Tryptophan: The Essential Amino Acid for Serotonin, Sleep, and Mood
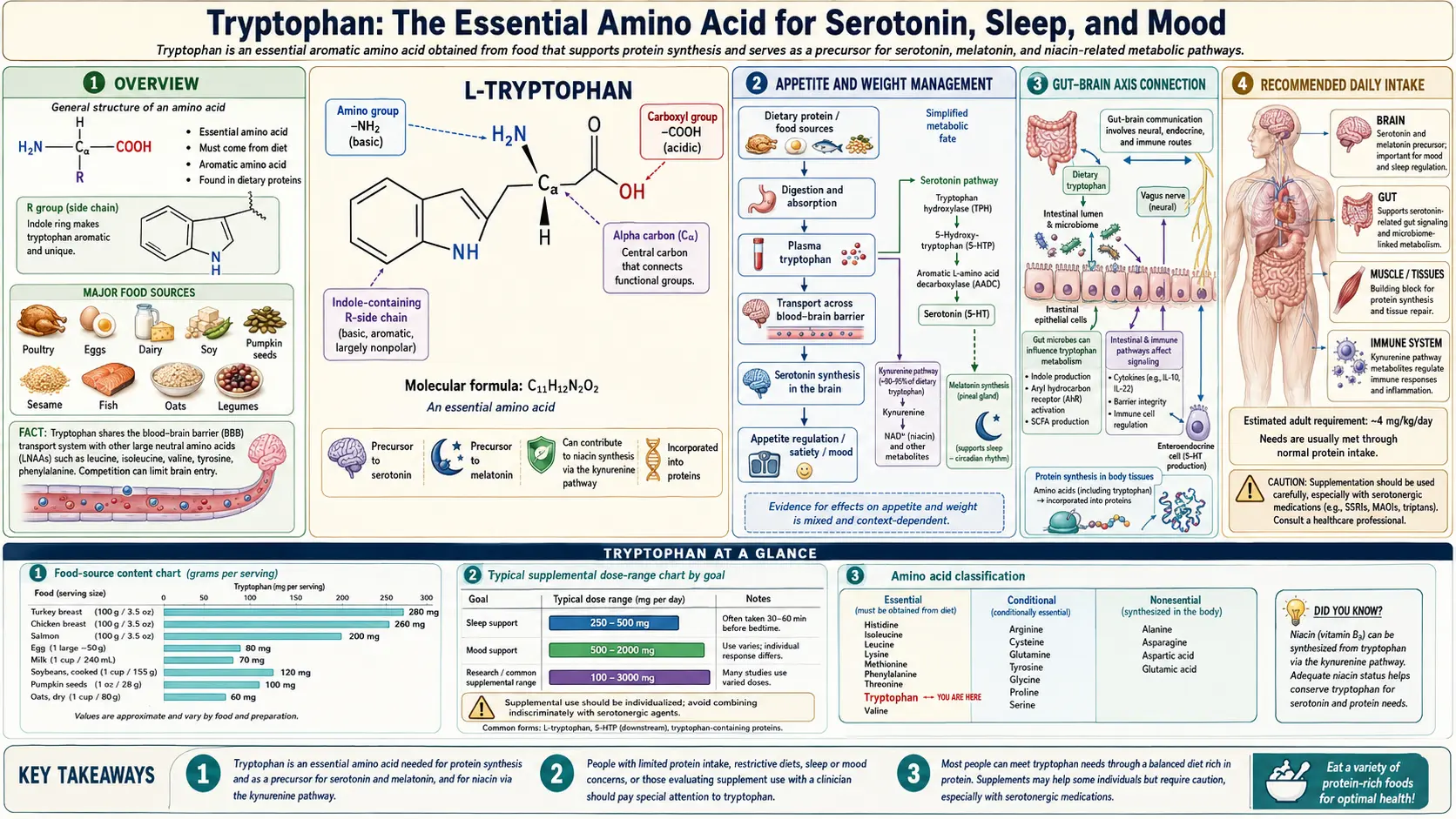
Table of Contents
- Overview
- Serotonin Production and Mood Regulation
- Melatonin Synthesis and Sleep Quality
- Depression and Anxiety Support
- Appetite and Weight Management
- Pain Tolerance and Sensitivity
- Niacin (Vitamin B3) Production
- Cognitive Function and Memory
- Immune System Modulation
- Gut-Brain Axis Connection
- Deficiency Signs
- Food Sources
- Supplementation Guidelines (L-Tryptophan vs 5-HTP)
- Recommended Daily Intake
- Research Papers
- Connections
- Featured Videos
Overview
Tryptophan is one of the nine essential amino acids that the human body cannot synthesize on its own, meaning it must be obtained through dietary sources or supplementation. As a building block of protein, tryptophan plays a critical structural role in tissue repair and growth. However, its significance extends far beyond simple protein synthesis. Tryptophan serves as the sole precursor to serotonin, the neurotransmitter most closely associated with emotional well-being, and to melatonin, the hormone that governs our circadian rhythm and sleep-wake cycles.
