Probiotics: Restoring Balance Through Beneficial Microorganisms
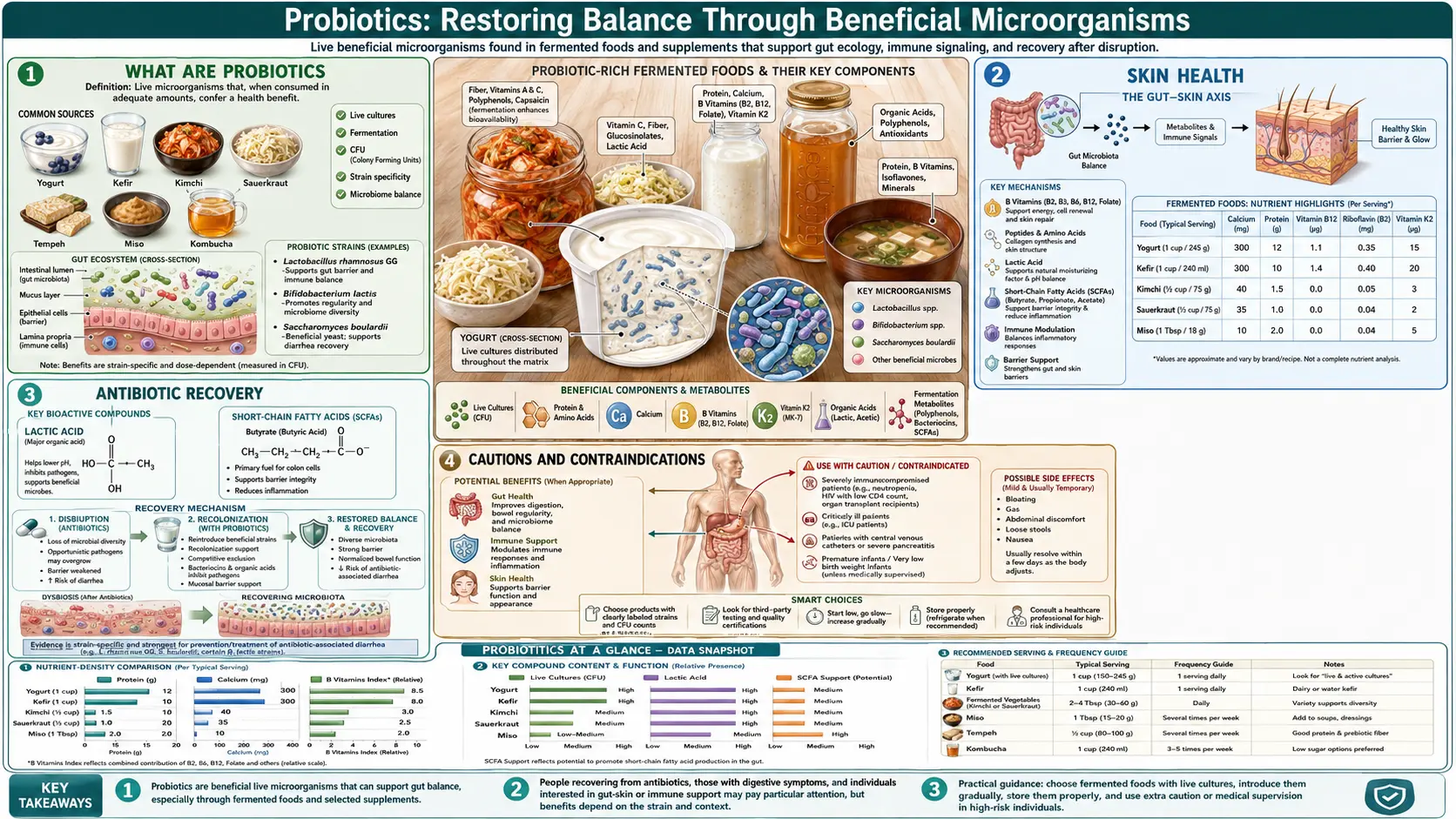

