Tick-Origin Science of Alpha-Gal Syndrome
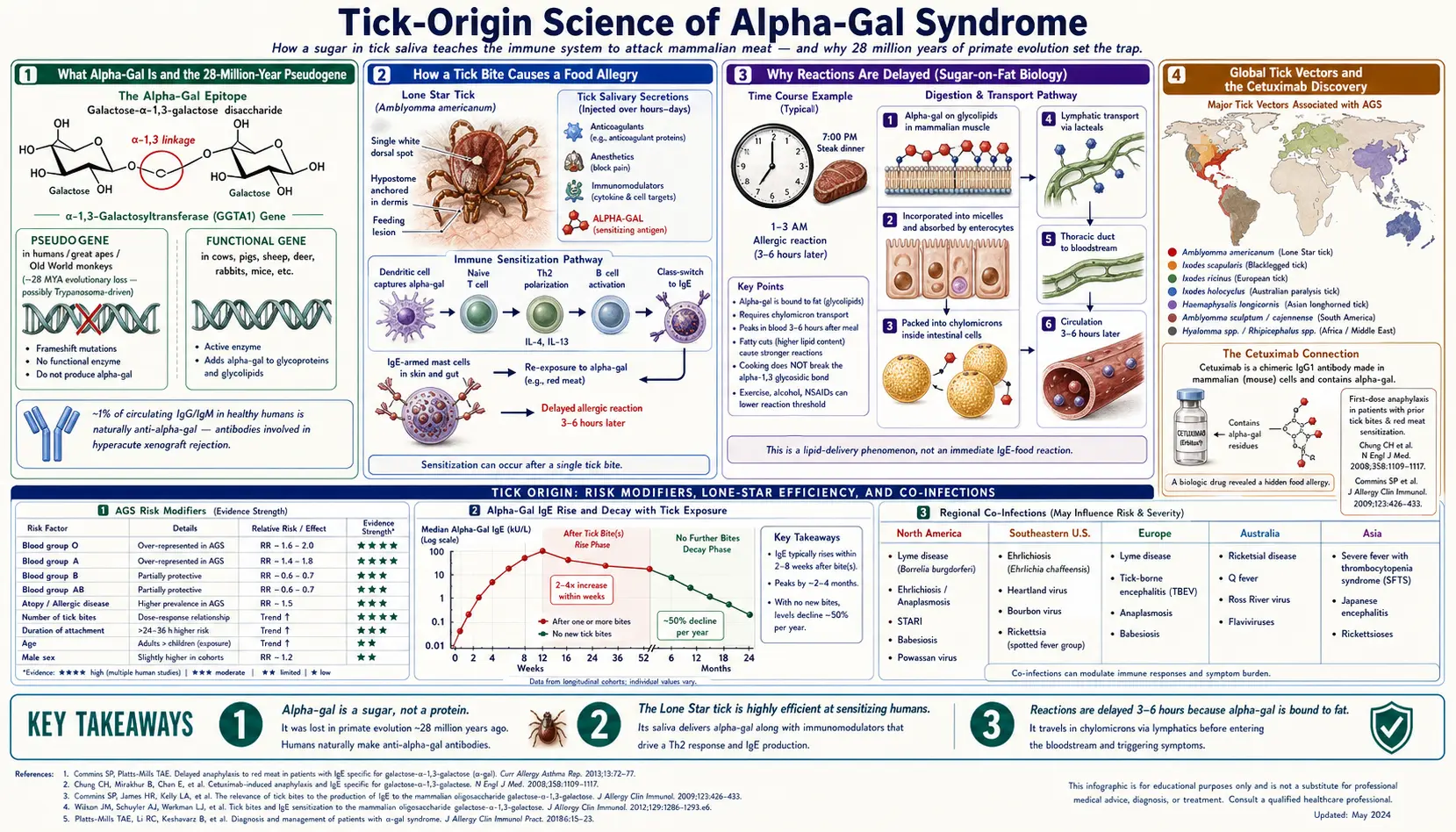
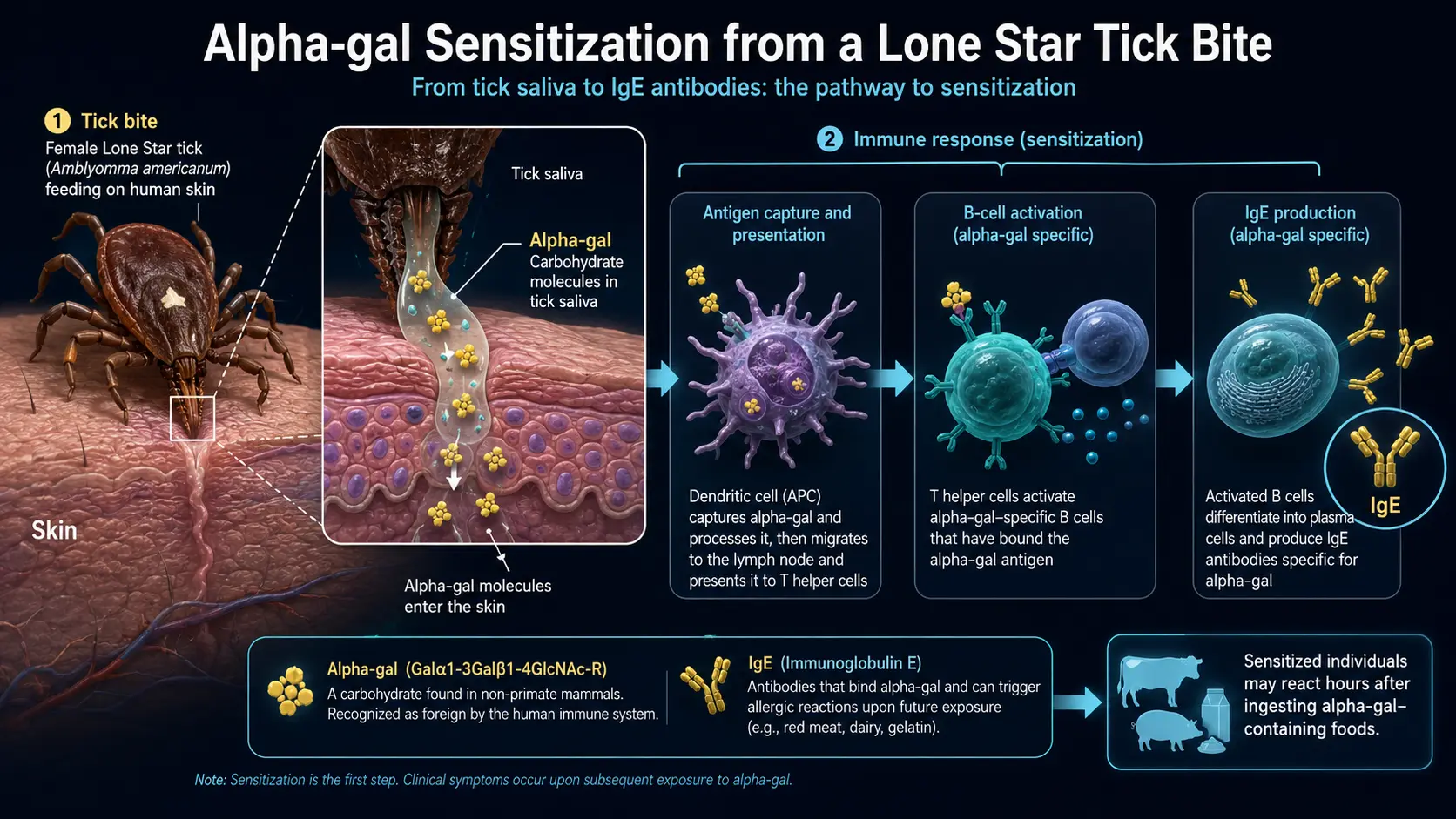
Table of Contents
- What Alpha-Gal Actually Is
- How a Tick Bite Causes a Food Allergy
- Why Reactions Are Delayed
- The Tick Species That Cause AGS
- Why the Lone Star Tick Is Especially Efficient
- Why Second Tick Bites Matter
- The Cetuximab Discovery
- Why Not Everyone Bitten Gets AGS
- Co-Infections to Watch For
- Prevention: The Only Real Treatment
- Key Research Papers
- Connections
- Featured Videos
What Alpha-Gal Actually Is
Alpha-gal — full name galactose-α-1,3-galactose — is a simple carbohydrate. Not a protein. That one fact explains most of what makes Alpha-Gal Syndrome (AGS) strange: virtually every other food allergy in medicine is triggered by a protein (peanut, shellfish, milk casein, egg albumin). AGS is one of the few well-documented IgE allergies to a sugar.