From a naturopathic perspective, tryptophan occupies a central position in the web of metabolic pathways that connect nutrition to mental health, sleep quality, immune resilience, and digestive function. It is metabolized through two primary pathways: the serotonin-melatonin pathway and the kynurenine pathway. Approximately 95 percent of dietary tryptophan is directed through the kynurenine pathway, where it contributes to niacin (vitamin B3) production and immune regulation, while the remaining portion fuels serotonin and melatonin synthesis. Understanding this amino acid and supporting its metabolism through whole-food nutrition, cofactor optimization, and targeted supplementation when appropriate can profoundly influence a patient's quality of life.
Tryptophan is unique among the amino acids in that it is typically the least abundant in most dietary proteins, making it a rate-limiting factor in protein synthesis and neurotransmitter production. This relative scarcity underscores the importance of intentional dietary planning to ensure adequate intake, particularly for individuals experiencing mood disorders, sleep disturbances, or chronic inflammation.
Serotonin Production and Mood Regulation
The conversion of tryptophan to serotonin is a two-step enzymatic process. First, the enzyme tryptophan hydroxylase converts tryptophan into 5-hydroxytryptophan (5-HTP). Then, aromatic L-amino acid decarboxylase converts 5-HTP into serotonin (5-hydroxytryptamine, or 5-HT). This process requires several essential cofactors, including iron, vitamin B6 (pyridoxal-5-phosphate), and tetrahydrobiopterin. Without adequate levels of these cofactors, even sufficient tryptophan intake may fail to produce optimal serotonin levels.
Serotonin is widely recognized as the body's primary mood-stabilizing neurotransmitter. It fosters feelings of calm, contentment, emotional resilience, and social connectedness. Low serotonin activity has been associated with irritability, impulsivity, aggression, and a pervasive sense of dissatisfaction. In clinical practice, patients who present with persistent low mood, emotional reactivity, or difficulty coping with everyday stressors often benefit from strategies that support the tryptophan-to-serotonin pathway.
It is important to note that tryptophan must cross the blood-brain barrier to be converted into serotonin within the central nervous system. Tryptophan competes with other large neutral amino acids, including leucine, isoleucine, valine, tyrosine, and phenylalanine, for transport across this barrier. Consuming carbohydrate-rich meals triggers insulin release, which drives competing amino acids into muscle tissue, thereby improving tryptophan's relative access to the brain. This mechanism explains why many people instinctively crave carbohydrate-heavy comfort foods when feeling emotionally low.
Melatonin Synthesis and Sleep Quality
Once serotonin has been produced in the pineal gland, it can be further converted into melatonin through acetylation and methylation reactions. The enzyme arylalkylamine N-acetyltransferase (AANAT) converts serotonin to N-acetylserotonin, and then hydroxyindole-O-methyltransferase (HIOMT) produces melatonin. This conversion is stimulated by darkness and suppressed by light exposure, linking tryptophan metabolism directly to circadian biology.
Melatonin is the body's primary sleep-signaling hormone. It does not directly induce unconsciousness but rather communicates to the brain and body that nighttime has arrived, promoting the physiological shift toward rest. Adequate melatonin production supports healthy sleep onset latency, meaning the time it takes to fall asleep, as well as sleep duration and subjective sleep quality. Melatonin is also a potent antioxidant, scavenging free radicals and supporting mitochondrial health during the restorative phases of sleep.
