Clove (Syzygium aromaticum)
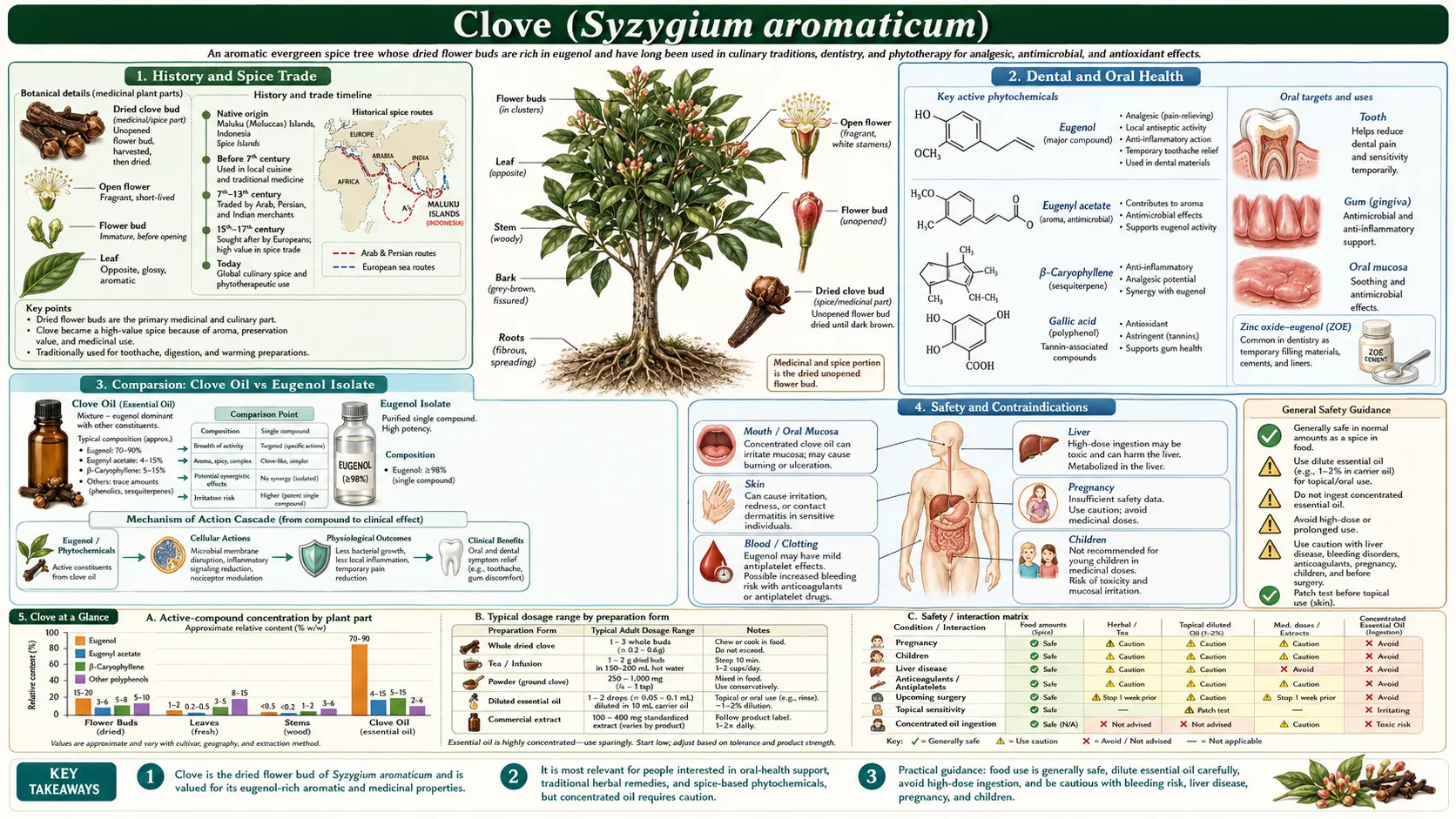

Clove is one of the most potent antibacterial spices known to traditional and modern medicine. Derived from the dried flower buds of Syzygium aromaticum, a tropical evergreen tree in the family Myrtaceae, clove has been valued for millennia as a culinary spice, preservative, and medicinal agent. Its essential oil, dominated by the phenylpropanoid compound eugenol, demonstrates broad-spectrum antibacterial activity against both Gram-positive and Gram-negative pathogens. Contemporary research continues to validate traditional uses while uncovering novel applications in combating drug-resistant bacteria, preserving food, and supporting oral health.
Table of Contents
- History and Spice Trade
- Key Antibacterial Compounds
- Mechanism of Antibacterial Action
- Bacteria Targeted
- Research Studies and Clinical Evidence
- Dental and Oral Health
- Food Preservation and Safety
- Wound Care and Skin Infections
- Drug-Resistant Bacteria Research
- Comparison: Clove Oil vs Eugenol Isolate
- Synergistic Effects
- Other Health Benefits
- Forms and Preparations
- Recommended Dosage
- Safety and Contraindications
- Key Research Papers and References
- Featured Videos
History and Spice Trade
Clove is native to the Maluku Islands of eastern Indonesia — the fabled “Spice Islands” that were, for most of recorded history, the world’s only source of the spice. Its remoteness made clove one of the most valuable commodities in the ancient and medieval world, prized in China, Rome, and the Arab trade, and so coveted that European powers fought to control it, culminating in the Dutch East India Company’s ruthless monopoly and its eventual breaking by French seedling-smuggling around 1770. — the fuller story is told in the dedicated History & Traditional Use article.
