Sickle Cell Disease
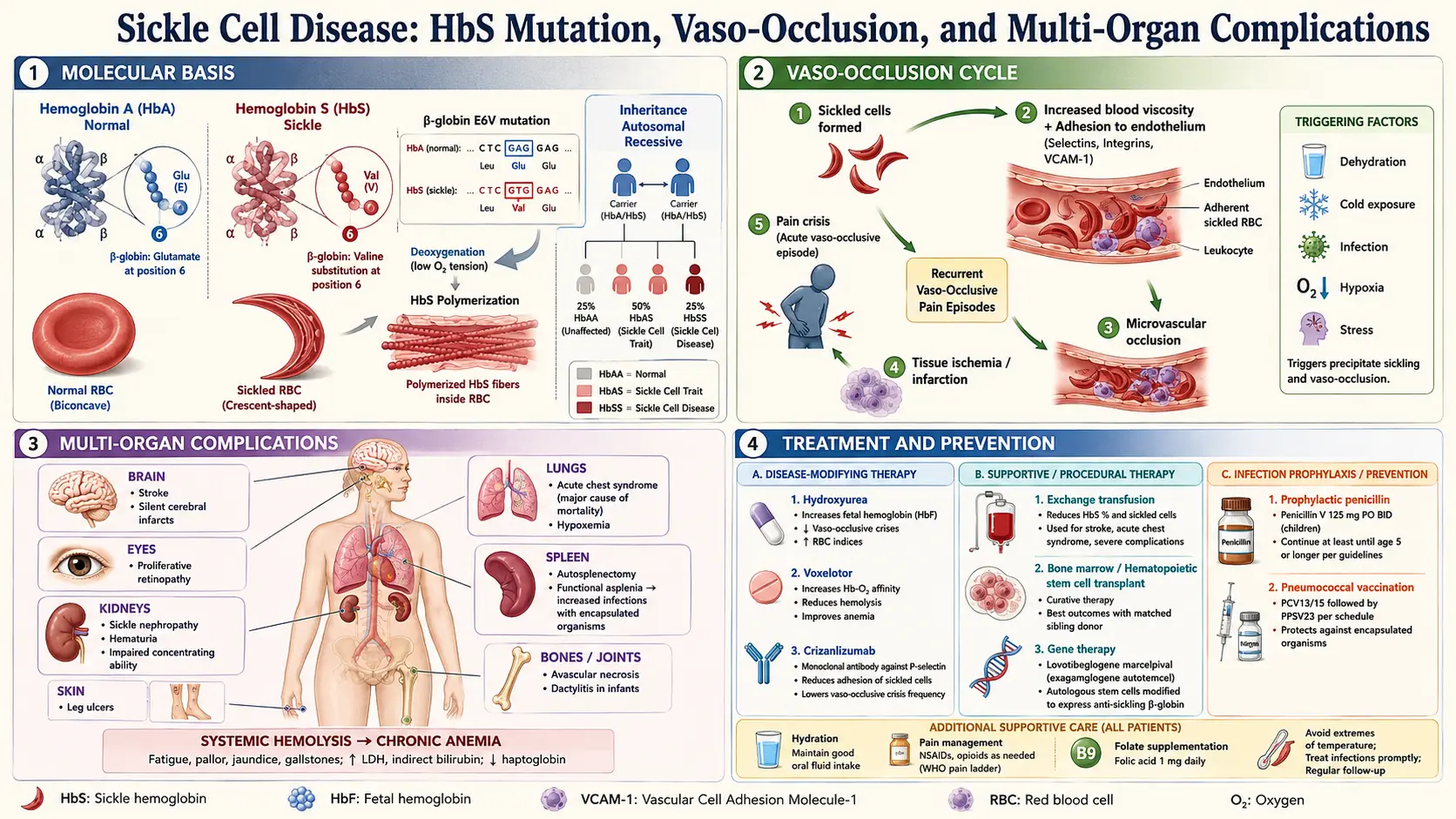
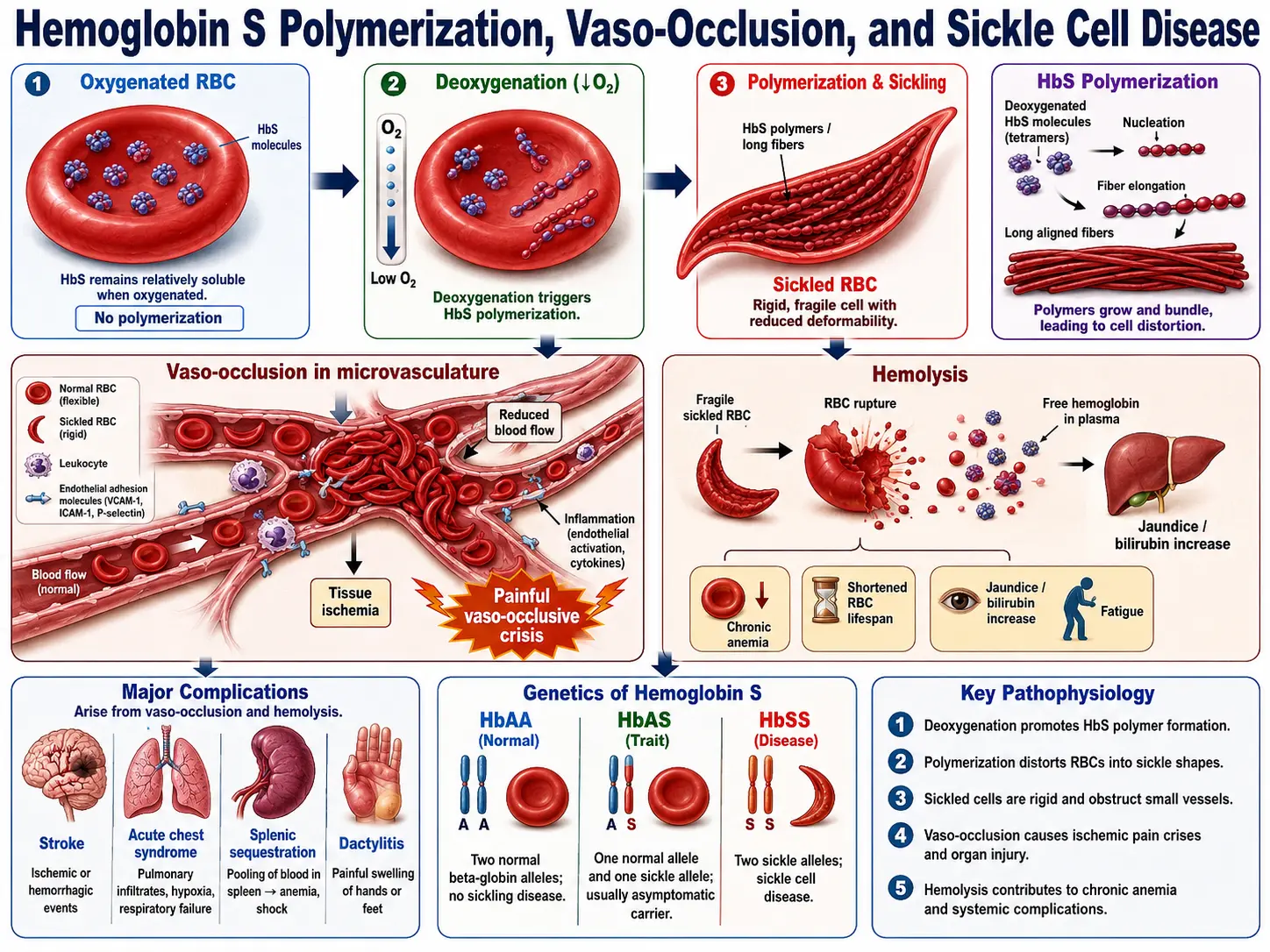
Table of Contents
- What is Sickle Cell Disease?
- Types of Sickle Cell Disease
- Common Symptoms of Sickle Cell Disease
- Causes and Risk Factors
- Diagnosis
- Treatment Options
- Prevention and Management Strategies
- Complications of Sickle Cell Disease
- Research Papers
- Connections
- Featured Videos
What is Sickle Cell Disease?
Sickle Cell Disease (SCD) is a group of inherited blood disorders characterized by the presence of abnormal hemoglobin, known as hemoglobin S. This causes red blood cells to become rigid, sticky, and shaped like crescent moons or sickles. These misshaped cells can block blood flow, leading to pain, organ damage, and other serious complications.