Patients with insomnia or disrupted sleep architecture may have insufficient tryptophan intake or impaired conversion along the serotonin-melatonin pathway. Before reaching for exogenous melatonin supplements, a naturopathic approach first investigates whether the body has the raw materials and cofactors needed to produce melatonin endogenously. Ensuring adequate tryptophan, vitamin B6, magnesium, and folate while minimizing blue light exposure in the evening can often restore healthy melatonin rhythms naturally.
Depression and Anxiety Support
The relationship between tryptophan and mood disorders has been extensively studied. Acute tryptophan depletion experiments, in which subjects consume an amino acid mixture lacking tryptophan, consistently demonstrate rapid declines in mood, increased anxiety, and heightened stress reactivity, particularly in individuals with a personal or family history of depression. These findings strongly support the role of tryptophan availability in maintaining emotional stability.
In naturopathic medicine, supporting tryptophan metabolism is considered a foundational strategy for patients with mild to moderate depression and generalized anxiety. Rather than viewing depression solely as a serotonin deficiency, we recognize it as a complex condition influenced by inflammation, gut health, nutrient status, hormonal balance, and psychosocial factors. Tryptophan optimization addresses one important thread in this multifactorial web.
Chronic stress and systemic inflammation can divert tryptophan away from serotonin production and toward the kynurenine pathway, where it may generate neurotoxic metabolites such as quinolinic acid. This inflammatory shunting of tryptophan is increasingly recognized as a contributor to depression in the context of chronic illness, autoimmune conditions, and prolonged psychological stress. Addressing underlying inflammation through anti-inflammatory nutrition, omega-3 fatty acids, curcumin, and stress management techniques can help redirect tryptophan metabolism toward more favorable pathways.
Appetite and Weight Management
Serotonin plays a significant role in regulating appetite and satiety. Within the hypothalamus, serotonin signaling promotes feelings of fullness and reduces cravings, particularly for carbohydrate-rich and sugar-laden foods. Individuals with low serotonin activity often experience persistent carbohydrate cravings, emotional eating, and difficulty maintaining a sense of satisfaction after meals.
Research has demonstrated that tryptophan supplementation can reduce caloric intake, diminish snacking behavior, and improve the overall quality of food choices. By supporting serotonin production, adequate tryptophan helps break the cycle of cravings, overeating, and guilt that characterizes disordered eating patterns in many patients. This mechanism is particularly relevant for individuals who notice that their appetite and food choices worsen during periods of stress, seasonal darkness, or emotional difficulty.
From a naturopathic standpoint, addressing tryptophan status is an essential component of any comprehensive weight management program. Rather than relying on willpower alone, we support the neurochemistry that governs appetite regulation, giving patients a genuine physiological advantage in achieving and maintaining a healthy body composition.
Pain Tolerance and Sensitivity
Serotonin is a key modulator of pain perception within both the central and peripheral nervous systems. It participates in descending pain inhibition pathways that originate in the brainstem and project down to the spinal cord, effectively dampening incoming pain signals before they reach conscious awareness. Low serotonin states are associated with heightened pain sensitivity, reduced pain tolerance, and conditions such as fibromyalgia, chronic tension headaches, and migraines.
Tryptophan depletion studies have confirmed that reducing serotonin availability increases sensitivity to both thermal and mechanical pain stimuli. Conversely, supporting tryptophan intake and serotonin synthesis may raise the pain threshold and improve quality of life for patients with chronic pain conditions. In clinical practice, ensuring optimal tryptophan status is particularly valuable for patients who report widespread pain, heightened sensitivity to touch or pressure, or pain that worsens with emotional stress.
Niacin (Vitamin B3) Production
The kynurenine pathway, which processes the majority of dietary tryptophan, ultimately leads to the production of nicotinamide adenine dinucleotide (NAD+) via niacin. NAD+ is a coenzyme essential for over 400 enzymatic reactions in the body, including energy metabolism, DNA repair, cellular signaling, and the activity of sirtuins, a family of longevity-associated proteins.
Approximately 60 milligrams of tryptophan can yield about 1 milligram of niacin, making this a relatively inefficient conversion. Nonetheless, this pathway represents an important endogenous source of niacin, particularly when dietary niacin intake is marginal. Severe tryptophan deficiency, combined with low niacin intake, can lead to pellagra, a condition characterized by dermatitis, diarrhea, dementia, and, if untreated, death.