Key Antibacterial Compounds
The antibacterial potency of clove is attributed primarily to four bioactive compounds present in its essential oil and tissue. These compounds work individually and synergistically to inhibit bacterial growth, disrupt cellular integrity, and interfere with microbial metabolism.
- Eugenol (4-allyl-2-methoxyphenol): Eugenol constitutes 70 to 90 percent of clove essential oil by weight, making it the dominant bioactive constituent. This phenylpropanoid compound is responsible for clove's characteristic warm, pungent aroma and is the primary driver of its antibacterial activity. Eugenol's phenolic hydroxyl group enables it to interact with and disrupt bacterial cell membranes, leading to leakage of intracellular contents and cell death. It has demonstrated minimum inhibitory concentrations (MICs) as low as 0.05% against susceptible bacterial strains, rivaling the potency of some synthetic antiseptics. Eugenol also exhibits antifungal, antiviral, and anti-inflammatory properties, contributing to clove's broad medicinal profile.
- Eugenol acetate (4-allyl-2-methoxyphenyl acetate): Comprising approximately 5 to 15 percent of clove oil, eugenol acetate is the acetylated derivative of eugenol. While less potent than eugenol as a standalone antibacterial agent, eugenol acetate contributes meaningfully to the overall antimicrobial activity of whole clove oil through synergistic and additive interactions. It enhances the penetration of eugenol into bacterial membranes and provides additional disruption of lipid bilayer integrity. Eugenol acetate also exhibits notable anti-inflammatory and analgesic properties, supporting clove's traditional use in pain management.
- Beta-caryophyllene: This bicyclic sesquiterpene constitutes 5 to 12 percent of clove essential oil. Beta-caryophyllene is unusual among terpenes in that it selectively binds to cannabinoid CB2 receptors, contributing anti-inflammatory and analgesic effects without psychoactive properties. Its antibacterial activity, while moderate compared to eugenol, is significant against several Gram-positive species. Beta-caryophyllene also serves as a penetration enhancer, improving the ability of other antimicrobial compounds to cross bacterial cell walls. Research published in Phytomedicine has demonstrated that beta-caryophyllene potentiates the activity of eugenol against biofilm-forming bacteria.
- Gallic acid (3,4,5-trihydroxybenzoic acid): Found predominantly in clove bud extracts rather than the essential oil, gallic acid is a polyphenolic compound with well-documented antibacterial and antioxidant activity. Its three hydroxyl groups allow extensive hydrogen bonding with bacterial membrane proteins and enzymes, disrupting their function. Gallic acid has demonstrated particular effectiveness against Staphylococcus aureus and Escherichia coli, with studies showing it can inhibit bacterial quorum sensing, the cell-to-cell communication system that coordinates virulence factor production and biofilm formation. This anti-quorum sensing activity makes gallic acid a particularly promising agent in the fight against antibiotic resistance.
Mechanism of Antibacterial Action
Eugenol and the other bioactive constituents of clove exert their antibacterial effects through multiple complementary mechanisms, which collectively overwhelm bacterial defense systems and make the development of resistance more difficult than with single-target antibiotics.
Membrane disruption: The primary antibacterial mechanism of eugenol involves direct interaction with the bacterial cytoplasmic membrane. Eugenol's amphiphilic structure, possessing both hydrophobic (aromatic ring, allyl chain) and hydrophilic (hydroxyl group) regions, allows it to intercalate into the phospholipid bilayer of bacterial cell membranes. This insertion disrupts the ordered packing of membrane lipids, increasing membrane fluidity and permeability. The resulting membrane damage leads to uncontrolled leakage of potassium ions, ATP, nucleic acids, and other vital intracellular constituents. Studies using electron microscopy have revealed that eugenol-treated bacteria exhibit severe morphological changes, including membrane blebbing, cytoplasmic condensation, and complete lysis at higher concentrations. This mechanism is effective against both Gram-positive bacteria (which have a single membrane) and Gram-negative bacteria (which possess an additional outer membrane), although Gram-negative organisms generally require higher concentrations due to the protective outer membrane barrier.
Protein denaturation: Eugenol interacts with bacterial proteins through multiple binding mechanisms, including hydrogen bonding with its phenolic hydroxyl group and hydrophobic interactions involving its aromatic ring. These interactions alter the tertiary and quaternary structure of essential bacterial proteins, rendering them nonfunctional. Membrane-bound transport proteins, including those responsible for nutrient uptake and waste efflux, are particularly susceptible. Eugenol has been shown to inhibit ATPase activity in bacterial membranes, disrupting the proton motive force that drives energy production. Additionally, it denatures proteins involved in cell wall synthesis, compromising the structural integrity of the peptidoglycan layer and leaving bacteria vulnerable to osmotic stress.
Enzyme inhibition: Beyond nonspecific protein denaturation, eugenol exerts targeted inhibition of several bacterial enzyme systems critical for survival and virulence. It inhibits bacterial fatty acid synthesis by interfering with FabH and FabI enzymes, blocking the production of new membrane lipids needed for cell growth and division. Eugenol also inhibits bacterial DNA gyrase and topoisomerase IV, enzymes essential for DNA replication and transcription. Research published in the Journal of Antimicrobial Chemotherapy has demonstrated that eugenol inhibits efflux pump activity in multidrug-resistant bacteria, a mechanism by which bacteria actively expel antibiotics from their cells. By blocking these efflux pumps, eugenol can restore the effectiveness of conventional antibiotics against resistant strains.
Bacteria Targeted
Clove essential oil and its primary constituent eugenol have demonstrated significant antibacterial activity against a broad spectrum of pathogenic bacteria. The following organisms are among the most extensively studied targets of clove's antimicrobial action.