Table of Contents
- What Are Probiotics
- The Gut Microbiome
- Key Probiotic Strains
- Digestive Health
- Immune System Modulation
- Gut-Brain Axis and Mental Health
- Skin Health
- Weight Management
- Cardiovascular Benefits
- Oral Health
- Vaginal and Urinary Tract Health
- Antibiotic Recovery
- Food Sources vs Supplements
- CFU Counts and Strain Diversity
- Prebiotics as Probiotic Fuel
- Spore-Based vs Traditional Probiotics
- Recommended Dosage
- Cautions and Contraindications
- Research Papers
- Connections
- Featured Videos
What Are Probiotics
Probiotics are live beneficial microorganisms that, when consumed in adequate amounts, confer a measurable health benefit on the host. The term itself derives from the Latin pro (for) and the Greek bios (life), literally meaning "for life." These organisms include specific strains of bacteria, yeasts, and other microbes that have co-evolved with the human body over hundreds of thousands of years.
From a naturopathic perspective, probiotics represent one of the most fundamental tools for restoring health. The principle of treating the root cause rather than merely suppressing symptoms aligns perfectly with probiotic therapy, which works by re-establishing the microbial equilibrium that underlies so many aspects of wellness. Rather than introducing a foreign pharmaceutical agent, we are replenishing organisms that belong in the human ecosystem.
Not all bacteria are created equal. To qualify as a true probiotic, an organism must meet several criteria: it must survive the acidic environment of the stomach, it must be able to colonize or at least transiently inhabit the intestinal tract, it must demonstrate a clinically validated health benefit, and it must be safe for human consumption. Many commercially available products fail to meet one or more of these standards, making informed selection essential.
The Gut Microbiome
The human gut microbiome is a staggeringly complex ecosystem. It contains approximately 100 trillion microorganisms, outnumbering our own human cells by a factor of roughly ten to one. This microbial community weighs between 3 and 5 pounds in a healthy adult, making it comparable in mass to the brain or the liver. It is, in many respects, a hidden organ performing functions essential to survival.
The microbiome houses over 1,000 distinct species of bacteria, along with viruses, fungi, archaea, and other microorganisms. The diversity and balance among these species determines whether the gut environment promotes health or disease. A diverse microbiome with a robust population of beneficial organisms creates a resilient ecosystem capable of resisting pathogenic invasion, producing essential nutrients, and regulating immune function.
In naturopathic medicine, we recognize that modern life has placed the microbiome under unprecedented stress. Antibiotic overuse, processed food consumption, chronic stress, caesarean section births, formula feeding, environmental toxin exposure, and excessive hygiene practices have all contributed to widespread microbial depletion. This phenomenon, sometimes called dysbiosis, is increasingly linked to the epidemic rise in chronic diseases seen across industrialized nations.
The microbiome begins forming at birth, with vaginal delivery and breastfeeding providing the foundational inoculation of beneficial organisms. By approximately age three, the core microbiome is established, though it remains responsive to dietary and environmental influences throughout life. This plasticity is precisely what makes probiotic therapy so promising.
Key Probiotic Strains
Understanding the major probiotic genera and species is essential for targeted therapeutic use. Each strain possesses unique properties and clinical applications.
Lactobacillus
The Lactobacillus genus is among the most extensively researched probiotic groups. These lactic acid-producing bacteria naturally inhabit the small intestine, mouth, and vaginal tract. Key species include Lactobacillus acidophilus, which supports lactose digestion and vaginal health; Lactobacillus rhamnosus GG, one of the most clinically studied strains for diarrhea prevention and immune support; Lactobacillus plantarum, valued for its anti-inflammatory properties and ability to strengthen the intestinal barrier; and Lactobacillus reuteri, which produces antimicrobial compounds called reuterin and supports oral and gastrointestinal health.
Bifidobacterium
Bifidobacterium species are predominant inhabitants of the large intestine and are among the first colonizers of the infant gut. Bifidobacterium longum is noted for its ability to reduce anxiety and cortisol levels. Bifidobacterium infantis is critical for infant gut development and has shown efficacy in irritable bowel syndrome. Bifidobacterium lactis enhances immune function and has demonstrated benefits for constipation relief. These organisms produce short-chain fatty acids, particularly acetate and lactate, which nourish colonic cells and maintain an acidic environment hostile to pathogens.
Saccharomyces boulardii
Saccharomyces boulardii is a beneficial yeast, distinct from bacterial probiotics, that offers unique advantages. Because it is a yeast, it is inherently resistant to antibiotics, making it particularly valuable during and after antibiotic therapy. It has strong evidence for preventing and treating Clostridioides difficile infection, traveler's diarrhea, and acute gastroenteritis. It works by producing proteases that break down bacterial toxins and by stimulating secretory immunoglobulin A production.
Bacillus coagulans