The kynurenine pathway requires adequate levels of vitamin B6, vitamin B2 (riboflavin), and iron to function optimally. When these cofactors are deficient, intermediate metabolites such as 3-hydroxykynurenine and quinolinic acid may accumulate. These compounds are neurotoxic and pro-inflammatory, contributing to neurodegeneration and mood disturbances. Supporting cofactor status is therefore essential to ensuring healthy tryptophan metabolism through both the serotonin and kynurenine pathways.
Cognitive Function and Memory
Serotonin influences multiple domains of cognitive function, including learning, memory consolidation, attention, and executive function. Tryptophan availability directly affects serotonin synthesis in brain regions critical for cognition, such as the hippocampus and prefrontal cortex. Studies have shown that acute tryptophan depletion impairs long-term memory consolidation and reduces cognitive flexibility, the ability to adapt one's thinking and behavior in response to changing circumstances.
Beyond serotonin's direct cognitive effects, the kynurenine pathway metabolite kynurenic acid acts as an antagonist at glutamate NMDA receptors, which play a central role in synaptic plasticity and learning. The balance between neuroprotective kynurenic acid and neurotoxic quinolinic acid within the kynurenine pathway has significant implications for cognitive health, particularly in aging populations and individuals with neurodegenerative conditions.
For patients experiencing brain fog, difficulty concentrating, or age-related cognitive decline, optimizing tryptophan metabolism is a worthwhile strategy. This includes ensuring adequate dietary tryptophan, supporting cofactor nutrients, managing inflammation that may divert tryptophan toward neurotoxic kynurenine metabolites, and maintaining gut health to support peripheral serotonin production and the gut-brain axis.
Immune System Modulation
Tryptophan metabolism plays a surprisingly important role in immune regulation. The enzyme indoleamine 2,3-dioxygenase (IDO), which catalyzes the first step of the kynurenine pathway, is strongly upregulated by pro-inflammatory cytokines, particularly interferon-gamma. This activation serves as an immune defense mechanism: by depleting local tryptophan levels, IDO starves invading pathogens and inhibits the proliferation of T cells at sites of infection or inflammation.
While this tryptophan-depleting mechanism is protective in acute infection, chronic IDO activation in the setting of persistent inflammation, autoimmune disease, or cancer can lead to sustained tryptophan depletion and serotonin deficiency. This provides a mechanistic explanation for the high prevalence of depression and fatigue in patients with chronic inflammatory conditions such as rheumatoid arthritis, inflammatory bowel disease, and chronic infections.
Kynurenine pathway metabolites also influence the balance between regulatory T cells and effector T cells, shaping the overall tone of the immune response. Supporting healthy tryptophan metabolism through anti-inflammatory nutrition and targeted supplementation may help maintain immune balance and prevent the collateral mood and cognitive effects of chronic immune activation.
Gut-Brain Axis Connection
Approximately 90 to 95 percent of the body's serotonin is produced in the gastrointestinal tract by enterochromaffin cells. While this peripheral serotonin does not cross the blood-brain barrier, it plays critical roles in regulating gut motility, secretion, visceral sensitivity, and intestinal inflammation. The gut microbiome directly influences tryptophan metabolism, with certain bacterial species capable of metabolizing tryptophan into bioactive indole compounds that support intestinal barrier integrity and immune homeostasis.
Dysbiosis, the disruption of healthy microbial balance in the gut, can alter tryptophan availability and metabolism in ways that affect both gastrointestinal and mental health. Some pathogenic bacteria and inflammatory states activate IDO in the gut wall, diverting tryptophan toward the kynurenine pathway and away from serotonin synthesis. This may contribute to the well-established association between irritable bowel syndrome, inflammatory bowel disease, and mood disorders.
From a naturopathic perspective, supporting gut health is inseparable from supporting tryptophan metabolism. Probiotics, prebiotics, fermented foods, and an anti-inflammatory diet rich in fiber and polyphenols can promote a microbial environment that favors healthy tryptophan utilization. Healing intestinal permeability and resolving chronic gut inflammation may restore more balanced tryptophan partitioning between the serotonin and kynurenine pathways.
Deficiency Signs
Because tryptophan is the least abundant essential amino acid in most foods and the precursor to several critically important molecules, even moderate insufficiency can produce noticeable symptoms. Common signs of low tryptophan status include the following:
- Mood disturbances: Persistent low mood, irritability, emotional reactivity, increased anxiety, and reduced stress tolerance.
