Lead Poisoning: Sources, Health Effects, and Prevention
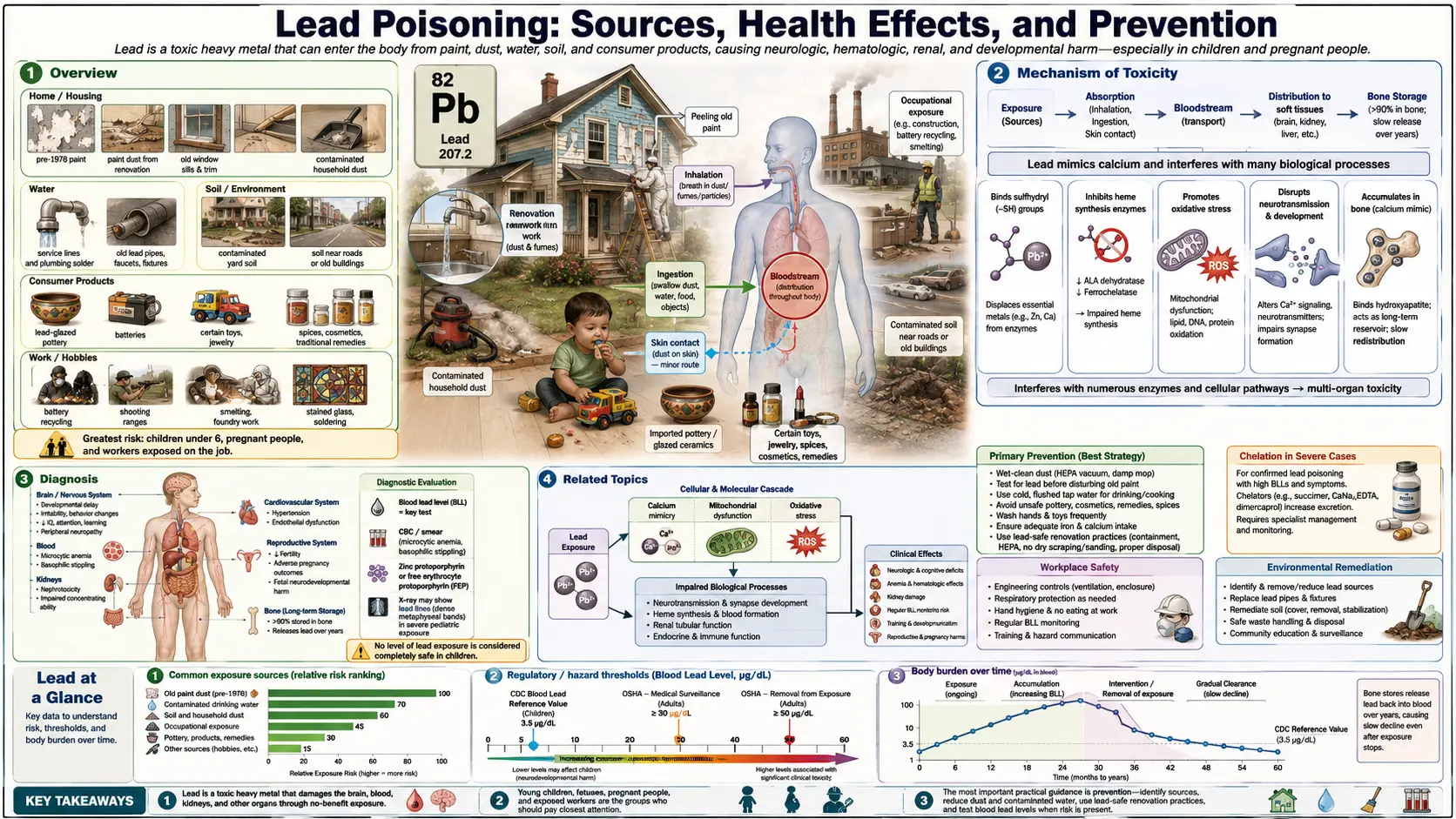

Table of Contents
- Overview
- Sources of Exposure
- Toxicokinetics
- Mechanism of Toxicity
- Health Effects
- Diagnosis
- Treatment
- Prevention
- Related Topics
- References
- Connections
- Featured Videos
1. Overview
Lead (Pb) is a naturally occurring heavy metal and one of the most extensively studied environmental toxicants. Unlike many hazardous substances, there is no identified safe blood lead level (BLL). Even very low concentrations — below 5 µg/dL — are associated with measurable neurocognitive deficits in children, cardiovascular disease in adults, and reproductive harm. The World Health Organization (WHO) lists lead among the ten chemicals of major public health concern.
