Insomnia
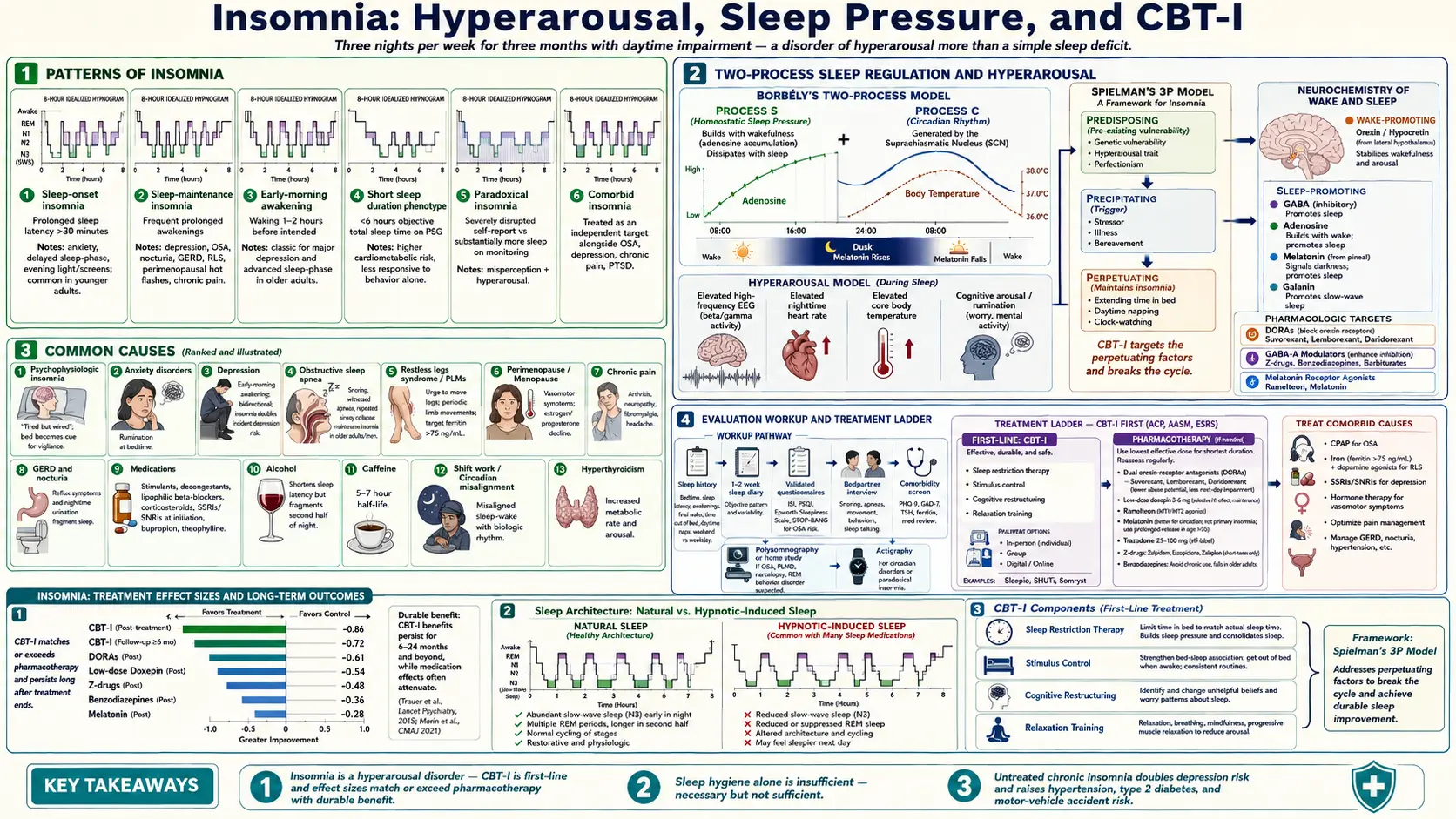

Table of Contents
- Overview
- Types of Insomnia
- Common Causes
- Mechanisms
- Evaluation
- Management
- When to Seek Medical Care
- Connections
- References & Research
- Featured Videos
Overview
Insomnia is dissatisfaction with sleep quantity or quality, characterized by difficulty initiating sleep, difficulty maintaining sleep, or early-morning awakening with inability to return to sleep. The International Classification of Sleep Disorders, Third Edition (ICSD-3) defines chronic insomnia disorder as sleep difficulty occurring at least three nights per week for at least three months, despite adequate opportunity for sleep, and accompanied by clinically meaningful daytime impairment — fatigue, mood disturbance, cognitive dysfunction, or impaired social or occupational performance. Insomnia affects roughly 10 percent of adults as a chronic disorder and another 20–30 percent in transient or short-term form. It is more common in women, older adults, shift workers, and people with psychiatric or chronic-pain comorbidities. Untreated chronic insomnia is associated with increased risk of depression, anxiety disorders, hypertension, type 2 diabetes, and motor-vehicle accidents.
