Methylene Blue Photodynamic Therapy and Cancer Research
Photodynamic therapy (PDT) is a treatment that combines a light-sensitive drug (a "photosensitizer") with targeted light exposure to generate cytotoxic reactive oxygen species at the treatment site. Methylene blue is one of the oldest and most-studied photosensitizers, with established clinical uses in dermatology, dentistry, and gastroenterology, and an active research pipeline in oncology. This page reviews the established uses, the mechanism of singlet-oxygen generation under red light, the antimicrobial photodynamic applications, and what current cancer research does and does not support.
Table of Contents
- What Photodynamic Therapy Is
- Methylene Blue as a Photosensitizer
- Approved and Common Clinical Uses
- Antimicrobial Photodynamic Therapy
- Cancer Research
- Barrett's Esophagus
- Dermatology Applications
- Dental and Periodontal PDT
- What This Does Not Mean
- Research Papers and References
- Connections
What Photodynamic Therapy Is
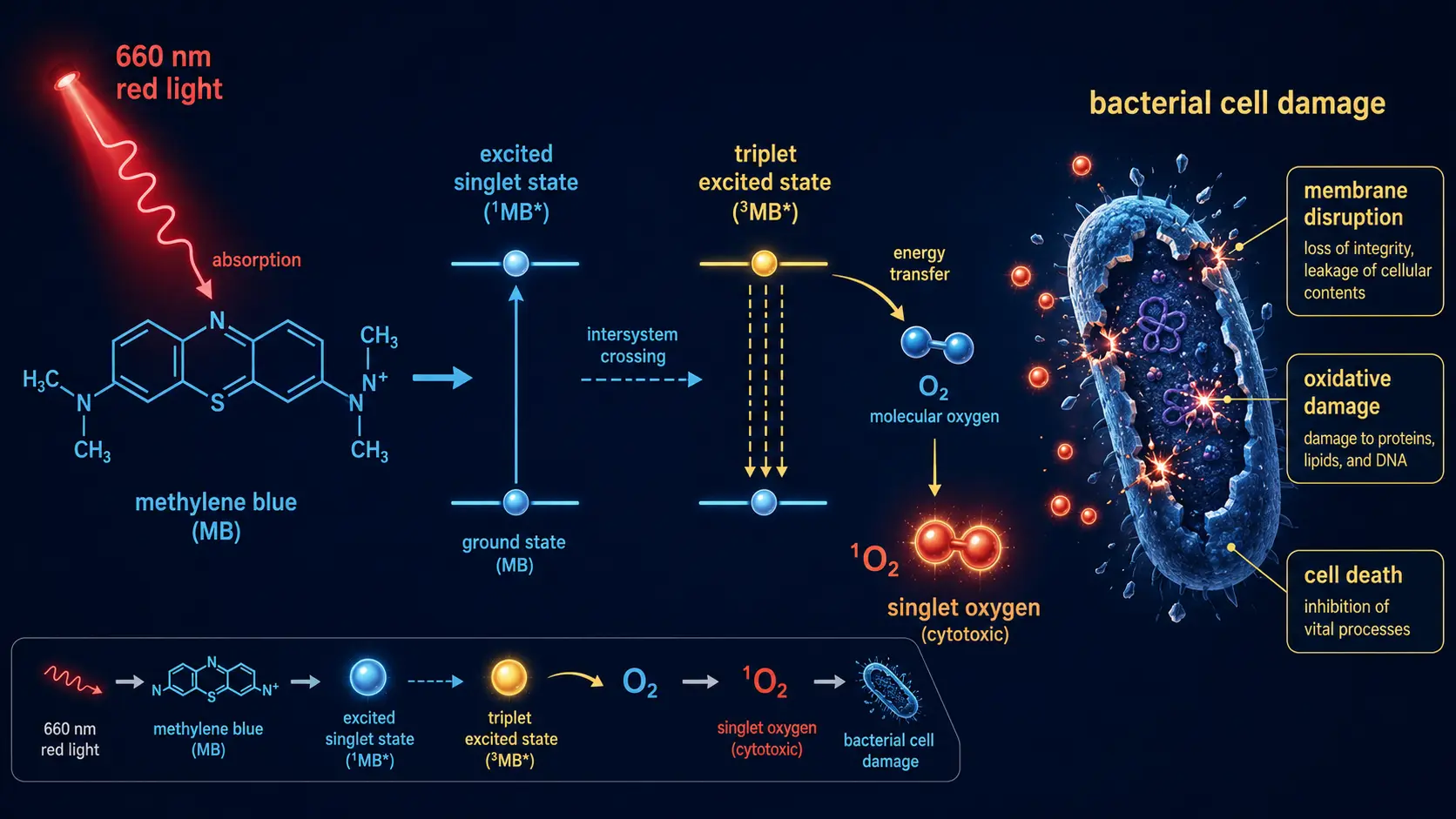
Photodynamic therapy involves three components: a photosensitizing drug, a light source of the appropriate wavelength, and oxygen at the treatment site. The drug is administered (topically, orally, or intravenously) and accumulates preferentially in target tissue. Light at the absorption wavelength of the drug is then directed at the lesion. The drug absorbs the photon, transitions to an excited state, and