Widespread human exposure to lead accelerated dramatically during the 20th century. Leaded gasoline, introduced in the 1920s, deposited lead particulates into air, soil, and dust on a global scale. In the United States alone, over 30 million tons of lead were combusted in vehicle fuel before the phaseout was completed in 1996. Lead-based paint was used in homes and buildings until banned for residential use in the U.S. in 1978; hundreds of millions of housing units worldwide still contain lead paint. In other nations, leaded gasoline remained in use into the 2000s, and legacy contamination persists in soil near roadways and urban centers.
The global burden of lead toxicity is substantial. A 2019 analysis published in The Lancet Planetary Health estimated that lead exposure was responsible for approximately 900,000 deaths annually and accounted for 21.7 million years of healthy life lost (DALYs), predominantly from cardiovascular disease. Low- and middle-income countries bear a disproportionate share of this burden due to ongoing industrial exposure, informal battery recycling, and limited regulatory infrastructure.
2. Sources of Exposure
Lead exposure occurs through multiple environmental, dietary, occupational, and consumer product pathways.
Lead-Based Paint
Pre-1978 residential paint is the primary source of lead exposure for children in the United States. As paint ages and deteriorates, it generates lead-containing dust and chips. Renovation and remodeling activities in older homes are a particularly high-risk activity. The EPA's Renovation, Repair, and Painting (RRP) Rule requires certified contractors and specific containment protocols when working in homes built before 1978.
Contaminated Drinking Water
Lead enters drinking water primarily through corrosion of lead service lines and lead-containing solder in plumbing. The Flint, Michigan water crisis (2014–2019) became a widely studied example of systemic failure: a change in water source without adequate corrosion control leached lead from aging pipes, resulting in BLLs above 5 µg/dL in nearly 5% of children tested. An estimated 6–10 million lead service lines remain in use across the U.S., and the EPA Lead and Copper Rule Revisions mandate their replacement.
Lead Pipes and Solder
Beyond service lines, lead solder used in household plumbing prior to 1986 and brass fixtures continue to contribute lead to tap water, particularly when water is allowed to sit in pipes overnight or water chemistry promotes corrosion.
Imported Spices and Turmeric Adulteration
A significant and underrecognized source is adulterated spices. Lead chromate (a yellow pigment) has been found in imported turmeric from Bangladesh, India, and other countries, added to enhance the color. Investigations by the FDA and independent researchers have documented BLLs above 5 µg/dL in families with high turmeric consumption. Chili powder, coriander, and other spices have also been implicated.
Baby Food and Infant Formula
Investigations by the U.S. House Subcommittee on Economic and Consumer Policy (2021) found measurable lead in commercially prepared baby foods, including sweet potatoes, carrots, and fruit juices. Fruit juices, particularly apple and grape juice, have been identified as a dietary lead source for toddlers due to accumulation in root crops and orchard soils.
Chocolate and Cocoa Products
Dark chocolate and cocoa powder can contain significant lead. A 2022 Consumer Reports analysis found that many dark chocolate products contained lead above California's daily maximum allowable dose. Lead accumulates in cocoa beans from contaminated soil in West African growing regions and from post-harvest drying on roadsides.
Soil and Dust Near Roads and Old Buildings
Legacy lead from decades of leaded gasoline combustion persists in urban soils, particularly in areas with high historical traffic volume. Children who play in bare soil near busy roads or in yards of pre-1978 homes are at elevated risk through hand-to-mouth ingestion. Dust from deteriorating lead paint similarly contaminates interior surfaces.