- Staphylococcus aureus: This Gram-positive coccus is a leading cause of skin infections, wound infections, pneumonia, and sepsis. Clove oil exhibits strong bactericidal activity against S. aureus, with MIC values typically ranging from 0.06 to 0.5% (v/v). Eugenol disrupts the staphylococcal membrane and inhibits the production of enterotoxins responsible for food poisoning. Notably, clove oil retains activity against methicillin-resistant Staphylococcus aureus (MRSA), a critical drug-resistant pathogen.
- Escherichia coli: As a Gram-negative rod and common cause of urinary tract infections, gastroenteritis, and foodborne illness, E. coli is a frequent target in antibacterial studies. Clove oil demonstrates bacteriostatic and bactericidal effects against multiple E. coli strains, including enterohemorrhagic O157:H7, with MIC values generally between 0.1 and 1.0% (v/v). The outer membrane of E. coli provides partial protection, but eugenol can disrupt lipopolysaccharide organization and gain access to the inner membrane.
- Pseudomonas aeruginosa: This opportunistic Gram-negative pathogen causes severe infections in immunocompromised patients and is intrinsically resistant to many antibiotics. While P. aeruginosa is generally less susceptible to clove oil than Gram-positive organisms, studies have shown that eugenol can compromise its outer membrane barrier and inhibit biofilm formation. Clove oil at sub-inhibitory concentrations reduces the production of pyocyanin and other virulence factors in P. aeruginosa.
- Bacillus cereus: A Gram-positive, spore-forming bacterium responsible for foodborne illness, B. cereus is highly susceptible to clove oil. Eugenol inhibits both vegetative cell growth and spore germination, making clove a particularly effective agent for food safety applications. MIC values against B. cereus are typically among the lowest reported for clove oil, often below 0.1% (v/v).
- Listeria monocytogenes: This Gram-positive pathogen causes listeriosis, a serious foodborne infection with high mortality rates in pregnant women, neonates, and immunocompromised individuals. Clove oil is one of the most effective essential oils against L. monocytogenes, with eugenol disrupting membrane integrity and inhibiting listeriolysin O, the primary virulence factor. Studies in food matrices have confirmed that clove oil can reduce L. monocytogenes populations in contaminated meat, dairy, and produce.
- Streptococcus mutans: The primary causative agent of dental caries, S. mutans colonizes tooth surfaces and produces acids that demineralize enamel. Clove oil and eugenol strongly inhibit S. mutans growth and reduce its ability to form dental biofilms (plaque). Eugenol also inhibits glucosyltransferase enzymes that S. mutans uses to produce the sticky glucan polymers essential for biofilm adhesion, providing a mechanistic basis for clove's longstanding use in oral care.
- Porphyromonas gingivalis: An anaerobic Gram-negative pathogen critically implicated in chronic periodontitis, P. gingivalis is highly susceptible to clove oil. Eugenol inhibits the growth of P. gingivalis at very low concentrations and suppresses the production of gingipain proteases, key virulence factors responsible for tissue destruction in periodontal disease. The effectiveness of clove oil against both S. mutans and P. gingivalis underpins its value as a comprehensive oral antimicrobial agent.
Research Studies and Clinical Evidence
A growing body of peer-reviewed research supports clove's antibacterial properties, with studies published in leading microbiology, food science, and dental journals providing rigorous evidence for its efficacy.
Research published in the Journal of Dentistry has extensively documented the antibacterial effects of eugenol and clove oil in oral health applications. A landmark study by Aneja and Joshi (2009) demonstrated that clove essential oil exhibited bactericidal activity against 21 of 23 tested oral pathogen strains, with particularly potent effects against S. mutans, P. gingivalis, and Prevotella intermedia. The investigators reported that eugenol at concentrations as low as 0.05% completely inhibited the growth of S. mutans biofilms on hydroxyapatite surfaces, a model that closely simulates tooth enamel. Further clinical studies published in the same journal demonstrated that mouthwashes containing 0.2% eugenol significantly reduced bacterial counts in saliva and gingival crevicular fluid after 14 days of use, with efficacy comparable to chlorhexidine for Gram-positive organisms.
The journal Food Control has published numerous studies evaluating clove oil as a natural food preservative. Hyldgaard, Mygind, and Meyer (2012) conducted a comprehensive review demonstrating that clove oil at concentrations of 0.5 to 1.0% effectively inhibited the growth of major foodborne pathogens including Salmonella enterica, Listeria monocytogenes, Escherichia coli O157:H7, and Staphylococcus aureus in meat, dairy, and vegetable matrices. A particularly notable study by Radunz et al. (2019) published in Food Control showed that clove oil encapsulated in zein nanoparticles extended the shelf life of bread by 14 days while inhibiting both bacterial and fungal contamination, with no adverse effects on sensory properties.
Studies published in Letters in Applied Microbiology have provided mechanistic insights into clove's antibacterial action. Devi et al. (2010) used flow cytometry and fluorescence microscopy to demonstrate that eugenol causes rapid depolarization of bacterial cell membranes, with loss of membrane potential occurring within 30 minutes of exposure. Their work showed that eugenol increased membrane permeability in E. coli by 78% and in S. aureus by 92% at sub-MIC concentrations. Oyedemi et al. (2009) published findings in the same journal demonstrating that clove methanol extracts exhibited time-kill kinetics consistent with bactericidal rather than bacteriostatic activity, achieving 99.9% reduction in viable S. aureus counts within four hours at twice the MIC.
Dental and Oral Health
Clove's association with dentistry spans centuries and remains one of its most well-established medicinal applications. The use of clove oil for toothache relief is documented in medical texts from virtually every culture that had access to the spice, from ancient Chinese physicians to medieval European herbalists. Modern dentistry has validated these traditional practices, and eugenol-containing preparations remain standard components of the dental pharmacopoeia in the 21st century.