Alpha-gal is manufactured by the enzyme α-1,3-galactosyltransferase, which decorates cell-surface glycolipids and glycoproteins with this two-sugar tag. Almost every non-primate mammal on Earth — cows, pigs, sheep, goats, deer, rabbits, bison, whales, mice, cats, dogs — produces alpha-gal in enormous quantities. Their red blood cells, muscle tissue, organs, and milk fat globules are all coated with it.
Humans, great apes, and Old World monkeys are the exceptions. Around 28 million years ago, a catastrophic mutation knocked out the α-1,3-galactosyltransferase gene in our shared ancestor. The gene is still in our DNA, but it's a pseudogene — a broken copy. We don't make the sugar. The leading evolutionary hypothesis is that the loss was driven by a pathogen (possibly a pandemic Trypanosoma-like parasite) that used alpha-gal as a cell-entry ligand.
Because we don't make alpha-gal, our immune systems treat it as foreign. Nearly 1% of all circulating antibodies in a healthy human are naturally occurring anti-alpha-gal IgG and IgM, produced in response to gut bacteria that bear alpha-gal-like residues. These are the same antibodies that cause hyperacute xenograft rejection when pig organs are transplanted into humans — your body sees pig tissue as covered in a flag that reads "not self," and attacks within minutes.
In AGS, something different happens: the immune system additionally produces IgE-class antibodies against alpha-gal. IgE is the allergy antibody, the one that arms mast cells for explosive histamine release. And the trigger for that class switch is almost always a tick bite.
How a Tick Bite Causes a Food Allergy
A tick doesn't eat and leave. It cements its mouthparts into your skin and feeds for hours to days, cycling saliva in and blood out. That saliva is a pharmacological cocktail — anesthetics so you don't feel the bite, anticoagulants to keep blood flowing, immunomodulators to suppress local defenses. And, critically for AGS, it contains alpha-gal.
Where does the tick's alpha-gal come from? Two sources, possibly overlapping. First, the tick picks it up from earlier blood meals on mammals (a nymph that fed on a white-tailed deer carries deer alpha-gal into its next host). Second, and more provocatively, recent work suggests ticks can synthesize alpha-gal themselves in their salivary glands — detecting the sugar even in larval ticks that have never fed on a mammal.
Either way, the result is that tick saliva delivers alpha-gal directly into the dermis, alongside powerful immune adjuvants, over many hours. From the immune system's perspective, this looks like a persistent parasitic invasion. The textbook response to a long-running parasitic challenge is an IgE and Th2 response — the same arm of immunity that evolved to expel worms. Mast cells and basophils get armed with anti-alpha-gal IgE.
Now the person has a silent trap. They feel fine. But every cell of mammalian meat they eat — every bite of beef, pork, lamb, venison, bison, goat, rabbit — is studded with the exact sugar their mast cells are primed to attack.
Why Reactions Are Delayed
A peanut-allergic child reacts within minutes. An AGS patient reacts 3 to 6 hours after eating red meat — often in the middle of the night after a dinner steak. This delay is not psychological and it is not "mild." It's a direct consequence of sugar-on-fat biology.
In mammalian meat, alpha-gal is bound predominantly to glycolipids — sugars attached to fat molecules, especially in membrane cerebrosides and in neutral lipid droplets. Fat digestion is slow. Dietary fat doesn't enter the bloodstream directly; it's packaged into chylomicrons inside intestinal cells, released into the lymphatic system, and only reaches the general circulation through the thoracic duct hours later.
This is why lipid-heavy meals are worse. A fatty ribeye, pork belly, lamb shank, or cream-heavy dish often produces far worse reactions than a lean cut of beef. Dairy fat (butter, cheese, whole milk) carries alpha-gal for the same reason. Cooked or rendered fat does not destroy the sugar — heat doesn't break the glycosidic bond.
The delayed onset also explains why AGS went unrecognized for decades. Patients and doctors rarely connect a 2 a.m. hives attack or anaphylaxis to a steak eaten at 7 p.m. the night before.