Occupational Exposure
Workers in battery manufacturing and recycling, smelting, radiator repair, painting and sandblasting, shooting ranges (lead bullet residue), and plumbing are at elevated risk. Informal and artisanal battery recycling — common in South and Southeast Asia, Latin America, and Sub-Saharan Africa — is a major contributor to community-level lead contamination in low-income countries.
Cosmetics: Kohl and Surma
Traditional eye cosmetics including kohl (kajal) and surma, used in South Asia, the Middle East, and parts of Africa, frequently contain high concentrations of lead sulfide (galena). Application around the eyes of infants and children is practiced in some communities for perceived protective or cosmetic purposes, but has been documented to cause elevated BLLs.
Folk Remedies
Certain traditional medicines contain lead compounds. Examples include azarcon and greta (Mexican folk remedies used for digestive complaints), litargirio (used as a deodorant and antifungal in some Caribbean communities), and various Ayurvedic and Chinese herbal preparations containing lead minerals. These can cause severe acute lead poisoning.
3. Toxicokinetics
Absorption
Lead is absorbed primarily through the gastrointestinal tract and lungs, with minimal dermal absorption. Children absorb approximately 40–50% of ingested lead, compared with only 5–10% in adults. This difference is driven by higher intestinal permeability, faster gastric emptying, and upregulation of divalent metal transporter 1 (DMT-1) — the same transporter used for calcium and iron uptake. Nutritional deficiencies in calcium, iron, and zinc significantly increase GI lead absorption, making malnourished children particularly vulnerable. Fasting also increases absorption.
Inhaled lead particles are absorbed at rates of 30–50% depending on particle size; finer particles reach the alveoli and are absorbed more completely.
Distribution and Bone Storage
Once absorbed, lead distributes to blood, soft tissue, and bone. Approximately 95% of the adult body burden of lead is stored in bone, where it substitutes for calcium in hydroxyapatite crystals. Blood lead reflects recent exposure and is the primary clinical measurement tool. The half-life of lead in blood is approximately 30 days, in soft tissue approximately 40 days, and in cortical bone 20–30 years.
Mobilization During Physiological States
Bone lead is not inert. During periods of increased bone resorption — pregnancy, lactation, menopause, and osteoporosis — stored lead is released back into circulation, causing endogenous re-exposure. Pregnant women with high lifetime lead burdens can transfer lead to the fetus even without current external exposure. Studies have documented measurable fetal blood lead from maternal bone mobilization alone.
Excretion
Lead is excreted primarily in urine (via glomerular filtration) and to a lesser degree in bile and feces. Sweat and hair contribute minor amounts. Because of its long bone half-life, total body elimination is extremely slow without chelation therapy, and lifelong accumulation occurs with chronic low-level exposure.
4. Mechanism of Toxicity
Calcium Channel Mimicry
Lead's primary mechanism at the molecular level is its ability to mimic calcium ions. Lead(II) has a similar ionic radius to calcium and substitutes for it in numerous biological processes, including neuronal signaling, muscle contraction, and second-messenger cascades. Lead passes through voltage-gated calcium channels and inhibits calcium-dependent processes at concentrations far below those required to saturate normal calcium pools.
Inhibition of Delta-Aminolevulinic Acid Dehydratase (ALAD)
Lead potently inhibits delta-aminolevulinic acid dehydratase (ALAD), a zinc-dependent enzyme critical to heme biosynthesis. Inhibition of ALAD results in accumulation of delta-aminolevulinic acid (ALA), which is itself neurotoxic and structurally similar to the inhibitory neurotransmitter GABA. This mechanism underlies the anemia of lead poisoning (microcytic, hypochromic) and contributes to neurological effects. Lead also inhibits ferrochelatase, the enzyme that inserts iron into protoporphyrin IX to form heme, causing elevated zinc protoporphyrin (ZPP) — a clinically useful marker.
Oxidative Stress
Lead generates reactive oxygen species (ROS) and depletes antioxidant defenses. It depletes glutathione, inhibits superoxide dismutase and catalase, and promotes lipid peroxidation in neuronal membranes. Oxidative damage to the hippocampus and prefrontal cortex contributes to cognitive impairment.