Bacillus coagulans is a spore-forming probiotic that offers exceptional stability. Its spore form allows it to survive extreme temperatures, stomach acid, and bile salts with ease. Once it reaches the intestine, it germinates into an active, lactic acid-producing organism. Clinical studies have demonstrated its efficacy for irritable bowel syndrome symptoms, rheumatoid arthritis, and immune enhancement. Its shelf stability makes it a practical choice for supplementation without refrigeration.
Digestive Health
The most well-established application of probiotics lies in digestive health, where they address a wide spectrum of gastrointestinal complaints.
Irritable Bowel Syndrome (IBS): Probiotics have become a cornerstone of naturopathic IBS management. Multiple meta-analyses confirm that specific strains, particularly Bifidobacterium infantis 35624, Lactobacillus plantarum 299v, and multi-strain formulations, significantly reduce abdominal pain, bloating, and irregular bowel habits. Probiotics address IBS at its root by reducing visceral hypersensitivity, modulating serotonin production in the gut, and restoring the integrity of the intestinal barrier.
Bloating and Gas: Excessive bloating often results from an overgrowth of gas-producing bacteria or from impaired carbohydrate fermentation. Probiotics help by competing with gas-producing organisms for resources, producing enzymes that aid in the breakdown of complex carbohydrates, and restoring a fermentation profile that generates less hydrogen and methane.
Diarrhea: Probiotics have robust evidence for several types of diarrhea. They reduce the duration of acute infectious diarrhea by approximately one day, decrease the risk of antibiotic-associated diarrhea by 42 percent, and significantly lower the incidence of traveler's diarrhea. Saccharomyces boulardii and Lactobacillus rhamnosus GG are the most effective strains for diarrheal conditions.
Constipation: Certain probiotic strains accelerate gut transit time and increase stool frequency. Bifidobacterium lactis has been shown in clinical trials to increase bowel movements by an average of 1.5 per week compared to placebo. Probiotics address constipation by producing short-chain fatty acids that stimulate peristalsis, increasing mucus production for easier stool passage, and modulating the enteric nervous system.
Immune System Modulation
One of the most profound insights of modern immunology is that approximately 70 to 80 percent of the entire immune system resides in the gut. The gut-associated lymphoid tissue (GALT) represents the largest immune organ in the body, and the microbiome plays a central role in training, calibrating, and activating immune responses.
Probiotics modulate the immune system through several mechanisms. They stimulate the production of secretory immunoglobulin A (sIgA), the first line of defense at mucosal surfaces. They enhance the activity of natural killer cells, which patrol the body for virally infected and cancerous cells. They promote the maturation of dendritic cells, which serve as key antigen-presenting cells that bridge innate and adaptive immunity. They also regulate the balance between pro-inflammatory T-helper 1 and T-helper 17 cells and anti-inflammatory regulatory T cells.
From a naturopathic standpoint, the immune-modulating capacity of probiotics is particularly relevant for individuals who experience frequent infections, slow wound healing, or chronic inflammatory conditions. Clinical trials have demonstrated that probiotic supplementation reduces the incidence of upper respiratory tract infections by approximately 25 percent and shortens the duration of colds by nearly two days. In children attending daycare, probiotics significantly reduce the number of sick days and antibiotic prescriptions.
Importantly, probiotics do not simply "boost" the immune system in a one-dimensional way. They modulate it, meaning they can upregulate immune responses when needed and downregulate them when overactivity leads to autoimmunity or allergy. This bidirectional regulation is what makes probiotics such a sophisticated therapeutic tool.
Gut-Brain Axis and Mental Health
The gut-brain axis is a bidirectional communication network linking the enteric nervous system of the gastrointestinal tract with the central nervous system of the brain. This connection operates through the vagus nerve, the endocrine system, immune signaling molecules, and microbial metabolites. The emerging field of psychobiotics studies specific probiotic strains that confer mental health benefits through this axis.
The gut produces approximately 90 percent of the body's serotonin and significant quantities of dopamine, gamma-aminobutyric acid (GABA), and other neurotransmitters. The microbiome directly influences the production and availability of these signaling molecules. When the microbiome is disrupted, neurotransmitter production can become impaired, contributing to mood disorders, anxiety, and cognitive dysfunction.
Clinical studies on psychobiotics have yielded encouraging results. Lactobacillus rhamnosus has been shown to reduce anxiety-like behavior and modulate GABA receptor expression via the vagus nerve. Bifidobacterium longum 1714 has demonstrated stress-reducing effects in healthy volunteers, lowering cortisol levels and improving cognitive performance under pressure. A combination of Lactobacillus helveticus and Bifidobacterium longum reduced depression and anxiety scores in a randomized controlled trial.