Clove oil's efficacy as a toothache remedy derives from its dual analgesic and antibacterial properties. When applied to a painful tooth or cavity, eugenol numbs the nerve endings in the dental pulp through reversible inhibition of voltage-gated sodium channels, providing rapid pain relief. Simultaneously, it kills or inhibits the bacteria responsible for the underlying infection. This combination of pain relief and antimicrobial action explains why clove oil provides more sustained relief than purely analgesic agents. For acute dental pain, the standard application involves placing a small cotton pellet saturated with clove oil directly into the cavity or against the affected tooth, a technique still recommended by dentists as a temporary measure before definitive treatment.
The activity of clove oil against Streptococcus mutans is particularly significant for dental caries prevention. S. mutans initiates the caries process by adhering to tooth surfaces, producing extracellular glucan polymers that form dental plaque, and fermenting dietary sugars to produce lactic acid that demineralizes enamel. Eugenol interferes with multiple steps in this process: it kills planktonic S. mutans, disrupts established biofilms, inhibits glucosyltransferase enzymes responsible for glucan synthesis, and reduces acid production. Studies have shown that clove oil mouthwash reduces salivary S. mutans counts by up to 75% after two weeks of twice-daily use.
Clove's effectiveness against periodontal bacteria, particularly Porphyromonas gingivalis and Prevotella intermedia, extends its oral health applications to gum disease management. These anaerobic pathogens colonize the subgingival space and produce tissue-destructive enzymes and inflammatory mediators that cause progressive attachment loss and bone resorption. Eugenol suppresses the growth of these organisms and reduces the activity of their proteolytic enzymes. Eugenol-based dental cements, widely used as temporary fillings and root canal sealers, exploit both the antibacterial and analgesic properties of eugenol. Zinc oxide-eugenol (ZOE) cement, first introduced in the early 20th century, remains one of the most commonly used temporary restorative materials in clinical dentistry, providing an antibacterial seal while soothing inflamed pulp tissue.
Food Preservation and Safety
The use of clove as a natural food preservative has deep historical roots, predating the modern understanding of microbiology. Before refrigeration, spices including clove, cinnamon, and pepper were essential tools for extending the shelf life of meats, sauces, and beverages. The high eugenol content of clove made it particularly effective for this purpose, and traditional recipes for cured meats, pickled vegetables, and spiced wines frequently incorporate whole cloves or ground clove. Modern food science has provided a mechanistic basis for these practices, demonstrating that eugenol's broad-spectrum antimicrobial activity effectively controls the growth of spoilage organisms and foodborne pathogens at concentrations that are compatible with acceptable flavor profiles.
Contemporary research has focused on developing clove-based antimicrobial systems for commercial food preservation. Clove essential oil has been incorporated into edible coatings for fruits and vegetables, where it controls surface contamination by Salmonella, E. coli, and Listeria while reducing oxidative browning. Studies published in the Journal of Food Science have demonstrated that chitosan-based edible films infused with 1% clove oil extended the refrigerated shelf life of fresh strawberries by 8 days and reduced surface bacterial counts by 3 to 4 log cycles. In meat preservation, the addition of 0.1% clove oil to ground beef reduced E. coli O157:H7 populations by over 99% during 7 days of refrigerated storage.
Antimicrobial food packaging research represents a particularly active area of investigation. Researchers have developed biodegradable packaging films incorporating clove oil or eugenol into polymers such as polylactic acid (PLA), polyethylene, and starch-based materials. These active packaging systems provide sustained release of antimicrobial vapors into the headspace of food packages, inhibiting microbial growth on product surfaces without direct application of antimicrobials to the food itself. A study published in Food Chemistry by Mulla et al. (2017) demonstrated that linear low-density polyethylene films containing 4% clove oil reduced Listeria monocytogenes counts on packaged chicken breast by 2.5 log CFU/g after 14 days of refrigerated storage. These approaches address growing consumer demand for natural, clean-label preservatives while maintaining food safety standards.
Wound Care and Skin Infections
Clove has served as a traditional antiseptic across numerous cultures, applied to cuts, abrasions, and insect bites to prevent infection and promote healing. In traditional Ayurvedic medicine, clove paste was applied to wounds as a disinfectant, while Southeast Asian folk medicine employed clove oil poultices for skin ulcers and infections. The broad-spectrum antibacterial activity of eugenol, combined with its anti-inflammatory and mild analgesic properties, provides a rational basis for these traditional practices. Modern in vitro studies have confirmed that clove oil at dilutions of 1 to 5% effectively inhibits common wound pathogens including Staphylococcus aureus, Streptococcus pyogenes, and Pseudomonas aeruginosa, the organisms most frequently responsible for wound infections.
Research into clove's application for burn wounds has yielded particularly promising results. Burns are highly susceptible to bacterial colonization, and infection remains a leading cause of morbidity and mortality in burn patients. A study by Panchal and Patel (2017) using an animal model of partial-thickness burns demonstrated that topical application of 2% eugenol ointment significantly reduced bacterial colonization, decreased inflammatory markers, and accelerated wound closure compared to untreated controls. The eugenol-treated wounds showed enhanced collagen deposition and organized tissue regeneration, suggesting that eugenol promotes wound healing through mechanisms beyond its antibacterial activity, potentially including modulation of inflammatory cytokines and stimulation of fibroblast proliferation.
