Pleural Effusion
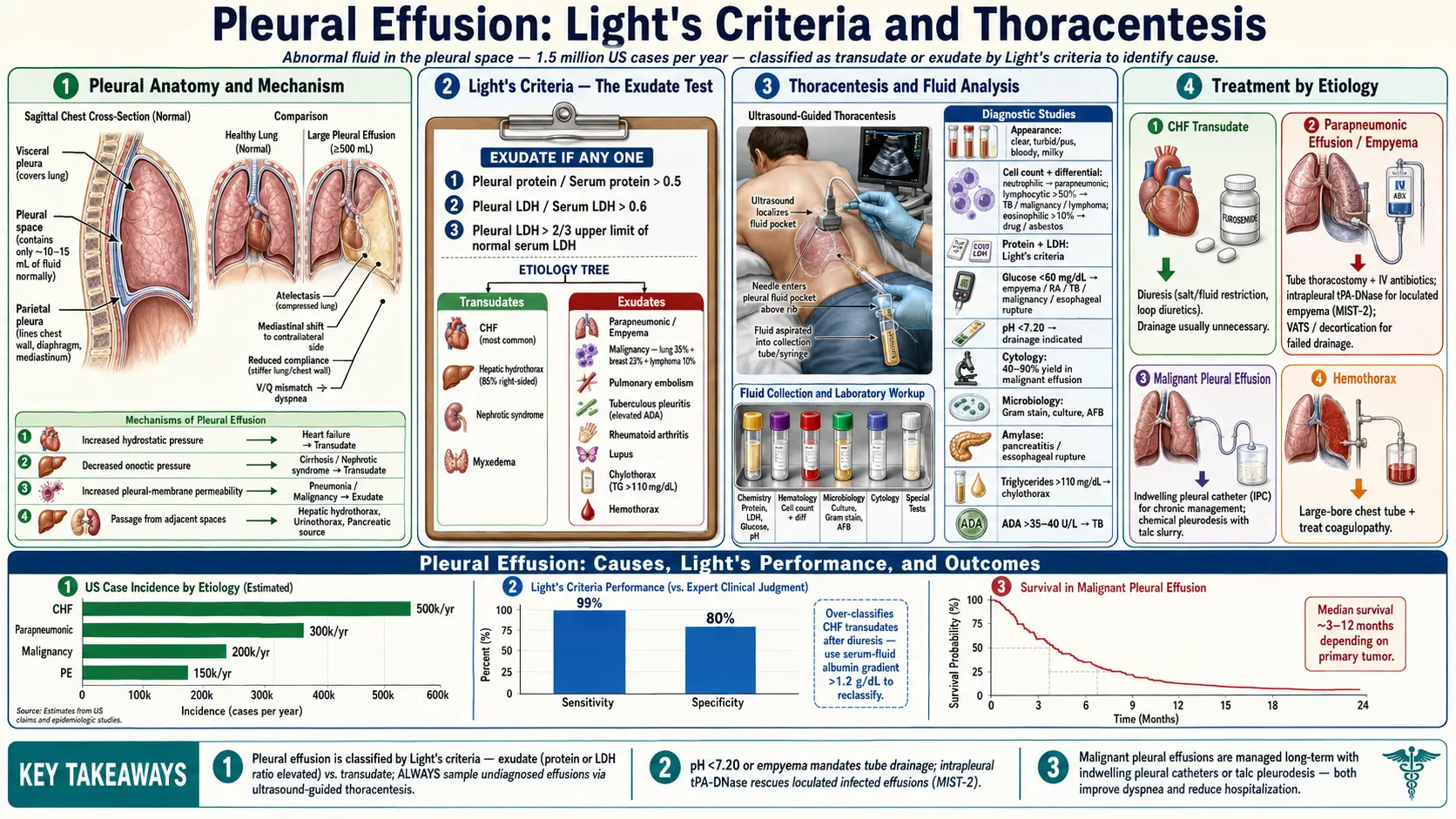
Table of Contents
- Overview
- Epidemiology
- Pathophysiology
- Etiology and Risk Factors
- Clinical Presentation
- Diagnosis — Light's Criteria
- Treatment
- Complications
- Prognosis
- Prevention
- Recent Research and Advances
- Research Papers
- Connections
- Featured Videos
1. Overview
A pleural effusion is an abnormal accumulation of fluid in the pleural space — the potential space between the visceral and parietal pleural membranes that surround each lung. Under normal conditions, approximately 10–15 mL of fluid is present in the pleural space, maintained by a dynamic balance of hydrostatic, oncotic, and lymphatic forces. When this balance is disrupted, fluid accumulates and can progressively impair respiratory mechanics.