Types of Insomnia
- Sleep-onset insomnia — difficulty falling asleep at the desired bedtime, with sleep latency typically exceeding 30 minutes. Most common in younger adults and frequently tied to anxiety, delayed sleep-phase tendency, or evening light/screen exposure.
- Sleep-maintenance insomnia — frequent or prolonged awakenings during the night with difficulty returning to sleep. Often reflects depression, OSA, nocturia, GERD, restless legs syndrome, perimenopausal hot flashes, or chronic pain.
- Early-morning awakening — waking 1–2 hours before the intended rise time and being unable to resume sleep. Classically associated with major depression and with advanced sleep-phase tendency in older adults.
- Short sleep duration phenotype — chronic insomnia with objectively documented short total sleep time (typically <6 hours on polysomnography). Carries a higher cardiometabolic risk profile and tends to respond less robustly to behavioral therapy alone.
- Paradoxical insomnia — the patient reports severely disrupted or absent sleep, yet objective monitoring shows substantially more sleep than perceived. Driven by misperception and hyperarousal rather than true sleep deficit.
- Comorbid insomnia — insomnia occurring alongside another medical or psychiatric disorder (depression, OSA, chronic pain, PTSD). The current consensus is to treat insomnia as an independent target rather than waiting for the comorbid condition to remit.
Common Causes
- Psychophysiologic insomnia — conditioned arousal in which the bed and bedroom become cues for wakefulness rather than sleep. Patients describe themselves as “tired but wired” and often sleep better away from home.
- Anxiety disorders — rumination, worry, and elevated cognitive arousal at bedtime are among the most common drivers of sleep-onset insomnia.
- Depression — characteristically causes early-morning awakening; bidirectional risk — insomnia roughly doubles the risk of incident depression.
- Obstructive sleep apnea (OSA) — repeated airway collapse fragments sleep and presents as maintenance insomnia, especially in older adults, men, and people with snoring or witnessed apneas.
- Restless legs syndrome and periodic limb movements — uncomfortable evening leg sensations relieved by movement; PLMs cause repetitive arousals during sleep.
- Perimenopause and menopause — vasomotor symptoms, declining estrogen and progesterone, and increased OSA risk all contribute to maintenance insomnia in midlife women.
- Chronic pain — arthritis, neuropathy, fibromyalgia, and headache disorders disrupt sleep architecture and lower arousal threshold.
- GERD and nocturia — nocturnal reflux and frequent voiding fragment sleep; often overlooked as primary contributors.
- Medications — stimulants, decongestants (pseudoephedrine), beta-blockers (especially lipophilic ones like propranolol), corticosteroids, SSRIs and SNRIs at initiation, bupropion, theophylline, and rebound from sedative-hypnotic withdrawal.
- Alcohol and caffeine — alcohol shortens sleep latency but fragments the second half of the night; caffeine has a 5–7 hour half-life and impairs sleep even when consumed in early afternoon.
- Shift work and circadian misalignment — rotating or night shifts, jet lag, and delayed sleep-phase tendency create a mismatch between the internal clock and the desired sleep schedule.
- Hyperthyroidism — elevated thyroid hormone increases arousal, heart rate, and core body temperature, all of which oppose sleep.
Mechanisms
Insomnia is best understood as a disorder of hyperarousal rather than a simple sleep deficit. Several overlapping models inform current diagnosis and treatment:
- Hyperarousal model — chronic insomnia is associated with elevated cortical activity (high-frequency EEG during sleep), autonomic arousal (elevated heart rate and core temperature at night), and cognitive arousal (rumination, worry about sleep itself). Treatment that reduces arousal — behavioral, cognitive, or pharmacologic — outperforms treatment that simply forces sleep.
- Two-process model of sleep regulation — sleep timing reflects the interaction of Process S (homeostatic sleep pressure that builds with wakefulness, mediated by adenosine) and Process C (the circadian clock in the suprachiasmatic nucleus). Insomnia can arise from inadequate sleep pressure (excessive napping, low daytime activity) or from circadian misalignment (delayed or advanced phase).
- Spielman’s 3P model — predisposing factors (genetic vulnerability, hyperarousal trait, perfectionism), a precipitating event (stressor, illness, bereavement), and perpetuating behaviors (extending time in bed, daytime napping, clock-watching, anticipatory anxiety) explain why acute insomnia transitions to chronic disorder. CBT-I is designed to dismantle the perpetuating behaviors.