The Tick Species That Cause AGS
AGS has now been reported on every inhabited continent. Different tick species drive it in different regions.
Lone Star Tick (Amblyomma americanum)
The dominant cause in the United States and by far the best-characterized. Historically a southeastern and south-central species, it has expanded aggressively north into the Ohio Valley, Mid-Atlantic, and New England, and west into the eastern Great Plains. The adult female has an unmistakable single white dot on her back — the "lone star."
Blacklegged / Deer Tick (Ixodes scapularis)
The same species that transmits Lyme disease. Evidence of alpha-gal transmission exists but appears minor compared to A. americanum. Some European and northern US AGS cases where lone star ticks are uncommon may be driven by Ixodes.
Castor Bean Tick (Ixodes ricinus)
The primary European AGS vector. Endemic across the United Kingdom, France, Germany, the Benelux countries, Scandinavia, and much of central Europe. Also the main Lyme vector in Europe.
Paralysis Tick (Ixodes holocyclus)
Drives Australian AGS, concentrated along the eastern coast from Queensland through New South Wales. Australia had some of the earliest anecdotal reports of tick-bite-associated meat allergy, predating the US recognition.
Asian Longhorned Tick (Haemaphysalis longicornis)
Native to East Asia (Japan, Korea, China) and linked to AGS there. Established in the United States since 2017 and spreading rapidly; its role in US AGS is still being mapped.
South American Ticks (Amblyomma sculptum, A. cajennense)
Drive AGS across Brazil, Argentina, and neighboring countries. Closely related to the lone star tick and behaviorally similar.
African Ticks (Hyalomma, Rhipicephalus)
Implicated in AGS cases from southern and eastern Africa, though surveillance is thin and prevalence is poorly measured.
Why the Lone Star Tick Is Especially Efficient
If you live in the US and have AGS, odds overwhelmingly favor Amblyomma americanum as the culprit. Several biological features make it unusually good at sensitizing humans:
Aggressive host-seeking. Unlike many ticks that wait passively on grass tips, lone star ticks actively pursue carbon dioxide plumes. They'll run toward you across open ground. They're nicknamed "the seed tick" when larvae cluster in the hundreds and swarm a passing leg.
Multiple blood meals per life cycle. Larva, nymph, and adult stages each require a separate host, and all three stages readily bite humans. Nymphs are the size of a poppy seed and easily missed — many AGS patients cannot recall the bite that caused their disease.
Heavy salivary alpha-gal load. Comparative studies show lone star tick saliva carries notably more alpha-gal reactivity than Ixodes species, consistent with why it produces AGS more reliably per bite.
Ecological amplification. White-tailed deer populations have exploded across the eastern US over the last 60 years, and deer are the reproductive host for adult lone star ticks. Where deer thrive — suburbs, fragmented forest, brushy edges — lone star tick density is now orders of magnitude higher than historical baselines.
Why Second Tick Bites Matter
This is the single most important thing for an AGS patient to understand: additional tick bites are not neutral events — they are re-sensitizing exposures. Every new bite delivers another round of alpha-gal-laden saliva, which boosts anti-alpha-gal IgE titers back up the way a vaccine booster raises antibody levels.
Patients who continue to get bitten tend to have persistent or worsening AGS. Patients who rigorously eliminate new bites often see IgE titers fall by 50% or more per year, and many regain partial or full tolerance to mammalian meat over a 1–5 year window (see Natural History & Tolerance).
In practical terms this reframes AGS treatment. Avoidance isn't only about what you eat — it's equally about where you walk. Tick avoidance is part of the therapy, not merely the diagnosis. Details of permethrin-treated clothing, DEET/picaridin, yard management, and proper tick-check protocols are in Tick-Bite Prevention.
The Cetuximab Discovery
AGS was discovered essentially by accident — through a cancer drug.
Cetuximab (brand name Erbitux) is a monoclonal antibody targeting the EGFR receptor, used to treat metastatic colorectal cancer and head-and-neck cancers. In early post-marketing experience a peculiar signal emerged: patients in Tennessee, North Carolina, Virginia, Arkansas, and Missouri were having severe anaphylactic reactions to their very first infusion at rates approaching 20%, while patients in Boston and the northeast had reaction rates under 3%.
