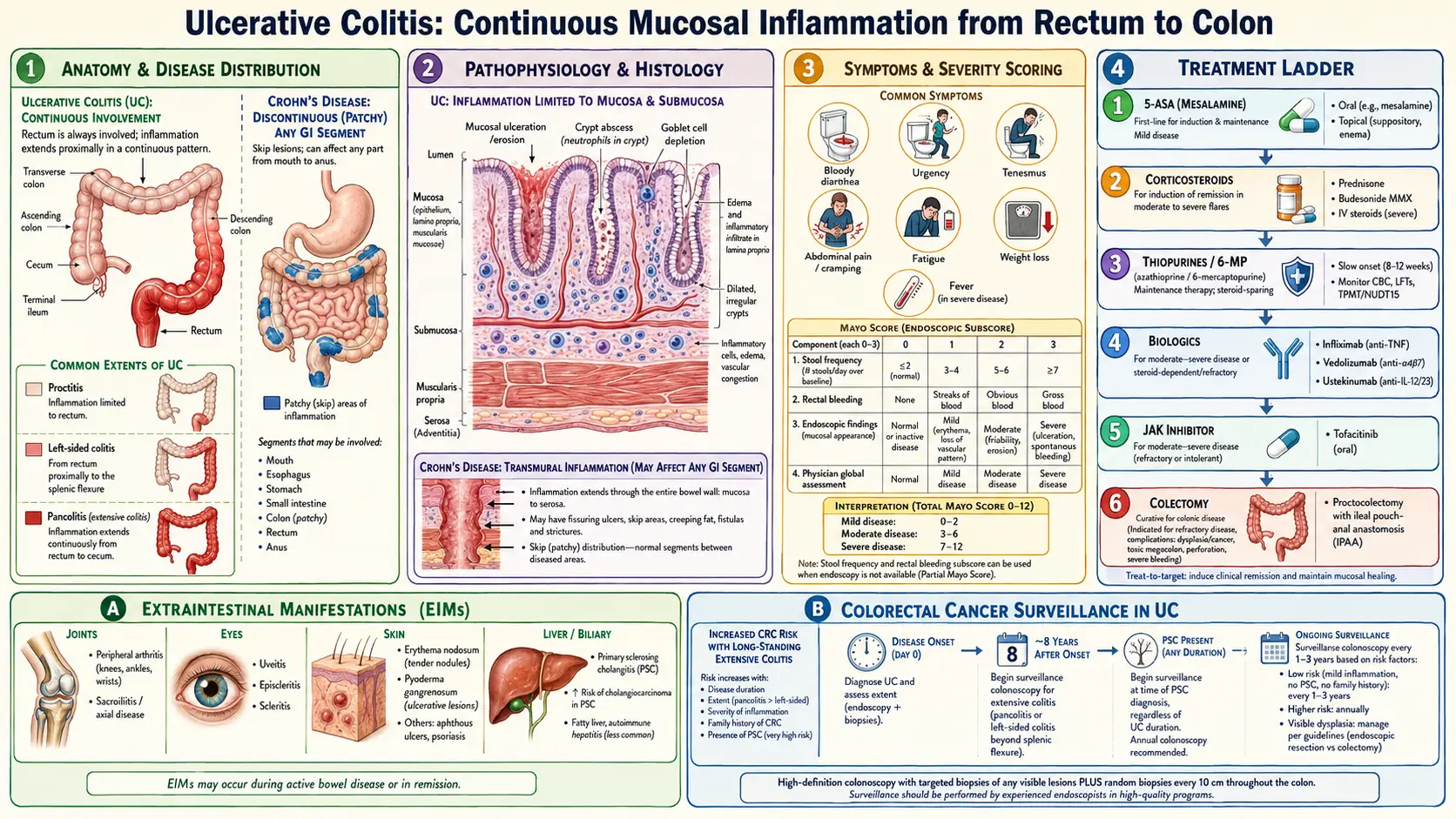
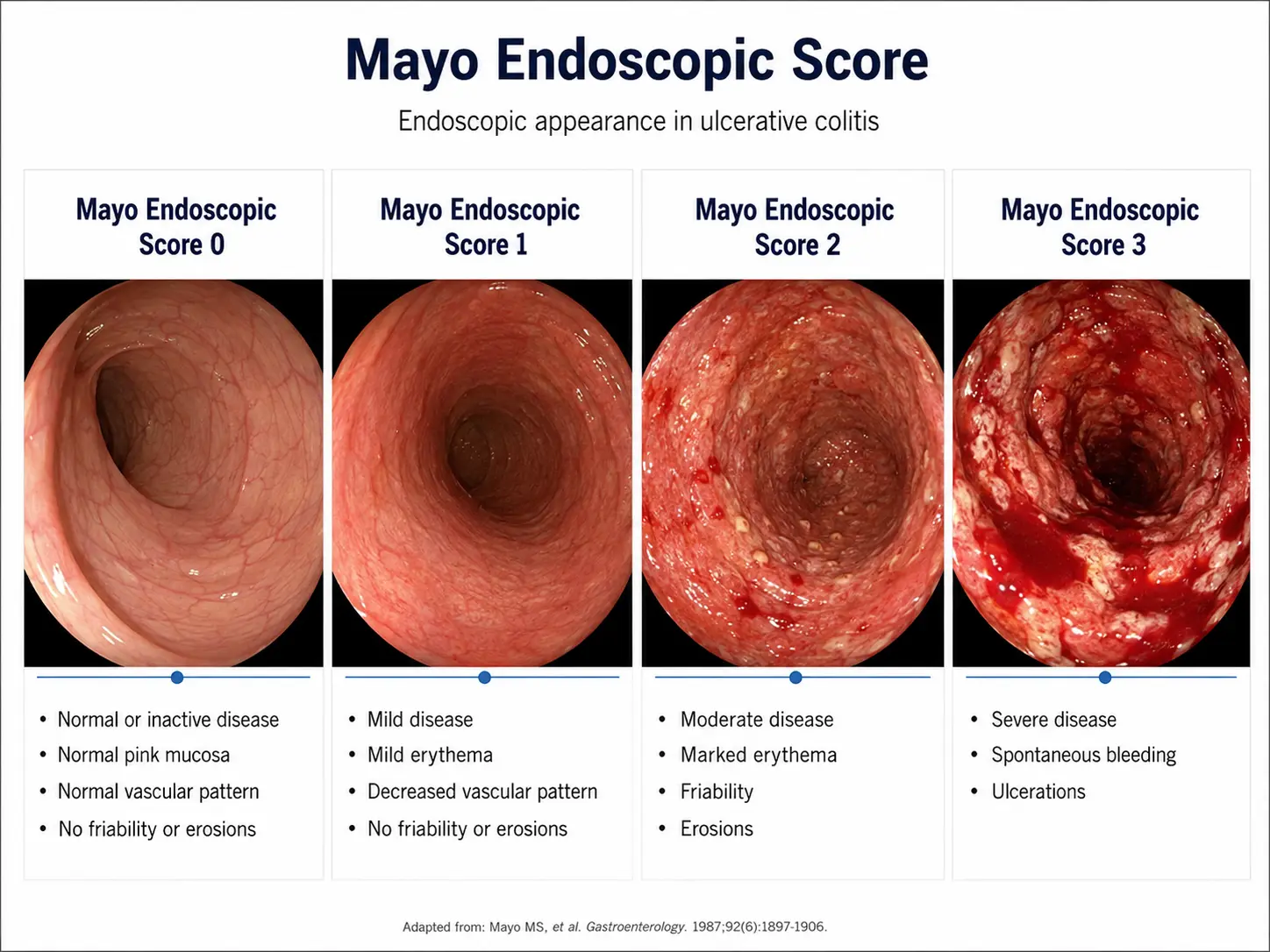
Table of Contents
- What is Ulcerative Colitis?