In naturopathic practice, addressing gut health is considered a foundational step in managing mood disorders. Rather than viewing the brain in isolation, we recognize it as part of an interconnected system where gastrointestinal health, microbial balance, inflammation, and nutrient status all converge to influence mental well-being. Probiotics represent a safe, well-tolerated intervention that addresses this interconnection directly.
Skin Health
The connection between gut health and skin health has been recognized in naturopathic medicine for over a century, and modern research has validated this relationship through the concept of the gut-skin axis. Intestinal dysbiosis increases systemic inflammation, impairs nutrient absorption, and compromises immune regulation, all of which manifest on the skin.
Eczema (Atopic Dermatitis): Probiotics have the strongest dermatological evidence for eczema prevention and management. Prenatal and early postnatal supplementation with Lactobacillus rhamnosus GG has been shown to reduce the incidence of eczema in high-risk infants by up to 50 percent. In established eczema, probiotics reduce symptom severity scores by modulating the Th1/Th2 immune balance that underlies atopic disease.
Acne: The gut-skin connection in acne involves increased intestinal permeability, systemic inflammation, and insulin/IGF-1 signaling. Probiotics address acne by reducing intestinal permeability (sometimes called "leaky gut"), decreasing circulating inflammatory cytokines, and modulating the mTOR pathway involved in sebum production. Oral probiotics containing Lactobacillus acidophilus and Bifidobacterium bifidum have shown clinical improvements in acne severity.
Rosacea: The association between rosacea and small intestinal bacterial overgrowth (SIBO) highlights the gut-skin connection. Studies have found that eradication of SIBO leads to significant improvement or complete remission of rosacea in a majority of patients. Probiotics support this process by restoring healthy small intestinal ecology and reducing the inflammatory cascade that drives rosacea flares.
Weight Management
The microbiome plays a significant role in energy extraction from food, fat storage signaling, appetite regulation, and metabolic inflammation, all of which influence body weight. Research has revealed that the gut microbiome composition of lean individuals differs systematically from that of obese individuals, with obesity associated with reduced microbial diversity and an altered ratio of major bacterial phyla.
Specific probiotic strains have demonstrated weight management benefits in clinical trials. Lactobacillus gasseri SBT2055 reduced abdominal fat by 8.5 percent over 12 weeks in a Japanese study. Lactobacillus rhamnosus CGMCC1.3724 helped women lose 50 percent more weight than placebo over a 24-week period. Multi-strain formulations have been shown to reduce waist circumference, body mass index, and markers of metabolic inflammation.
Probiotics influence weight through several pathways. They produce short-chain fatty acids that signal satiety to the brain via the gut-brain axis. They reduce the extraction of calories from food by shifting the fermentation profile in the colon. They decrease metabolic endotoxemia, a condition where bacterial lipopolysaccharides leak into the bloodstream and trigger inflammation that promotes insulin resistance and fat storage. They also modulate the production of hormones such as GLP-1 and peptide YY that regulate appetite and glucose metabolism.
Cardiovascular Benefits
Emerging research has identified several mechanisms through which probiotics support cardiovascular health. The microbiome influences cholesterol metabolism, blood pressure regulation, and systemic inflammation, all major risk factors for heart disease.
Certain Lactobacillus strains produce bile salt hydrolase, an enzyme that deconjugates bile acids in the intestine. This process forces the liver to draw upon circulating cholesterol to synthesize new bile acids, effectively lowering serum cholesterol levels. A meta-analysis of randomized controlled trials found that probiotic supplementation reduced total cholesterol by an average of 7.8 mg/dL and LDL cholesterol by 7.3 mg/dL, with Lactobacillus reuteri NCIMB 30242 showing particularly strong effects.
Probiotics also contribute to blood pressure regulation. A meta-analysis of nine trials found that probiotic consumption reduced systolic blood pressure by 3.56 mmHg and diastolic blood pressure by 2.38 mmHg. These effects are mediated through the production of bioactive peptides that inhibit the angiotensin-converting enzyme (ACE), improved endothelial function, and reduced systemic inflammation.
Additionally, the gut microbiome influences the production of trimethylamine N-oxide (TMAO), a metabolite strongly associated with atherosclerosis and cardiovascular events. Probiotics can reduce TMAO production by altering the microbial conversion of dietary choline and carnitine, potentially decreasing cardiovascular risk through this pathway.
Oral Health
The oral microbiome is the second most diverse microbial community in the human body, harboring over 700 species. Dysbiosis of the oral microbiome contributes to dental caries, periodontal disease, halitosis, and oral candidiasis. Probiotic therapy for oral health represents a paradigm shift from the antimicrobial approach of conventional dentistry to an ecological approach that favors beneficial organisms.
Lactobacillus reuteri strains have demonstrated the ability to reduce gingival bleeding, pocket depth in periodontal disease, and levels of pathogenic organisms such as Porphyromonas gingivalis and Streptococcus mutans. Streptococcus salivarius K12 produces bacteriocin-like inhibitory substances that suppress the bacteria responsible for halitosis and streptococcal pharyngitis.