Pleural effusions are classified by fluid composition as either transudates or exudates using Light's criteria — a distinction that is fundamental to identifying the underlying etiology and guiding management. They represent one of the most common pulmonary conditions encountered in clinical medicine, with over 1.5 million cases annually in the United States.
2. Epidemiology
Pleural effusions affect approximately 1.5 million patients per year in the United States. The most common etiologies in developed countries are:
- Congestive heart failure (~500,000 cases/year in the US) — most common cause of transudative effusion
- Pneumonia/parapneumonic effusion (~300,000 cases/year)
- Malignancy (~200,000 cases/year) — most common cause of exudative effusion in adults >60 years
- Pulmonary embolism (~150,000 cases/year)
Malignant pleural effusions have a particularly high burden: lung cancer accounts for ~35%, breast cancer ~23%, and lymphoma ~10% of cases. Tuberculosis remains the most common cause of pleural effusion globally, particularly in high-burden regions (sub-Saharan Africa, South and Southeast Asia, Eastern Europe). In hospitalized patients, the prevalence of pleural effusion detected by ultrasound is approximately 8% of all admissions.
3. Pathophysiology
The normal pleural space maintains physiological fluid homeostasis through four mechanisms that, when disrupted, lead to effusion:
- Increased hydrostatic pressure: Elevated pulmonary capillary wedge pressure (left heart failure) or systemic venous hypertension (right heart failure) increases filtration of fluid across the pleural membrane, overwhelming lymphatic absorption. Result: transudate.
- Decreased oncotic pressure: Hypoalbuminemia (<1.5 g/dL typically required) — from cirrhosis, nephrotic syndrome, malnutrition — reduces the osmotic force retaining fluid within vessels. Result: transudate (often bilateral).
- Increased pleural membrane permeability: Pleural inflammation (from pneumonia, malignancy, PE, rheumatoid arthritis) disrupts tight junctions, allowing protein-rich fluid to accumulate. Lymphatic obstruction (tumor infiltration of mediastinal lymphatics, chylothorax) impairs fluid drainage. Result: exudate.
- Fluid passage from adjacent spaces: Hepatic hydrothorax — ascitic fluid traverses diaphragmatic defects (typically right-sided) due to negative intrathoracic pressure; urinothorax — urine from urinary tract obstruction or injury; pancreatic effusion — amylase-rich pancreatic secretions track through the aortic or esophageal hiatus.
Large effusions (>500 mL) compress the underlying lung (atelectasis), shift the mediastinum toward the contralateral side, and reduce lung compliance. This mechanically restricts tidal volume, increases respiratory work, and causes V/Q mismatch, producing dyspnea and hypoxemia proportional to effusion size and the patient's underlying respiratory reserve.
