Tuberculosis (TB)
What is Tuberculosis?
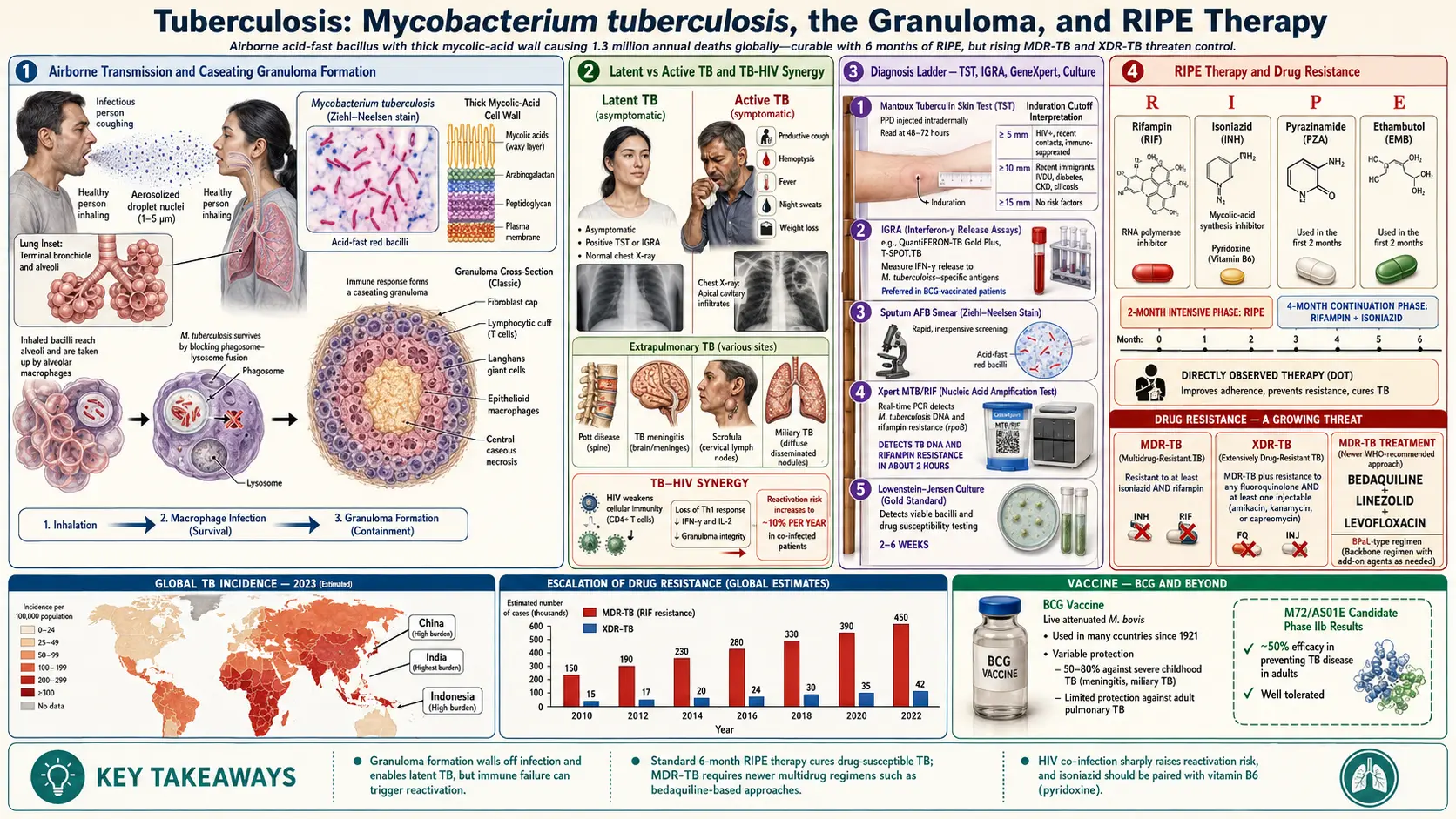
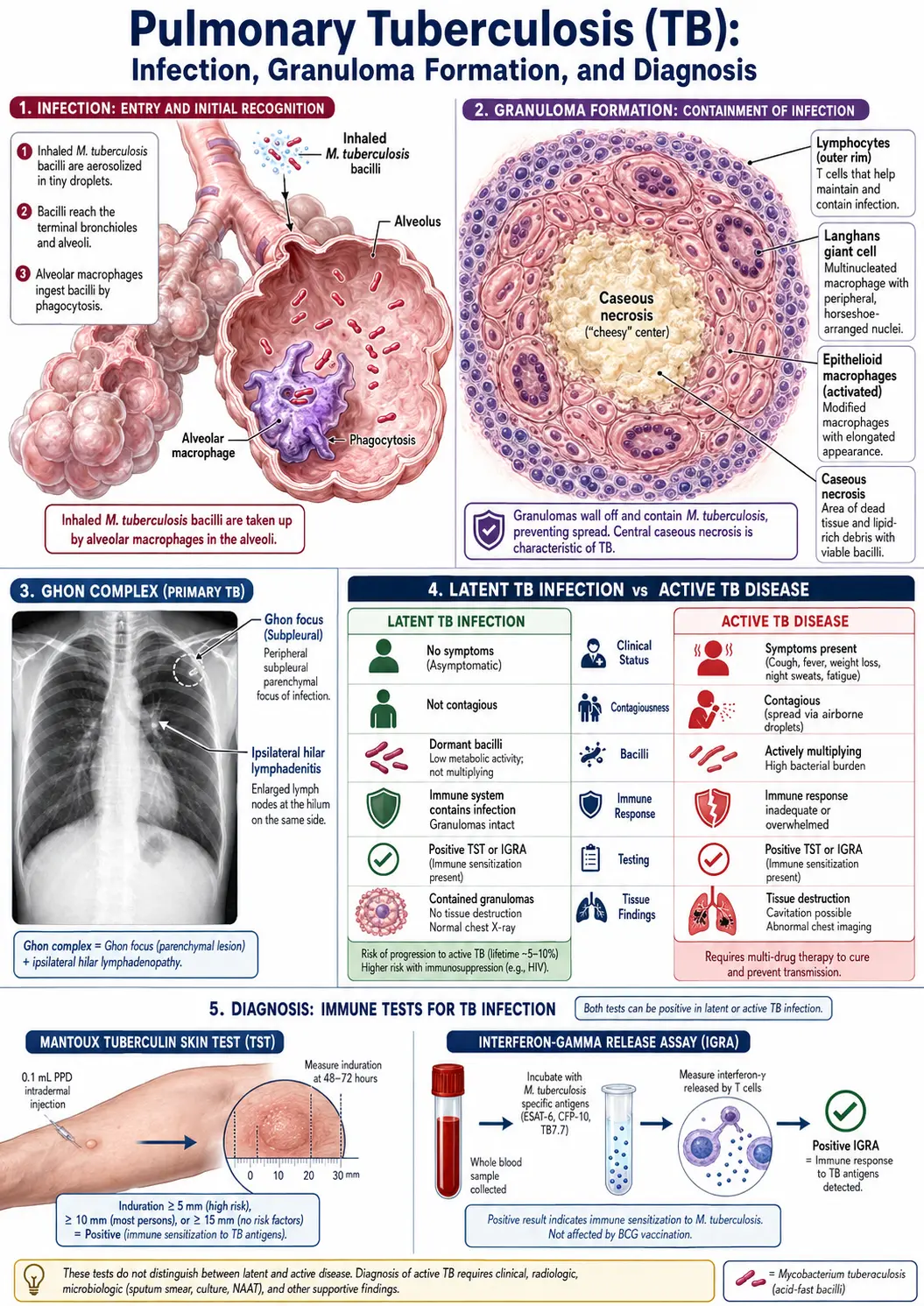
Tuberculosis (TB) is an infectious disease caused by the bacterium Mycobacterium tuberculosis. It primarily affects the lungs but can spread to other parts of the body, such as the kidneys, spine, and brain. TB can be latent or active, with active TB being contagious and requiring treatment.
Types of Tuberculosis
1. Latent TB
- No symptoms: The bacteria remain inactive in the body and do not cause illness.
- Not contagious
- Can become active: Without treatment, latent TB can progress to active TB.
2. Active TB
- Shows symptoms and can spread to others.
- Requires immediate treatment to prevent complications and transmission.
Symptoms of Active TB
Common symptoms include:
- Persistent cough: Lasting three weeks or longer, sometimes with blood-tinged sputum.
- Chest pain
- Unintentional weight loss
- Fatigue
- Fever and chills
- Night sweats
- Loss of appetite
Causes and Transmission
- Caused by Mycobacterium tuberculosis
- Airborne transmission: TB spreads when an infected person coughs, sneezes, or talks, releasing respiratory droplets containing the bacteria.
- Close contact with someone who has active TB increases the risk of infection.
Risk Factors
- Weakened immune system: People with HIV/AIDS, diabetes, or those undergoing immunosuppressive therapy are more susceptible.
- Close contact with someone who has active TB.
- Living or working in high-risk environments: Such as prisons, shelters, or healthcare facilities.
- Substance abuse: Drug and alcohol use can weaken the immune system.
- Poor nutrition
Diagnosis
- TB skin test (Mantoux test): A small amount of tuberculin is injected under the skin to see if a reaction occurs.
- TB blood tests: Such as the interferon-gamma release assays (IGRAs).
- Chest X-ray: Helps detect lung damage associated with active TB.
- Sputum tests: Microscopic examination and culture to identify TB bacteria.
Treatment Options
- Antibiotic regimen:
- First-line drugs: Include isoniazid, rifampin, ethambutol, and pyrazinamide.