Probiotic lozenges and oral-specific formulations are increasingly available and provide targeted delivery of beneficial organisms to the oral cavity. In naturopathic practice, oral probiotics are recommended as adjunctive therapy alongside good oral hygiene, particularly for patients with recurrent gum disease, chronic bad breath, or frequent upper respiratory infections.
Vaginal and Urinary Tract Health
The vaginal microbiome is dominated by Lactobacillus species, which maintain an acidic pH of 3.8 to 4.5, produce hydrogen peroxide and bacteriocins, and compete with pathogenic organisms for adhesion sites. When this Lactobacillus-dominant ecology is disrupted, conditions such as bacterial vaginosis, vulvovaginal candidiasis, and urinary tract infections become significantly more likely.
Probiotic supplementation with vaginal-specific strains, particularly Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14, has been shown to restore healthy vaginal flora, reduce recurrence of bacterial vaginosis, and decrease the incidence of urinary tract infections. These strains can be administered both orally and intravaginally. Oral administration is effective because Lactobacillus strains can transit from the intestine to the vaginal tract via the perineum.
For women experiencing recurrent urinary tract infections, probiotics offer a compelling alternative to repeated antibiotic courses, which perpetuate dysbiosis and promote antimicrobial resistance. A study comparing Lactobacillus prophylaxis to low-dose trimethoprim-sulfamethoxazole found comparable UTI prevention rates, establishing probiotics as a viable non-antibiotic strategy. In naturopathic practice, vaginal probiotics are often combined with cranberry extract, D-mannose, and adequate hydration for comprehensive urinary tract support.
Antibiotic Recovery
Antibiotic therapy, while sometimes necessary and life-saving, inflicts significant collateral damage on the gut microbiome. A single course of broad-spectrum antibiotics can reduce microbial diversity by 25 percent, and some species may not recover for months or even years. Repeated antibiotic courses compound this damage, leading to progressive microbial depletion that increases susceptibility to opportunistic infections, particularly Clostridioides difficile.
Probiotic supplementation during and after antibiotic therapy is one of the most evidence-based applications in the field. A Cochrane review of 31 randomized trials found that probiotics reduce the risk of antibiotic-associated diarrhea by 42 percent. Saccharomyces boulardii is especially valuable during antibiotic courses because, as a yeast, it is unaffected by antibacterial agents and can maintain gut ecological stability while antibiotics eliminate bacterial populations.
From a naturopathic perspective, the post-antibiotic recovery protocol should be comprehensive. It begins with probiotic supplementation started at the onset of antibiotic therapy (taken at least 2 hours apart from the antibiotic dose) and continuing for at least 4 weeks after the course is completed. This is complemented by prebiotic-rich foods to nourish recovering bacterial populations, fermented foods to provide diverse microbial exposure, and bone broth or L-glutamine to support intestinal barrier repair.
Food Sources vs Supplements
Both fermented foods and probiotic supplements offer therapeutic value, but they differ in important ways. A comprehensive naturopathic approach typically incorporates both, recognizing that they serve complementary functions.
Fermented Food Sources:
- Yogurt: Contains Lactobacillus bulgaricus and Streptococcus thermophilus; choose plain, unsweetened varieties with live active cultures
- Kefir: A more diverse probiotic source than yogurt, containing up to 61 distinct microbial strains including beneficial yeasts
- Sauerkraut: Raw, unpasteurized sauerkraut provides Lactobacillus plantarum and other lactic acid bacteria along with prebiotic fiber
- Kimchi: Korean fermented vegetables rich in Lactobacillus kimchii and other unique strains, along with vitamins and antioxidants
- Kombucha: Fermented tea containing a symbiotic culture of bacteria and yeast (SCOBY), providing organic acids and diverse probiotics
- Miso and Tempeh: Fermented soy products offering Bacillus subtilis and other beneficial organisms alongside complete protein
- Kvass: Traditional fermented beet beverage rich in Lactobacillus species and beneficial enzymes
Advantages of Food Sources: Fermented foods provide probiotics in a food matrix that includes prebiotics, enzymes, vitamins, and organic acids that enhance microbial survival and activity. They deliver a broader diversity of organisms than most supplements and have been consumed safely by human cultures for thousands of years.
Advantages of Supplements: Supplements provide specific, clinically studied strains at precise, standardized doses. They are essential when therapeutic CFU counts are needed, when targeting specific health conditions with evidence-based strains, or when dietary preferences or sensitivities limit fermented food intake.
CFU Counts and Strain Diversity
Colony Forming Units (CFUs) represent the number of viable, living organisms in a probiotic product. Understanding CFU counts and strain diversity is critical for selecting effective formulations.
General CFU Guidelines:
- General maintenance: 5 to 10 billion CFUs daily
- Active digestive support: 15 to 30 billion CFUs daily
- Therapeutic applications: 50 to 100 billion CFUs daily or higher, depending on the condition
- Post-antibiotic recovery: 50 to 100 billion CFUs daily for 4 to 8 weeks
