Obstructive Sleep Apnea (OSA)
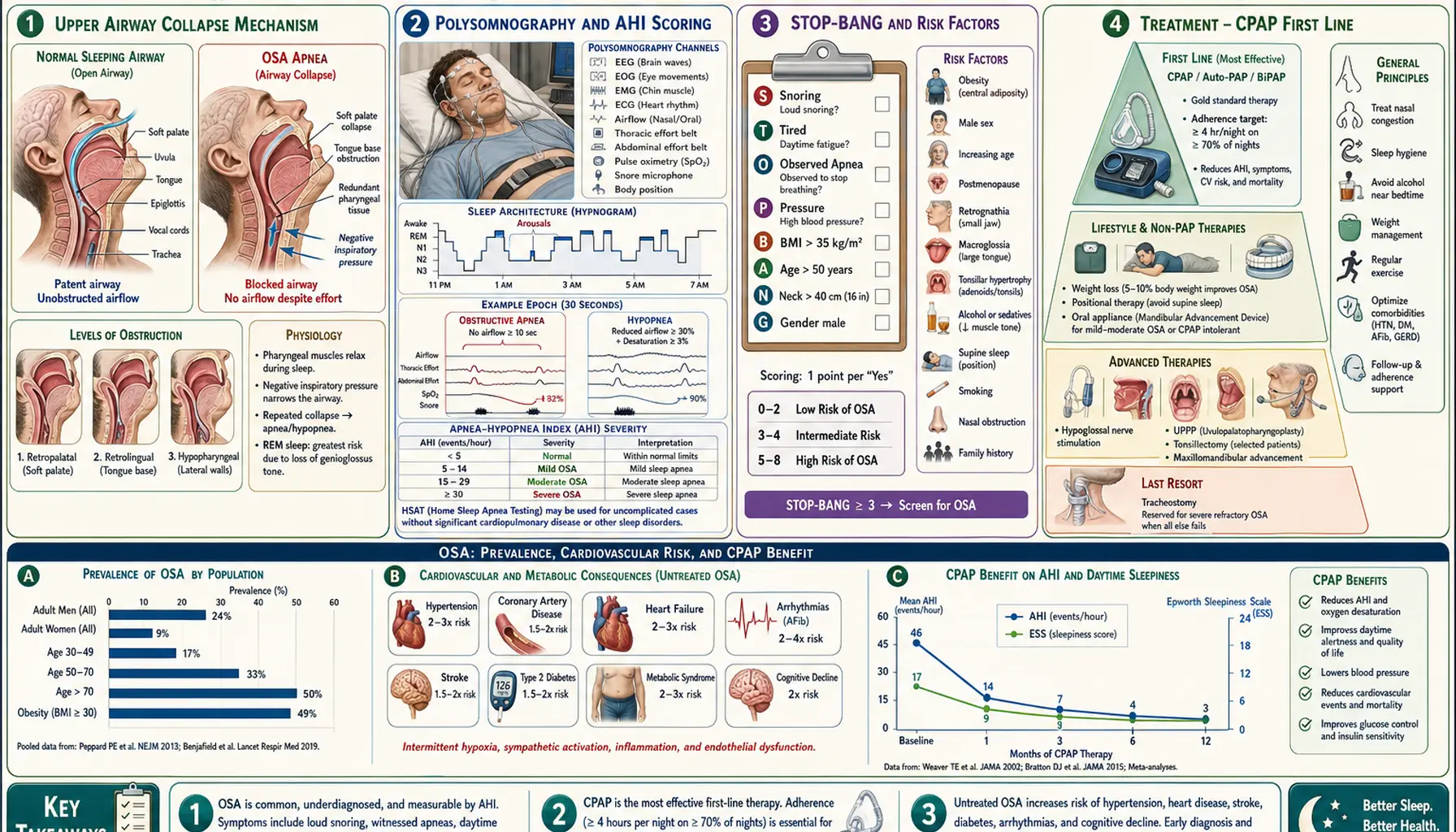
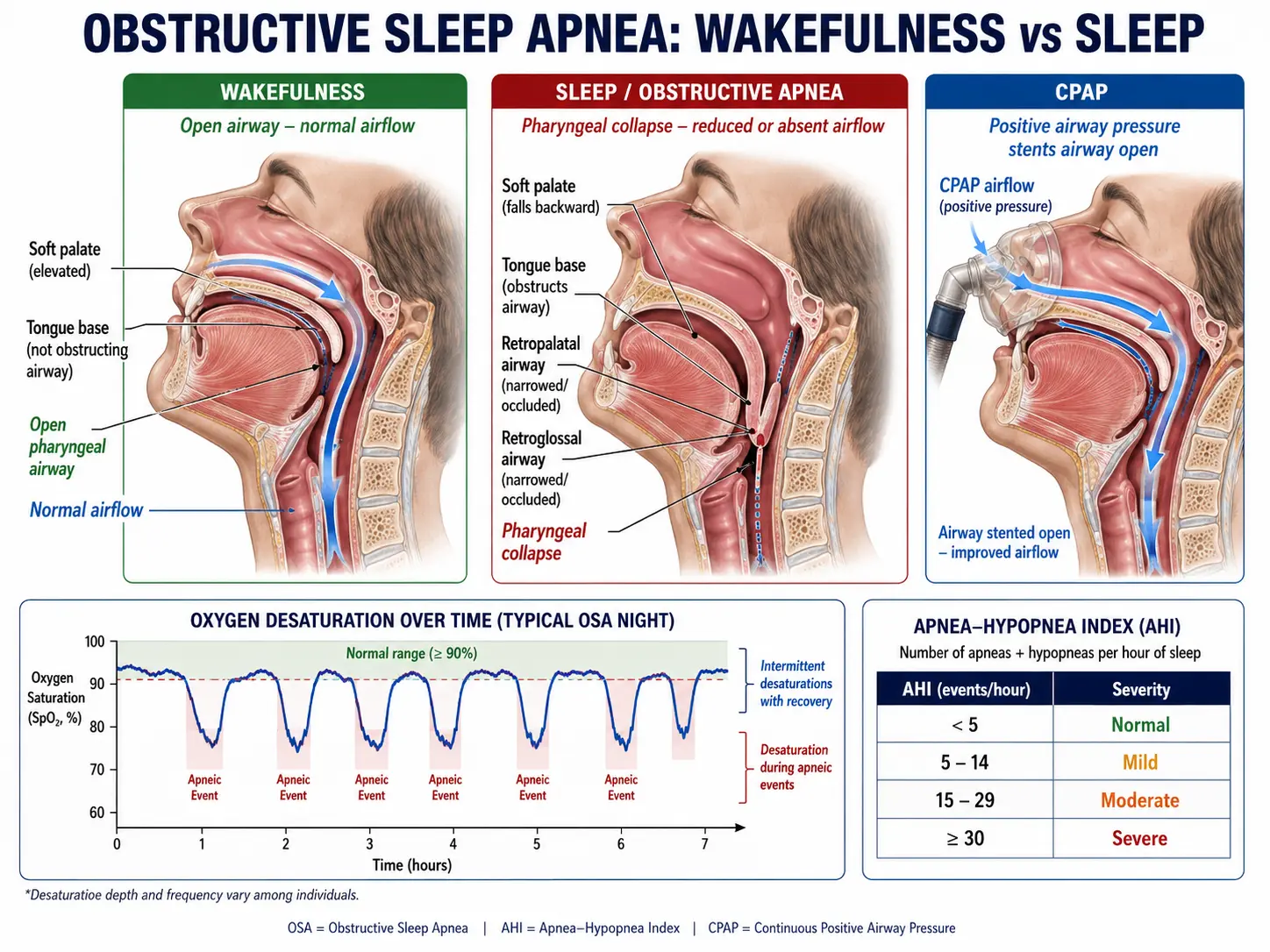
Table of Contents
- What is Obstructive Sleep Apnea?
- Common Symptoms of OSA
- Causes and Risk Factors
- Diagnosis
- Treatment Options
- Prevention and Management Strategies
- Complications of OSA
- Research Papers
- Connections
- Featured Videos
What is Obstructive Sleep Apnea?
Obstructive Sleep Apnea (OSA) is a sleep disorder in which breathing repeatedly stops and starts during sleep due to the relaxation and blockage of the upper airway. This can lead to disrupted sleep and reduced oxygen levels in the blood. OSA can affect overall health and increase the risk of various medical conditions.
Common Symptoms of OSA
- Loud snoring
- Gasping or choking during sleep
- Pauses in breathing: Witnessed by a partner or recorded by monitoring devices.
- Daytime sleepiness: Feeling excessively tired or drowsy during the day.
- Morning headaches
- Difficulty concentrating or memory problems
- Dry mouth or sore throat upon waking
- Restless sleep
Causes and Risk Factors
- Excess weight: A major risk factor due to fat deposits around the upper airway, which can obstruct breathing.
- Neck circumference: A larger neck can narrow the airway.
- Aging: OSA is more common in older adults.
- Gender: More common in men, but risk increases in women after menopause.
- Family history: Genetics can play a role in the likelihood of developing OSA.
- Nasal congestion: Difficulty breathing through the nose increases the risk of airway obstruction.
- Use of alcohol or sedatives: These relax the muscles in the throat, increasing the likelihood of airway obstruction.
Diagnosis
- Medical history and symptom review: Discuss symptoms with a healthcare provider.
- Physical examination: Includes checking for signs like enlarged tonsils or high blood pressure.
- Sleep study (polysomnography):
- In-lab sleep study: Monitors breathing, oxygen levels, and brain activity during sleep.
- Home sleep apnea test: A simplified test done at home to monitor heart rate, airflow, and breathing patterns.
Treatment Options
- Lifestyle changes:
- Weight loss: Reduces airway obstruction.
- Avoid alcohol and sedatives: Helps maintain muscle tone in the throat.
- Sleep position adjustment: Sleeping on the side instead of the back can reduce symptoms.