transfers energy to molecular oxygen, generating singlet oxygen (¹O₂) and other reactive oxygen species. These species damage proteins, lipids, and DNA in the immediate vicinity, killing cells locally without significant systemic toxicity.
The selectivity of PDT comes from three sources: (1) the drug's preferential accumulation in target tissue (often vasculature or rapidly-dividing cells); (2) targeted light delivery; (3) the very short diffusion distance of singlet oxygen (~20–160 nm) means damage is confined to where the drug, light, and oxygen overlap.
Methylene Blue as a Photosensitizer
Methylene blue absorbs strongly in the red region of the visible spectrum (peak around 660–670 nm). Red light penetrates tissue better than blue or green — useful clinically because it can reach lesions a few millimeters deep without surgery. When the absorbed photon excites MB to its triplet state, MB transfers energy to oxygen with reasonable efficiency, generating singlet oxygen plus smaller amounts of superoxide and hydroxyl radical.
Compared to porphyrin-based photosensitizers (e.g., Photofrin), methylene blue is:
- Cheaper and widely available
- Cleared faster from healthy tissue (less prolonged photosensitivity)
- Active at red wavelengths that penetrate tissue better
- More effective against gram-positive bacteria than against many cancer cell lines
The combination has made MB the workhorse photosensitizer for antimicrobial PDT and a steady research subject for cancer applications.