However, more is not always better. The specific strain matters more than the total CFU count. A product containing 5 billion CFUs of a well-studied, clinically validated strain may be more effective than a product containing 100 billion CFUs of poorly characterized organisms. Always look for products that identify organisms to the strain level (genus, species, and strain designation), not merely to the species level.
Strain Diversity: Multi-strain formulations often outperform single-strain products in clinical trials because different strains colonize different niches within the gut, produce different metabolites, and modulate different aspects of immune function. A well-designed multi-strain probiotic typically contains 8 to 15 complementary strains spanning the Lactobacillus, Bifidobacterium, and sometimes Streptococcus or Bacillus genera.
Quality matters enormously in the supplement market. Look for products that guarantee CFU counts at the time of expiration (not at the time of manufacture), that have undergone third-party testing for potency and purity, and that specify proper storage conditions. Many probiotics require refrigeration, though spore-based and certain encapsulated products are shelf-stable.
Prebiotics as Probiotic Fuel
Prebiotics are non-digestible fibers and compounds that selectively nourish beneficial gut bacteria. They serve as the fuel that allows probiotics to thrive, multiply, and produce their health-promoting metabolites. A probiotic strategy without prebiotic support is like planting seeds in barren soil.
Key Prebiotic Compounds:
- Inulin: Found in chicory root, Jerusalem artichoke, garlic, onions, and leeks; preferentially feeds Bifidobacterium species
- Fructooligosaccharides (FOS): Found in bananas, asparagus, and wheat; promotes growth of Lactobacillus and Bifidobacterium
- Galactooligosaccharides (GOS): Found in legumes and human breast milk; strongly bifidogenic
- Resistant Starch: Found in cooked and cooled potatoes, green bananas, and legumes; fermented to produce butyrate, a critical fuel for colonocytes
- Beta-glucan: Found in oats, mushrooms, and barley; supports both microbial and immune health
- Polyphenols: Found in berries, dark chocolate, green tea, and red wine; serve as prebiotic substrates for diverse microbial species
The combination of a probiotic and a prebiotic is called a synbiotic, and this combination has been shown in multiple studies to produce superior results compared to either component alone. In naturopathic practice, dietary counseling to increase prebiotic-rich whole foods forms the foundation, with supplemental prebiotics added as needed. A target intake of 5 to 15 grams of prebiotic fiber daily is generally recommended, introduced gradually to minimize gas and bloating as the microbiome adapts.
Spore-Based vs Traditional Probiotics
Spore-based probiotics, primarily from the Bacillus genus, represent a distinct category with unique advantages and considerations compared to traditional Lactobacillus and Bifidobacterium formulations.
Spore-Based Probiotics: Organisms such as Bacillus coagulans, Bacillus subtilis, and Bacillus clausii form endospores, a dormant, highly resistant structure that protects the organism from heat, acid, bile, and desiccation. These spores pass through the stomach with near-100 percent survival and germinate in the favorable environment of the small intestine. Key advantages include complete shelf stability without refrigeration, guaranteed survival through gastric transit, longer shelf life, and the ability to withstand concurrent antibiotic use.
Traditional Probiotics: Lactobacillus and Bifidobacterium strains are vegetative (non-spore-forming) organisms. They are more fragile and may suffer significant die-off during manufacturing, storage, and gastric transit. However, they have a much longer history of research, a larger body of clinical evidence for specific conditions, and have been consumed in fermented foods for millennia. Advanced encapsulation technologies such as delayed-release capsules and microencapsulation have significantly improved their survival rates.
In naturopathic practice, the choice between spore-based and traditional probiotics is guided by clinical context. Spore-based formulations are often preferred for patients with compromised digestive function, those taking antibiotics, or those who travel frequently and cannot maintain cold storage. Traditional multi-strain formulations may be preferred when targeting specific conditions with strain-specific evidence. Many practitioners combine both approaches for comprehensive microbial support.
Recommended Dosage
Probiotic dosing is not one-size-fits-all. The optimal dose depends on the specific strain, the health condition being addressed, the individual's current microbiome status, and concurrent medications. The following guidelines represent general naturopathic recommendations.
General Wellness and Prevention:
- 5 to 15 billion CFUs daily of a multi-strain formula
- Include at least 4 to 6 different strains spanning Lactobacillus and Bifidobacterium
- Take with or just before a meal to improve survival through stomach acid
- Complement with daily fermented foods and prebiotic-rich vegetables
Therapeutic Applications:
- 25 to 100 billion CFUs daily, depending on condition severity
- Select strains with specific clinical evidence for the target condition
- Consider divided dosing (morning and evening) for higher therapeutic doses
- Duration typically ranges from 8 to 12 weeks for measurable clinical outcomes