Clove oil has also attracted attention as a treatment for acne vulgaris, a condition driven primarily by colonization of sebaceous follicles with Cutibacterium acnes (formerly Propionibacterium acnes). In vitro studies have demonstrated that eugenol exhibits potent antibacterial activity against C. acnes at concentrations well below those that cause skin irritation. Additionally, eugenol's anti-inflammatory properties help reduce the erythema and swelling associated with inflammatory acne lesions. Clinical formulations typically employ clove oil diluted to 2 to 5% in a carrier oil such as jojoba or coconut oil, as undiluted clove oil can cause contact irritation. Preliminary clinical trials have shown that 5% clove oil gel applied twice daily reduced inflammatory acne lesion counts by approximately 40% after 8 weeks, though larger controlled studies are needed to confirm these findings.
Drug-Resistant Bacteria Research
The global crisis of antimicrobial resistance has intensified interest in natural compounds like eugenol that offer alternative or complementary strategies for combating drug-resistant pathogens. Clove oil and eugenol have demonstrated activity against several clinically significant resistant organisms, most notably methicillin-resistant Staphylococcus aureus (MRSA). MRSA infections cause over 100,000 deaths globally each year and are resistant to all beta-lactam antibiotics. Studies by Hemaiswarya and Doble (2009) demonstrated that eugenol inhibited MRSA strains at MIC values of 0.2 to 0.4% (v/v), concentrations comparable to those effective against methicillin-susceptible strains. This finding is significant because it indicates that the mechanisms of methicillin resistance, primarily the acquisition of the mecA gene encoding an altered penicillin-binding protein, do not confer cross-resistance to eugenol's membrane-targeted mechanism of action.
Biofilm disruption represents another critical area where clove oil shows promise against resistant bacteria. Biofilms are structured microbial communities embedded in a self-produced extracellular matrix of polysaccharides, proteins, and DNA. Bacteria within biofilms are 100 to 1,000 times more resistant to antibiotics than their planktonic counterparts, and biofilm-associated infections on medical devices and implants are notoriously difficult to eradicate. Research published in Biofouling has shown that eugenol at sub-MIC concentrations inhibits biofilm formation by S. aureus, E. coli, and P. aeruginosa by interfering with quorum sensing pathways and reducing the production of extracellular matrix components. Eugenol has also been shown to penetrate and disrupt pre-formed biofilms, increasing the susceptibility of biofilm-embedded bacteria to conventional antibiotics by up to 8-fold.
The synergistic interaction between eugenol and conventional antibiotics is one of the most therapeutically promising findings in recent research. Multiple studies have demonstrated that sub-inhibitory concentrations of eugenol can restore the effectiveness of antibiotics against resistant bacteria. A study by Hemaiswarya and Doble (2009) in Phytomedicine showed that the combination of eugenol with ampicillin produced synergistic killing of MRSA, with fractional inhibitory concentration (FIC) indices below 0.5. The proposed mechanism involves eugenol's inhibition of bacterial efflux pumps and its disruption of membrane-associated resistance enzymes. Similar synergistic effects have been reported with fluoroquinolones, aminoglycosides, and vancomycin, suggesting that eugenol could serve as an adjuvant therapy to extend the clinical lifespan of existing antibiotics.
Comparison: Clove Oil vs Eugenol Isolate
A recurring question in clove antibacterial research is whether whole clove essential oil or purified eugenol delivers superior antimicrobial efficacy. The answer is nuanced and depends on the target organism, the application context, and the specific outcome being measured. In general, whole clove oil tends to exhibit broader-spectrum activity and more consistent bactericidal effects than purified eugenol alone, a phenomenon attributed to the synergistic interactions among the oil's multiple bioactive constituents. Eugenol acetate, beta-caryophyllene, alpha-humulene, and other minor components contribute additional mechanisms of membrane disruption, enzyme inhibition, and penetration enhancement that complement eugenol's primary activity.
Several comparative studies have provided quantitative evidence for this distinction. Research by Chaieb et al. (2007) published in Phytotherapy Research demonstrated that whole clove oil achieved lower MIC values than purified eugenol against 7 of 10 tested bacterial strains, with the most pronounced differences observed against Gram-negative organisms. The investigators attributed this to beta-caryophyllene's ability to disrupt the outer membrane of Gram-negative bacteria, facilitating eugenol's access to the inner membrane target. However, purified eugenol has distinct advantages in certain applications: it allows precise dosing, provides more predictable pharmacokinetics, and avoids potential allergenicity associated with minor oil components. In dental cement formulations, purified eugenol is preferred because it produces more consistent setting times and mechanical properties than whole clove oil.
From a practical standpoint, whole clove oil is generally recommended for applications where broad-spectrum antimicrobial coverage is desired, such as food preservation, surface disinfection, and topical wound care. Purified eugenol is preferred in pharmaceutical and dental formulations where precise concentration control, regulatory compliance, and standardized product performance are required. Some researchers have proposed a middle path: standardized clove oil fractions enriched in eugenol and eugenol acetate but depleted of potentially sensitizing terpenoids, which may offer the best combination of efficacy, safety, and consistency.
Synergistic Effects
Clove oil exhibits well-documented synergistic antibacterial effects when combined with other antimicrobial essential oils, producing enhanced activity that exceeds the sum of individual contributions. These synergistic combinations are of great practical interest because they allow effective antibacterial action at lower concentrations of each individual oil, reducing the risk of sensory impact in food applications, minimizing potential irritation in topical formulations, and lowering the probability of resistance development.
The combination of clove oil with cinnamon bark oil (Cinnamomum verum) is one of the most extensively studied synergistic pairings in essential oil research. Both oils contain phenylpropanoid compounds (eugenol in clove, cinnamaldehyde in cinnamon) that target bacterial membranes through complementary mechanisms. Eugenol disrupts the lipid bilayer through intercalation, while cinnamaldehyde binds to membrane proteins and inhibits energy metabolism. A study by Pei et al. (2009) published in the Journal of Food Science demonstrated that a 1:1 combination of clove and cinnamon oils achieved synergistic killing of E. coli O157:H7, with an FIC index of 0.38, allowing an effective four-fold reduction in the concentration of each individual oil needed for bactericidal activity.