Approved and Common Clinical Uses
- Antimicrobial photodynamic therapy for periodontal disease, root canal disinfection, and chronic wounds
- Topical PDT for actinic keratosis and superficial basal cell carcinoma in some jurisdictions
- Methylene blue staining for Barrett's esophagus surveillance (chromoendoscopy)
- Investigational PDT for esophageal dysplasia, oral leukoplakia, fungal infections, and onychomycosis
- Surgical mapping — sentinel lymph node identification, parathyroid surgery
Antimicrobial Photodynamic Therapy
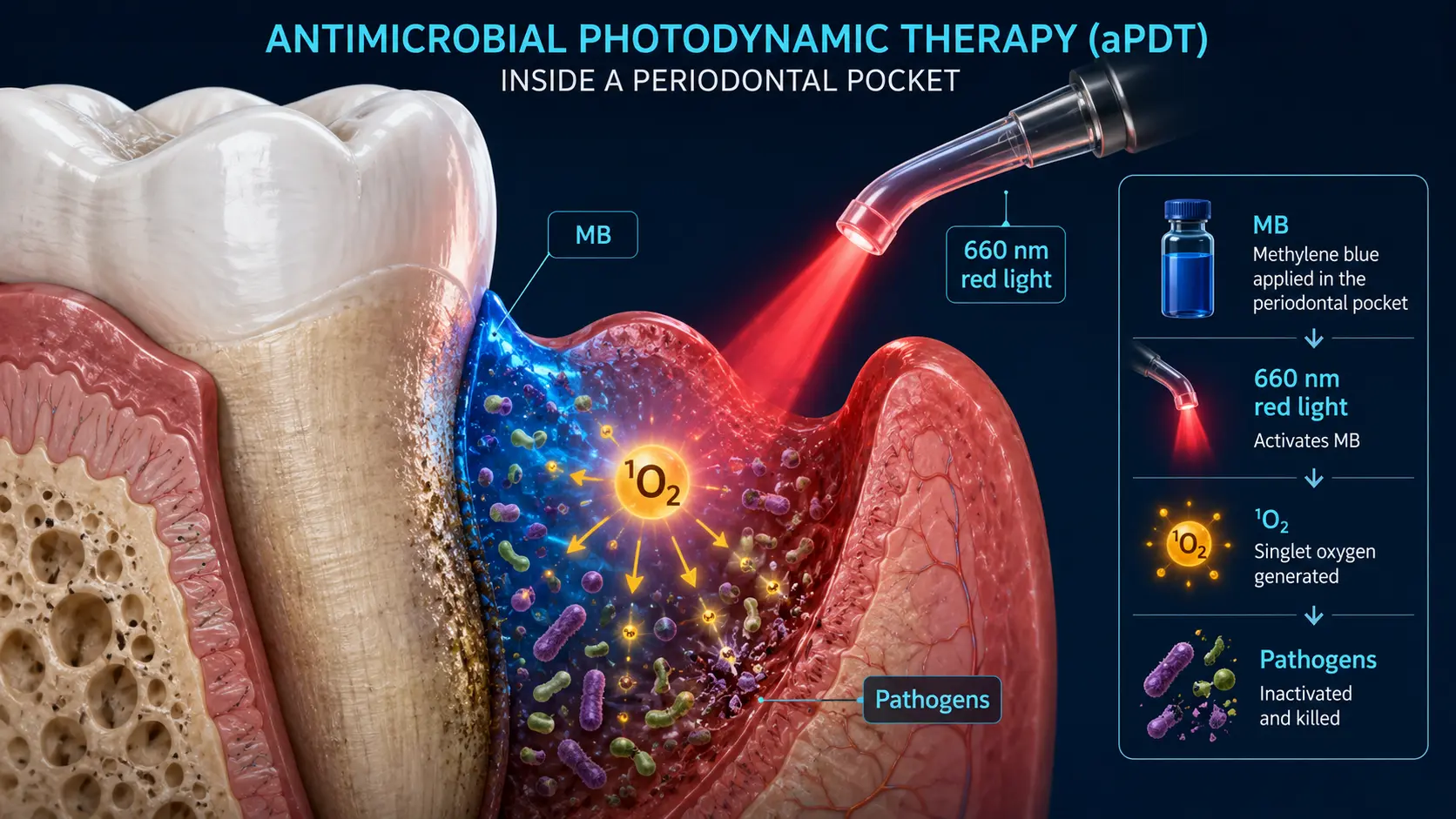
Antimicrobial PDT (aPDT) using methylene blue has the strongest evidence base. Mechanism: MB binds to bacterial cell walls and intracellular nucleic acids; red-light exposure generates singlet oxygen that damages bacterial membranes and DNA. Effective against gram-positive bacteria (including MRSA), gram-negative bacteria (with somewhat reduced efficacy due to outer membrane), fungi, and some viruses.
Clinical applications:
- Periodontal disease — meta-analyses support adjunctive aPDT after scaling and root planing
- Endodontics — root canal disinfection
- Chronic wounds — pressure ulcers, diabetic foot ulcers
- Acne vulgaris — targeting Cutibacterium acnes
- Onychomycosis (toenail fungus) — emerging evidence as alternative to oral antifungals
- Oral candidiasis
aPDT has the appeal of being non-antibiotic (no resistance development) and locally targeted.