4. Etiology and Risk Factors
Transudates
- Congestive heart failure (most common cause): bilateral effusions; right > left
- Hepatic hydrothorax: cirrhosis with portal hypertension; right-sided in 85%
- Nephrotic syndrome: severe hypoalbuminemia; bilateral; dependent edema
- Peritoneal dialysis: dialysate tracking into pleural space via diaphragmatic defects
- Myxedema: severe hypothyroidism; serositis
- Superior vena cava obstruction: impaired venous drainage
- Atelectasis: increased transpleural pressure gradient (suction effect)
Exudates
Parapneumonic effusions and empyema:
- Simple parapneumonic (sterile exudate): bacterial pneumonia adjacent to pleural space
- Complicated parapneumonic: bacterial invasion; low pH, low glucose, LDH >1000 IU/L
- Empyema thoracis: frank pus in the pleural space; Streptococcus milleri, S. aureus, anaerobes most common pathogens
- Tuberculous pleuritis: hypersensitivity reaction to mycobacterial antigens; lymphocytic exudate; elevated adenosine deaminase (ADA)
Malignant pleural effusions:
- Lung carcinoma (most common primary)
- Breast cancer, lymphoma, ovarian cancer, gastric cancer, mesothelioma
- Mechanism: direct pleural metastases, lymphatic obstruction, superior vena cava syndrome
Other exudative causes:
- Pulmonary embolism (usually small; exudate or transudate; bloody)
- Rheumatoid arthritis (typically left-sided; very low glucose; elevated cholesterol)
- Systemic lupus erythematosus (bilateral; pleuritis; positive ANA in fluid)
- Pancreatitis/pancreatic pseudocyst (left-sided or bilateral; elevated amylase)
- Drug-induced: amiodarone, methotrexate, nitrofurantoin, dasatinib, hydralazine
- Chylothorax: thoracic duct disruption (trauma, lymphoma, surgery); milky fluid; elevated triglycerides (>110 mg/dL)
- Hemothorax: trauma, malignancy, coagulopathy; pleural fluid hematocrit >50% of serum hematocrit
- Post-cardiac injury syndrome (Dressler's): after MI or cardiac surgery
- Meigs syndrome: benign ovarian fibroma + right pleural effusion + ascites
- Yellow nail syndrome: triad of yellow nails + lymphedema + pleural effusion
5. Clinical Presentation
Symptoms depend on effusion volume, rate of accumulation, and underlying disease. Small effusions (<300 mL) may be asymptomatic.
Symptoms:
- Dyspnea (most common; proportional to effusion size and underlying lung reserve)
- Pleuritic chest pain (sharp, worsened by inspiration; suggests pleural inflammation — parapneumonic, PE, pleuritis)
- Dry, nonproductive cough (diaphragmatic irritation)
- Chest heaviness or pressure
- Orthopnea (when bilateral, as in CHF)
- Symptoms of underlying disease (fever/chills in empyema, weight loss in malignancy, ankle edema in CHF)
Physical examination:
- Decreased breath sounds (dullness to percussion, reduced tactile fremitus, diminished air entry) at the affected base(s)
- Stony dullness to percussion (effusion) contrasted with tympany above (compressed lung)
- Egophony ("E" to "A" change) at the upper border of the effusion (compressed atelectatic lung)
- Tracheal deviation away from large effusion; toward effusion if underlying collapse
- Signs of underlying etiology: JVD/peripheral edema (CHF), spider nevi/ascites (cirrhosis), lymphadenopathy (malignancy, lymphoma, TB), joint deformities (RA), fever (infection)
6. Diagnosis — Light's Criteria
Imaging
- Chest X-ray: Blunting of costophrenic angle (requires >200–300 mL on PA view; 50 mL on lateral view); meniscus sign; subpulmonic effusion (mimics elevated hemidiaphragm); bilateral effusions suggest systemic cause (CHF, hypoalbuminemia)
- Ultrasound: Most sensitive bedside tool; detects as little as 20 mL; identifies complex, loculated, and septated effusions; guides thoracentesis (recommended to reduce pneumothorax risk)
- CT chest: Characterizes pleural versus parenchymal disease; identifies loculations, pleural thickening (mesothelioma), empyema (lenticular shape, pleural enhancement), mediastinal lymphadenopathy, underlying lung lesions
Thoracentesis
Diagnostic and/or therapeutic aspiration of pleural fluid. Indicated for all undiagnosed effusions and symptomatic relief. Contraindicated if very small (<10 mm layering on lateral decubitus X-ray) or uncontrolled coagulopathy (relative). Ultrasound-guided approach recommended.