NMDA Receptor Effects
Lead inhibits N-methyl-D-aspartate (NMDA) receptors, which are essential for synaptic plasticity and long-term potentiation — the cellular basis of learning and memory. Even at very low concentrations, lead blocks NMDA receptor function in the developing brain, impairing the formation of new synaptic connections during critical developmental windows. This is a major mechanism underlying the IQ deficits and learning disabilities observed in exposed children.
Protein Kinase C (PKC) Disruption
Lead activates protein kinase C (PKC) at picomolar concentrations by substituting for calcium, dysregulating cellular signaling pathways involved in neurotransmitter release, cell proliferation, and differentiation. This mechanism may underlie effects on dopaminergic and serotonergic systems, contributing to behavioral dysregulation and hyperactivity.
5. Health Effects
Effects in Children: Neurodevelopmental Toxicity
The developing brain is exquisitely sensitive to lead. Landmark epidemiological studies — including the work of Herbert Needleman and the longitudinal Bellinger cohort studies — established that there is no threshold below which neurotoxic effects are absent. For every 1 µg/dL increase in blood lead level, studies consistently estimate a loss of 1–5 IQ points, with the greatest slope of effect at the lowest concentrations. Because the dose-response curve is steepest at low BLLs, the population-level IQ loss from lead at currently prevalent levels is enormous.
Beyond IQ, lead exposure is associated with:
- Attention-deficit/hyperactivity disorder (ADHD) and executive function deficits
- Reading and language learning disabilities
- Impaired working memory and processing speed
- Increased antisocial behavior and delinquency (epidemiological associations)
- Hearing loss at higher exposures
Effects in Adults
Adult health effects are primarily cardiovascular, renal, and reproductive:
- Hypertension: Lead increases blood pressure through endothelial dysfunction, renin-angiotensin system activation, and direct vascular effects. The NHANES data demonstrate a relationship between BLL and blood pressure even at levels below 5 µg/dL.
- Chronic kidney disease (CKD): Lead accumulates in the proximal tubule and causes tubular dysfunction and interstitial nephritis. Long-term exposure accelerates CKD progression.
- Gout: Lead inhibits urate excretion in the proximal tubule, causing hyperuricemia. "Saturnine gout" was described historically among lead workers.
- Peripheral neuropathy: Occupational lead exposure causes a predominantly motor neuropathy with wrist drop and foot drop as classic manifestations.
- Reproductive effects: Lead crosses the blood-testis barrier and impairs sperm motility and morphology. In women, lead exposure is associated with spontaneous abortion, preterm birth, and reduced fertility.
- Cognitive effects in adults: High-level occupational exposure causes encephalopathy; long-term lower exposure is associated with accelerated cognitive aging.
Acute Lead Poisoning
Acute high-dose lead poisoning — typically from ingestion of lead-containing folk remedies, paint chips, or occupational accidents — presents with abdominal colic, vomiting, constipation, headache, and encephalopathy (seizures, coma). The classic "lead line" (Burton's line) — a bluish-black gingival discoloration — reflects lead sulfide deposition. Basophilic stippling of red blood cells is seen on peripheral smear. Encephalopathy carries significant mortality without emergency chelation.
6. Diagnosis
Blood Lead Level (BLL)
The venous blood lead level is the standard clinical test and reflects recent exposure (past 1–3 months). Capillary (fingerstick) samples are used for screening but require venous confirmation if elevated due to risk of skin-surface contamination. The CDC established a blood lead reference value of 3.5 µg/dL (updated in 2021, down from 5 µg/dL), defined as the 97.5th percentile of BLLs in U.S. children — a surveillance threshold rather than a "safe" level. Universal BLL screening is recommended for children at ages 1 and 2 years in high-risk communities.