Cancer Research
Methylene blue's role in cancer is best described as a research-stage adjunct, not a primary therapy. Mechanisms with theoretical relevance:
- Photodynamic killing at target lesions when topical or interstitial light delivery is feasible
- Mitochondrial-targeted oxidative stress — cancer cells often have dysregulated mitochondrial function and may be more sensitive to MB's redox effects than normal cells (the "Warburg effect" reversal hypothesis)
- Anti-Warburg metabolism — promoting oxidative phosphorylation over glycolysis
- Sensitization to chemotherapy — MB enhances doxorubicin and cisplatin cytotoxicity in some cell-line and animal studies
- Tumor microenvironment effects via NO-synthase inhibition and immune modulation
Clinical evidence is currently limited to:
- Phase 1–2 trials of MB-PDT for skin lesions (basal cell carcinoma, actinic keratosis) with reasonable efficacy
- Case series in Barrett's esophagus dysplasia
- Investigational use in palliative care for chemo brain (mitochondrial cognitive support during chemotherapy)
Larger randomized cancer trials with methylene blue specifically are limited. The grey-market promotion of methylene blue as a "cancer cure" or as a primary cancer therapy is not supported by evidence and runs the risk of distracting from established treatments.
Barrett's Esophagus
Barrett's esophagus is metaplastic columnar replacement of the normal squamous esophageal epithelium, often as a consequence of chronic gastroesophageal reflux. It carries an elevated risk of esophageal adenocarcinoma. Methylene blue has two roles in Barrett's care:
- Chromoendoscopy — topical methylene blue staining during upper endoscopy improves detection of dysplasia by highlighting absorbing intestinal-type epithelium. Used as an adjunct to standard high-resolution endoscopy.
- Photodynamic therapy — MB-PDT has been studied for ablation of Barrett's mucosa with high-grade dysplasia, though it has been largely supplanted by radiofrequency ablation in current practice.
This is a legitimate, established gastroenterology use that does not extrapolate to general "anti-cancer" benefit of oral methylene blue.
Dermatology Applications
Topical methylene blue plus red-light therapy has been studied for:
- Actinic keratosis (precancerous sun-damage spots)
- Superficial and nodular basal cell carcinoma in patients who are not surgical candidates
- Bowen's disease (squamous cell carcinoma in situ)
- Acne vulgaris (combined antimicrobial and anti-inflammatory action)
- Cutaneous T-cell lymphoma (specialized centers)
Treatment is performed by trained dermatologists with calibrated light sources. The DIY at-home use of red light + methylene blue for skin lesions is not the same procedure and is not recommended without dermatologic evaluation of the lesion first.
Dental and Periodontal PDT
The dental literature on aPDT with methylene blue is one of the more mature application areas. Multiple systematic reviews and meta-analyses support the use of aPDT as an adjunct to standard scaling and root planing in moderate-to-severe periodontitis. Improvements in probing depth, clinical attachment level, and bleeding indices are typically modest but statistically significant. Endodontic disinfection of root canals after mechanical instrumentation is another well-supported use.
What This Does Not Mean
The legitimate photodynamic uses of methylene blue do not translate into general anti-cancer benefit of oral methylene blue without targeted light delivery. Several common confusions to clear up:
- Oral MB without light delivery to a tumor is not photodynamic therapy. It does not generate the targeted singlet oxygen that drives PDT efficacy.
- "Methylene blue cures cancer" claims are not supported by current evidence and have prompted FDA enforcement actions on several grey-market sellers.
- Mitochondrial support is not the same as direct anti-cancer activity. Some cancers may benefit from mitochondrial reactivation; others use mitochondria for aggressive growth and might be accelerated by it. The picture is not yet clear, and self-treating cancer with oral MB is not a substitute for evidence-based oncology.
- Photodynamic therapy with MB is a clinical procedure, not a home protocol. It requires correct dosing, wavelength-specific light, and patient selection.
For patients with cancer interested in methylene blue, the conversation should happen with their oncology team, who can evaluate whether any specific PDT or research-protocol use is appropriate.
Research Papers and References
- MB photodynamic therapy — PubMed search
- aPDT for periodontal disease — PubMed search
- MB and Barrett's esophagus — PubMed search
- MB-PDT for basal cell carcinoma — PubMed search
- MB as chemo sensitizer — PubMed search
- MB and Warburg effect — PubMed search
- aPDT for onychomycosis — PubMed search
Connections
- Methylene Blue Deep-Dive Articles:
- Methylene Blue Overview
- Mitochondrial Mechanism
- Pharmaceutical vs Industrial
- Oncology
- Dermatology
- Gastroenterology
- Oxidative Stress
- Silver Nanoparticles (antimicrobial)