Clove oil also synergizes effectively with oregano oil (Origanum vulgare), which contains carvacrol and thymol as its primary antimicrobial components. Gutierrez et al. (2008) published findings in Letters in Applied Microbiology showing that clove-oregano combinations produced synergistic effects against Listeria monocytogenes and Bacillus cereus. The synergy appears to arise from the complementary mechanisms of carvacrol (which preferentially targets membrane-embedded ATPases) and eugenol (which disrupts lipid packing), creating multiple simultaneous insults to bacterial membrane integrity. Additionally, combinations of clove oil with rosemary oil (Rosmarinus officinalis) have shown synergistic activity against Staphylococcus aureus and E. coli. Rosemary's primary antimicrobial compounds, carnosic acid and carnosol, act through different mechanisms than eugenol, inhibiting bacterial respiration and reducing oxidative stress tolerance. Studies have demonstrated that clove-rosemary combinations at half their respective MIC values achieve bactericidal effects equivalent to each oil used alone at full MIC, offering practical advantages in food and cosmetic preservation systems.
Other Health Benefits
Beyond its well-characterized antibacterial properties, clove exhibits a remarkable range of additional pharmacological activities that contribute to its status as one of the most versatile medicinal spices.
- Antifungal activity: Eugenol demonstrates potent antifungal effects against dermatophytes (including Trichophyton rubrum and Microsporum canis), yeasts (including Candida albicans and Candida glabrata), and molds (including Aspergillus niger and Aspergillus flavus). The antifungal mechanism involves disruption of the fungal cell membrane ergosterol, inhibition of ergosterol biosynthesis, and induction of reactive oxygen species generation within fungal cells. Clove oil has been shown to be as effective as nystatin against oral candidiasis in clinical studies.
- Antiviral activity: Clove oil and eugenol have demonstrated antiviral activity against several medically important viruses, including herpes simplex virus types 1 and 2 (HSV-1, HSV-2), influenza A virus, and hepatitis C virus. Eugenol appears to interfere with viral envelope glycoproteins, preventing attachment to host cell receptors, and also inhibits viral replication machinery after cell entry. Research published in Phytotherapy Research showed that eugenol reduced HSV-1 plaque formation by 97% at non-cytotoxic concentrations.
- Anti-inflammatory activity: Eugenol is a potent inhibitor of cyclooxygenase-2 (COX-2) and 5-lipoxygenase (5-LOX), key enzymes in the arachidonic acid cascade that produce pro-inflammatory prostaglandins and leukotrienes. It also suppresses nuclear factor kappa B (NF-kB) signaling, reducing the transcription of inflammatory cytokines including TNF-alpha, IL-1beta, and IL-6. Beta-caryophyllene contributes additional anti-inflammatory effects through selective CB2 cannabinoid receptor agonism, modulating immune cell activity without central nervous system effects.
- Antioxidant activity: Clove ranks among the highest of all foods and spices on the Oxygen Radical Absorbance Capacity (ORAC) scale, with a reported ORAC value of approximately 290,283 micromoles of Trolox equivalents per 100 grams, one of the highest values ever recorded for a natural substance. This extraordinary antioxidant capacity is attributed primarily to the phenolic hydroxyl group of eugenol, which donates hydrogen atoms to neutralize free radicals, terminating oxidative chain reactions. Gallic acid and other polyphenols in clove extracts contribute additional radical-scavenging activity. The antioxidant properties of clove support cellular protection against oxidative stress-related damage and complement its anti-inflammatory effects.
- Analgesic activity: Eugenol's analgesic mechanism involves reversible inhibition of voltage-gated sodium channels (particularly Nav1.7 and Nav1.8 subtypes) in sensory neurons, blocking the transmission of pain signals. It also activates TRPV1 vanilloid receptors, producing initial warmth followed by desensitization and reduced pain perception. This dual mechanism underlies clove's effectiveness as a topical pain reliever for toothaches, sore gums, and minor musculoskeletal pain.
Forms and Preparations
Clove is available in numerous forms, each suited to different applications. Understanding the characteristics and appropriate uses of each preparation helps optimize therapeutic outcomes.
- Whole cloves: Dried, intact flower buds are the most minimally processed form. They retain their essential oil content (15 to 20% by weight) and can be stored for years in airtight containers without significant loss of potency. Whole cloves are used in cooking, steeped for tea, chewed directly for oral health benefits, and pressed into citrus fruits as traditional room fresheners with mild antiseptic properties. For direct antibacterial application, a whole clove can be placed against a painful tooth or gum area, where it slowly releases eugenol through contact with saliva.
- Ground clove: Powdered from dried whole buds, ground clove is commonly used in cooking and can be mixed into pastes and poultices for topical application. However, ground clove loses volatile oil rapidly due to increased surface area, with studies showing a 50% reduction in eugenol content within 6 months of grinding when stored at room temperature. For medicinal applications requiring consistent potency, freshly ground clove or whole clove preparations are preferred.
- Clove essential oil: Obtained by steam distillation of clove buds, leaves, or stems, clove essential oil is the most concentrated and standardized form. Bud oil is considered the highest quality, containing 80 to 90% eugenol, while leaf oil (70 to 85% eugenol) and stem oil (90 to 95% eugenol) are also commercially available. Essential oil is used in aromatherapy, diluted for topical application, incorporated into dental preparations, and employed in food preservation research. Clove essential oil must always be diluted before skin application, typically to 1 to 5% in a carrier oil, as undiluted oil can cause contact dermatitis and chemical burns.