- Sleep-related cognitions — catastrophic thoughts about the consequences of poor sleep amplify autonomic arousal and create a self-fulfilling cycle. The bed becomes a stimulus for vigilance rather than sleep.
- Neurochemistry — orexin (hypocretin) drives wakefulness; GABA, adenosine, melatonin, and galanin promote sleep. Modern hypnotics target these pathways — orexin antagonists (DORAs), GABA-A modulators (Z-drugs, benzodiazepines), and melatonin-receptor agonists.
Evaluation
Evaluation centers on a careful sleep history and is largely clinical. Polysomnography is reserved for cases where a sleep-disordered breathing or movement disorder is suspected.
- Sleep history — bedtime, sleep latency, number and duration of awakenings, final wake time, time out of bed, daytime napping, weekend versus weekday pattern, snoring, witnessed apneas, leg discomfort, and dream behaviors.
- Sleep diary — one to two weeks of self-reported bedtime, sleep latency, awakenings, and rise time. Reveals patterns invisible in a single recall and is the cornerstone of CBT-I.
- Validated questionnaires — the Insomnia Severity Index (ISI) grades severity and tracks treatment response; the Pittsburgh Sleep Quality Index (PSQI) screens for global sleep dysfunction; the Epworth Sleepiness Scale quantifies daytime sleepiness; the STOP-BANG screens for OSA risk.
- Bedpartner interview — essential for identifying snoring, witnessed apneas, periodic limb movements, and parasomnias the patient may not be aware of.
- Targeted comorbidity screen — PHQ-9 for depression, GAD-7 for anxiety, TSH for thyroid disease, ferritin for restless legs syndrome (target >75 ng/mL), and a medication review.
- Polysomnography (in-lab or home study) — indicated when OSA, periodic limb movement disorder, narcolepsy, or REM-sleep behavior disorder is suspected; not routinely required to diagnose insomnia itself.
- Actigraphy — wrist-worn motion monitoring useful for circadian-rhythm disorders, paradoxical insomnia, and objective treatment monitoring.
Management
- Cognitive behavioral therapy for insomnia (CBT-I) — first-line. The American College of Physicians, the American Academy of Sleep Medicine, and the European Sleep Research Society all recommend CBT-I as the initial treatment for chronic insomnia in adults. Core components are sleep restriction (limiting time in bed to actual sleep time, then gradually extending), stimulus control (reserving the bed for sleep, getting up if not asleep within 15–20 minutes), cognitive restructuring (challenging catastrophic thoughts about sleep), and relaxation training. Effect sizes match or exceed pharmacotherapy and persist long after treatment ends. Delivered in person, in groups, or via digital programs (Sleepio, SHUTi, Somryst).
- Sleep hygiene alone is insufficient — recommendations such as avoiding caffeine and keeping a regular schedule are necessary but rarely sufficient for chronic insomnia. Sleep hygiene is a component of CBT-I, not a substitute.
- Dual orexin-receptor antagonists (DORAs) — suvorexant, lemborexant, and daridorexant block wake-promoting orexin signaling. Lower abuse potential and less next-day impairment than benzodiazepines or Z-drugs; preferred when long-term pharmacotherapy is needed.
- Low-dose doxepin (3–6 mg) — selective H1 antihistamine effect at this dose; FDA-approved for sleep maintenance with minimal anticholinergic burden.
- Ramelteon — melatonin MT1/MT2 agonist; modest effect on sleep onset, no abuse potential, useful in older adults.
- Melatonin — immediate-release melatonin has limited efficacy for primary insomnia but is useful for circadian-rhythm disorders (delayed sleep-phase, jet lag, shift work). Prolonged-release formulations have a stronger evidence base in adults over 55.
- Trazodone — off-label sedating antidepressant widely prescribed for insomnia at 25–100 mg; modest evidence, but useful in patients with concurrent depression or anxiety.
- Z-drugs — zolpidem, eszopiclone, zaleplon; effective short-term but carry risks of complex sleep behaviors, next-day impairment, dependence, and rebound insomnia. Use the lowest effective dose for the shortest duration.
- Benzodiazepines — temazepam, triazolam; effective but generally avoided for chronic use because of tolerance, dependence, falls, and cognitive impairment in older adults.
- Treat comorbid conditions directly — CPAP for OSA, iron repletion plus dopamine agonists or alpha-2-delta ligands for RLS, SSRIs/SNRIs for anxiety and depression, hormone therapy or non-hormonal options for vasomotor symptoms.
- Honest discussion of hypnotic-induced sleep — sedative hypnotics produce sleep that differs from natural sleep in EEG architecture (often less slow-wave and REM sleep), and the subjective improvement may exceed the objective improvement. Patients should understand this when weighing long-term medication versus CBT-I.
When to Seek Medical Care
- Sleep difficulty present three or more nights per week for more than three months with daytime impairment.