Timing Considerations: Most research suggests taking probiotics with food or within 30 minutes of a meal. The fat and protein in food buffer stomach acid and improve organism survival. However, spore-based probiotics can be taken at any time regardless of meals. Saccharomyces boulardii is also acid-resistant and can be taken without regard to food timing.
It is important to note that probiotics may take 2 to 4 weeks of consistent use before benefits become noticeable. Patience and consistency are essential. If no improvement is observed after 8 weeks, consider rotating to a different strain combination or investigating underlying conditions such as SIBO, parasitic infection, or food sensitivities that may be impeding progress.
Cautions and Contraindications
While probiotics have an excellent overall safety profile and are well tolerated by the vast majority of individuals, certain populations and conditions warrant caution.
Immunocompromised Individuals: Patients with severely suppressed immune systems, including those receiving chemotherapy, post-organ-transplant immunosuppressive therapy, advanced HIV/AIDS, or those with central venous catheters, should exercise caution with probiotic supplementation. In rare cases, live organisms can translocate from the gut into the bloodstream, causing bacteremia or fungemia. Saccharomyces boulardii has been associated with rare cases of fungemia in critically ill patients with central lines. Always consult with all members of the healthcare team before initiating probiotics in immunocompromised individuals.
Small Intestinal Bacterial Overgrowth (SIBO): In patients with diagnosed or suspected SIBO, probiotic supplementation requires careful consideration. Some patients with SIBO experience worsening of symptoms such as bloating, gas, and abdominal distension when taking probiotics, particularly Lactobacillus-dominant formulations. The small intestine, normally relatively low in bacterial population, becomes overwhelmed by organisms that typically reside in the colon. In SIBO cases, it is often advisable to address the overgrowth first with antimicrobial herbs or antibiotics before introducing probiotics. Spore-based probiotics and Saccharomyces boulardii are generally better tolerated in SIBO patients than traditional Lactobacillus formulations.
Additional Cautions:
- Histamine sensitivity: Certain probiotic strains, particularly Lactobacillus casei and Lactobacillus bulgaricus, produce histamine and may exacerbate symptoms in histamine-intolerant individuals; choose low-histamine strains such as Bifidobacterium infantis and Lactobacillus rhamnosus
- D-lactic acidosis: In rare cases involving short bowel syndrome, excessive Lactobacillus supplementation can contribute to D-lactic acid accumulation and neurological symptoms
- Initial die-off reactions: Some individuals experience transient bloating, gas, or altered bowel habits during the first week of probiotic therapy as the microbial ecosystem shifts; start with a lower dose and increase gradually
- Dairy and allergen concerns: Some probiotic supplements are cultured on dairy, soy, or other allergenic media; verify the product is free from relevant allergens if sensitivities exist
- Medication interactions: Immunosuppressant medications may interact with the immune-stimulating effects of probiotics; antifungal medications will inactivate Saccharomyces boulardii
Despite these cautions, probiotics remain one of the safest and most broadly beneficial interventions in naturopathic medicine. The overwhelming majority of people tolerate them well and experience meaningful improvements in digestive function, immune resilience, and overall vitality.
Research Papers
Selected peer-reviewed literature. Links resolve to PubMed or DOI.
- Hill C, Guarner F, Reid G, et al. The ISAPP consensus statement on the scope and appropriate use of the term probiotic. Nat Rev Gastroenterol Hepatol. 2014;11(8):506-514.
- McFarland LV. Meta-analysis of probiotics for the prevention of antibiotic associated diarrhea and the treatment of Clostridium difficile disease. Am J Gastroenterol. 2006;101(4):812-822.
- Goldenberg JZ, Yap C, Lytvyn L, et al. Probiotics for the prevention of Clostridium difficile-associated diarrhea in adults and children. Cochrane Database Syst Rev. 2017;12(12):CD006095.
- Moayyedi P, Ford AC, Talley NJ, et al. The efficacy of probiotics in the treatment of irritable bowel syndrome: a systematic review. Gut. 2010;59(3):325-332.
- Ford AC, Quigley EMM, Lacy BE, et al. Efficacy of prebiotics, probiotics, and synbiotics in irritable bowel syndrome and chronic idiopathic constipation. Am J Gastroenterol. 2014;109(10):1547-1561.
- Hempel S, Newberry SJ, Maher AR, et al. Probiotics for the prevention and treatment of antibiotic-associated diarrhea: a systematic review and meta-analysis. JAMA. 2012;307(18):1959-1969.
- Tillisch K, Labus J, Kilpatrick L, et al. Consumption of fermented milk product with probiotic modulates brain activity. Gastroenterology. 2013;144(7):1394-1401.
- Suez J, Zmora N, Segal E, Elinav E. The pros, cons, and many unknowns of probiotics. Nat Med. 2019;25(5):716-729.
- Zmora N, Zilberman-Schapira G, Suez J, et al. Personalized gut mucosal colonization resistance to empiric probiotics. Cell. 2018;174(6):1388-1405.
- PubMed — probiotics RCT meta-analysis search.
- PubMed — Lactobacillus / Bifidobacterium human trial search.
Connections
- SIBO
- Fermented Foods
- Irritable Bowel Syndrome
- Yogurt
- Gut Microbiome
- Bone Broth
- Gut Healing
- Resistant Starches
- Gut-Brain Axis
- Anxiety
- Bloating
- Eczema
- Acne
- Oral Microbiome
- Kefir
- Kimchi
- Clostridium Difficile
- Leaky Gut
Featured Videos