First-dose anaphylaxis to a drug you've never received implies the patient already had antibodies against something on that drug. Thomas Platts-Mills and Scott Commins at the University of Virginia traced the target: cetuximab is produced in a murine (mouse) cell line, and mouse cells glycosylate the antibody's Fab region with alpha-gal. The southeastern patients had pre-existing IgE against alpha-gal. The geographic map of reactions matched the geographic map of the lone star tick almost exactly.
This was reported in Chung et al., NEJM 2008, and the food-allergy counterpart — delayed anaphylaxis to red meat in the same populations — was pinned down in Commins et al., JACI 2009. Those two papers founded the field.
Why Not Everyone Bitten Gets AGS
Plenty of people are bitten by lone star ticks and never develop AGS. Several factors modulate risk:
Blood type. Alpha-gal is structurally similar to the blood group B antigen. Individuals with blood type B or AB already circulate antibodies that engage the B antigen and appear to be relatively protected from developing AGS — the immune system may treat alpha-gal as partly "seen before." Blood type O and A individuals are over-represented among AGS patients. This is a population-level tendency, not an individual guarantee.
Number and duration of bites. AGS follows a dose-response curve. A single brief bite is less likely to sensitize than repeated or prolonged attachment. Outdoor workers, hunters, landscapers, and rural residents carry the heaviest risk.
Individual immune variation. Atopic individuals (history of asthma, eczema, hay fever, other food allergies) may be more prone to the Th2/IgE class switch.
Co-exposure to tick-borne pathogens. Ticks that also transmit Borrelia, Ehrlichia, or Anaplasma may tip the immune response in ways that either amplify or dampen AGS sensitization — the data are still coming in.
Co-Infections to Watch For
A tick bite capable of causing AGS can deliver other pathogens in the same saliva. Any patient with a strong suspected tick bite and atypical symptoms — fever, severe headache, joint pain, neurologic symptoms, a spreading rash — deserves a fuller workup. Common co-infections by region:
- Lyme disease — primarily Ixodes scapularis / I. ricinus; less common in pure lone star range but possible.
- Ehrlichiosis (Ehrlichia chaffeensis, E. ewingii) — lone star tick is the primary vector.
- STARI (southern tick-associated rash illness) — a Lyme-like rash following A. americanum bite; cause still debated.
- Heartland virus — emerging in the central US; lone star tick vector.
- Bourbon virus — rare, sometimes fatal; lone star tick vector.
- Rocky Mountain spotted fever (Rickettsia rickettsii) — American dog tick, brown dog tick.
- Anaplasmosis, Babesiosis, Powassan virus — blacklegged tick range.
Prevention: The Only Real Treatment
There is no approved desensitization protocol for AGS. No injection course, no oral immunotherapy, no pill. The only proven therapeutic strategy is the combination of strict avoidance of mammalian meat and mammalian-derived products plus rigorous prevention of further tick bites. In that combined regimen, many patients recover tolerance on a multi-year timescale. See Tick-Bite Prevention for the practical playbook — permethrin-treated clothing, repellents, landscaping, and tick-removal technique.
Key Research Papers
Foundational and recent peer-reviewed publications on tick biology, salivary glycans, the cetuximab observation that opened the field, and the global epidemiology of AGS-associated tick species. Author names, titles, and journals are plain text; the year/volume/issue/pages link opens the DOI.
- Commins SP, James HR, Kelly LA, Pochan SL, Workman LJ, Perzanowski MS, Kocan KM, Fahy JV, Nganga LW, Ronmark E, Cooper PJ, Platts-Mills TAE. The Relevance of Tick Bites to the Production of IgE Antibodies to the Mammalian Oligosaccharide Galactose-α-1,3-Galactose. Journal of Allergy and Clinical Immunology. 2011;127(5):1286–1293.e6.
- Chung CH, Mirakhur B, Chan E, Le QT, Berlin J, Morse M, Murphy BA, Satinover SM, Hosen J, Mauro D, Slebos RJ, Zhou Q, Gold D, Hatley T, Hicklin DJ, Platts-Mills TAE. Cetuximab-Induced Anaphylaxis and IgE Specific for Galactose-α-1,3-Galactose. New England Journal of Medicine. 2008;358(11):1109–1117.
