Methylene Blue for Cognitive Enhancement and ADHD: Evidence and Off-Label Use
Cognitive enhancement is the off-label use that has driven most of the recent interest in methylene blue. The premise: a molecule that improves mitochondrial function in the brain should improve attention, working memory, and the subjective experience of mental clarity, especially in people whose baseline mitochondrial function is impaired by aging, sleep deprivation, post-viral states, or undiagnosed metabolic issues. The evidence base is uneven — mechanistic studies are stronger than human trials, but a small set of well-designed studies suggests real, measurable effects.
Table of Contents
- The Rodriguez 2016 fMRI Trial
- Animal Memory Evidence
- Dose-Response for Cognition
- Brain Fog and Subjective Effects
- ADHD and Methylene Blue
- Post-Viral Cognitive Symptoms
- Aging and Mild Cognitive Impairment
- Realistic Expectations
- Research Papers and References
- Connections
The Rodriguez 2016 fMRI Trial
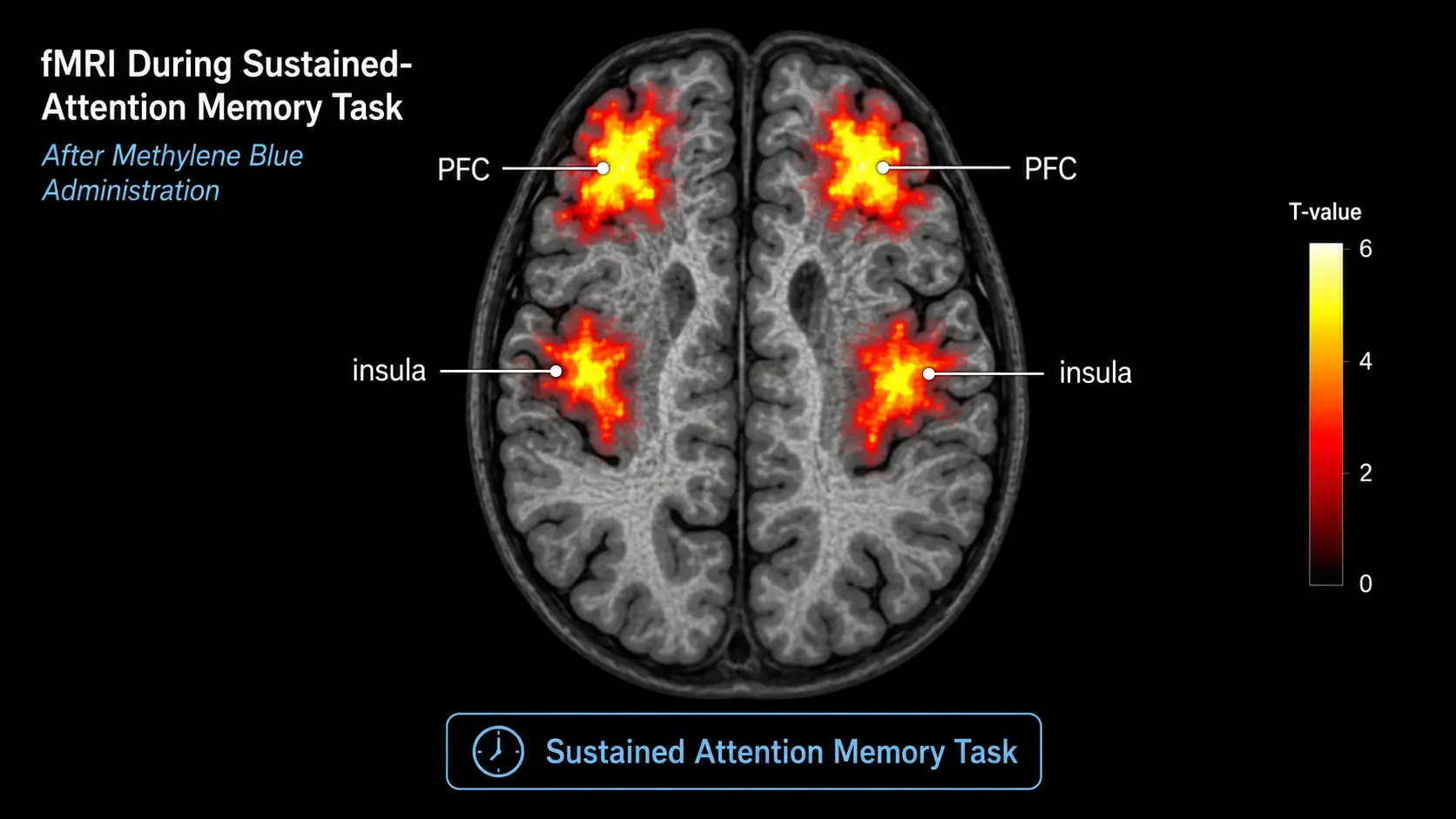
The most-cited human cognitive study is Rodriguez et al. 2016, published in Radiology. Twenty-six healthy adults received either 280 mg oral methylene blue or placebo in a double-blind crossover design. One hour after dosing, they performed sustained attention and memory-recall tasks during functional MRI. Methylene blue increased response accuracy on the sustained-attention task by approximately 7%, and increased fMRI signal in clusters covering the bilateral insular cortex and prefrontal regions during memory recall.
The strength of the trial: rigorous design, objective outcomes, mechanistic plausibility, modest but statistically significant effect. The limits: small sample (26), single dose (no chronic dosing data), healthy volunteers (no patient population), single dose level (no dose-response curve). The study supports the existence of a measurable cognitive effect at one dose in healthy young adults; it does not establish optimal dosing, durability, or population-level benefit.
Animal Memory Evidence
Animal studies have shown methylene blue effects on memory consistently across rats, mice, and rabbits. Key findings:
- Improved performance on the Morris water maze (spatial memory) at low doses (0.5–4 mg/kg)
- Enhanced cytochrome oxidase activity in hippocampus and cortex correlating with memory improvement