- Sleep difficulties: Trouble falling asleep, frequent nighttime waking, non-restorative sleep, and disrupted circadian rhythm.
- Carbohydrate and sugar cravings: Intense desire for starchy or sweet foods, particularly in the afternoon and evening.
- Cognitive impairment: Difficulty concentrating, poor memory recall, brain fog, and reduced mental clarity.
- Increased pain sensitivity: Lowered pain threshold, widespread aches, and heightened sensitivity to stimuli.
- Digestive disturbances: Altered bowel habits, including constipation or motility changes, and increased visceral sensitivity.
- Weakened immune resilience: Frequent infections, slow recovery, and signs of chronic low-grade inflammation.
Populations at elevated risk for tryptophan insufficiency include strict vegans consuming inadequate protein variety, individuals with malabsorption conditions such as celiac disease or inflammatory bowel disease, those under chronic psychological stress, the elderly with reduced appetite and protein intake, and individuals with eating disorders. Chronic inflammation of any origin can also functionally deplete tryptophan by shunting it through the kynurenine pathway.
Food Sources
The richest dietary sources of tryptophan are protein-dense whole foods. As a naturopathic physician, I encourage patients to obtain tryptophan from a varied diet of high-quality, minimally processed foods whenever possible. The following are among the most concentrated sources:
- Turkey and chicken: Among the highest animal sources, providing approximately 250 to 300 milligrams per 100-gram serving.
- Wild-caught salmon and other oily fish: Excellent sources that also provide anti-inflammatory omega-3 fatty acids.
- Eggs: Particularly the egg white, though whole eggs provide superior overall nutrition including B vitamins.
- Dairy products: Cheese, yogurt, and milk contain meaningful amounts of tryptophan along with calcium and other cofactors.
- Pumpkin seeds and sesame seeds: Outstanding plant-based sources, with pumpkin seeds providing approximately 575 milligrams per 100 grams.
- Soybeans and tofu: Among the best legume-based sources, offering a complete amino acid profile.
- Nuts: Cashews, almonds, and walnuts provide tryptophan along with magnesium and healthy fats.
- Oats and whole grains: Moderate sources that also supply the complex carbohydrates that facilitate tryptophan transport to the brain.
- Spirulina: An exceptionally dense source of tryptophan per gram of protein, suitable for those seeking plant-based supplementation.
- Bananas and dark chocolate: Modest sources that many patients find enjoyable to include in their daily diet.
To maximize brain uptake of tryptophan, consider pairing tryptophan-rich protein foods with complex carbohydrate sources. The insulin response to carbohydrates clears competing amino acids from the bloodstream, giving tryptophan preferential access to brain transporters. A meal of turkey with sweet potato, or oatmeal with pumpkin seeds, exemplifies this strategic pairing.
Supplementation Guidelines (L-Tryptophan vs 5-HTP)
When dietary optimization is insufficient, supplementation may be appropriate. Two forms are commonly available: L-tryptophan and 5-hydroxytryptophan (5-HTP). Each has distinct characteristics and clinical applications.
L-Tryptophan
L-tryptophan is the natural, unmodified form of the amino acid. When taken as a supplement, it enters the full range of metabolic pathways, including serotonin synthesis, melatonin production, kynurenine metabolism, and niacin production. This broader metabolic distribution makes L-tryptophan a gentler and more physiologically balanced option. Typical supplemental doses range from 500 to 2,000 milligrams daily, often taken in the evening or divided throughout the day. L-tryptophan is generally well tolerated and is considered particularly suitable for long-term use.
5-HTP (5-Hydroxytryptophan)
5-HTP is the intermediate metabolite between tryptophan and serotonin, bypassing the rate-limiting enzyme tryptophan hydroxylase. Because it is one enzymatic step closer to serotonin, 5-HTP is a more direct serotonin precursor and tends to have a more pronounced and rapid effect on mood and sleep. Typical doses range from 50 to 300 milligrams daily. 5-HTP is derived from the seeds of the African plant Griffonia simplicifolia.