Fluid analysis:
- Appearance: clear (transudate/simple exudate), turbid/purulent (empyema), bloody (malignancy, hemothorax, PE), milky (chylothorax)
- Cell count and differential: neutrophilic pleocytosis (parapneumonic, early TB); lymphocytic predominance (>50%: TB, malignancy, chylothorax, lymphoma, rheumatoid); eosinophilia (>10%: drug reaction, parasitic, malignancy, asbestos)
- Protein, LDH (for Light's criteria)
- Glucose: very low (<60 mg/dL or ratio <0.5): empyema, RA-pleuritis, TB, malignancy, esophageal rupture
- pH: <7.20 indicates need for drainage (complicated parapneumonic/empyema)
- Cytology: positive in 40–90% of malignant effusions (lower yield in mesothelioma)
- Microbiology: Gram stain, culture (aerobic and anaerobic), AFB smear and culture
- Amylase: elevated in pancreatic disease, esophageal rupture, some malignancies
- Triglycerides: >110 mg/dL confirms chylothorax; chylomicrons on lipoprotein analysis
- ADA (adenosine deaminase): >35–40 U/L highly suggestive of tuberculous pleuritis in endemic areas
Light's Criteria for Differentiating Exudate from Transudate
An effusion is classified as an exudate if any one of the following criteria is met:
- Pleural fluid protein / serum protein ratio >0.5
- Pleural fluid LDH / serum LDH ratio >0.6
- Pleural fluid LDH >2/3 the upper limit of normal serum LDH
Light's criteria have a sensitivity of ~98% and specificity of ~83% for exudates. The major limitation is misclassifying diuretic-treated CHF effusions as exudates (in ~25% of cases). In this context, the serum-to-pleural fluid albumin gradient >1.2 g/dL (or protein gradient >3.1 g/dL) correctly identifies transudates treated with diuretics, serving as a useful adjunct.
Additional criteria under investigation: N-terminal pro-BNP in pleural fluid (>1500 pg/mL strongly suggests CHF etiology); pleural cholesterol >45 mg/dL suggests exudate.
Pleural Biopsy
- Image-guided (CT or ultrasound) percutaneous pleural biopsy: preferred for suspected pleural malignancy or TB with negative cytology
- Thoracoscopy (medical or VATS): highest diagnostic yield for malignant mesothelioma and TB; allows direct visual inspection, targeted biopsy, and talc pleurodesis in a single procedure
7. Treatment
Treatment is directed at the underlying cause and at symptom relief.
Transudates
- CHF: Optimize heart failure management (diuretics, ACE inhibitors/ARBs, beta-blockers, sodium restriction); effusions typically resolve with improved cardiac compensation
- Hepatic hydrothorax: Sodium restriction and diuretics (spironolactone + furosemide); TIPS (transjugular intrahepatic portosystemic shunt) for refractory cases; liver transplantation as definitive treatment; chemical pleurodesis has limited success due to rapid reaccumulation
- Nephrotic syndrome: Treat underlying cause; albumin replacement; diuretics
Parapneumonic Effusions and Empyema
Management follows the British Thoracic Society (BTS) RAPID scoring system and pleural fluid characteristics:
- Simple parapneumonic (free-flowing, pH >7.20, glucose normal, sterile): antibiotics alone; repeat imaging in 48–72 hours
- Complicated parapneumonic (pH <7.20, glucose <60 mg/dL, positive culture, or loculated): intercostal chest tube drainage
- Empyema: Chest tube drainage + antibiotics; intrapleural fibrinolytic therapy (alteplase + DNase) for septated/loculated empyema (MRC Second Multi-centre Intrapleural Sepsis Trial — MIST2); VATS decortication for organized empyema resistant to catheter drainage
Malignant Pleural Effusions
- Therapeutic thoracentesis: Immediate symptomatic relief; effusion typically reaccumulates within 30 days
- Chemical pleurodesis: Obliteration of the pleural space with sclerosant to prevent reaccumulation; talc most effective agent (70–90% success); requires expandable underlying lung; administered via chest tube or thoracoscopy (insufflated talc preferred)
- Indwelling pleural catheter (IPC): Tunneled, ambulatory catheter (PleurX) allowing repeated outpatient drainage; preferred over pleurodesis when lung is trapped, patient has poor performance status, or rapid outpatient palliation is desired; spontaneous pleurodesis occurs in ~40% of patients; equally effective to talc pleurodesis in the TIME2 and AMPLE trials
- Systemic therapy: Chemotherapy, targeted therapy, or immunotherapy for chemo-sensitive malignancies (lymphoma, small cell lung cancer, breast cancer) may cause effusion resolution
Tuberculous Pleuritis
- Standard anti-tuberculosis chemotherapy (RIPE regimen: rifampin, isoniazid, pyrazinamide, ethambutol) for 6 months
- Therapeutic thoracentesis for symptomatic relief; chest tube rarely needed