Zinc Protoporphyrin / Free Erythrocyte Protoporphyrin (ZPP/FEP)
ZPP accumulates in red blood cells when lead inhibits ferrochelatase, and the ZPP/heme ratio is measurable by hematofluorometer. ZPP/FEP is less sensitive than BLL at low exposure levels but is useful as a screening tool and reflects the integrated lead exposure over the lifespan of a red blood cell (approximately 120 days). It also rises in iron deficiency, which must be distinguished.
X-Ray Fluorescence (XRF) Bone Lead Measurement
In vivo X-ray fluorescence (XRF) can quantify lead in bone (typically tibia or patella) non-invasively. Bone lead measurement provides an index of cumulative lifetime lead exposure — more directly relevant to long-term health outcomes than blood lead, which fluctuates. XRF is used in research settings and epidemiological studies but is not routinely available clinically.
Urine Lead
24-hour urine lead is used in some protocols, particularly in chelation challenge tests (historically used to estimate body burden, though now less common due to poor correlation with bone lead).
7. Treatment
Chelation Therapy
Chelation mobilizes lead from tissues and promotes urinary excretion. Indications, agents, and routes depend on the severity of poisoning:
- CaNa2EDTA (calcium disodium EDTA): Administered intravenously or intramuscularly. Used for BLL ≥ 45 µg/dL in children and for symptomatic adults. Does not cross the blood-brain barrier, so is typically combined with BAL in encephalopathy.
- DMSA (Succimer, Chemet): An oral chelating agent used for BLL 25–44 µg/dL in children. Better tolerated than parenteral agents; does not deplete essential minerals as severely as EDTA. Does not significantly reduce bone lead stores.
- BAL (British Anti-Lewisite, dimercaprol): Intramuscular oil-based chelator used for acute encephalopathy (BLL ≥ 70 µg/dL) and combined with CaNa2EDTA. BAL crosses the blood-brain barrier. Peanut oil base contraindicates use in peanut allergy; also contraindicated in hepatic insufficiency.
- D-penicillamine: Oral agent used historically; now less preferred due to side effect profile (nephrotoxicity, bone marrow suppression).
Critically, chelation therapy has not been demonstrated to reverse neurodevelopmental damage in children. The CHELATE trial showed no improvement in cognitive outcomes despite lowered BLL with succimer. Prevention of exposure, not post-exposure chelation, is the cornerstone of protecting children's neurodevelopment.
Nutritional Support and Mineral Competition
Adequate nutrition reduces lead absorption and may partially mitigate toxicity:
- Calcium: Competes with lead for intestinal absorption via DMT-1 and calcium channels. Adequate calcium intake (dairy, fortified foods) reduces GI lead uptake.
- Iron: Iron deficiency upregulates DMT-1 and dramatically increases lead absorption. Correcting iron deficiency anemia is an important adjunct measure.
- Vitamin C (ascorbic acid): Antioxidant properties reduce oxidative damage; some evidence for modest reductions in BLL with supplementation.
- Zinc: Competes with lead for binding sites and serves as a cofactor for ALAD (the lead-inhibited enzyme). Zinc supplementation may partially restore ALAD activity.
8. Prevention
Lead Paint Abatement
Professional lead paint abatement — encapsulation or physical removal — in pre-1978 housing is the most impactful intervention for reducing childhood lead exposure. HUD provides grants for lead hazard remediation in low-income housing. The EPA's RRP Rule mandates lead-safe work practices during renovations.
Water Testing and Filtration
Homeowners in older housing should test tap water for lead (test kits available; EPA-certified labs provide accurate results). NSF/ANSI Standard 53-certified water filters (pitcher filters, under-sink reverse osmosis systems, or faucet-mount filters) can reduce lead in drinking water to near zero. Running tap water for 30 seconds to 2 minutes before use (flushing) reduces lead from standing water in pipes.
Dietary Measures
Consuming meals regularly (avoiding fasting, which increases GI lead absorption), ensuring adequate calcium and iron intake, and limiting consumption of high-risk foods (imported spices from unverified sources, dark chocolate in large quantities, fruit juice in toddlers) reduce dietary lead load. Washing hands before eating and after outdoor play reduces dust ingestion.