Types of Sickle Cell Disease
1. Sickle Cell Anemia (HbSS)
- Most common and severe form of SCD.
- Occurs when a person inherits two sickle cell genes, one from each parent.
2. Sickle Hemoglobin-C Disease (HbSC)
- Occurs when a person inherits one sickle cell gene and one gene for hemoglobin C.
- Symptoms are generally milder than HbSS but can still lead to complications.
3. Sickle Beta-Thalassemia (HbSβ-thalassemia)
- Occurs when a person inherits one sickle cell gene and one beta-thalassemia gene.
- Severity can range from mild to severe depending on the type (β0 or β+).
Common Symptoms of Sickle Cell Disease
Symptoms typically appear in early childhood and can vary in severity:
- Anemia: Chronic fatigue due to the rapid breakdown of sickle cells.
- Episodes of pain (pain crises): Sudden, severe pain caused by blocked blood flow.
- Swelling of hands and feet (dactylitis)
- Frequent infections: Due to damage to the spleen.
- Delayed growth and development
- Jaundice: Yellowing of the skin and eyes due to rapid breakdown of red blood cells.
Causes and Risk Factors
- Genetic inheritance: SCD is inherited in an autosomal recessive pattern, meaning both parents must pass down a sickle cell gene for a child to have the disease.
- Ethnicity: More common in individuals of African, Mediterranean, Middle Eastern, and Indian descent.
Diagnosis
- Newborn screening: Most babies in developed countries are screened for SCD shortly after birth.
- Blood tests: To detect the presence of hemoglobin S or other abnormal hemoglobin types.
- Genetic testing: Can confirm the diagnosis and identify carriers.
Treatment Options
- Medications:
- Hydroxyurea: Reduces the frequency of pain crises and may decrease the need for blood transfusions.
- Antibiotics: Prevents infections, especially in young children.
- Folic acid supplements: Helps with red blood cell production.
- Newer therapies: Such as voxelotor and crizanlizumab for managing SCD complications.
- Blood transfusions: To increase the number of normal red blood cells and reduce the risk of complications.
- Bone marrow or stem cell transplant: The only potential cure for SCD but involves significant risks and is generally considered for severe cases.
- Pain management: Over-the-counter pain relievers and prescription medications as needed.
Prevention and Management Strategies
- Stay hydrated: Helps prevent pain crises by maintaining blood flow.
- Avoid extreme temperatures: Cold and heat can trigger pain episodes.
- Regular medical check-ups: To monitor for complications and maintain health.
- Prophylactic antibiotics: To prevent infections.
- Healthy lifestyle: Balanced diet, regular exercise, and stress management.
Complications of Sickle Cell Disease
- Stroke: Due to blocked blood flow to the brain.
- Acute chest syndrome: A life-threatening condition causing chest pain, fever, and difficulty breathing.
- Organ damage: Prolonged lack of blood flow can damage organs like the liver, kidneys, and spleen.
- Pulmonary hypertension: High blood pressure in the lungs, leading to heart problems.
- Vision problems: Damage to the retina due to blocked blood vessels in the eye.
Research Papers
The following PubMed topic searches return current peer-reviewed literature relevant to this condition. Each link opens a live PubMed query.
- Sickle cell disease pathophysiology
- Hydroxyurea sickle cell disease
- Sickle cell vaso-occlusive crisis
- Sickle cell acute chest syndrome
- Sickle cell hematopoietic stem cell transplant
- Sickle cell gene therapy
- Sickle cell newborn screening
- L-glutamine sickle cell
- Crizanlizumab sickle cell
- Voxelotor sickle cell
- Sickle cell stroke
- Sickle cell disease guidelines
Connections
- Anemia
- Thalassemia
- Stroke
- Hemophilia
- Iron
- Folate
- Complete Blood Count
- Heart Failure
- Fatigue
- Jaundice
- Pulmonary Hypertension
- Chest Pain
- Deep Vein Thrombosis
- Hemochromatosis
- Cardiovascular Disease
- Kidney Stones
- Thrombocytopenia
- Disseminated Intravascular Coagulation