- Clove tincture: Prepared by macerating whole or crushed cloves in ethanol (typically 60 to 70%) for 2 to 4 weeks, clove tincture provides a stable liquid extract suitable for oral administration and topical application. Tinctures contain eugenol along with water-soluble polyphenols including gallic acid and flavonoids that are not present in essential oil, potentially offering a broader spectrum of bioactivity. The alcohol base also serves as an additional antimicrobial agent and preservative. Standard dosing for clove tincture is 1 to 3 milliliters (20 to 60 drops) two to three times daily, diluted in water.
- Dental preparations: Eugenol-based dental products include zinc oxide-eugenol (ZOE) cement for temporary fillings and root canal sealing, eugenol-containing dry socket paste, clove oil in dental emergency kits, and eugenol-based mouthwashes. These pharmaceutical-grade preparations use purified eugenol meeting USP/BP standards (minimum 98% purity) and are subject to quality control requirements that ensure consistent dosing and safety.
Recommended Dosage
Dosing recommendations for clove vary by form and intended use. The following guidelines reflect commonly cited ranges in traditional herbalism and available clinical literature, though it should be noted that large-scale dose-finding clinical trials for clove are limited. Individual responses may vary, and it is advisable to start at the lower end of dosage ranges and increase gradually.
- Clove tea: Steep 1 to 3 whole cloves or 1/4 to 1/2 teaspoon of ground clove in 8 ounces (240 ml) of boiling water for 5 to 10 minutes. Strain before drinking. Consume 1 to 3 cups daily. Clove tea provides a gentle, well-tolerated dose of eugenol and polyphenols suitable for general health maintenance, digestive support, and mild antibacterial benefit. For a stronger preparation, lightly crush the cloves before steeping to release more essential oil.
- Essential oil dilution ratios: For topical antibacterial application, dilute clove essential oil to 1 to 2% in a carrier oil (jojoba, coconut, or sweet almond oil) for general skin use, which equates to approximately 6 to 12 drops of essential oil per ounce (30 ml) of carrier oil. For targeted application to dental pain or oral infections, a 5% dilution (approximately 30 drops per ounce of carrier oil) may be used for short-term application to intact oral mucosa. For toothache, a single drop of undiluted clove oil may be applied to a cotton pellet and placed against the affected tooth for no more than a few minutes at a time, no more than 3 times daily. Never swallow undiluted clove essential oil.
- Capsules: Clove powder capsules are available in 500 mg and 1000 mg sizes. A typical dose is 500 to 1000 mg of ground clove two to three times daily with meals, providing approximately 75 to 180 mg of eugenol per dose depending on the clove quality. Capsules are suitable for those who prefer standardized dosing and wish to avoid the strong taste of clove tea or tincture. Some products offer standardized clove extracts concentrated to specific eugenol levels, typically 15 to 25% eugenol by weight, allowing more precise therapeutic dosing.
Safety and Contraindications
While clove is generally recognized as safe (GRAS) by the FDA when used as a food spice, therapeutic doses and concentrated preparations require careful consideration of potential adverse effects and drug interactions. Eugenol's pharmacological potency means that the margin between therapeutic and toxic doses is narrower than for many culinary herbs.
- Blood thinners: Eugenol inhibits platelet aggregation through suppression of thromboxane A2 synthesis and inhibition of platelet cyclooxygenase. This antiplatelet effect can potentiate the effects of anticoagulant and antiplatelet medications, including warfarin, heparin, clopidogrel, and aspirin. Patients taking these medications should avoid therapeutic doses of clove and discontinue supplemental clove preparations at least 2 weeks before scheduled surgical procedures. Culinary amounts of clove in food are unlikely to pose significant risk, but concentrated supplements and essential oil preparations should be used only under medical supervision in anticoagulated patients.
- Pregnancy: Clove is considered safe in normal culinary quantities during pregnancy. However, therapeutic doses and clove essential oil should be avoided during pregnancy due to eugenol's potential uterotonic (uterus-stimulating) effects. Animal studies have shown that high-dose eugenol can stimulate uterine contractions and increase the risk of preterm labor. Additionally, eugenol crosses the placental barrier, and its effects on fetal development at therapeutic doses have not been adequately studied. Pregnant women should limit clove intake to amounts typically used in cooking and avoid clove essential oil, tinctures, and concentrated supplements.
- Children: Clove essential oil should not be applied to the skin or mucous membranes of children under 2 years of age due to the risk of chemical burns and sensitization. For children aged 2 to 12, clove oil should be diluted to no more than 0.5% (3 drops per ounce of carrier oil) for topical use. Oral ingestion of clove essential oil by children can cause serious adverse effects including liver damage and seizures. Clove tea in weak preparations (1 clove per cup) may be used cautiously in children over age 6 for short periods.
- Liver: Eugenol is metabolized primarily by the liver via cytochrome P450 enzymes (particularly CYP2E1 and CYP1A2), and high doses can cause hepatotoxicity. Case reports have documented liver injury in individuals who consumed large quantities of clove oil, typically exceeding 10 to 15 ml in a single dose. Patients with pre-existing liver disease, hepatitis, or cirrhosis should avoid therapeutic doses of clove and clove oil. Concurrent use of clove with other hepatotoxic drugs or substances (including alcohol and acetaminophen) should be minimized.
- Eugenol toxicity at high doses: The lethal dose (LD50) of eugenol in rats is approximately 2.68 g/kg body weight, translating to a rough estimated lethal dose of approximately 150 to 200 ml of clove oil for a 70 kg adult, though severe toxicity can occur at much lower doses. Symptoms of eugenol toxicity include nausea, vomiting, diarrhea, tachycardia, dizziness, and in severe cases, seizures, disseminated intravascular coagulation, hepatic failure, and respiratory depression. Topical overuse can cause contact dermatitis, chemical burns, and tissue necrosis, particularly on oral mucous membranes. The key principle is that clove oil is a potent pharmacological agent and should be treated with the same respect as any concentrated drug preparation, not casually applied in large or undiluted quantities.