Occupational and Regulatory Controls
OSHA's Lead Standard (29 CFR 1910.1025 for general industry; 1926.62 for construction) mandates engineering controls, personal protective equipment, biological monitoring, and medical surveillance for workers with occupational lead exposure. Workers should shower and change clothes before leaving the worksite to avoid take-home lead exposure to family members.
Regulatory Standards
The FDA has issued guidance limiting lead in baby foods (10 ppb for most foods, 20 ppb for single-ingredient root vegetables and dry cereals). The EPA's Lead and Copper Rule Revisions require utilities to identify and replace lead service lines within 10 years. International standards vary considerably, and advocacy for global elimination of lead from consumer products and industrial processes remains an ongoing public health priority.
9. Related Topics
- Heavy Metals Overview
- Arsenic Toxicity
- Mercury Toxicity
- Cadmium Toxicity
- Chlorella — Heavy Metal Detoxification
- Vitamin C — Antioxidant and Lead Mitigation
10. References
- Lanphear BP, et al. Low-level environmental lead exposure and children's intellectual function: an international pooled analysis. Environ Health Perspect. 2005;113(7):894–899.
- Lanphear BP, et al. Low-level lead exposure and mortality in US adults: a population-based cohort study. Lancet Public Health. 2018;3(4):e177–e184.
- Ericson B, et al. A systematic analysis of global lead exposure and health outcomes. Lancet Planet Health. 2021;5(3):e145–e153.
- Rogan WJ, Ware JH. Exposure to lead in children — how low is low enough? N Engl J Med. 2003;348(16):1515–1516.
- Centers for Disease Control and Prevention. Blood Lead Reference Value. Updated 2021. https://www.cdc.gov/niosh/topics/lead/
- Bellinger DC. Lead. Pediatrics. 2004;113(4 Suppl):1016–1022.
- Needleman HL, et al. Deficits in psychologic and classroom performance of children with elevated dentine lead levels. N Engl J Med. 1979;300(13):689–695.
- Dignam T, et al. Control of lead sources in the United States, 1970–2017: public health progress and current challenges to eliminating lead exposure. J Public Health Manag Pract. 2019;25(Suppl 1):S13–S22.
- Hanna-Attisha M, et al. Elevated blood lead levels in children associated with the Flint drinking water crisis. Am J Public Health. 2016;106(2):283–290.
- Forsyth JE, et al. Turmeric means "yellow" in Sanskrit: lead chromate and lead sulfate content of turmeric samples from Bangladesh. Environ Sci Technol Lett. 2019;6(4):233–238.
- Rogan WJ, et al. The effect of chelation therapy with succimer on neuropsychological development in children exposed to lead. N Engl J Med. 2001;344(19):1421–1426.
- Schwartz BS, et al. Occupational lead exposure and longitudinal decline in neurobehavioral test scores. Epidemiology. 2000;11(5):523–529.
- Kosnett MJ. The role of chelation in the treatment of arsenic and mercury poisoning. J Med Toxicol. 2013;9(4):347–354.
- Kim R, et al. A longitudinal study of low-level lead exposure and impairment of renal function: the Normative Aging Study. JAMA. 1996;275(15):1177–1181.
- Nash D, et al. Blood lead, blood pressure, and hypertension in perimenopausal and postmenopausal women. JAMA. 2003;289(12):1523–1532.
- Hu H, et al. Fetal lead exposure at each stage of pregnancy as a predictor of infant mental development. Environ Health Perspect. 2006;114(11):1730–1735.
- Canfield RL, et al. Intellectual impairment in children with blood lead concentrations below 10 µg per deciliter. N Engl J Med. 2003;348(16):1517–1526.
- World Health Organization. Lead poisoning. WHO fact sheet. Updated 2023. https://www.who.int/news-room/fact-sheets/detail/lead-poisoning-and-health
Connections
- Mercury
- Arsenic
- Cadmium
- Heavy Metals
- Vitamin C
- Chlorella
- Zinc
- Calcium
- Iron
- Turmeric
- Hypertension
- ADHD
- Kidney Disease
- Detoxification
- Glutathione
- Pesticides
- Oxidative Stress
- Selenium