- Duration: Treatment typically lasts 6 to 9 months, depending on the type and severity of TB.
- Directly observed therapy (DOT): Healthcare providers supervise patients taking their medication to ensure adherence.
Drug-Resistant TB
Drug-resistant TB occurs when the bacteria do not respond to the standard treatment due to resistance to certain medications.
1. Multidrug-Resistant TB (MDR-TB)
- Resistant to isoniazid and rifampin, the two most potent TB drugs.
- Requires alternative treatment regimens that are longer and may have more side effects.
2. Extensively Drug-Resistant TB (XDR-TB)
- Resistant to first-line drugs and some second-line drugs.
- More challenging to treat and requires specialized medications.
Prevention Strategies
- Avoid close contact with individuals known to have active TB.
- Use protective measures: Such as wearing masks in high-risk settings.
- Good ventilation: Helps reduce the concentration of TB bacteria in enclosed spaces.
- Early detection and treatment: Reduces the risk of spreading the disease.
Complications of Tuberculosis
- Lung damage: Can lead to permanent scarring and reduced lung function.
- Spread to other organs: Known as extrapulmonary TB, which can affect the kidneys, spine, brain, and other parts of the body.
- Spinal pain: TB in the spine (Pott's disease) can cause severe pain and deformities.
- Meningitis: TB affecting the membranes surrounding the brain, leading to life-threatening complications.
- Joint damage: TB arthritis can affect the hips and knees.
References & Research
Historical Background
Robert Koch identified Mycobacterium tuberculosis as the causative agent of tuberculosis on March 24, 1882, a discovery for which he received the 1905 Nobel Prize in Physiology or Medicine. The introduction of streptomycin in 1944 by Albert Schatz, Elizabeth Bugie, and Selman Waksman marked the beginning of effective antibiotic treatment for TB.
Key Research Papers
- Pai M, Behr MA, Dowdy D, et al. Tuberculosis. Nature Reviews Disease Primers. 2016;2:16076.
- Zumla A, Raviglione M, Hafner R, von Reyn CF. Tuberculosis. New England Journal of Medicine. 2013;368(8):745-755.
- Dorman SE, Nahid P, Kurbatova EV, et al. Four-month rifapentine regimens with or without moxifloxacin for tuberculosis. New England Journal of Medicine. 2021;384(18):1705-1718.
- Diacon AH, Pym A, Grobusch MP, et al. Multidrug-resistant tuberculosis and culture conversion with bedaquiline. New England Journal of Medicine. 2014;371(8):723-732.
- Conradie F, Diacon AH, Ngubane N, et al. Treatment of highly drug-resistant pulmonary tuberculosis. New England Journal of Medicine. 2020;382(10):893-902.
- Lawn SD, Zumla AI. Tuberculosis. The Lancet. 2011;378(9785):57-72.
- Sterling TR, Villarino ME, Borisov AS, et al. Three months of rifapentine and isoniazid for latent tuberculosis infection. New England Journal of Medicine. 2011;365(23):2155-2166.
- Boehme CC, Nabeta P, Hillemann D, et al. Rapid molecular detection of tuberculosis and rifampin resistance. New England Journal of Medicine. 2010;363(11):1005-1015.
- WHO consolidated guidelines on tuberculosis. Module 4: treatment -- drug-resistant tuberculosis treatment. The Lancet Infectious Diseases. 2019;19(11):e348-e364.
- Gandhi NR, Moll A, Sturm AW, et al. Extensively drug-resistant tuberculosis as a cause of death in patients co-infected with tuberculosis and HIV in a rural area of South Africa. The Lancet. 2006;368(9547):1575-1580.
- Houben RMGJ, Dodd PJ. The global burden of latent tuberculosis infection: a re-estimation using mathematical modelling. PLoS Medicine. 2016;13(10):e1002152.
Research Papers
The following PubMed topic searches retrieve current peer-reviewed literature on Tuberculosis. Each link opens a live PubMed query so you always see the most recent publications.
- Tuberculosis review
- Mycobacterium tuberculosis pathogenesis
- Multidrug resistant tuberculosis MDR-TB
- Bedaquiline tuberculosis treatment
- Isoniazid rifampin tuberculosis
- Latent tuberculosis infection treatment
- BCG vaccine tuberculosis efficacy
- Tuberculosis HIV coinfection
- GeneXpert tuberculosis diagnosis
- WHO tuberculosis global report
- Extrapulmonary tuberculosis
- Vitamin D tuberculosis
Connections
- HIV/AIDS
- Immune Boosting
- Vitamin D3
- Zinc
- Garlic
- Andrographis
- Meningitis
- Hepatitis B
- Hepatitis C
- Hepatitis
- Diabetes
- Fatigue
- Chest Pain
- Loss of Appetite
- Cellulitis
- Clostridium Difficile
- Eucalyptus
- Biologics TNF IL23 Integrin Inhibitors