- Corticosteroids: adjunctive prednisone may reduce fever and accelerate resolution; evidence for long-term benefit on pleural fibrosis is mixed
Chylothorax
- Low-fat diet with medium-chain triglycerides (bypass lymphatics); total parenteral nutrition for complete lymph rest
- Somatostatin/octreotide to reduce lymph flow
- Surgical thoracic duct ligation or embolization for persistent high-output chylothorax
- Treat underlying lymphoma with systemic therapy
8. Complications
- Empyema thoracis: Most serious complication of parapneumonic effusion; 15–20% mortality; requires aggressive drainage and antibiotics; organizing empyema may require surgery (VATS decortication)
- Fibrothorax: Organization of chronic exudative effusion or empyema into a thick pleural peel, restricting lung expansion; requires surgical decortication
- Trapped lung: Visceral pleural fibrosis prevents lung re-expansion after fluid removal; creates persistent pleural space; managed with IPC for drainage without pleurodesis
- Pneumothorax: Complication of thoracentesis (~1–6%); ultrasound guidance reduces risk; post-procedure chest X-ray when clinically indicated
- Re-expansion pulmonary edema: Rare; occurs after rapid drainage of large (>1.5 L) effusions; unilateral edema, cough, hypoxia; limit single-session drainage to 1–1.5 L (or stop when patient develops symptoms)
- Hemothorax: Injury to intercostal vessels during thoracentesis; treatment: chest tube drainage, VATS if persistent
- Respiratory failure: Massive effusion compressing viable lung; requires urgent drainage
- Mesothelioma seeding: Procedure-tract metastases following thoracentesis/thoracoscopy in mesothelioma; prophylactic radiotherapy to procedure sites reduces risk
9. Prognosis
Prognosis depends entirely on the underlying etiology:
- Transudates: Prognosis determined by the underlying condition (CHF, cirrhosis); pleural effusion itself is a marker of disease severity and portends worse outcomes in CHF and cirrhosis
- Parapneumonic/Empyema: With appropriate drainage and antibiotics, most patients recover; mortality 5–20% in empyema, higher in elderly and immunocompromised; delay in drainage worsens prognosis
- Malignant pleural effusion: Median survival after diagnosis ~3–12 months; varies by tumor type (better: breast cancer, lymphoma; worse: mesothelioma, lung cancer); effusion development signals advanced disease in most malignancies
- Tuberculous pleuritis: Excellent with treatment; risk of developing active pulmonary TB within 5 years if untreated (~65%)
- Chylothorax: Outcome related to underlying cause; lymphoma-associated has good prognosis with systemic therapy; traumatic chylothorax usually responds to conservative management or surgical repair
The RAPID score (Renal function, Age, Purulence, Infection source, Dietary factors) predicts 3-month mortality in pleural infection and can guide drainage intensity decisions.
10. Prevention
- Optimal management of CHF (medication adherence, sodium restriction, daily weights) reduces recurrent transudative effusions
- Early and adequate treatment of pneumonia with appropriate antibiotics reduces parapneumonic effusion progression to empyema
- Tuberculosis prevention and treatment (LTBI treatment) in endemic populations
- Monitoring for pleural toxicity with causative medications (amiodarone, methotrexate, dasatinib)
- Prophylactic radiotherapy to drainage sites in mesothelioma to prevent procedure-tract seeding
- Ultrasound guidance for all thoracenteses to minimize pneumothorax and hemothorax complications
11. Recent Research and Advances
Indwelling Pleural Catheters (IPCs) — Expanding Indications: The AMPLE-2 trial demonstrated non-inferiority of IPC to talc slurry pleurodesis for malignant effusions with non-expanded lung, challenging the traditional approach. IPC combined with talc (the IPC-Plus trial) can improve spontaneous pleurodesis rates. Emerging evidence supports IPCs in non-malignant recurrent effusions (hepatic hydrothorax, heart failure).
Intrapleural Enzyme Therapy: The MIST2 trial established dual intrapleural therapy with alteplase + DNase (dornase alfa) as superior to either agent alone or placebo for septated parapneumonic effusions, reducing surgical referral by 30%. This regimen is now standard practice for complex parapneumonic effusions and empyema.
Pleural Fluid Biomarkers: Mesothelin (soluble mesothelin-related protein, SMRP) in pleural fluid improves diagnostic accuracy for mesothelioma. VEGF levels correlate with malignant effusion recurrence. Telomerase activity in pleural fluid shows promise for cancer diagnosis. Next-generation sequencing of cell-free DNA in pleural fluid may improve malignancy detection.