- Continuous Positive Airway Pressure (CPAP) therapy:
- Primary treatment for OSA. Uses a machine that delivers air pressure through a mask to keep the airway open.
- Oral appliances:
- Mouth guards: Custom-fitted devices that help keep the airway open by repositioning the jaw or tongue.
- Surgery:
- Uvulopalatopharyngoplasty (UPPP): Removes excess tissue from the throat to widen the airway.
- Tonsillectomy: For individuals with enlarged tonsils contributing to airway obstruction.
- Maxillomandibular advancement: Moves the upper and lower jaw forward to enlarge the space behind the tongue and soft palate.
Prevention and Management Strategies
- Maintain a healthy weight: Reduces the risk and severity of OSA.
- Exercise regularly: Helps manage weight and improve breathing.
- Limit alcohol and sedatives: Reduces relaxation of throat muscles.
- Sleep on your side: Helps keep the airway open during sleep.
- Maintain good sleep hygiene: Establish a regular sleep schedule and create a comfortable sleep environment.
Complications of OSA
- High blood pressure: OSA can worsen hypertension due to repeated drops in oxygen levels.
- Heart disease: Increased risk of heart attack, atrial fibrillation, and stroke.
- Type 2 diabetes: OSA is associated with an increased risk of insulin resistance.
- Daytime fatigue: Can lead to poor performance at work or school and an increased risk of accidents.
- Metabolic syndrome: A cluster of conditions that includes high blood pressure, high cholesterol, and obesity.
- Liver problems: Evidence of liver damage, more common in people with OSA.
References & Research
Historical Background
Obstructive sleep apnea was first formally described in 1965 by gastroenterologists Henri Gastaut, Carlo Alberto Tassinari, and Bernard Duron in France, who documented repeated airway obstructions during sleep. Colin Sullivan introduced continuous positive airway pressure (CPAP) therapy in 1981, revolutionizing the treatment of OSA and remaining the standard of care to this day.
Key Research Papers
- Dempsey JA, Veasey SC, Morgan BJ, O'Donnell CP. Pathophysiology of sleep apnea. Physiol Rev. 2010;90(1):47-112.
- Jordan AS, McSharry DG, Malhotra A. Adult obstructive sleep apnoea. Lancet. 2014;383(9918):736-747.
- Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med. 2002;165(9):1217-1239.
- McEvoy RD, Antic NA, Heeley E, et al. CPAP for prevention of cardiovascular events in obstructive sleep apnea (SAVE). N Engl J Med. 2016;375(10):919-931.
- Peppard PE, Young T, Barnet JH, et al. Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol. 2013;177(9):1006-1014.
- Kapur VK, Auckley DH, Chowdhuri S, et al. Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 2017;13(3):479-504.
- Sullivan CE, Issa FG, Berthon-Jones M, Eves L. Reversal of obstructive sleep apnoea by continuous positive airway pressure applied through the nares. Lancet. 1981;1(8225):862-865.
- Marin JM, Carrizo SJ, Vicente E, Agusti AG. Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure. Lancet. 2005;365(9464):1046-1053.
- Patil SP, Ayappa IA, Caples SM, et al. Treatment of adult obstructive sleep apnea with positive airway pressure: an American Academy of Sleep Medicine systematic review. J Clin Sleep Med. 2019;15(2):301-334.
- Levy P, Kohler M, McNicholas WT, et al. Obstructive sleep apnoea syndrome. Nat Rev Dis Primers. 2015;1:15015.
- Gottlieb DJ, Punjabi NM. Diagnosis and management of obstructive sleep apnea: a review. JAMA. 2020;323(14):1389-1400.
- Drager LF, Togeiro SM, Polotsky VY, Lorenzi-Filho G. Obstructive sleep apnea: a cardiometabolic risk in obesity and the metabolic syndrome. J Am Coll Cardiol. 2013;62(7):569-576.
Research Papers
The following PubMed topic searches surface the current peer-reviewed literature on Obstructive Sleep Apnea. Each link opens a live PubMed query; results update as new papers are indexed.
- PubMed search: obstructive sleep apnea
- PubMed search: OSA CPAP therapy
- PubMed search: OSA polysomnography AHI
- PubMed search: hypoglossal nerve stimulation sleep apnea
- PubMed search: OSA cardiovascular risk
- PubMed search: OSA obesity hypoventilation
- PubMed search: OSA hypertension
- PubMed search: OSA mandibular advancement device
- PubMed search: OSA surgery UPPP
- PubMed search: OSA pediatric adenotonsillectomy
- PubMed search: OSA insulin resistance
- PubMed search: OSA excessive daytime sleepiness
Connections
- Hypertension
- Atrial Fibrillation
- Sleep Hygiene
- Fatigue
- Pulmonary Hypertension
- Magnesium
- Brain Fog
- Insomnia
- Headache
- Obesity
- Metabolic Syndrome
- Insulin Resistance
- Stroke
- Heart Failure
- Arrhythmia
- Anxiety
- Anemia
- Mouth Taping