However, 5-HTP exclusively feeds the serotonin pathway and does not contribute to kynurenine metabolism, niacin production, or protein synthesis. Long-term use of 5-HTP without concurrent dopamine precursor support (such as L-tyrosine) may theoretically create neurotransmitter imbalances, as serotonin and dopamine share metabolic enzymes and transport systems. For this reason, many naturopathic practitioners prefer L-tryptophan for extended use and reserve 5-HTP for short-term or acute applications.
Important Precautions
- Serotonin syndrome risk: Neither L-tryptophan nor 5-HTP should be combined with SSRI antidepressants, SNRI antidepressants, MAO inhibitors, or other serotonergic medications without medical supervision, due to the risk of serotonin syndrome, a potentially life-threatening condition.
- Cofactor support: Vitamin B6, magnesium, iron, and folate should be maintained at adequate levels to support enzymatic conversion.
- Timing: For sleep support, take supplements 30 to 60 minutes before bedtime. For mood support, divided daytime dosing may be more appropriate.
- Gastrointestinal effects: 5-HTP may cause nausea in some individuals, particularly at higher doses. Starting with a low dose and taking it with food can minimize this effect.
- Pregnancy and nursing: Supplementation should be undertaken only under professional guidance during pregnancy and lactation.
Recommended Daily Intake
The World Health Organization recommends a minimum tryptophan intake of 4 milligrams per kilogram of body weight per day for adults. For a 70-kilogram (154-pound) individual, this translates to approximately 280 milligrams per day. However, this represents a minimum to prevent deficiency, not an optimal therapeutic dose.
Many integrative and naturopathic practitioners suggest that optimal intake may be significantly higher, particularly for individuals dealing with mood disorders, sleep disturbances, chronic pain, or inflammatory conditions. A well-balanced diet containing adequate protein from varied sources typically provides between 250 and 1,000 milligrams of tryptophan per day, depending on total caloric and protein intake.
The following general guidelines apply to dietary and supplemental intake:
- General wellness: 250 to 500 milligrams daily from dietary sources is typically sufficient for healthy individuals.
- Mood and sleep support: 500 to 1,500 milligrams of supplemental L-tryptophan, or 100 to 300 milligrams of 5-HTP, may be beneficial when dietary intake is inadequate.
- Upper limit: Supplemental doses up to 2,000 milligrams of L-tryptophan daily have been used in clinical settings, though individual tolerance varies.
As with all nutritional interventions, the ideal approach begins with optimizing dietary intake through whole-food sources, addressing cofactor deficiencies, resolving underlying gut and inflammatory issues, and reserving supplementation for situations where these foundational strategies prove insufficient. A qualified naturopathic physician or integrative practitioner can help determine the most appropriate strategy based on individual assessment and, when available, functional testing of amino acid and neurotransmitter metabolite levels.
Research Papers
The following curated PubMed searches surface the peer-reviewed literature underpinning the claims on this page. Each link opens a live PubMed query for Tryptophan filtered by topic, so the results stay current as new studies are indexed.
- PubMed search — Tryptophan: Metabolism and biochemistry (review)
- PubMed search — Tryptophan: Dietary intake and requirements
- PubMed search — Tryptophan: Supplementation randomized controlled trials
- PubMed search — Tryptophan: Plasma levels and clinical outcomes
- PubMed search — Tryptophan: Muscle protein synthesis and exercise
- PubMed search — Tryptophan: Deficiency: signs and consequences
- PubMed search — Tryptophan: Cardiovascular effects
- PubMed search — Tryptophan: Neurological and cognitive effects
- PubMed search — Tryptophan: Immune function
- PubMed search — Tryptophan: Oxidative stress and antioxidant activity
- PubMed search — Tryptophan: Gastrointestinal and gut health
- PubMed search — Tryptophan: Safety, toxicity, and upper limit
For a broader literature review, see the full PubMed record for Tryptophan and the NIH Office of Dietary Supplements Fact Sheets.
This content is provided for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider before beginning any supplementation regimen.
Connections
- Tryptophan Benefits Deep Dive
- Tyrosine
- Phenylalanine
- Isoleucine
- Leucine
- Valine
- Serine
- Depression
- Anxiety
- Gut-Brain Axis
- Vitamin B6
- Vitamin B3
- Magnesium
- Inflammatory Bowel Disease
- Brain Fog
- Insomnia
- Omega-3 Fatty Acids
- Sleep Hygiene
- Magnesium Glycinate