- Protection against memory impairment from various toxic insults (cyanide, sodium azide, hypoxia)
- Reversal of age-related memory decline in older rats
- Inverted-U dose response: doses above 10 mg/kg often worsen performance, consistent with the hormetic mechanism
The mechanistic alignment between cognitive testing and cytochrome oxidase activity is strong evidence that the bioenergetic mechanism described in the Mitochondrial Mechanism page drives the cognitive effects in vivo.
Dose-Response for Cognition
Animal studies have mapped the dose-response curve for memory effects more thoroughly than humans. The pattern is consistent: peak effect at 0.5–4 mg/kg, declining and then reversing as dose increases. Above ~10 mg/kg in animals, memory tasks worsen. The mechanism is the same hormetic curve that underlies the antioxidant-to-pro-oxidant flip described in the mechanism page.
For humans, the implication is that "more is not better." Most users find the subjective ceiling at 1–3 mg/kg. Above this, common reports include flat affect, mild dissociation, and the sense that the cognitive benefit has paradoxically faded. The right dose is often the one where you notice quiet, durable focus rather than a stimulant-like intensity.
Brain Fog and Subjective Effects
"Brain fog" is the lay term for the subjective syndrome of impaired focus, slow recall, and reduced mental clarity that accompanies many conditions: post-viral states, sleep deprivation, perimenopause, hypothyroidism, depression, fibromyalgia, autoimmune flare-ups, and chronic stress. There is no biomarker for it. But there is consistent overlap between brain fog and measurable mitochondrial dysfunction, especially in post-viral conditions.
For brain-fog presentations, methylene blue at nootropic doses is one of several mechanistically-targeted options:
- Treat the underlying driver if identifiable (thyroid disease, sleep apnea, depression, anemia, B12 deficiency)
- Mitochondrial support — CoQ10, alpha-lipoic acid, creatine, nicotinamide riboside, methylene blue
- Neuroinflammation reduction — omega-3s, curcumin, resolvins, low-dose naltrexone
- Stimulant-like options — coffee, modafinil if clinically indicated, prescription ADHD medications
For details on brain fog as a clinical syndrome, see the Brain Fog page.