- Loud snoring, witnessed apneas, gasping awakenings, or unrefreshing sleep despite adequate time in bed (consider OSA).
- Depression, hopelessness, or thoughts of self-harm or suicide.
- Acting out of dreams, sleepwalking, or other parasomnia behaviors that pose a safety risk.
- Excessive daytime sleepiness with episodes of falling asleep at the wheel or during conversations (consider narcolepsy or severe OSA).
- Sudden worsening of insomnia in older adults — can herald depression, dementia, delirium, or a new medical illness.
- Evening leg discomfort relieved by movement (restless legs syndrome).
- Insomnia tied to a new medication, dose change, or substance (alcohol, cannabis, stimulants).
Connections
- Depression
- Anxiety
- Chronic Pain
- Obstructive Sleep Apnea
- Fatigue
- Fibromyalgia
- Magnesium
- Brain Fog
- Heart Palpitations
- Hashimoto's Thyroiditis
- Graves' Disease
- Insomnia (Psychiatry)
- Sleep Hygiene
- Headache
- PTSD
- Hormone Panel
- Lemon Balm
- Adrenal Fatigue
References & Research
Historical Background
Insomnia has been described for as long as medicine has been written. Hippocrates noted that sleep disturbance accompanied many illnesses and that prolonged sleeplessness foreshadowed worsening disease. For most of the twentieth century, insomnia was treated as a symptom of psychiatric or medical disease rather than a disorder in its own right, and pharmacotherapy with barbiturates and later benzodiazepines was the dominant approach. The intellectual turning point came in 1973, when Arthur Spielman began developing the sleep restriction technique that would become a pillar of modern behavioral treatment, followed by his 3P model of predisposing, precipitating, and perpetuating factors. Through the 1980s and 1990s, Charles Morin, Richard Bootzin (stimulus control), and others assembled these techniques into cognitive behavioral therapy for insomnia (CBT-I). Trazodone began being used off-label for sleep in the 1980s. The first orexin-receptor antagonist, suvorexant, received FDA approval in 2014, marking the first new pharmacologic mechanism for insomnia in decades, and was followed by lemborexant (2019) and daridorexant (2022). The 2016 American College of Physicians guideline formally elevated CBT-I to first-line treatment for chronic insomnia, a position now reflected in every major international guideline.
Key Research Papers
- Morin CM, Benca R. Chronic insomnia. The Lancet. 2012;379(9821):1129-1141.
- Qaseem A, Kansagara D, Forciea MA, Cooke M, Denberg TD. Management of chronic insomnia disorder in adults: a clinical practice guideline from the American College of Physicians. Annals of Internal Medicine. 2016;165(2):125-133.
- Sateia MJ, Buysse DJ, Krystal AD, Neubauer DN, Heald JL. Clinical practice guideline for the pharmacologic treatment of chronic insomnia in adults: an American Academy of Sleep Medicine clinical practice guideline. Journal of Clinical Sleep Medicine. 2017;13(2):307-349.
- Edinger JD, Arnedt JT, Bertisch SM, et al. Behavioral and psychological treatments for chronic insomnia disorder in adults: an American Academy of Sleep Medicine clinical practice guideline. Journal of Clinical Sleep Medicine. 2021;17(2):255-262.
- Herring WJ, Snyder E, Budd K, et al. Orexin receptor antagonism for treatment of insomnia: a randomized clinical trial of suvorexant. Neurology. 2012;79(23):2265-2274.
- Krystal AD, Durrence HH, Scharf M, et al. Efficacy and safety of doxepin 1 mg, 3 mg, and 6 mg in adults with primary insomnia. Sleep. 2010;33(11):1553-1561.
- Spielman AJ, Saskin P, Thorpy MJ. Treatment of chronic insomnia by restriction of time in bed. Sleep. 1987;10(1):45-56.
- Morin CM, Hauri PJ, Espie CA, Spielman AJ, Buysse DJ, Bootzin RR. Nonpharmacologic treatment of chronic insomnia. Sleep. 1999;22(8):1134-1156.
- Riemann D, Baglioni C, Bassetti C, et al. European guideline for the diagnosis and treatment of insomnia. Journal of Sleep Research. 2017;26(6):675-700.
- Mignot E, Mayleben D, Fietze I, et al. Safety and efficacy of daridorexant in patients with insomnia disorder: results from two multicentre, randomised, double-blind, placebo-controlled, phase 3 trials. The Lancet Neurology. 2022;21(2):125-139.
PubMed Topic Searches
- Chronic insomnia disorder
- Cognitive behavioral therapy for insomnia (CBT-I)
- Hyperarousal in insomnia
- Orexin-receptor antagonists for insomnia
- Sleep restriction therapy
- Insomnia and depression: bidirectional risk