BRAINY DOSE — 9 Signs You Need To Take Probiotics

Gabay sa Kalusugan - Dr. Gary Sy — Prebiotics & Probiotics for a Healthy Gut - Dr. Gary Sy

HEALTH MANTRA — Probiotics for Gut Health | Immune System | Friendly Bacteria | Curd | Manthena Satyanarayana Raju

Dr. Michael Ruscio, DC, DNM — Probiotics Are One of the Most Effective Treatments for Depression, New Study

Joe Leech (MSc) - Gut Health & FODMAP Dietitian — If You Take Probiotics For IBS, Watch This First Before You Spend More $$

Go See Christy — DO THIS FIRST IF Probiotics Gives U Gas & Bloating

Thomas DeLauer — Neuroscientist Reveals How to Repair Gut Health without Probiotics - Dr. Sherr

Curtis Alexander, Pharm.D. — Probiotic Side Effects [And Why I Don't Recommend Them]

Dr. DiNezza - Gut Microbiome Queen 👑 — Probiotic Side Effects
Healthnews — What's the PROBIOTICS Secret to IBS Relief?

Dr Chaithanya R — Gut Health | Gut Inflammation | Probiotics | Dr Chaithanya Explains!

Oswald Digestive Clinic — Probiotics Side Effects - Be Aware Of This!

Psychopharmacology Institute — Efficacy of Probiotics in Treating ADHD Symptoms

The Primal Podcast and Dr Sarah Myhill — Fix The Microbiome: FASTEST Way To Repair Gut Health (Without Probiotics)

Jill Therese — Acne and Probiotics-YOUR SECRET ACNE CLEARING WEAPON

Dr. Chanu Dasari, MD — Best Probiotic Supplements for [Psoriasis]- Gut Surgeon Explains