ADHD and Methylene Blue
ADHD is increasingly understood as having a meaningful mitochondrial dysfunction component, with mitochondrial gene polymorphisms over-represented in ADHD populations and lower brain energy metabolism on PET in some studies. This has driven informal interest in methylene blue as an off-label ADHD intervention, but the formal evidence base is limited:
- No randomized controlled trials of methylene blue specifically for ADHD
- Anecdotal reports of improved focus and reduced symptom severity in adults with ADHD using nootropic doses
- Theoretical concerns about methylene blue interacting with stimulant medications via MAO-A inhibition (amphetamines, methylphenidate) — not formally contraindicated but warrants caution
- Patients on SSRIs/SNRIs for comorbid anxiety or depression cannot safely combine methylene blue at therapeutic doses
The realistic position: methylene blue is not a substitute for stimulant medications in ADHD; it may be a useful adjunct in patients with treatment-refractory cognitive symptoms or in those who cannot tolerate stimulants, under medical supervision. Self-experimentation in the absence of a formal ADHD diagnosis is not recommended.
Post-Viral Cognitive Symptoms
Post-viral cognitive impairment — following influenza, mononucleosis, COVID-19, and other systemic viral illnesses — shares features with ME/CFS and shows measurable mitochondrial dysfunction in muscle biopsies and brain imaging. Several clinicians have reported using methylene blue at standard nootropic doses (1–2 mg/kg/day) for post-viral brain fog, citing the mitochondrial mechanism.
The evidence remains anecdotal and observational; no randomized trials have evaluated methylene blue for post-COVID cognitive symptoms specifically. See the Long COVID page for a more detailed treatment.
Aging and Mild Cognitive Impairment
The case for methylene blue in aging cognition:
- Mitochondrial function declines measurably with age, paralleling cognitive decline
- Methylene blue reverses age-related memory deficits in rodents
- The tau-aggregation inhibition pathway is independently relevant in tauopathies
- Phase-3 LMTX trials in Alzheimer's missed primary endpoints but showed monotherapy subgroup signals
The case against:
- No controlled trial of methylene blue itself (vs the LMTX prodrug) has demonstrated cognitive benefit in aging humans
- Drug-interaction limitations (SSRIs, SNRIs are extremely common in older adults)
- G6PD screening becomes more important as comorbidities accumulate
For older patients without prohibiting comorbidities or interactions, low-dose nootropic methylene blue is a reasonable adjunct to cognitive-aging protocols (sleep optimization, exercise, dietary patterns, treatment of vascular risk factors, social engagement).
Realistic Expectations
For a healthy adult starting at 1–2 mg/kg/day, the realistic effect is:
- Mild improvement in sustained focus, particularly during long cognitive tasks
- Better verbal fluency and word recall during the 2–4 hours after a dose
- Subtle mood elevation (likely from MAO-A inhibition)
- Blue urine; possibly mild blue staining of the tongue with sublingual administration
What it is not:
- A stimulant — the effect is not like caffeine, modafinil, or amphetamines
- An immediate-onset memory enhancer — subjective effects build over days to weeks
- A substitute for sleep, exercise, or addressing underlying drivers of cognitive impairment
- Without trade-offs — the drug-interaction list is significant; the dose has to be right; the source has to be pharmaceutical grade
Research Papers and References
- Rodriguez 2016 fMRI trial — PubMed search
- MB and Morris water maze — PubMed search
- MB and cytochrome oxidase — PubMed search
- MB and attention — PubMed search
- ADHD and mitochondrial dysfunction — PubMed search
- LMTX phase 3 in Alzheimer's — PubMed search
- Mitochondrial dysfunction in aging cognition — PubMed search
Connections
- Methylene Blue Deep-Dive Articles:
- Methylene Blue Overview
- Mitochondrial Mechanism
- Dosing Guide
- Long COVID
- Drug Interactions
- Brain Fog
- Psychiatry
- Depression
- Dementia
- NAD+ and NMN
- Creatine
- Bacopa Monnieri
- Ginkgo Biloba
- Oxidative Stress