- Common Symptoms of Ulcerative Colitis
- Types of Ulcerative Colitis
- Causes and Risk Factors
- Diagnosis
- Treatment Options
- Prevention and Management Strategies
- Complications of Ulcerative Colitis
- Research Papers
- Connections
- Featured Videos
What is Ulcerative Colitis?
Ulcerative colitis is a chronic inflammatory bowel disease (IBD) that causes long-lasting inflammation and ulcers (sores) in the innermost lining of the colon and rectum. It can lead to symptoms that develop over time, rather than suddenly, and can significantly affect daily life.
Common Symptoms of Ulcerative Colitis
- Persistent diarrhea, often with blood or pus.
- Abdominal pain and cramping
- Urgency to have a bowel movement
- Rectal pain and bleeding
- Fatigue
- Unintended weight loss
- Fever in severe cases.
Types of Ulcerative Colitis
- Ulcerative proctitis: Inflammation limited to the rectum, often causing rectal bleeding.
- Proctosigmoiditis: Affects the rectum and lower end of the colon (sigmoid colon), causing bloody diarrhea and abdominal pain.
- Left-sided colitis: Involves inflammation from the rectum up to the left side of the colon, leading to symptoms like weight loss, diarrhea, and pain on the left side.
- Pancolitis: Affects the entire colon and can cause severe bloody diarrhea, fatigue, and significant weight loss.
- Fulminant colitis: A rare and severe form of pancolitis that can lead to life-threatening complications.
Causes and Risk Factors
- Immune system response: An abnormal response of the immune system leads to inflammation in the colon.
- Genetics: A family history of ulcerative colitis or other IBDs increases the risk.
- Age: Most commonly diagnosed before age 30, but can occur at any age.
- Ethnicity: More common among people of Caucasian and Ashkenazi Jewish descent.
Diagnosis
- Medical history and physical examination: To assess symptoms and risk factors.
- Colonoscopy: Allows visualization of the colon and tissue sampling for biopsy.
- Flexible sigmoidoscopy: Examines the rectum and lower colon.
- Imaging tests: Such as X-rays, CT scans, or MRIs to detect complications or rule out other conditions.
- Stool tests: To rule out infections and detect markers of inflammation.
- Blood tests: To check for anemia and signs of inflammation.
Treatment Options
- Medications:
- Aminosalicylates (5-ASAs): Such as mesalamine to help control mild to moderate inflammation.
- Corticosteroids: Used for short-term treatment of flare-ups to reduce inflammation.
- Immunosuppressants: Such as azathioprine and cyclosporine to decrease immune system activity.
- Biologic therapies: Target specific parts of the immune system (e.g., infliximab, adalimumab) to control inflammation.
- JAK inhibitors: Such as tofacitinib for moderate to severe ulcerative colitis.
- Diet and Nutrition:
- Adjust diet during flare-ups: A low-residue or low-fiber diet may help reduce symptoms.
- Small, frequent meals: To maintain nutrition and minimize discomfort.
- Surgery:
- Colectomy: Removal of part or all of the colon, which may be necessary if medications are ineffective or complications arise.
- Ileal pouch-anal anastomosis (IPAA): A surgical option that allows stool to pass through the anus normally after removal of the colon and rectum.
Prevention and Management Strategies
- Stay hydrated: Drink plenty of fluids, especially water, to prevent dehydration during flare-ups.
- Avoid known trigger foods: Such as dairy products, spicy foods, and high-fiber foods if they aggravate symptoms.
- Manage stress: Stress-reduction techniques such as deep breathing, meditation, or yoga can help manage symptoms.
- Maintain a balanced diet and take vitamins and supplements as recommended by a healthcare provider.
- Regular medical follow-ups: To monitor the condition and adjust treatment as needed.
Complications of Ulcerative Colitis
- Severe bleeding
- Perforated colon: A hole in the colon can develop, which is a medical emergency.
- Severe dehydration
- Toxic megacolon: A rare but serious complication where the colon rapidly expands.