- Commins SP, Satinover SM, Hosen J, Mozena J, Borish L, Lewis BD, Woodfolk JA, Platts-Mills TAE. Delayed Anaphylaxis, Angioedema, or Urticaria after Consumption of Red Meat in Patients with IgE Antibodies Specific for Galactose-α-1,3-Galactose. Journal of Allergy and Clinical Immunology. 2009;123(2):426–433.
- Steinke JW, Platts-Mills TAE, Commins SP. The Alpha-Gal Story: Lessons Learned from Connecting the Dots. Journal of Allergy and Clinical Immunology. 2015;135(3):589–596.
- Hashizume H, Fujiyama T, Umayahara T, Kageyama R, Walls AF, Satoh T. Repeated Amblyomma testudinarium Tick Bites Are Associated with Increased Galactose-α-1,3-Galactose Carbohydrate IgE Antibody Levels: A Retrospective Cohort Study in a Single Institution. Journal of the American Academy of Dermatology. 2018;78(6):1135–1141.e3.
- Chinuki Y, Ishiwata K, Yamaji K, Takahashi H, Morita E. Haemaphysalis longicornis Tick Bites Are a Possible Cause of Red Meat Allergy in Japan. Allergy. 2016;71(3):421–425.
- Hamsten C, Starkhammar M, Tran TAT, Johansson M, Bengtsson U, Sædén A, Grönlund H, van Hage M. Identification of Galactose-α-1,3-Galactose in the Gastrointestinal Tract of the Tick Ixodes ricinus; Possible Relationship with Red Meat Allergy. Allergy. 2013;68(4):549–552.
- Karim S, Singh P, Ribeiro JMC. A Deep Insight into the Sialotranscriptome of the Gulf Coast Tick, Amblyomma maculatum. PLoS ONE. 2011;6(12):e28525.
- Cabezas-Cruz A, Espinosa PJ, Alberdi P, Simo L, Valdes JJ, Mateos-Hernandez L, Contreras M, Rayo MV, de la Fuente J. Tick Galactosyltransferases Are Involved in α-Gal Synthesis and Play a Role during Anaplasma phagocytophilum Infection and Ixodes scapularis Tick Vector Development. Scientific Reports. 2018;8(1):14224.
- Wilson JM, Schuyler AJ, Workman L, Gupta M, James HR, Posthumus J, McGowan EC, Commins SP, Platts-Mills TAE. Investigation Into the α-Gal Syndrome: Characteristics of 261 Children and Adults Reporting Red Meat Allergy. Journal of Allergy and Clinical Immunology: In Practice. 2019;7(7):2348–2358.e4.
- Hilger C, Fischer J, Wölbing F, Biedermann T. Role and Mechanism of Galactose-Alpha-1,3-Galactose in the Elicitation of Delayed Anaphylactic Reactions to Red Meat. Current Allergy and Asthma Reports. 2019;19(1):3.
- Wilson JM, Erickson L, Levin M, Ailsworth SM, Commins SP, Platts-Mills TAE. Tick Bites, IgE to Galactose-α-1,3-Galactose, and Urticarial or Anaphylactic Reactions to Mammalian Meat: The Alpha-Gal Syndrome. Allergy. 2024;79(6):1440–1454.
- Vaz-Rodrigues R, Mazuecos L, de la Fuente J. Current and Future Strategies for the Diagnosis and Treatment of the Alpha-Gal Syndrome (AGS). Journal of Asthma and Allergy. 2022;15:957–970.
Live PubMed Searches
Live PubMed queries that update as new papers are indexed.
- Galactose-α-1,3-galactose IgE
- Amblyomma americanum and alpha-gal
- Tick saliva and alpha-gal
- Cetuximab anaphylaxis and alpha-gal
- Alpha-gal and blood type
- Ixodes ricinus and red meat allergy
- Alpha-gal global epidemiology
- Alpha-gal syndrome natural history
Connections
- Natural History and Tolerance
- Tick Bite Prevention
- Alpha-Gal Syndrome Overview
- Allergies
- Lyme Disease
- Mammalian Foods List
- Restaurant and Travel Survival
- Cross-Reactive Medications
- Anaphylaxis Emergency Plan
- Testing and Diagnosis
- Mast Cell Activation Syndrome
- POTS
- SIBO
- Asthma
- Alpha-Gal and Cardiovascular Risk
- Lyme Disease Prevention and Tick Removal