Thoracoscopy vs. Thoracentesis for Malignant Effusions: The SIMPLE trial and other data suggest that medical thoracoscopy at first diagnosis of malignant effusion (combining diagnostic biopsy with talc poudrage) may be more cost-effective than sequential thoracentesis then pleurodesis.
AI and Ultrasound: Machine learning algorithms applied to pleural ultrasound images can identify complex effusions, guide sampling locations, and predict drainage outcomes with accuracy comparable to expert sonographers.
Pleural Fluid Microbiome: Next-generation sequencing has identified diverse microbial communities in empyema fluid beyond conventional culture-positive organisms, potentially explaining the high rate of culture-negative empyema (>30%) and informing antibiotic selection.
12. References
- Light RW. Pleural effusions. N Engl J Med. 2002;346(25):1971–1977.
- Light RW, et al. Pleural effusions: the diagnostic separation of transudates and exudates. Ann Intern Med. 1972;77(4):507–513.
- Davies HE, et al. (TIME2). Effect of an indwelling pleural catheter vs chest tube and talc pleurodesis for relieving dyspnea in patients with malignant pleural effusion. JAMA. 2012;307(22):2383–2389.
- Rahman NM, et al. (MIST2). Intrapleural use of tissue plasminogen activator and DNase in pleural infection. N Engl J Med. 2011;365(6):518–526.
- Clive AO, et al. (AMPLE). Randomised clinical trial of indwelling pleural catheter versus talc pleurodesis in malignant pleural effusion (AMPLE). BMJ. 2014;348:g7018.
- Hooper C, et al. BTS Pleural Guideline Group. Investigation of a unilateral pleural effusion in adults: British Thoracic Society Pleural Disease Guideline 2010. Thorax. 2010;65(Suppl 2):ii4–17.
- Porcel JM. Pleural fluid tests to identify complicated parapneumonic effusions. Curr Opin Pulm Med. 2010;16(4):357–361.
- Roberts ME, et al. BTS guidelines for the management of pleural infection. Thorax. 2010;65(Suppl 2):ii41–53.
- Heffner JE, Brown LK, Barbieri CA. Diagnostic value of tests that discriminate between exudative and transudative pleural effusions. Chest. 1997;111(4):970–980.
- Bibby AC, et al. ERS/EACTS statement on the management of malignant pleural effusions. Eur Respir J. 2018;52(1):1800349.
- Maskell NA, et al. (MIST1). UK Controlled Trial of Intrapleural Streptokinase for Pleural Infection. N Engl J Med. 2005;352(9):865–874.
- Porcel JM, Light RW. Diagnostic approach to pleural effusion in adults. Am Fam Physician. 2006;73(7):1211–1220. PMID:16623208
- Feller-Kopman D, Light R. Pleural Disease. N Engl J Med. 2018;378(8):740–751.
- Ferreiro L, et al. Diagnosis of pleural effusion caused by heart failure. J Thorac Dis. 2019;11(Suppl 9):S1364–S1372.
- Skok K, et al. Pleural Effusion—A Concise Review. Ann Thorac Cardiovasc Surg. 2019;25(6):326–331.
- Thomas R, et al. Pleurodesis for malignant pleural effusions: current controversies and variations in practices. Curr Opin Pulm Med. 2015;21(4):341–346.
Research Papers
The following PubMed topic searches surface the current peer-reviewed literature on Pleural Effusion. Each link opens a live PubMed query; results update as new papers are indexed.
- PubMed search: pleural effusion
- PubMed search: pleural effusion Light criteria
- PubMed search: thoracentesis pleural fluid analysis
- PubMed search: malignant pleural effusion
- PubMed search: parapneumonic effusion empyema
- PubMed search: pleural effusion heart failure
- PubMed search: chylothorax
- PubMed search: hemothorax
- PubMed search: transudative exudative pleural effusion
- PubMed search: indwelling pleural catheter
- PubMed search: pleurodesis
- PubMed search: tuberculous pleural effusion
Connections
- Pneumonia
- Heart Failure
- Pulmonary Embolism
- Lymphoma
- Kidney Disease
- Metastatic Cancers
- Cancer
- Edema
- Cirrhosis
- Hypertension
- Tuberculosis
- Nephrotic Syndrome
- Chest Pain
- Sepsis
- Rheumatoid Arthritis
- Lupus
- Pancreatitis
- Shortness Of Breath