- Increased risk of colon cancer: Especially in those with extensive or long-term ulcerative colitis.
- Primary sclerosing cholangitis: Inflammation and scarring of the bile ducts, leading to liver damage.
- Bone loss (osteoporosis): Can result from long-term corticosteroid use.
9. References & Research
Historical Background
Ulcerative colitis was first clearly described as a distinct disease by Sir Samuel Wilks at Guy's Hospital, London, in 1859, differentiating it from infectious dysentery. In 1909, Sir Arthur Hurst provided the first endoscopic descriptions of the disease. The introduction of sulfasalazine by Nanna Svartz in 1942 marked the beginning of effective medical therapy for the condition.
Key Research Papers
- Ordas I, Eckmann L, Talamini M, Baumgart DC, Sandborn WJ. Ulcerative colitis. The Lancet. 2012;380(9853):1606-1619.
- Danese S, Fiocchi C. Ulcerative colitis. N Engl J Med. 2011;365(18):1713-1725.
- Rubin DT, Ananthakrishnan AN, Siegel CA, et al. ACG clinical guideline: ulcerative colitis in adults. Am J Gastroenterol. 2019;114(3):384-413.
- Feagan BG, Rutgeerts P, Sands BE, et al. Vedolizumab as induction and maintenance therapy for ulcerative colitis (GEMINI 1). N Engl J Med. 2013;369(3):699-710.
- Sandborn WJ, Su C, Sands BE, et al. Tofacitinib as induction and maintenance therapy for ulcerative colitis (OCTAVE). N Engl J Med. 2017;376(18):1723-1736.
- Rutgeerts P, Sandborn WJ, Feagan BG, et al. Infliximab for induction and maintenance therapy for ulcerative colitis (ACT trials). N Engl J Med. 2005;353(23):2462-2476.
- Ng SC, Shi HY, Hamidi N, et al. Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century. The Lancet. 2017;390(10114):2769-2778.
- Magro F, Gionchetti P, Eliakim R, et al. Third European evidence-based consensus on diagnosis and management of ulcerative colitis (ECCO). J Crohns Colitis. 2017;11(6):649-670.
- Jostins L, Ripke S, Weersma RK, et al. Host-microbe interactions have shaped the genetic architecture of inflammatory bowel disease. Nature. 2012;491(7422):119-124.
- Kornbluth A, Sachar DB. Ulcerative colitis practice guidelines in adults: American College of Gastroenterology Practice Parameters Committee. Am J Gastroenterol. 2010;105(3):501-523.
- Ungaro R, Mehandru S, Allen PB, Peyrin-Biroulet L, Colombel JF. Ulcerative colitis. The Lancet. 2017;389(10080):1756-1770.
- Kaplan GG. The global burden of IBD: from 2015 to 2025. Nat Rev Gastroenterol Hepatol. 2015;12(12):720-727.
Research Papers
Curated PubMed topic searches of peer-reviewed literature on Ulcerative Colitis. Each link opens a live PubMed query so you always see the most current studies.
- PubMed: UC treatment guidelines
- PubMed: Mesalamine in UC
- PubMed: Biologic therapy in UC
- PubMed: Vedolizumab in UC
- PubMed: Tofacitinib in UC
- PubMed: Colectomy and IPAA
- PubMed: CRC surveillance
- PubMed: FMT in UC
- PubMed: Acute severe UC
- PubMed: Pediatric UC
- PubMed: UC and PSC
- PubMed: Quality of life in UC
Connections
- Inflammatory Bowel Disease
- Crohn's Disease
- Irritable Bowel Syndrome
- Celiac Disease
- Crohn's vs Ulcerative Colitis
- Ankylosing Spondylitis
- AS and IBD Overlap
- Gut Healing
- Elimination Diet
- Turmeric
- Vitamin D3
- Zinc
- Diverticulitis
- Anemia
- Abdominal Pain
- Fatigue
- Osteoporosis
- Cancer