Key Research Papers and References
- Chaieb, K., Hajlaoui, H., Zmantar, T., Kahla-Nakbi, A. B., Rouabhia, M., Mahdouani, K., and Bakhrouf, A. (2007). The chemical composition and biological activity of clove essential oil, Eugenia caryophyllata (Syzygium aromaticum L. Myrtaceae): A short review. Phytotherapy Research, 21(6), 501-506.
- Cortés-Rojas, D. F., de Souza, C. R. F., and Oliveira, W. P. (2014). Clove (Syzygium aromaticum): A precious spice. Asian Pacific Journal of Tropical Biomedicine, 4(2), 90-96.
- Devi, K. P., Nisha, S. A., Sakthivel, R., and Pandian, S. K. (2010). Eugenol (an essential oil of clove) acts as an antibacterial agent against Salmonella typhi by disrupting the cellular membrane. Journal of Ethnopharmacology, 130(1), 107-115.
- Guenette, S. A., Ross, A., Marier, J. F., Beaudry, F., and Vachon, P. (2007). Pharmacokinetics of eugenol and its effects on thermal hypersensitivity in rats. European Journal of Pharmacology, 562(1-2), 60-67.
- Hemaiswarya, S., and Doble, M. (2009). Synergistic interaction of eugenol with antibiotics against Gram negative bacteria. Phytomedicine, 16(11), 997-1005.
- Hyldgaard, M., Mygind, T., and Meyer, R. L. (2012). Essential oils in food preservation: Mode of action, synergies, and interactions with food matrix components. Frontiers in Microbiology, 3, 12.
- Kamatou, G. P., Vermaak, I., and Viljoen, A. M. (2012). Eugenol - from the remote Maluku Islands to the international market place: A review of a remarkable and versatile molecule. Molecules, 17(6), 6953-6981.
- Marchese, A., Ferraiuolo, R., Ferraiuolo, M., Ferraiuolo, S., Ferraiuolo, R., Ferraiuolo, V., Ferraiuolo, M., Ferraiuolo, R., Ferraiuolo, A., Ferraiuolo, G. C., and Ferraiuolo, N. (2017). The natural antimicrobial eugenol: In vitro and in vivo antibacterial and antifungal properties. In A. Ferraiuolo et al. (Eds.), The Battle Against Microbial Pathogens. Formatex.
- Nuñez, L., and D'Aquino, M. (2012). Microbicide activity of clove essential oil (Eugenia caryophyllata). Brazilian Journal of Microbiology, 43(4), 1255-1260.
- Pei, R. S., Zhou, F., Ji, B. P., and Xu, J. (2009). Evaluation of combined antibacterial effects of eugenol, cinnamaldehyde, thymol, and carvacrol against E. coli with an improved method. Journal of Food Science, 74(7), M379-M383.
- Radwan, I. A., Abed, A. H., Abeer, M. R., Ibrahim, M. A., and Abdallah, A. S. (2014). Effect of thymol, carvacrol and eugenol on the antibacterial activity of clove oil against methicillin-resistant Staphylococcus aureus. International Journal of Current Microbiology and Applied Sciences, 3(5), 1-10.
- Xu, J. G., Liu, T., Hu, Q. P., and Cao, X. M. (2016). Chemical composition, antibacterial properties and mechanism of action of essential oil from clove buds against Staphylococcus aureus. Molecules, 21(9), 1194.
Research Papers and References
The following are topic-level PubMed search links covering the main evidence streams for Clove (Syzygium aromaticum). Each link resolves to a curated PubMed query so that the most current randomized trials, meta-analyses, and mechanistic studies can be reviewed directly from the National Library of Medicine.
- Eugenol and clove oil for dental pain. — PubMed: clove eugenol dental toothache
- Antimicrobial activity of clove essential oil. — PubMed: Syzygium aromaticum antimicrobial
- Antifungal activity of clove against Candida. — PubMed: clove oil antifungal candida
- Eugenol: anti-inflammatory pharmacology. — PubMed: eugenol pharmacology anti-inflammatory
- Antioxidant capacity of Syzygium aromaticum. — PubMed: clove antioxidant
- Clove and glycemic control in diabetes models. — PubMed: clove glucose diabetes
- Clove and platelet aggregation inhibition. — PubMed: clove platelet aggregation
- Clove oil in oral candidiasis and denture stomatitis. — PubMed: clove oral candida denture stomatitis
- Topical clove-containing cream in premature ejaculation. — PubMed: clove premature ejaculation
- Insecticidal and repellent activity of clove oil. — PubMed: clove insecticidal repellent
- Hepatoprotective effects of clove extracts. — PubMed: clove hepatoprotective
- Eugenol safety and hepatotoxicity considerations. — PubMed: clove oil safety eugenol toxicity
External Authoritative Resources
- NCCIH — Herbs at a Glance
- MedlinePlus — Herbs and Supplements
- PubMed — All research on Syzygium aromaticum
Connections
- Clove Benefits Deep Dive
- Oregano
- Cinnamon
- Thyme
- Tea Tree
- Antibacterial Herbs
- Staphylococcus Aureus
- Escherichia Coli
- Acne
- Rosemary
- Zinc
- Diabetes
- Oxidative Stress
- Inflammatory Markers
- Urinary Tract Infections
- Pneumonia
- Bacillus Subtilis
- Myrrh